
Special Article - Current Endoscopic Therapy in Japan
Austin J Gastroenterol. 2015;2(2): 1037.
Endoscopic Submucosal Dissection for Colorectal Tumors in the Dentate Line Area and Those Adjacent to the Dentate Line
Satohiro Matsumoto* and Yukio Yoshida
Department of Gastroenterology, Saitama Medical Center, Jichi Medical University, Japan
*Corresponding author: Satohiro Matsumoto, Department of Gastroenterology, Saitama Medical Center, Jichi Medical University, 1-847 Amanuma, Omiya, Saitama, Saitama 330-8503, Japan
Received: December 19, 2014; Accepted: February 23, 2015; Published: February 25, 2015
Abstract
Colorectal Endoscopic Submucosal Dissection (ESD) is technically more difficult, as compared to gastric ESD, and a higher incidence of associated accidental events still poses a great concern. The mainstay of treatment for tumors in the bowel region from the rectum to the anal canal is shifting from surgery to ESD. ESD for a lesion in the dentate line area differs from that for common colorectal lesions in terms of anatomic characteristics and attention must be paid to some points in particular. At the time of incision of the anal side of the lesion, because the orientation may be difficult to determine, the visual field should be expanded using an attachment. In order to prevent bleeding, care should be taken to prevent deep incision on the anal side of the lesion so as to avoid damage to the venous plexus. Intraprocedural pain should be sufficiently controlled by local or intravenous injection of anesthetics.
Keywords: Endoscopic submucosal dissection; Colorectal tumors; Dentate line
Abbreviations
ESD: Endoscopic Submucosal Dissection; TEM: Transanal Endoscopic Microsurgery; ST: Small-Caliber-Tip Transparent
Introduction
Colorectal Endoscopic Submucosal Dissection (ESD) for the treatment of colorectal tumors measuring 20 to 50 mm in diameter, which is covered by the national health insurance system, has come into widespread use in Japan [1-6]. However, as compared to gastric ESD, colorectal ESD is technically more difficult and is associated with a higher risk of accidental events, which still raises concerns about its use. The therapeutic strategies for tumors between the rectum and anal canal are shifting. For lesions in the upper part of rectum that are difficult to treat by endoscopic procedures, transanal surgery and Transanal Endoscopic Microsurgery (TEM) used to be performed, whereas nowadays, ESD is becoming the mainstay of treatment for tumors between the rectum and the anal canal.
Anatomy of the anal area
The anus is the terminal part of the gastrointestinal tract, and consists of the anal verge and the anal canal, which extends 3–4 cm medially from the anal verge. The dentate line is the border between the anal epithelium and rectal mucosa, and is located approximately 2 cm proximal from the anal verge. The portion from the dentate line to the anal verge, which is abundantly supplied by sensory neurons, is highly sensitive to pain, whereas the portion extending upward from the dentate line, which contains no sensory neurons, is insensitive to pain and is associated with physiological functions, mainly defecation. The superior rectal venous plexus is located above the dentate line and corresponds to the site of internal hemorrhoids. The inferior rectal venous plexus is located below the dentate line and corresponds to the site of external hemorrhoids. Therefore, in performing ESD for lesions in the dentate line area, measures against pain and bleeding are important.
ESD techniques for lesions in the dentate line area and those proximal to the dentate line
For lesions in the dentate line area, use of appropriate therapeutic strategies is the key (Figure 1a). Handling of the portion at the oral side of the lesion is relatively easy under the inverted view of the endoscope, whereas that of the portion at the anal side is slightly difficult. Thus, the anal side of the lesion should be incised first and detached (Figure 1b). In some cases, even the dentate line area can be visualized with the inverted view of the endoscope; in such cases, the anal side of the lesion is incised under the inverted view. When incision under this condition is difficult, both ends of the anal side of the lesion are incised under the inverted view of the endoscope, and the incision lines at the ends are used to guide the incision of the anal side of the lesion under the look-down view. In order to prevent damage to the venous plexus, caution is needed against deep incision of the anal side of the lesion (Figure 1c). Then, the anal side of the lesion is detached under the look-down view (Figure 1d). Because the lumen is narrow, the visual field is usually expanded using a shorttype, Small-Caliber-Tip Transparent (ST) hood (Fujifilm Medical Co., Tokyo, Japan) when the anal side is detached. Sensory neurons are distributed in the region from the dentate line to the anal verge. Because incision and detachment in this area cause pain, lidocaine (1% Xylocaine, AstraZeneca, Tokyo, Japan) is locally injected as a local anesthetic. When the portion above the dentate line is treated, sodium hyaluronate (MucoUp: Seikagaku Co., Tokyo, Japan) is locally injected, and the anal side of the lesion is detached. After this portion of the lesion is sufficiently detached, the oral side of the lesion is incised and detached under the inverted view of the endoscope. The lesion is then detached from the oral side to the detached anal side, and is completely removed (Figure 1e & 1f). While coagulation of exposed blood vessels at the ulcer base is performed with Coagrasper (FD-410LR; Olympus Medical Systems Co., Tokyo, Japan), a monopolar type of hemostatic forceps, caution is needed against excessive cauterization. In general, reefing of the wound with a clip is not performed.
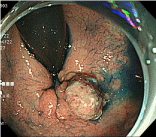
Figure 1a: Chromoendoscopic images.
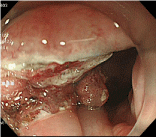
Figure 1: Incision of the anal side of the lesion under the look-down view.
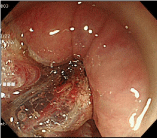
Figure 1c: Incision should be shallow to avoid damage to the venous plexus.
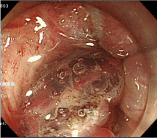
Figure 1d: After the visual field is sufficiently expanded by the ST hood, the anal side of the lesion is detached.
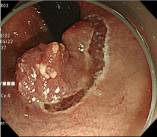
Figure 1e: Incision and detachment of the oral side of the lesion under the
inverted view.
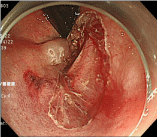
Figure 1f: Wound after complete resection.
Discussion
Transanal surgery and TEM are more invasive and associated with higher recurrence rates, as compared to ESD [7,8]. Moreover, in cases of tumors in the anorectal area, surgery may result in bladder and rectal disturbance or anastomotic leak, and a stoma may be permanently needed after surgery; thus, the merits of endoscopic treatment are obvious. However, we consider that ESD in the dentate line area should be performed by operators with sufficient knowledge of the anatomy of the perianal area and abundant experience in the performance of ESD. The special techniques for ESD of lesions in the dentate line area and those adjacent to the dentate line are as follows: 1) at the time of incision of the anal side of the lesion, because the orientation may be difficult to determine, the visual field should be expanded using a ST hood; 2) caution should be exercised against deep incision of the anal side of the lesion to avoid damage to the venous plexus; 3) intraprocedural pain should be sufficiently controlled by local or intravenous injection of anesthetics.
Conclusion
For ESD of lesions in the dentate line area and those adjacent to the dentate line, use of appropriate therapeutic techniques is especially important, and measures against pain and control of bleeding on account of the abundant nerve and blood supply are required.
References
- Yamazaki K, Saito Y, Fukuzawa M. Endoscopic submucosal dissection of a large laterally spreading tumor in the rectum is a minimally invasive treatment. Clin Gastroenterol Hepatol. 2008; 6: e5–e6.
- Tamegai Y, Saito Y, Masaki N, Hinohara C, Oshima T, Kogure E, et al. Endoscopic submucosal dissection: A safe technique for colorectal tumors. Endoscopy. 2007; 39: 418–422.
- Toyonaga T, Man-i M, Chinzei R, Takada N, Iwata Y, Morita Y, et al. Endoscopic treatment for early stage colorectal tumors: The comparison between EMR with small incision, simpli?ed ESD, and ESD using the standard ?ush knife and the ball tipped ?ush knife. Acta Chir Iugosl. 2010; 57: 41–46.
- Hotta K, Yamaguchi Y, Saito Y, Takao T, Ono H. Current opinions for endoscopic submucosal dissection for colorectal tumors from our experiences: Indications, technical aspects and complications. Dig Endosc. 2012; 24: 110–116.
- Tajika M, Niwa Y, Bhatia V, Kondo S, Tanaka T, Mizuno N, et al. Comparison of endoscopic submucosal dissection and endoscopic mucosal resection for large colorectal tumors. European journal of gastroenterology & hepatology. 2011; 23: 1042–1049.
- Kobayashi N, Yoshitake N, Hirahara Y, Konishi J, Saito Y, Matsuda T, et al. Matched case-control study comparing endoscopic submucosal dissection and endoscopic mucosal resection for colorectal tumors. J Gastroenterol Hepatol. 2012; 27: 728–733.
- Kiriyama S, Saito Y, Matsuda T, Nakajima T, Mashimo Y, Joeng HK, et al. Comparing endoscopic submucosal dissection with transanal resection for non-invasive rectal tumor: A retrospective study. J Gastroenterol Hepatol. 2011; 26: 1028–1033.
- Park SU, Min YW, Shin JU, Choi JH, Kim YH, Kim JJ, et al. Endoscopic submucosal dissection or transanal endoscopic microsurgery for nonpolypoid rectal high grade dysplasia and submucosa-invading rectal cancer. Endoscopy. 2012; 44: 1031–1036.