1Department of Cardiology, Castle Hill Hospital, UK
2Department of Pathology, Scarborough General Hospital, UK
3Department of Gastroenterology, Scarborough General Hospital, UK
*Corresponding author:Mohammad Waleed, Department of Cardiology, Castle Hill Hospital, Hull. HU16 5JQ, UK
Received: October 01, 2014; Accepted: October 24, 2014; Published: October 27, 2014
Citation: Waleed M, Raza A, Elhag AM and Saraj O. Bland Cholestasis and Bilirubinostasis: Rare Etiology. Austin J Gastroenterol. 2014;1(5): 1024. ISSN:2381-9219
Anabolic steroids use has been increased in the last decades mostly among young group of population including prisoners, weightlifters, bodybuilders and athletes. Use of anabolic steroids can cause liver damage, acute pancreatitis and acute kidney injury. It is of utmost clinical importance to consider the use of anabolic steroids in young patients with non-specific presentations and abnormal liver functions tests as, missing this fact can lead to the detrimental progressive liver injury. Also clinician needs to be aware of the various formulations of anabolic steroids available these days.
Keywords: Anabolic steroids; Jaundice; Hepatitis; Chronic liver disease; Cirrhosis
A 24 year old patient presented with painless yellow discoloration of skin and eyes in the past four days, noticed by the work colleagues. He also complained of on and off dark colour urine and pale stools for the last 2 weeks. For the past three months he increased exercise and visiting gym five times a week. There was a history of some weight loss, but, he used protein drinks and an OTC (over-the-counter) anabolic steroid to build muscles. He stopped taking the anabolic steroid three weeks ago. He denies any IV drugs use and has no any transfusions in the past. No recent illness or other infections. No recent contact with known hepatitis. He travelled to Canada four months ago. Past medical and family history was unremarkable. He is heterosexual with no male partners. He is a binge drinker, with almost 22 units on Saturday nights, but, no drinks on week days.
On initial assessment temperature 37.1 0 C, blood pressure 140/90mm Hg, heart rate 95bpm, respiratory rate 16 with 98 % saturation on pulse-oximetry. General physical examination showed overweight patient with yellow skin and sclera, no lymphadenopathy, no tattoos and no stigmata/evidence of chronic liver disease. Cardio respiratory, abdominal and neurological examinations were unremarkable.
Blood tests are summarised in Table 1.1. Dipstick for urine was negative for urobilinogen, red blood cells, bilirubin, proteins, glucose and white blood cells.
Ultrasound of the abdomen showed normal appearance of the liver. Portal venous flow is ante grade. No evidence of biliary obstruction. The gallbladder was contracted (patient said he has starved) but no evidence of calculi. The common bile duct was not dilated. Normal appearance of the kidneys and spleen. The pancreas was not visualized due to overlying bowel gas but no obvious abnormality seen.
Magnetic Resonance Cholangio-Pancreatography (MRCP) showed normal gallbladder, common bile duct and the biliary system. No evidence of calculi or obstruction. Pancreas and pancreatic duct were normal.
Liver biopsy showed cholestasis mostly perivenular. Some of the portal tracts showed slight expansion by a minimal increase in chronic inflammatory cells and a slight increase in bile duct profiles. The infiltrate includes lymphocytes and plasma cells, and there are neutrophils associated with the cholangioles. Native bile ducts are normal. There is no periductal fibrosis and there are no portal granulomas (Figure 1). In the parenchyma there is moderate degree of bilirubinostasis within hepatocytes and canaliculi (Figure 2 and 3). There is no evidence of confluent necrosis. A Periodic-Acid Schiff (PAS) stain shows small numbers PAS-positive Kupffer cells in area showing bilirubinostasis (Figure 3). Connective tissue stain shows no evidence of increased portal fibrosis or of bridging fibrosis. Special stains for iron deposition and for copper associated protein are negative. The appearances are considered to be within the spectrum of appearances seen in bland cholestasis secondary to anabolic steroid use. Patient was informed about the abnormal liver function tests and the histo-pathological changes due to anabolic steroid use and advised about complete abstinence from anabolic steroids use in future. Patient was reviewed in clinic after few weeks and blood tests showed normal liver functions.
Anabolic steroids used by the athletes have been very common for decades to increase their performance [1]. Nowadays, the use of anabolic steroids is also found in other young groups of people like prison populations, bodybuilders and weight lifters. In United Kingdom, according to the figures from the Department of Health, 0.2 % of young people had tried anabolic steroids in 2001-2004 and 0.5 % in 2006 [2].
Androgenic anabolic steroids are available in various types and formulations, but, it is the carbon-17-alkylated anabolic steroids, such as methandrostenolone and methyl testosterone- that are more hepatotoxic [3].
In our case, the young patient has also used methandrostenolone for body building. Methandrostenolone (Dianabol) was first introduced as an anabolic steroid by Ciba in the 1960s [4]. Methandrostenolone has various adverse effects common to anabolic steroids, but, very few cases has been reported as methandrostenolone to cause cholestasis and clinical jaundice [5]. A Canadian case report has reported the occurrence of cholestasic jaundice, acute pancreatitis and acute injury simultaneously [4].
In conclusion, it is very important to consider about the use of anabolic steroids in young patients with non-specific presentation and abnormal liver functions, so that its further use can be stopped and prevent progressive liver injury. Patients should be followed up in clinic after stopping the use of anabolic steroids with repeat liver function tests.
Blood test results.
PARAMETER |
VALUES |
PARAMETER |
VALUES
|
Haemoglobin |
13.8 g/dl |
International normalization ratio (INR) |
1.0 |
White cell count |
6.8 x 109/L |
Prothrombin time (PT) |
11.9 seconds |
Platelets |
269 x 109/L |
Activated partial thromboplastin time (APTT) |
26.3 seconds |
|
|
|
|
Sodium |
138mmol/L |
Aspartate transaminase (AST) |
48 IU/L |
Potassium |
4.2mmol/L |
Alanine transaminase (ALT) |
161 IU/L |
Urea |
3.2mmol/L |
Alkaline phosphatase (ALP) |
90 IU/L |
Creatinine |
|
Albumin |
42 g/L |
|
|
Total Bilirubin |
247umol/L |
|
|
Conjugated bilirubin |
238 umol/L |
|
|
|
|
Serum electrophoresis |
No paraproteins |
Hepatitis A IgM antibodies |
Not detected |
Serum IgA level |
1.94 g/L (0.80-2.80) |
Hepatitis B surface antigen (HBsAg) |
Not detected |
Serum IgG level |
12.7 g/L (5.3-16.1) |
Hepatitis C antibody (anti- HCV) |
Not detected |
Serum IgM level |
1.04 g/L (0.50-1.90) |
Paul Bunnell test |
Negative |
|
|
|
|
Amylase |
34 u/L |
Alpha1 anti-trypsin |
1.8 g/L (1.1-2.1 g/L) |
Serum iron |
9.2 umol/L |
serum alpha-fetoprotein |
0.8ku/L (< 7.0) |
Serum ferritin |
365 ug/L |
|
|
Serum B12 |
640 ng/L |
|
|
Serum folate |
8.6 ug/L |
|
|
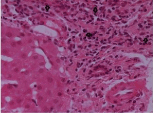
A portal tract showing a mild increase in chronic inflammatory cells including lymphocytes and some plasma cells (arrows). There is no bile duct damage, bile duct inflammation, portal granulomata or interface hepatitis. There is no increase in fibrous tissue.
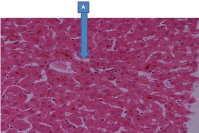
There is a moderate degree of cholestasis mainly within biliary canaliculi (A).
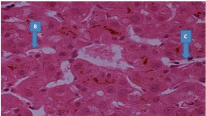
Cholestasis/ bilirubinostasis also seen within hepatocytes (B) and some Kuppffer Cells (C).