
Clinical Image
Austin J Gastroenterol. 2015; 2(5): 1050.
Choledochoduodenal Fistula in a Young Patient of Peptic Ulcer Disease
Gyanendu Kumar*
Department of Gastroenterology, S M S Medical College and Hospital, India
*Corresponding author: Gyanendu Kumar, Department of Gastroenterology, S M S Medical College and Hospital, J L N Marg, Jaipur, Rajasthan, India
Received: May 30, 2015; Accepted: September 04, 2015; Published: September 05, 2015
Clinical Image
A 22 years young boy presented with complaints of pain upper abdomen for 6 months and fever for 1 month. Pain is colicky, moderate to severe in intensity and associated with episodes of non bilious, non projectile vomiting. There is no stale food in vomitus, no ball of wind formation or abdominal distension. Fever is intermittent, high grade associated with chills and rigors and increased pain episodes. There is no radiation of pain, constipation, obstipation or jaundice. He was non alcoholic, non smoker, non-diabetic and without any history of abdominal surgery, but there was history of peptic ulcer disease with endoscopic diagnosis of duodenal ulcer 3 years back. For that patient took prolonged ppi for more than a year and also had anti h.pylori regimen. Before this new onset pain episodes patient was totally pain free for last one and half years.
On examination patient had tachycardia, fever and mild tenderness in his right upper abdomen. Laboratory data showed leucocytosis (12000/cmm) deranged liver function tests with increased ast (61 u/l), alt (134 u/l) and alp (292 u/l) with total and direct bilirubin within normal range. Kidney function tests, serum amylase and lipase were normal. Chest and abdominal x- ray as well as usg abdomen were normal. Ct abdomen showed grossly dilated stomach upto duodenal bulb and air in biliary tree (pneumobilia) (Figure 1).
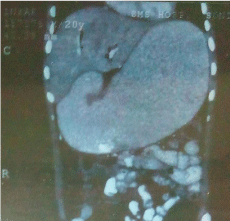
Figure 1: CT abdomen showed grossly dilated stomach upto duodenal Bulb
and Air in Biliary Tree.
Ugi endoscopy showed narrowing at d1-d2 junction and scope not negotiable into d2, d1 showed mucosal irregularity with bubbles of bile coming through it but no evidence of ulcerations (Figure 2).
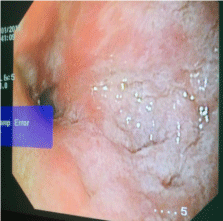
Figure 2: Ugi endoscopy showed narrowing at d1-d2 junction and scope
not negotiable into d2, d1 showed mucosal irregularity with bubbles of bile
coming through it but no evidence of ulcerations.
Barium meal follow through was done and there was reflux of barium into common bile duct with opacification of intra hepatic biliary radicles (Figure 3).
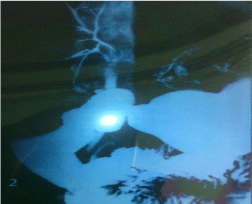
Figure 3: Barium meal follows through was done and there was reflux of
barium into common bile duct with opacification of intra hepatic biliary radicles.
Patient was put on long term ppi therapy and was planned for serial endoscopic dilatation of stricture followed by ercp.
Choledochoduodenal fistulas (cddf) account for 1-25% of bilioenteric fistulas [1]. Although 75-90% of these fistula cases are associated with cholelithiasis [1], only 5-6% of them are associated with duodenal peptic ulcers [2]. Choledochoduodenal fistulas usually occur after peptic ulcer perforation. The first sign of this abnormal biliary-enteric communication may be the presence of air in the biliary tree as seen on x ray of the abdomen or with ultrasound or ct [3].
References
- Misra MC, Grewal H, Kapur BML. Spontaneous Choledochoduodenal fistula complicating peptic ulcer diseas. A case report. Jpn J Surg. 1989; 19: 367-369.
- Iso Y, Yoh R, Okita R, et al. Choledochoduodenal fistula: a rare complication of a penetrated duodenal ulcer. Hepato-Gastroenterol. 1996; 43: 489-491.
- Topai U, Savei G, Sadikoglu MY. Choledochoduodenal fistula secondary to duodenal peptic ulcer. A case report. Acta Radiolologica. 1997; 38: 1007-1009.