Abstract
The talar body fractures are rare but a great challenge for the treatment. The frequently intra-articular fractures, vulnerable blood supply of talar body and high weight pressure make it in high risk of complications. To obtain an excellent access allowing for anatomical reconstruction of the articular surfaces and the axial deviation, an appropriate approach is necessary. Medial malleolus osteotomy approach (Chevron osteotomy) is frequently used. In rare cases of the lateral talar dome fracture, a lateral malleolar osteotomy becomes necessary. Additionally we’ve done a cadaver anatomy research designed to measure exposure area of the two approaches that shows each approach exposes the talar body articular surface about 35%. Thus, fully informing prognosis, careful analysis of the fracture, detailed acknowledgement of anatomy, and therefore choosing an appropriate approach seem important for the surgeons.
Keywords: Talar body fractures; Surgery, Medial/Lateral malleolus osteotomy approach
Abbreviations
AVN: Avascular Necrosis; CT: Computed Tomography
Introduction
Talar fractures account for only 0.5% of all fractures and 3% of the fractures in the foot [1-4]. The talus has a unique anatomical shape and function that provides the junction between the lower leg and the foot. It consists of head, neck and body. Talar body fractures are produced by an axial compression of the talus between the tibial plafond and calcaneus, accounting for 13% ~ 23% of all talar fractures [5]. Although occurring uncommonly, talar body fractures have confounded physicians for centuries. There have been isolated reports of treatment for talar body fracture, all of which complain the poor outcome with complications such as avascular necrosis of the talar body, posttraumatic arthritis, malunions and infections [1,5,6].
The fact that most fractures are intra-articular, vulnerable blood supply and high weight pressure, are main factors that make talar body fractures in high risk of long-term complications [7].
Although there are multiple capsular and ligamentous attachments, no muscles attach directly to the talus [8]. The body of the talus articulates with tibia, fibula and the calcaneus and about 60- 70% of the talus is covered with cartilage leaving only the area around the talar neck and the posterior aspect of the body for periosteal blood supply [9,10].
Extraosseous blood is supplied to the talus by three vessels: the peroneal, anterior tibial, and posterior tibial vessels [11]. The blood supply of the talus body: deltoid artery (medial 1/4); tarsal canal artery which is branch of posterior tibial artery (middle 1/2); tarsal sinus artery which is branch of anterior tibial artery and artery of the fibula (lateral 1/4) [10]. Fracture dislocations can easily compromise the blood supply to the body of the talus and lead to Avascular Necrosis (AVN). When exposing the talus, the deltoid ligament therefore must not be dissected in order to minimise the risk of AVN. The reported incidence of avascular necrosis for severely comminuted talar fracture is around 50%-75% [12,13].
Treatments
The vast majority of talar body fractures are either intra-articular or lead to a joint incongruity by extra-articular axial displacement. Thus, conservative treatment is very seldom indicated [14]. Only strictly non-displaced talar fracture in the CT scan can be treated in a cast in neutral position of the foot and ankle for 6 weeks [9,15]. Such treatment does not allow early motion, which is very important in the re-habitation care. In addition, malunions after talar fractures almost invariably lead to disabling impairment of foot function, it’s of great importance to recover anatomical integrity of the talus and its joints. Sneppen et al. [16] reported high rates of malunion, osteonecrosis, and arthritis with non-surgical treatment.
As a consequence, surgical treatment is almost always indicated. The purposes of surgical reconstruction in displaced body fractures are to anatomically reduce the articular surfaces of the talar body, and also to ensure that the remaining precarious blood supply to the talus is not reduced further.
Surgical Approaches
Since the talar body fracture is surrounded by the distal part of fibula and tibia combined with other important structure that stabilize lower tibiofibular joint, talus is difficult to be addressed. Multiple surgical approaches are reported. Others include anteromedial approach, posteromedial approach, anterolateral approach posterolateral approach [10,17,18]. These are mainly used in talar neck fractures. The most commonly used approach is the anteromedial approach. For talar body fractures, the approaches could not provide good exposure and thus increases the likelihood of poor reduction and destroying the main sources of blood supply. Thus the incision may be extended proximally and a medial malleolar osteotomy for the treatment of body fractures.
A medial/lateral malleolus osteotomy approach allows perfect control of the whole medial/lateral part of the talus, which is also suggested by other surgeons for talar body fracture, especially in cases of comminuted body fractures [9,10].
Medial malleolus osteotomy approach (Chevron osteotomy) is frequently used [17]. By extending the anteromedial incision proximally, one reaches the medial malleolus. The capsule should be opened in order to identify the apex between the medial malleolus and the plafond of the tibia. This allows one accurate positioning of the medial malleolar osteotomy. The osteotomy must be in such a way that it avoids the distal tibial plafond. The articular surface is violated only in the infratectal region. This is done first by visualizing the joint surface before cutting. The medial malleolus is predrilled and pre-tapped. After pre-drilling and pre-tapping for the lag screws, the saw cut goes almost to the articular surface. Chevron osteotomy goes at 5cm proximal to the medial malleolus tip from the front to the back (120 degrees) and opening downward (45 degrees). Every effort should be made to protect the triangular ligament and the triangle. In that fashion, the articular surface can be re-apposed without articular loss at the end of the operation. Anterior and posterior small flat retractors are inserted around the malleolus into the joint before the osteotomy is completed to protect the dome of the talus and the posterior tibialis tendon. Then an osteotome is used to crack the medial malleolar piece and to reflect it distally on its retained soft tissue and blood supply. Once the medial malleolus is out of the way, it can achieve excellent access and deal with an irreducible dislocation of the body. Different from routine oblique osteotomy, wedge-shaped Chevron osteotomy can achieve more stability after medial malleolus reduction. Besides, it retains integrity of the deltoid ligament. During the approach, there’s less chance to damage main artery as to lead to AVN for the blood supply is scarce in the field.
Rarely, in cases of comminution of the lateral aspect of the talar dome, a lateral malleolar osteotomy becomes necessary [9]. An incision parallel to the lateral of the fibula is made. The fibular osteotomy is planned 5 cm proximal to the lateral malleolus tip with an oscillating saw after fully exposure of the fibula between the tibiofibular syndesmosis and peroneus. This osteotomy should be transverse to allow compression plating at the end of the procedure. The anterior distal tibiofibular ligaments are also needed to incise. Then overturn the distal segment of fibula posterior-inferiorly and effort should be made to protect anterior/posterior talofibular ligament, calcaneofibular ligament, and peroneus. At the end of the procedure, once the anterior tibiofibular ligaments are reconstructed, stability of the ankle will have been restored. The osteotomy provides excellent visualization of the tibial plafond and the lateral talus and talar articular surface.
However, there’s little study about exposure area of the two approaches. To share our experience of medial/lateral malleolus osteotomy approach and measure the exposure percentage of the talar body of each osteotomy approach, we have conducted a cadaver anatomy research. When exposing the media talus (Figure 1) and lateral talus (Figure 2) via approach as previous statement, we dye red in order to measure the exposure percentage of medial talar body articular surface and green for lateral counterpart. With different dyeing color, we could measure the exposure percentage of talar body. Each approach exposes the talar body articular surface about 35% (Figure 3). We could not elucidate an optimal one that mostly fit talar fractures with better outcomes, but to make the reduction more facilitating and direct, we could make an appropriate surgical approach depending on fracture-line position on the CT-scan, soft tissue conditions.
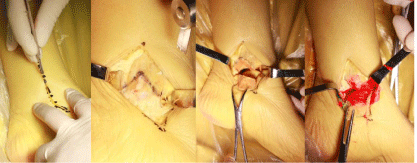
Figure 1: Medial malleolus osteotomy approach and exposing area of medial
talar body with red dyeing.
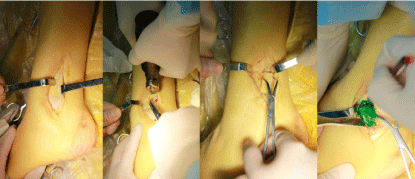
Figure 2: Lateral malleolus osteotomy approach and exposing area of lateral
talar body with green dyeing.
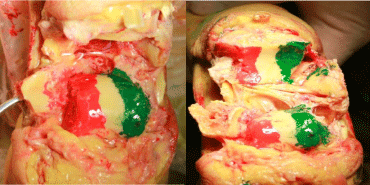
Figure 3: Exposing area of lateral talar body with green dyeing and exposing
area of medial talar body with red dyeing.
Conclusion
Talar body fractures are rare but due to the position of talus in the most important joints of the foot and ankle area, the little flaw in treatments can lead to considerably severe consequences. Even with appropriate surgical treatment, there are still significant challenges associated with treating displaced talar body fractures, as these often have poor long-term functional and radiological results according to limited studies now available. An approach, that provides good exposure in order to achieve anatomical reduction and preserve blood supply, is of great importance. Given the conclusions of previous and our studies, it seems logical to recommend the following actions to make therapy plan and choose the surgical approach:
- Systematic preoperative CT scan to fully analysis of the fracture line and fracture displacement;
- Detailed acknowledge of blood supply, fracture classification and exposing area of each approach;
- Fully informing prognosis.
Acknowledgement
This study was funded by the Key Disciplines Group Construction Project of Pudong Health Bureau of Shanghai (grant no. PWZxq2014-03).
References
- Stake IK, Madsen JE, Hvaal K, Johnsen E, Husebye EE. Surgically treated talar fractures. A retrospective study of 50 patients. Foot and ankle surgery: official journal of the European Society of Foot and Ankle Surgeons. 2016; 22: 85-90.
- Ohl X, Harisboure A, Hemery X, Dehoux E. Long-term follow-up after surgical treatment of talar fractures: Twenty cases with an average follow-up of 7.5 years. International orthopaedics. 2011; 35: 93-99.
- Schulze W, Richter J, Russe O, Ingelfinger P, Muhr G. Surgical treatment of talus fractures: a retrospective study of 80 cases followed for 1-15 years. Acta orthopaedica Scandinavica. 2002; 73: 344-351.
- Sanders DW, Busam M, Hattwick E, Edwards JR, McAndrew MP, Johnson KD. Functional outcomes following displaced talar neck fractures. Journal of orthopaedic trauma. 2004; 18: 265-270.
- Kilic A, Kabukcuoglu Y, Sokucu S. The treatment of talar body fractures with compression screws: a case series. Cases journal. 2009; 2: 7953.
- Lemaire RG, Bustin W. Screw fixation of fractures of the neck of the talus using a posterior approach. The Journal of trauma. 1980; 20: 669-673.
- Dale JD, Ha AS, Chew FS. Update on talar fracture patterns: a large level I trauma center study. AJR American journal of roentgenology. 2013; 201: 1087-1092.
- Ahmad J, Raikin SM. Current concepts review: talar fractures. Foot & ankle international. 2006; 27: 475-482.
- Rammelt S, Zwipp H. Talar neck and body fractures. Injury. 2009; 40: 120-135.
- Cronier P, Talha A, Massin P. Central talar fractures--therapeutic considerations. Injury. 2004; 35: Sb10-22.
- Haliburton RA, Sullivan CR, Kelly PJ, Peterson LF. The extra-osseous and intra-osseous blood supply of the talus. The Journal of bone and joint surgery American volume. 1958; 40: 1115-1120.
- Chan G, Sanders DW, Yuan X, Jenkinson RJ, Willits K. Clinical accuracy of imaging techniques for talar neck malunion. Journal of orthopaedic trauma. 2008; 22: 415-418.
- Metzger MJ, Levin JS, Clancy JT. Talar neck fractures and rates of avascular necrosis. The Journal of foot and ankle surgery: official publication of the American College of Foot and Ankle Surgeons. 1999; 38: 154-162.
- Fortin PT, Balazsy JE. Talus fractures: evaluation and treatment. The Journal of the American Academy of Orthopaedic Surgeons. 2001; 9: 114-127.
- Vallier HA, Nork SE, Barei DP, Benirschke SK, Sangeorzan BJ. Talar neck fractures: results and outcomes. The Journal of bone and joint surgery American volume. 2004; 86: 1616-1624.
- Sneppen O, Christensen SB, Krogsoe O, Lorentzen J. Fracture of the body of the talus. Acta orthopaedica Scandinavica. 1977; 48: 317-324.
- Ziran BH, Abidi NA, Scheel MJ. Medial malleolar osteotomy for exposure of complex talar body fractures. Journal of orthopaedic trauma. 2001; 15: 513-518.
- Trillat A, Bousquet G, Lapeyre B. Displaced fractures of the neck or of the body of the talus. Value of screwing by posterior surgical approach. Revue de chirurgie orthopedique et reparatrice de l'appareil moteur. 1970; 56: 529-536.
