Abstract
Background: Ingrown toenails (unguis incarnatus) are common in persons with Diabetes Mellitus (DM) and Peripheral Arterial Disease (PAD). Minimal invasive treatment of ingrown toenails with spiculectomy and/or orthonyxia might be a promising treatment option.
Aim: The aim of this study was to evaluate the efficacy and safety of minimal invasive treatment spiculectomy and orthonyxia
Design/Setting: Prospective observational cohort study in an outpatient podiatric clinic
Method: Eighty-eight patients with unguis incarnatus were included. Primary outcomes were post-procedural complication rate (infection and hemorrhage), and duration of pain. Patient satisfaction during and after treatment procedure was evaluated.
Results: Healing was achieved in 80/88 (90.9%) persons; non-DM group 28/32 (87.5%) vs DM group 51/56 (91.1%); median healing time (21 [14, 42] days) and median treatment time; (56 [30, 86] days) were comparable between the non-DM and the DM groups. (Sixty-four patients (72.7%) had a significant pain reduction within 0-2 days. Median reduction of the VAS score after the first treatment was 2.0 points [0.0, 6.0] (non-DM group 3.5[1.0, 6.0]; DM group 2.0[0.0, 5.0] (p=0.0117)). Forty-eight (94, 4%) patients, 31(96.9%) non-DM group vs 53(94.6%) DM group (p=0.534)) had no limitations in daily activities by the affected toe after 14 days. There were no treatment-related complications like bleeding or infection.
Conclusion: Spiculectomy and orthonyxia resulted in a high patient satisfaction. Five of 88 patients needed referral for a partial nail resection. This treatment seems to be very suiTable for persons with a high risk for foot ulcerations.
Keywords: Orthonyxia; Spiculectomy; Unguis incarnates; Ingrown toenail; Diabetic foot
Abbreviations
DM: Diabetes Mellitus; PAD: Peripheral Arterial Disease; IWGDF: International Working Group of the Diabetic Foot; VAS: Visual Analogue Scale; ABI: Ankle Brachial Index; TP: Toe Pressure; GP’s: General Practitioners; MODY: Maturity Onset Diabetes of the Young
Introduction
Background/Rationale
Unguis incarnatus (ingrown toenail) is a highly prevalent condition with a prevalence of 54 per 10.000 persons per year in Dutch general practice [1]. Persons with Diabetes Mellitus (DM), especially those with neuropathy and/or Peripheral Arterial Disease (PAD), are at increased risk of developing unguis incarnates [2] and prone to develop complications, such as subungual ulcers with impaired healing and/or infection [3]. This is emphasized in the current guidelines, urging treatment of unguis incarnatus as if it is a pre-ulcerative sign and risk of amputation [4]. Depending on the presence of pain, drainage, inflammation and granulation tissue, unguis incarnatus is classified into 3 stages (Table 1), [1]. For patients with stage 1 conservative treatment is recommended [5]. Nail matrix excision and application of phenol is the advised treatment option in stages 2 and 3 [1, 6]. In persons with increased risk for foot complications, such as DM and PAD, there are complication risks with nail matrix excision and phenol application; therefore these patients have been often excluded from studies on effectiveness of phenol matricectomy [7].
Characteristic
Total group n=88
Non-DM group n=32
DM group n=56
Age at baseline (year)
62.6 [42.5,73.2]
50.6 [26.7,70.2]
66.6 [45.7,74.11]
Gender (Female)
44 (50)
20 (62.5)
24 (42.9)
Duration of ingrown toenail (days)
14 [7.0,29.0]
28 [10.3,87.5]*
14 [7.0,26.3]*
Digitus 1 involved
73 (83.0)
27 (84.4)
46 (82.1)
Left/right/bilateral
42(47.7)/ 33 (7.5)/13(14.8)
18 (56.3) /10(31.3)/4(12.5)
24(42.9)/23(41.1)/9(16.1)
Partial nail resection in medical history (yes)
10 (11.4)
5 (15.6)
5 (15.6)
Performed by general practitioner
7 (8.0)
4 (12.5)
3 (5.4)
Performed by Surgeon
3 (3.4)
1 (3.1)
2 (3.6)
Regular pedicure visit (yes)
60 (68.2)
13 (40.6)
47 (83.9)
Heifetz gradation
Stage 1
48 (54.5)
16 (50)
32 (57.1)
Stage 2
29 (33.0)
10 (31.3)
19 (33.9)
Stage 3
11 (12.5)
6 (18.8)
5 (8.9)
Normal shoe wear impossible (yes)
38 (43.2)
15 (46.9)
23 (41.1)
Toe limiting normal day functioning (yes)
39 (44.3)
18 (56.3)
21 (37.5)
Diabetes (yes)
56 (63.6)
Type1/Type2/Mody
15 (17)/40 (45.5)/1(1.1)
Glucose lowering drugs
Diet
1 (1.9)
Oral
11 (19.6)
Insulin
25 (44.6)
Oral and insulin
19 (33.9)
Duration DM baseline
46.9 [24.4,56.6]
Last measured Hba1c at baseline mmol/mol
60.0 [50.5,74.3
Sensory Loss (yes)
40 (45.5)
3 (9.4)*
37(66.1)*
Immune compromised (yes)
12 (13.6)
6 (18.7)
6 (10.7)
Peripheral arterial disease (yes)
25 (28.4)
6 (18.7)
19 (33.9)
Fontaine 1
1 (1.1)
0 (0)
1 (1.8)
Fontaine 2a
7 (8.0)
1 (3.1)
6 (10.7)
Fontaine 2b
6 (6.8)
1 (3.1)
5 (8.9)
Fontaine 3
3 (3.4)
1 (3.1)
2 (3.6)
Fontaine 4
8 (9.1)
3 (9.4)
5 (8.9)
Table 1: Baseline characteristics of 88 included patients.
In persons without DM, some evidence exists that orthonyxia (nail branching) is equally effective compared to phenol matricectomy [8]. No studies have investigated the combination of spiculectomy (removing the nail part piercing the skin) and orthonyxia. Spiculectomy could increase orthonyxia procedure efficacy without overly compromising safety. This treatment could especially be suitable for the high-risk patient, obviating the need for local anaesthesia and a tourniquet, and restricting the wound size associated with more extensive surgical interventions.
In our hospital, high risk patients are discussed within a specialized foot team, and often the decision is made to opt for a conservative approach when surgeons estimate the risk of complications as too high. For that reason, and despite limited evidence, spiculectomy and orthonyxia have been introduced several years ago in our hospital in high-risk patients.
Objectives
Aim of this study was to evaluate the effectiveness and safety of combined spiculectomy and orthonyxia performed by a podiatrist in patients with high risk for foot ulcers.
Materials/Methods
Study design and setting
Single centre prospective cohort study. Patients referred to the outpatient podiatric clinic in the Isala hospital (Zwolle, the Netherlands) with the diagnosis ingrown toenail were assessed for eligibility. This manuscript was written in accordance with the STROBE checklist.
Participants
All high-risk patients, >18 years, with a diagnosis of ingrown toenail were invited to participate. High risk for foot problems was defined as having peripheral sensory loss, peripheral arterial disease and/or immune compromised therapy. Patients with chrome or nickel contact allergy were excluded for orthonyxia, since the remanium wire which is used contains chrome/nickel steel. Patients with severe obstructive artery disease with a toe pressure (TP) <15 mmHg were excluded for orthonyxia because of the risk for (pressure) ulcers due to poor skin conditions. For spiculectomy there were no reasons for exclusion. Patients not able to give written informed consent, to understand the Dutch language or with insufficient cognitive abilities to understand the study information were excluded.
Variables/Outcomes
Primary outcomes were complete cure, post-procedural complication rate (infection and hemorrhage) and duration of pain. Secondary outcomes were participant satisfaction, satisfying procedural result, healing time, time to relief of symptoms, time to normal functioning, recurrence of symptoms, time till clinical cure and failure rate. These outcomes are in accordance with the end-points used in the most recent Cochrane review [1]. Complete cure was defined as an intact skin in the nail sulcus and no signs of inflammation of the affected toe and a (VAS) Visual Analogue Scale score of 0. A satisfying procedural result was defined as complete cure and free from recurrence at week 26 without complications. Complications were defined as an increase of infection symptoms, ulcers with a delayed healing (>3 weeks) process. Healing time was defined as the time between entering the study and consulting date when the podiatrist saw an intact skin and a VAS score of 0. Treatment time was defined as the time between entering the study and the last treatment date for the nail problem. All outcomes were analysed for the total group, and for the groups with and without DM separately.
Interventions
Treatment could be spiculectomy and/or orthonyxia. During spiculectomy, the nail spicule that pierces the skin is removed (Figure 1). After the skin has healed (after one or two weeks), the orthonyxia (Figure 2) can be placed. The wire is hooked under the nail edges and guides regrowth [1]. Tension on the nail is applied by pinching the omega shape of the orthonyxia together. In some cases, the podiatrist placed a tamponade under the nail edge, to lift the nail and to protect the underlying skin. Silver nitrate was applied on hypergranulation tissue. All patients were analyzed after 26 weeks.
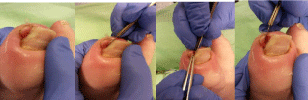
Figure 1: Procedure of spiculectomy.
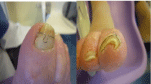
Figure 2: Bilateral orthonyxia.
Data sources/Measurements
During the first visit, baseline data were collected. These contained data of demographics, duration, history of (partial) nail resections, use of analgesics, the affected toe and nailfold, and possible aetiology or contributing factors. Local signs for inflammation, Heifetz gradation, presence of hypergranulation and amount of exudate (none, limited, severe) were described. In case of DM, disease duration, most recent Hba1c and use of glucose lowering treatment were registered. All patients were screened for PAD with a handheld Doppler ultrasound. In patients with a triphasic of biphasic Doppler sound and palpable pulses a diagnosis arterial disease could be refuted and treatment initiated by the podiatrist. A vascular surgeon saw all patients with biphasic doppler sounds without palpable pulses, or monophasic signals. In patients with PAD, ankle brachial index, toe pressure and Fontaine classification were registered. All patients were screened for a loss of protective sensation with a 10-gram Weinstein monofilament.
Patients indicated the VAS score for pain three times during the first visit. The first VAS score was asked before starting the treatment. The second provided information about the pain score during treatment and the last about the pain directly after treatment.
Statistical methods
Data entry was performed in duplicate. All variables were structured in a digital patient record form. All statistical calculations were performed using SPSS 23 (IBM). Descriptive statistics included number (percentage), mean (± SD) and median [Interquartile Range [IQR)]. Data were compared with the Fisher’s exact test in case of categorical data. In case of continuous data, Student’s t-test or Mann-Whitney U test were used if the data was distributed normally or skewed, respectively. Q-Q plots and histograms were used to determine if the tested variable had a normal distribution or not. To visualize the duration until closure of the nail fold and reduction of the VAS score to zero, a Kaplan-Meier curve was constructed. Hodges-Lehmann confidence interval was used to describe the difference between two medians. A 5% significance level was used.
Results
Recruitment
In the period from November 2016 to August 2018, 96 patients were invited to participate.
Participants
Of the 96 potential participants, 8 patients were excluded (Figure 3). One patient was diagnosed with a subungual exostosis causing the nail problem, one patient had infected necrosis of the hallux. Two patients did not understand the Dutch language. One patient was not able to read. Three patients refused to participate. No patients were lost to follow up. Therefore, 88 patients could be analysed after 26 weeks.
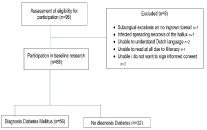
Figure 3: Flowchart.
Descriptive data
The 88 patients (50% female) included in this study had a median age of 63 [42, 73] years (Table 1). In 73 (83%) patients, the affected toenail was a hallux nail. In 52 (63.4%) patients, the medial nail fold of the hallux was affected; 42 (47.7%) ingrown toenails were on the left foot. The median duration of the ingrown toenail before entering the study was 14 [7.0, 29.5] days (the non-DM group 28 [10.3, 86.5]; DM group 14 [7.0, 26.3] days (difference between medians p=0.006, 95% CI: 2, 23). 48 patients (54.5%), had a Heifetz stage 1(Table S1), 29 stage 2 (33.0%), eleven (12.5%) a stage 3. Peripheral neuropathy was present in 40 (45.5%) persons: non-DM group 3 (9.4%), DM group 37 (66.1%) (Difference between percentages p=0.000: 95% CI 40.7, 72.69).
Twenty-five (28.4%) persons had a diagnosis of peripheral arterial disease (PAD); non-DM group 6 (18.8%), DM group 19 (33.9%) (Difference between percentages p=0.148, 95% CI: -3.17, 33.53). The ABI and toe pressure were measured only in persons with unpalpable a. dorsalis pedis or a. tibialis anterior (Table 2).
Total Sub-group n=25
Non-DM group n=6
DM group n=19
ABI left foot
0.80 [0.56,1.01] n=25
0.57 [0.50,0.70] n=6
0.89 [0.66,1.04] n=19
ABI right foot
0.84 [0.55,1.04] n=23
0.83 [0.21,1.02] n=5
0.88 [0.62,1.04] n=18
Toe pressure left foot
61.5 [33.3,75.0] n=16
43.5 [27.3,57.5] n=4
65.0 [35.0,80.3] n=12
Toe pressure right foot
58.0 [33.0,97.0] n=16
24.5 [0.0,70.8] n=4
76.0 [35.5,80.3] n=12
Table 2: Ankle Brachial Index and Toe Pressure.
Nine (10.1%) patients had a subungual ulcer beneath the toenail; non-DM group0, DM group 9 (16.1%) (Difference between percentages p=0.02395, 95% CI: 6.45, 25.69).
Healing was achieved in 80/88 (90.9%) patients; non-DM group 28/32 (87.5%), DM group 52/56 (91.1%) (Difference between percentages p=0.455, 95% CI: -7.94, 18.65). Median healing time was 21 [14, 42] days; non-DM group 21.5 [14, 43], DM group 21.0 [14, 42] (difference between medians p=0.825, 95%-CI: -7, 9.0) (Figure 4) Kaplan Meier curve Healing. Median treatment time was 56 [30, 86] days; non-DM group 63.5 [35, 84.8], DM group 53.0 [27.3, 91.0] days (difference between medians p=0.690, 95% CI: -16, 21). The percentage of patients healing within two visits was 63 (71.6%); the non-DM group 21(65.6%), the DM group 42(75%) (Difference between two percentages p=0.576, 95% CI: -5.75, -25.06).
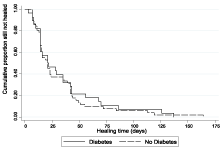
Figure 4: Kaplan Meier survival curves days to healing (diabetes vs nodiabetes).
The median number of treatments was 3.0 [2.0, 4.0]; non-DM group 3.0 [2.3, 4.0], DM group 3.0 [2.0, 4.0] (difference between medians p=0.825, 95% CI: 0.0, 1.0).
Nine (10.3%) patient needed referral to the surgeon. Five (5.7%) patients for a partial nail resection because of treatment failure; non- DM group 4 (12.5%), DM group 1 (1.8%). Four (4.5%) patients needed referral for vascular analysis after the first podiatric treatment of the nail, because a clinical suspicion of peripheral arterial disease; non- DM group 1 (3.1%), DM group 3 (5.4%). Eighty-two of 88 (93.2%) patients could wear normal shoes 0-2 days after first treatment. Sixtyfour patients (72.7%) reported a significant pain reduction in 0-2 days. The median VAS pain score reduced from 6.0 [2.0,8.0]; non- DM group 6.5 [3.3,8.0], DM group 5.0 [0.0,7.0] at the first visit, to 3.5[0.25,6.0]; non-DM group 4.0 [2.0,6.7], DM group 3.0 [0.0,6.0] during the first treatment, to 1.0 [0,3]; non-DM group 1.0 [0.0,4.75 ], DM group 0.5 [0.0,3.0] immediately after the first treatment. The median reduction in VAS score within the first treatment was 2.0 [0.0, 6.0]; non-DM group 3.5 [1.0, 6.0], DM group 2.0 [0.0, 5.0] (difference between medians: p=0.0117, 95% CI: 0.0, 2.0). After a median duration of 14 [7, 35] days the patients were seen again. 84 (94, 4%) patients, 31(96.9%) non-DM group vs 53(94.6%) DM group (difference between medians: p=0.534: 95% CI -1, 31, 8.58) had no limitations in daily activities anymore.
Median patient satisfaction was 9 [8, 10] (scale 0-10) with the second visit (n=88), 9 [8, 10] with the third visit (n=51), 9 [8, 10] with the fourth visit (n=19) and 9.0 [7, 9.5] with the fifth visit (n=9). Nine (10.2%) patients (5 (15.6%) non-DM group/4 (7.1%) DM group) had a recurrence within 26 weeks (difference between medians: p=0.284, 95% CI: -23.27, 6.398).
Discussion
Summary
The aim of this observational study was to see if spiculectomy with orthonyxia performed by a podiatrist could be a successful treatment option in high risk patients. From the 88 patients analysed, 89.8% of patients evaluated for suitability could be cured. Median duration until healing was 21 (95% CI 14 to 42) days. Total treatment time is longer because the nail outgrowth must be guided, to prevent recurrence. Patient satisfaction was high and most patients experienced a relief of pain immediately after the first treatment. Patients didn’t experience the orthonyxia as troublesome, and it did not hamper daily activities. Five patients were referred to the surgeon for partial nail resection because of treatment failure. There were no treatment-related complications like bleeding or infection.
Strengths and limitations
This has not been a randomized controlled study that studied treatment with either a non-treated or surgically treated control group. Also, inclusion was not defined by strict referral indications. Still, we consider the mixed study population and the referral pattern as being more or less representative for the actual situation in the Netherlands. Therefore, we see the results as being in support of the conclusion that for the Dutch situation with experienced podiatrists and a multidisciplinary team a more conservative approach to unguis incarnatus problems results in satisfactory outcomes.
Comparison with existing literature
In a Cochrane review the role of the non-surgical interventions to treat ingrown toenails was reported to be unclear [1]. There has been only one study (n=109) in which surgery (partial matrix excision) was compared to orthonyxia.
The findings were favourable for orthonyxia [2]. Although this more conservative treatment option has theoretical advantages in patients with DM and/or PAD mostly for safety reasons, up to now, there are no comparable randomized studies that investigated efficacy and safety of surgery vs orthonyxia in groups of patients with e.g. PAD and/or diabetes [1, 3].
Implication for research and/or practice
It is important to treat these patients at risk for serious foot problems involving a multidisciplinary team. A seemingly simple diagnosis of ingrown toenail could be the manifestation of a serious underlying problem (subungual fistula, osteomyelitis, PAOD4). In this specific group recognizing and assessing the severity of the situation is essential. Short communication lines with quick referrals and access to knowledgeable colleagues is very important for successful treatment results.
Notably all nine patients with a subungual ulcer at baseline belonged to the DM group, presenting with a combination of sensory loss and a diagnosis of PAD. This is also a great challenge in clinical practice. Due to peripheral neuropathy (significantly more frequent in DM patients), patients often don’t experience discomfort, don’t see the problem because it is positioned beneath the nail, and often can’t see or inspect their own feet at all. This can have serious consequences. The international working group of the diabetic foot therefore advises appropriate and timely screening for, and treatment of ingrown toe nails to help prevent foot ulcers (see the original online document of the IWGDF). Twenty-one percent of the persons with diabetes in our cohort showed an ingrown toenail without noticing this themselves. Often, there was a chance finding by the podiatrist during regular check-up. In patients without DM wrong cutting of the nails was significantly more often the reason for the ingrown nail problem. According to our study, spiculectomy and orthonyxia can be a recommended treatment option in patients with high risk at foot ulcers. It seems to be a safe and effective treatment.
Acknowledgements
The authors want to thank the staff of Isala Diabetes Centre and surgery, all podiatrist from Innofeet for their participation. Also, we wish to thank all patients who participated in this study and gave written informed consent for the use of the pictures. The authors want to thank Dr. N. Kleefstra, he was one of the initiators of this study.
Funding
This study was funded by the Dutch Diabetes Research Foundation [2014.00.1741]. The NVvP (Dutch association of Podiatrists), Innofeet podiatry and The Diabetes Research Foundation Zwolle.
Trial registration
Netherlands trial register: NL5824 (NTR5979).
References
- Eekhof JAH, Van Wijk B, Knuistingh Neven A and van der Wouden JC. Interventions for ingrowing toenails. Cochrane Database Syst Rev. 2012; 18: CD001541.
- Vural S, Bostanci S, Koçyigit P, Caliskan D, Baskal N and Aydin N. Risk Factors and Frequency of Ingrown Nails in Adult Diabetic Patients. J Foot Ankle Surg. 2018; 57: 289–295.
- Alavi A, Sibbald RG, Mayer D, Goodman L, Botros M and Armstrong DG, et al. Diabetic foot ulcers: Part I. Pathophysiology and prevention. J Am Acad Dermatol. 2014; 1.e1-18: quiz 19–20.
- Bus SA, van Netten JJ, Lavery LA, Monteiro-Soares M, Rasmussen A and Jubiz Y, et al. IWGDF guidance on the prevention of foot ulcers in at-risk patients with diabetes. Diabetes Metab Res Rev. 2016; 1: 16–24.
- Heidelbaugh JJ and Lee H. Management of the ingrown toenail. Am FAM Physician. 2009; 15: 303–308.
- Litzelman DK, Marriott DJ and Vinicor F. Independent physiological predictors of foot lesions in patients with NIDDM. Diabetes Care. 1997; 20: 1273–1278.
- Karaca N and Dereli T. Treatment of ingrown toenail with proximolateral matrix partial excision and matrix phenolization. Ann FAM Med. 2012; 10: 556–559.
- Kruijff S, van Det RJ, van der Meer GT, van den Berg ICMAE, van der Palen J and Geelkerken RH. Partial matrix excision or orthonyxia for ingrowing toenails. J Am Coll Surg. 2008; 20: 148–153.
