
Case Report
Austin J Gastroenterol. 2016; 3(1): 1057.
A Rare Cause of Massive Rectal Bleeding: A Case Report
Sidki I*, Essamri W and Essaid A
Department of Gastroenterology, Mohammed V University, Marocco
*Corresponding author: Imane Sidki, Department of Gastroenterology, CHU Ibn Sina, Mohammed V University, Souissi, Marocco
Received: January 28, 2016; Accepted: March 30, 2016; Published: April 02, 2016
Keywords
Bleeding; Rectal; Vascular
Introduction
Arteriovenous malformation (AVM) of the bowel is known to be an important cause of intestinal bleeding. However AVM in the rectum is even rarer with an incidence of 0.9% to 2.9% of all gastrointestinal AVMs. We report the case of a patient having a rectal arteriovenous malformation.
Case Presentation
A 34 years old women, with no remarkable past, she developed a massive and repeating anal bleeding for 6 years requiring the itératives transfusions, clinically the abdomen is flexible, the rectal examination confirms the presence of red blood in the rectum.
The rate of hemoglobin to the admission is with 3.3g/dl, PQ : 400000 and TP at 100%.
The biological test, the fibrescopy and the ultrasonography with Doppler of the hepatic veins didn’t shows signs of a cirrhosis, a portal hypertension or thrombosis of the mesenteric vein.
Colonoscopic examination showed 3 blues venous cords in the low and middle rectum with internal hémorroïds (Figure 1a,1b).
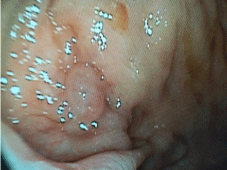
Figure 1a: Text here.
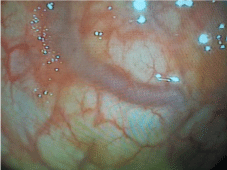
Figure 1b: Text here.
The angioscan Objectified the presence of a parietal vascularization marked in the low and the middle of rectum with a vascular group in the anterior wall of the middle rectum, which is considered like a parietal vascular malformation of the middle rectum (Figure 2a,2b,2c).
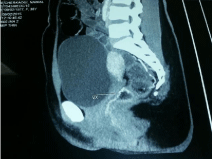
Figure 2a: Text here.
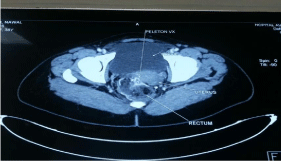
Figure 2b: Text here.

Figure 2c: Text here.
The treatment which was considered is an arterial embolisation with a good clinical evolution marked by the absence of bleeding and the disappearance of the malformation in endoscopy of control.
Discussion
AVM in the gastrointestinal tract has been reported as vascular dysplasia,angiodysplasia and vascular ectasia [1].
It was found in 1.4% to 3% of patients who underwent the colon fibrescopy for an acute or chronic perianal hemorrhage or anemia.
The localization and fréquency of AVMs in the clon and rectum was reported as follows : the ceacum and ascending colon: 54%; the transverse colon: 7%; the descending colon: 7%; the sigmoid colon: 18%, the rectum: 14% [2].
AVMs can be caused by tissue ischaemia secondary to circulatory failure or acquiried vascular degenerative disease associated with aging, since younger patients can develop AVMs, congenital factors are also possible, in addition to acquiered factors or aging factors [3- 8].
To establish the diagnotic of the AVM requires the exclusion of the other causes in particular a portal hypertension during a chronic liver disease, a thrombosis of the portal vein, a cardiac failure or a circulatory failure of the azygos system, by the biological examinations, radiological imagery [2,9].
The venous phase of the selective angiography visualize the origin and the extension of the AVM.
Diverse therapeutic approaches are available, including the medical, endoscopic, surgical treatment or interventional angiography, however no randomized study was able to prove the efficiency of a therapeutic method because of their low incidence [10,11].
However the endoscopic treatment by sclerotherapy or the elastic ligation has an interest at the same time diagnostic and therapeutic in the initial management of the bleeding [3,12] but it is not always applicable and often has undesirable effects potentially grave, such an incomplete obliteration due to toxicity of the sclerosing product calcifying especially in big vessels; consequently an alternative approach should be used. The surgical treatment, in particular a resection of the concerned segment is rarely indicated.
Because the endoscopic and surgical therapeutic approaches have their own limits, the embolisation by angiography is considered as a relatively safe and effective method [3-5,12,13].
The haemostasis by embolization is obtained by obliteration of the principal vein in the AVM, and diverse materials of embolization are used, including reels, Gelfoam, the thrombine, the collagen, autologous blood clot and ethanol [4]. The intestinal ischaemia is the complication dreaded with a rate of occured from 14% to 20% [6], however this method has a therapeutic interest, so facilitating its realization at our patient with a good short and medium-term answer.
Conclusion
The AVM is a rarer vascular disease in the rectum. It should be considered in recurrent rectal bleeding. Colonoscopy and CT angiography are the good methods of diagnostic.
The embolization angiography is considered as an effective and conservative treatment modality.
References
- Nikolopoulos N, Xynos E, Datsakis K, Kasapidis P, Vassilakis JS. Varicosis coli totalis: report of a case of idiopathic aetiology. Digestion. 1990; 47: 232-235.
- Feldman M Sr, Smith VM, Warner CG. Varices of the colon. Report of three cases. JAMA. 1962; 179: 729-730.
- Okada M, Nakashima Y, Kishi T, Matsunaga N, Ishikawa T, Tamesa T et al. Percutaneous transhepatic obliteration for massive variceal rectal bleeding. Emerg Radiol. 2012; 19: 355-358.
- Kochar N, Tripathi D, McAvoy NC, Ireland H, Redhead DN, Hayes PC. Bleeding ectopic varices in cirrhosis: the role of transjugular intrahepatic portosystemic stent shunts. Aliment Pharmacol Ther. 2008; 28: 294–303.
- Krämer SC, Görich J, Rilinger N, Siech M, Aschoff AJ, Vogel J. Embolization for gastrointestinal hemorrhages. Eur Radiol. 2000; 10: 802-805.
- Fishman SJ, Shamberger RC, Fox VL, Burrows PE. Endorectal pull through abates gastrointestinal hemorrhage from colorectal venous malformations. J Pediatr Surg. 2000; 35: 982-984.
- Hayakawa H, Kusagawa M, Takahashi H, Okamura K, Kosaka A, Mizumoto R. Arteriovenous Malformation of the Rectum: Report of a Case. Surg Today. 1998; 28: 1182-1187.
- Boley SJ, Sprayregen S, Sammartano RJ, Adam A, Kleinhans S. Pathophysiologie basis for the angiographie signs of vascular ectasia of the colon. Diagn Radiol. 1997; 125: 615-621.
- Gentilli S, Aronici M, Portigliotti L, Pretato T, Garavoglia M. Idiopathic ileo-colonic varices in a young patient. Updates Surg. 2012; 64: 235-238.
- Katz JA, Rubin RA, Cope C, Holland G, Brass CA. Recurrent bleeding from anorectal varices: successful treatment with a transjugular intrahepatic portosystemic shunt. Am J Gastroenterol 1993; 88: 1104-1107.
- Shibata D, Brophy DP, Gordon FD, Anastopoulos HT, Sentovich SM, Bleday R. Transjugular intrahepatic portosystemic shunt for treatment of bleeding ectopic varices with portal hypertension. Dis Colon Rectum. 1999; 42: 1581-1585.
- Seffinger MA. Our Past, Present and Future are in our hands. J American Osteopath Assoc. 2014; 114: 4-70.
- Almadi MA, Almessabi A, Wong P, Ghali PM, Barkun A. Ectopic varices. Gastrointest Endosc. 2011; 74: 380–388.