Abstract
Introduction: Calcific tendinitis is an uncommon presentation in the forefoot with relatively few cases reported in the medical literature. It is commonly overlooked and should form part of a differential diagnosis when assessing patients presenting with acute pain of the forefoot localised to a single joint or tendon. We present two cases of young women involved in amateur running and martial arts respectively who presented with acute pain of their forefoot.
Case Description: These 2 cases describe a 44 year old amateur female runner and 23 year old female martial arts athlete who presented with acute onset of pain affecting the dorsal aspect of their great toe interphalangeal joint and base of 1st metatarsal respectively. Both patients had tender erythematous swellings at the site of pain and difficulty weightbearing. Plain radiography revealed areas of calcification at the respective sites which was confirmed with ultrasound. Both patients underwent US guided corticosteroid injections with significant symptom improvement within 48 hours of injections and rapid return to sport.
Discussion: These two cases demonstrate an atypical presentation of acute calcific tendinitis affecting the forefoot and add two more cases to the reported literature. Combining the characteristic clinical presentation of acute pain affecting a tendon or joint with a tender erythematous swelling on examination with the typical radiographic features of calcification can promptly diagnose this often misdiagnosed condition and avoid unnecessary investigations. Conservative treatment and intralesional injection with corticosteroids can lead to rapid resolution and favourable patient outcomes.
Keywords: Calcific tendinitis; Calcific periarthritis; Foot
Introduction
Calcific tendinitis is a disorder of uncertain aetiology characterised by the deposition of calcium hydroxyapatite crystals in any tendon of the body [1-2]. The rotator cuff tendons are most commonly affected with the prevalence of radiographic calcific tendinitis in the shoulder being 2.7% [2]. The majority of patients are healthy and middle aged with case collections demonstrating twice as many women as men being affected [4]. Foot involvement is relatively uncommon. It typically affects the tendons around the plantar aspect of the first metatarsophalangeal joint with young women predominantly affected [5]. It less commonly affects the peroneus longus or tibialis posterior tendon.
A comprehensive literature review revealed relatively few cases of forefoot calcific tendinitis [6-12]. There has only been one published case in the English literature to the best of our knowledge of calcific tendinitis affecting the extensor aspect of the great toe [13]. In this case series, we present two cases of young women who presented with acute calcific tendinitis of the forefoot affecting the dorsal aspect of the great toe and base of 1st metatarsal respectively.
Case Presentation
Case 1
A 44-year-old woman with no known medical problems presented to the emergency department with a 24-hour history of sudden onset pain and swelling affecting the dorsal aspect of her right great toe interphalangeal joint. The pain and swelling came on suddenly following a run the previous day. She was an otherwise healthy patient with no previous history of pain, surgery or injury to the foot. She was an avid amateur athlete running on average 50km weekly. She was unable to weight bear on her foot in the emergency department.
On clinical examination there was notable erythema and swelling extending from the dorsal aspect of her first MTP joint along her great toe to the distal phalanx. It was associated with pain on palpation and passive extension and flexion of her great toe MTP joint and interphalangeal joint elicited pain.
A plain radiograph of the foot (Figure 1) demonstrated an area of calcification medial to the first interphalangeal joint which was confirmed as calcific periarthritis on US (Figure 2). The patient underwent US guided injection with 10mg Depo-Medrol mixed with 0.25% Marcaine. She reported significant improvement in symptoms within 48 hours and returned to light running 7 days later and normal activities at 14 days. A repeat x-ray 3 months later revealed complete resolution of the area of calcification (Figure 3) and the patient remained asymptomatic.
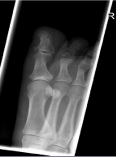
Figure 1: Oblique radiograph of right foot demonstrating an area of calcification
adjacent to the dorsal, medial aspect of the great toe interphalangeal joint.
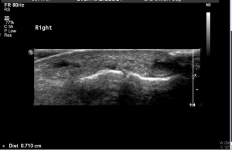
Figure 2: US of the right foot revealing the ill-defined area of calcification
demonstrated on radiograph of the right foot medial to the interphalangeal
joint.
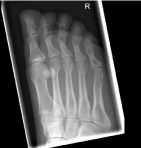
Figure 3: Oblique right foot radiograph with complete resolution of the focus
of calcification demonstrated previously.
Case 2
A 23-year-old martial arts athlete presented with a 4 day history of right foot pain and difficulty weightbearing. She was otherwise well with no medical problems. She reported kicking a boxing bag causing pain over the dorsal aspect of her first metatarsal 4 days previously. She noted progressive pain and swelling to the plantar aspect of her first metatarsal.
On examination of the plantar aspect of her foot was erythematous extending the length of her first metatarsal and tender to touch. She had significant pain on weightbearing.
A plain foot radiograph of the foot (Figure 4) showed an area of calcification at the level of the neck of the first metatarsal and US (Figure 5) confirmed a 1.3cm focus of calcification of the right flexor hallucis longus tendon sheath at the first metatarsal neck. 40mg of Depo-Medrol mixed with 0.25% Marcaine was injected under US guidance. 2 days after the injection she was weightbearing with complete resolution of erythema but still had slight residual pain on walking. She was reviewed one month later when she was symptom free and advised on a gradual return to sport.
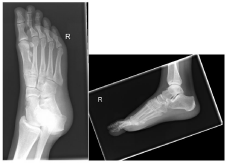
Figure 4: Oblique and lateral right foot radiograph demonstrating a globular
amorphous calcification on the plantar aspect of the first metatarsal.
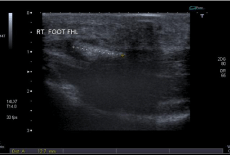
Figure 5: US of right foot revealing 1.3cm focus of calcification on the plantar
aspect of the right FHL tendon sheath at the level of the neck of the first
metatarsal.
Discussion and Conclusion
The aetiology of tendinous Basic Calcium Phosphate crystal (BCP) formation is not fully understood [2]. They can occur as a result of local tissue damage at sites associated with injury and inflammation. They produce symptoms once formed and mediate tissue damage by a variety of mechanisms including the direct interaction of nearby cells resulting in tissue damage in the absence of inflammation as well as the induction of inflammatory responses [14-16]. A three phase process has been described [17]. The precalcific phase is typically asymptomatic where fibrocartilaginous change is occurring. The calcification phase is further subdivided into three subphases (formative, resting and resorptive). It initially involves the formation of calcium deposits followed by a resting phase where calcifications produce symptoms. The resorptive phase is typically the most symptomatic where phagocyte infiltration and neoangiogenesis occurs. Granulation tissue forms at the site which is replaced by mature collagen in the post calcific phase.
Patients typically present as was the case with our two patients with acute onset of pain affecting a joint, bursa or tendon commonly associated with recent history of trauma or overuse as a preceding factor. Most patients are healthy young to middle aged women similar to our patients [4]. The affected area is typically tender and swollen with associated erythema.
Plain film radiography is usually sufficient for diagnosis. They appear as fluffy or sharply outlined extraarticular heterogenous deposits. They are typically described as amorphous or ‘cloud like’ when they are acute whereas chronic manifestations are more homogenous and denser. Ultrasound in appropriately trained hands can be used for diagnosis and is as sensitive as X-ray [18]. MRI can play a role in diagnosis with the appearance of a hypodense signal of calcific deposits in T1 and T2 sequences. However, it cannot as easily distinguish calcifications from other types of tissue damage when compared to CT scanning.
Management is typically conservative with rest, activity modification and the use of non-steroidal anti-inflammatory drugs. The injection of intralesional glucocorticoids is an alternative and produced rapid resolution of symptoms with our patients. Extracorporeal shockwave therapy or surgical intervention can be considered for those patients unresponsive to conservative measures. The prognosis of calcific periarthritis is variable and not well studied but may be site dependent. A study from 1986 of calcific periarthritis affecting the foot revealed symptoms were present from 3-30 days with a mean duration of 10 days [19]. The administration of intralesional glucocorticoids of our two patients resulted in near complete resolution of symptoms within 48 hours.
While an uncommon presentation, these two cases demonstrate the importance of having calcific tendinitis as part of your differential assessing patients. It is easily diagnosed with the typical clinical presentation of sudden onset pain around a joint with associated tenderness and swelling combined with the characteristic calcifications apparent on x-ray are usually sufficient for diagnosis. Conservative management is the mainstay of treatment and intralesional glucocorticoid injection can produce rapid resolution.
References
- Hamada J, Ono W, Tamai K, et al. Analysis of calcium deposits in calcific periarthritis. J Rheumatol. 2001; 28: 809-813.
- Oliva F, Via AG, Maffulli N. Physiopathology of intratendinous calcific deposition. BMC Med. 2012; 10: 95.
- Bosworth BM. Calcium deposits in the shoulder and subacromial bursitis. A survey of 12,122 shoulders. JAMA. 1941; 116: 2477.
- Lehmer LM, Ragsdale BD. Calcific periarthritis: more than a shoulder problem: a series of fifteen cases. J Bone Joint Surg Am. 2012; 94: e157.
- Fam AG, Rubenstein J. Hydroxyapatite pseudopodagra. A syndrome of young women. Arthritis Rheum 1989; 32: 741-747.
- Borgersen A. Myotendinitis calcarea at the proximal joint of the great toe. Acta Radiol. 1958; 50: 361-364.
- Schapira D, Scharf Y. Acute calcific tendonitis of the foot. Br. J. Rheumatol. 1994; 33: 1092-1094.
- Cox D, Paterson FW. Acute calcific tendinitis of peroneus longus. J Bone Joint Surg Br. 1991; 73: 342.
- Berge M, Wagner S, Jex J. Calcific Tendinopathy of the Abductor Hallucis Tendon in an Adolescent Gymnast. JBJS Case Connector. 2015; 5: 9.
- Garner H, Whelan J. Acute Calcific Tendinosis of the Flexor Hallucis Brevis: Case Report. Foot & Ankle Int. 2013; 34: 1451-1455.
- Melsom DS. Acute calcific tendinitis of the adductor brevis tendon of the foot. Foot Ankle Surg. 2006; 12: 109-111.
- Rhodes R, Stelling C. Calcific tendinitis of the flexors of the forefoot. Ann Emerg Med. 1986; 15: 751-753.
- Tomilson M, Williams L. Extensor hallucis longus calcific tendonitis: a case report. Foot Ankle Int. 2006; 27: 144-145.
- Stack J, McCarthy G. Basic calcium phosphate crystals and osteoarthritis pathogenesis: novel pathways and potential targets. Curr Opin Rheumatol. 2016; 28: 122-126.
- Roemhildt ML, Gardner-Morse MG, Morgan CF, et al. Calcium phosphate particulates increase friction in the rat knee joint. Osteoarthritis Cartilage 2014; 22: 706-709.
- Molloy ES, Morgan MP, Doherty GA, et al. Microsomal prostaglandin E2 synthase 1 expression in basic calcium phosphate crystal-stimulated fibroblasts: role of prostaglandin E2 and the EP4 receptor. Osteoarthritis Cartilage. 2009; 17: 686-692.
- Uhthoff HK, Loehr JW. Calcific tendinopathy of the rotator cuff: pathogenesis, diagnosis and management. J Am Acad Orthop Surg. 1997; 5: 183-191.
- Hodgson RJ, O’Connor PJ, Grainger AJ. Tendon and ligament imaging. Br J Radiol. 2012; 85: 1157-1172.
- Fam AG, Rubenstein J. Hydroxyapatite pseudopodagra. A syndrome of young women. Arthritis Rheum. 1989; 32: 741-747.
