
Special Article - Pancreatic Cancer
Austin J Gastroenterol. 2016; 3(2): 1065.
A Case of Pancreatic Hemangioma in Adult which Mimics Adenocarcinoma of the Pancreas
Bratu AM¹*, Zaharia C², Cristian DA², Popa BV³ and Salcianu IA¹
¹Department of Radiology and Medical Imaging Coltea Clinical Hospital, Carol Davila University of Medicine and Pharmacy, Romania
²Department of General Surgery Coltea Clinical Hospital, Carol Davila University of Medicine and Pharmacy, Romania
³Department of Radiology and Medical Imaging Floreasca Clinical Emergency Hospital, Carol Davila University of Medicine and Pharmacy, Romania
*Corresponding author: Bratu AM, Department of Radiology and Medical Imaging, Coltea Clinical Hospital, Carol Davila University of Medicine and Pharmacy, 1 I.C. Bratianu Blvd, Bucharest, Romania
Received: August 08, 2016; Accepted: September 09, 2016; Published: September 13, 2016
Abstract
Pancreatic hemangiomas are benign tumors extremely rare in adults, rarer than in children. Although were reported a small number of pancreatic hemangiomas, mostly were proved to be hyper vascular tumors.
We present the case of a sixty-four years old male who had acute upper abdominal pain, and who was admitted, with the suspicion of acute pancreatitis.
Imagistic examinations detected a tissular nodule in the body of the pancreas, with well- defined margins, without capsule, with heterogeneous structure, and with maximum size of 1.9 cm. Also, it was discovered a similar lesion, regarding the imagistic appearance, in the fourth segment of the liver, and a hemangioma in the sixth segment of the liver. There were no lymphadenopathies in ultrasound and computed tomography exams.
Although was suspected a pancreatic adenocarcinoma with liver metastasis, the patient was planned for surgery, knowing that this type of neoplasia is extremely aggressive with a poor prognosis if is not surgically removed. Histopathological exam indicate that the pancreatic mass was a hemangioma.
Keywords: Pancreatic hemangioma; Pancreatic adenocarcinoma; Computed tomography
Abbreviations
CT: Computed Tomography; LDH: Lactate Dehydrogenase; US: Ultrasonography
Introduction
Pancreatic hemangiomas are benign tumors extremely rare in adults [1,2], rarer than in children [3]. Pancreatic vascular neoplasms, including hemangioma, account for 0.1% of all pancreatic tumors [1]. Only nine cases of adult pancreatic hemangiomas have been reported in literature since 1939 [1].
Most of those who were reported had large sizes, a cystic appearance, and intense contrast enhancement in arterial phase [4] on CT scans.
Hemangiomas tend to undergo proliferation during infancy followed by a period of slow involution lasting several years and eventual regression leaving a fibro-fatty residuum [1]. They may occur in any region of the body but have a predilection for the head, neck and trunk [3]. However, complications due to their size or site may warrant medical or surgical intervention [3].
In terms of clinically, the symptoms are nonspecific, but depending on the tumor location (head, body, tail of pancreas), regardless of its nature, the patient may present suggestive symptoms [5]. Most patients with pancreatic hemangioma present with vague abdominal pain, although one case presented with melena and hematemesis, another with nausea and thrombocytopenia [1,4], and another with recurrent dizziness and palpitations [4].
Case Presentation
Sixty-four years old male was presenting for acute upper abdominal pain. He was admitted, with the suspicion of acute pancreatitis; specific laboratory tests (amylase and lipase) were only slightly increased compared to the upper normal limit. It was continued with laboratory tests, which indicated a value slightly higher than normal of total bilirubin, direct bilirubin, and serum creatinine, but without biological inflammatory signs.
Anamnesis indicated that the patient experienced a weight loss of about 5 kg in the last two months.
Although nonspecific, it was detected an increase in serum LDH, with a value of 658 U/L, the maximum normal value being 618 U/L.
Tumor markers were found to be slightly higher (CA19-9 had a value of 50 u/ml, the upper limit being 40.1 u/ml).
Abdominal ultrasound did not reveal the presence of gallstones, or free or loculated ascites in the upper abdomen. But, US detected a hypoechoic heterogeneous nodule, with hyperechoic areas, relatively well-defined margins, size of 3.2 cm, located on the body of the pancreas. Also, it showed a hypoechoic nodule, also with inhomogeneous structure, in fourth segment of the liver, with sub capsular localization. Withal, US detected a hemangioma, with the size of 1cm, in the sixth segment of the liver.
Upper digestive tract endoscopy did not detect any changes with pathological significance.
Investigations continued with native computed tomography, and two phases post contrast. The equipment used was Siemens Emotion Duo. The acquisition was performed in spiral mode, with contiguous 3 mm-thick section, followed by MPR reconstruction in sagittal and coronal plans. The contrast agent was administered intravenously with the concentration of 370 mg/ml, and the flow used was 3 ml/sec.
Native CT examination showed a nodule in the pancreatic body, hypodense, with well-defined margins, without capsule, with heterogeneous structure, and peripheral micro calcifications (Figure 1). The nodule has a round shape, with maximum diameter of 1.9 cm, it is in the middle of the pancreatic body, and it comes in direct contact but with interface of demarcation with splenic vein. After the contrast administration, the nodule remains hypodense compared to the rest of the pancreatic parenchyma, but presents contrast enhancement (Figure 2). The contrast enhancement of the lesion is progressive and centripetal in venous phase (Figure 3), making the periphery of the nodule to be apparently isodense with pancreatic parenchyma in the late phase (Figure 4). Peripancreatic fat, adjacent to the nodule, is discreetly densified. The nodular lesion from the fourth segment of the liver has the same behavior as pancreatic lesion (Figure 5). There are no lymphadenopathies and vascular structures are normal on CT examination.
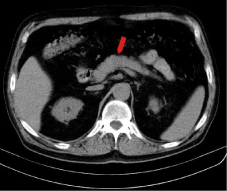
Figure 1: Abdominal native CT: hypodense nodule in the body of pancreas,
with well-defined margins, without capsule, with heterogeneous structure,
and peripheral microcalcifications.
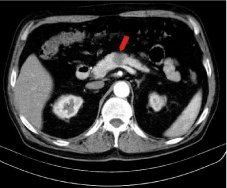
Figure 2: Postcontrast abdominal CT – arterial phase: The pancreatic nodule
remains hypodense from the rest of pancreatic parenchyma but shows
contrast enhancement.
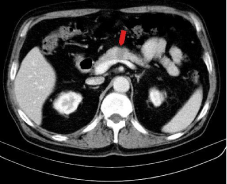
Figure 3: Postcontrast abdominal CT – venous phase: the contrast
enhancement of the nodule is centripetal.
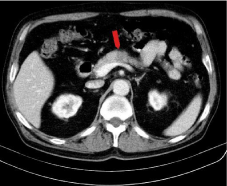
Figure 4: Postcontrast abdominal CT – late phase: the periphery of the
pancreatic nodule becomes isodense with pancreatic parenchyma.
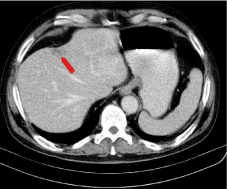
Figure 5: Postcontrast abdominal CT - late phase: liver nodule (fourth
segment) has the same behavior as the pancreatic mass: centripetal contrast
enhancement and the periphery becomes isodense with liver parenchyma.
The size difference of the pancreatic nodule in ultrasound examination and CT scan may be due to the fact that when the echography was performed the lesion presented surrounding edema, and the CT examination was made 10 days after, time during the patient received anti-inflammatory and antispastic medication for abdominal pain.
After surgery, histopathological exam indicate that the mass was a pancreatic hemangioma. After surgical resection of the pancreatic lesion, the patient had suffered peripancreatic bleeding. After the second surgery, the patient’s evolution was favorable.
Discussion
Although were reported a small number of pancreatic hemangiomas, mostly were proved to be hyper vascular tumors, and they were compared with portal cavernoma [6]. Since this is a hyper vascular tumor, the differential diagnosis includes lymphangioma, hemangioendothelioma, hemangiopericytoma, and angiosarcoma [7]. It may also consider neuroendocrine tumors and metastases, but mainly they are invasive on adjacent anatomical structures causing obstruction of the pancreatic duct, since the mass is in the body of the pancreas [6].
Furthermore, of all pancreatic hemangiomas described in the literature, most of them have been found in women [8], but in our case it was a male person.
Naito, et al. [9] reported that CEA and CA 19-9 values were within normal limits, and in our case the value of CA 19-9 was slightly increased than normal maximum value, but this increase was not pathognomonic for a neoplastic lesion.
At the same time, the majority of pancreatic hemangiomas were described as multilocular cystic lesions [10,11,12,13].
Lu and Yang [14] identified pancreatic hemangiomas at contrast-enhanced computed tomography as multilocular cysts with moderately enhanced septa and fluid-fluid levels in the body and tail of the pancreas. In this case, the pancreatic lesion is in terms of density, a tissular mass.
The pancreatic lesion had small dimensions compared to most pancreatic hemangiomas described in the literature [15]. However, Jarboui, et al. [16] present the case of a patient who had a small pancreatic nodule, with tissue density, and which has been proved to be a hemangioma.
Unlike hemangioma, pancreatic cancer is diagnosed on CT in 97% of cases as a hypodense mass on native scan with low enhancement, or isodense on native CT and poor enhancement [17].
When tumor sizes are smaller than 2 cm and is limited to the pancreas, with lymph nodes or parenchymal metastasis most likely nonexistent, it is a T1 tumor stage [18]. However even at these dimensions are not excluded organ metastases. According to Lu and Yang [14] pancreatic hemangiomas range in size from 3 cm to 20 cm, and are most frequently located in the pancreatic head, and the diagnosis of pancreatic hemangioma should not be ruled out solely based on poor arterial phase enhancement on contrast-enhanced CT. In our case, there was in the liver a sub capsular lesion with the same CT behavior as the pancreatic lesion, excluding of course the liver lesion which was clearly a hemangioma. This raised the question: is it a pancreatic cancer with liver metastasis? According to statistics, was the most likely variant. But taken out of context, the pancreatic lesion had a benign behavior (dimensions, shapes). The presence of peripheral tumor calcifications with dimensions under 1mm are considered to be rare, being more common in solid pseudo papillary tumor that have a low degree of malignancy [19], but this type of tumor is also cystic [20]. Also, Weidenfeld [21] describes the case of a small pancreatic hemangioma with the presence of micro calcifications.
Although there was a liver lesion with uncertain CT features, due to the small size of the pancreatic tumor, the lack of invasion of vascular structures and its well defined margins, the patient was planned for surgery, knowing that the pancreatic adenocarcinoma is extremely aggressive with a poor prognosis if is not surgically removed [22]. Another argument favorable for surgery was the post contrast behavior of the pancreatic lesion, namely progressive centripetal enhancement, which is not common for adenocarcinomas, but rather for hemangiomas.
References
- Mundinger GS, Gust S, Micchelli ST, Fishman EK, Hruban RH, Wolfgang CL. Adult pancreatic hemangioma: case report and literature review. Gastroenterol Res Pract. 2009; 2009: 839730.
- Le Borgne J, de Calan L, Partensky C. Cystadenomas and cystadenocarcinomas of the pancreas: a multiinstitutional retrospective study of 398 cases. French Surgical Association. Ann Surg. 1999; 230: 152-161.
- England RJ, Woodley H, Cullinane C, McClean P, Walker J, Stringer MD. Pediatric pancreatic hemangioma: a case report and literature review. JOP. 2006; 7: 496-501.
- Lee J, Raman K, Sachithanandan S. Pancreatic hemangioma mimicking a malignant pancreatic cyst. Gastrointest Endosc. 2011; 73: 174-176.
- Kersting S, Janot MS, Munding J, Suelberg D, Tannapfel A, Chromik AM, et al. Rare solid tumors of the pancreas as differential diagnosis of pancreatic adenocarcinoma. JOP. 2012; 13: 268-277.
- Plank C, Niederle B, Ba-Ssalamah A, Schima W. Pancreatic hemangioma: Imaging features with contrast-enhanced CT and with gadolinium- and mangafodipir-enhanced MRI. Eur J Radiol Extra. 2006; 57: 59-62.
- Karaosmanoglu AD, Arellano R, Baker G. Case report. Peripancreatic intranodal haemangioma mimicking pancreatic neuroendocrine tumour: imaging and pathological findings. Br J Radiol. 2011; 84: e236-e239.
- Kim SH, Kim JY, Choi JY, Choi YD, Kim KS. Incidental detection of pancreatic hemangioma mimicking a metastatic tumor of renal cell carcinoma. Korean J Hepatobiliary Pancreat Surg. 2016; 20: 93-96.
- Naito Y, Nishida N, Nakamura Y, Torii Y, Yoshikai H, Kawano H, et al. Adult pancreatic hemangioma: A case report. Oncol Lett. 2014; 8: 642-644.
- Schoen FJ. Blood vessels. Kumar V, Fausto N, Abbas A, editors. In: Robbins and Cotran Pathologic Basis of Disease, 7th edition. WB Saunders. 2004; 545-547.
- Lu ZH, Wu M. Unusual features in an adult pancreatic hemangioma: CT and MRI demonstration. Korean J Radiol. 2013; 14: 781-785.
- Mondal U, Henkes N, Henkes D, Rosenkranz L. Cavernous hemangioma of adult pancreas: A case report and literature review. World J Gastroenterol. 2015; 21: 9793-9802.
- Søreide JA, Greve OJ, Gudlaugsson E. Adult pancreatic hemangioma in pregnancy--concerns and considerations of a rare case. BMC Surg. 2015; 15: 119.
- Lu T, Yang C. Rare case of adult pancreatic hemangioma and review of the literature. World J Gastroenterol. 2015; 21: 9228-9232.
- Malik M, Ahmed I, Kurban L. Pancreatic Hemangioma – A Case Report. J Gastroenterol Hepatol Res. 2013; 2: 545-548.
- Jarboui S, Salem A, Gherib BS, Ben Moussa M, Rajhi H, Mnif N, et al. Hemangioma of the pancreas in a 60-year-old woman: a report of a new case. Gastroenterol Clin Biol. 2010; 34: 569-571.
- Diehl SJ, Lehmann KJ, Sadick M, Lachmann R, Georgi M. Pancreatic cancer: value of dual-phase helical CT in assessing resectability. Radiology. 1998; 206: 373-378.
- Edge SB, Compton CC. The American Joint Committee on Cancer: the 7th edition of the AJCC cancer staging manual and the future of TNM. Ann Surg Oncol. 2010; 17: 1471-1474.
- Baek JH, Lee JM, Kim SH, Kim SJ, Kim SH, Lee JY, et al. Small (
- Adsay NV. Cystic neoplasia of the pancreas: pathology and biology. J Gastrointest Surg. 2008; 12: 401-404.
- Weidenfeld J, Zakai BB, Faermann R, Barshack I, Aviel-Ronen S. Hemangioma of pancreas: a rare tumor of adulthood. Isr Med Assoc J. 2011; 13: 512-514.
- Frampas E, Morla O, Regenet N, Eugène T, Dupas B, Meurette G. A solid pancreatic mass: tumour or inflammation? Diagn Interv Imaging. 2013; 94: 741-755.