
Clinical Image
Austin J Gastroenterol. 2016; 3(4): 1071.
Speckled Duodenum – A Rare Case of Pseudomelanosis Duodeni
Omar HA¹*, Siglin S², Qazi B² and Kavin H²
¹Department of Medicine, Advocate Lutheran General Hospital, USA
²Division of Gastroenterology, Advocate Lutheran General Hospital, USA
*Corresponding author: Hina Omar, Department of Medicine, Advocate Lutheran General Hospital, 1775 Dempster Street, Park Ridge, IL 60068, USA
Received: November 16, 2015; Accepted: September 19, 2016; Published: October 06, 2016
Clinical Image
75-year-old ventilator-dependent female with chronic respiratory failure, stroke, gastrostomy tube and a mechanical aortic valve on coumadin presented with anemia secondary to melena. Esophagogastroduodenoscopy [1] performed didn’t reveal the source of bleeding but showed an abnormal speckled brown pigmentation of the duodenal bulb extending down past the second portion (Figure 1). Duodenal biopsies showed chronic inflammation, foveolar metaplasia and Brunner’s gland hyperplasia (Figure 2). Brown pigment in duodenal villous macrophages was negative for iron on Prussian blue stains.
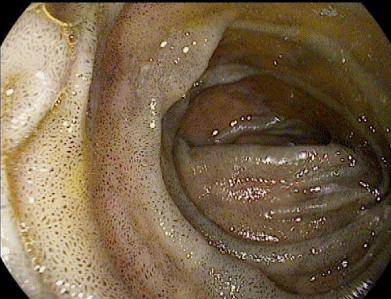
Figure 1: Speckled brown areas of hyperpigmentation in the proximal
duodenum.
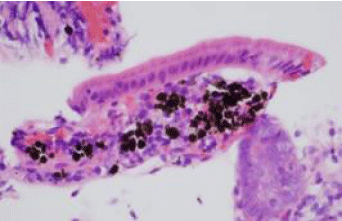
Figure 2: Hematoxylin and eosin stain illustrating macrophages laden with
brown pigment in the lamina propria of duodenal mucosa.
Pseudomelanosis Duodeni (PD) [2] is a rare, benign condition described in 1976 by Bisordi and Kleinman. Endoscopically, it appears as discrete speckled brown or back areas of hyperpigmentation in the duodenal villi, usually in females aged >60 years. Cause is unknown. Histological manifestation is due to deposition of ferrous sulfide pigment in the lysosomes of mucosal macrophages within the lamina propria. PD is more common in patients, with chronic illnesses, as in our patient.
References
- Siderits R, Hazra A, Mikhail N, Chiaffarano J, Lou W, Fyfe B. Endoscopically Identified Pseudomelanosis Duodeni: Striking Yet Harmless. Gastrointest Endosc. 2014; 80: 508-510.
- de Magalhes Costa MH, Fernandes Pegado Mda G, Vargas C, Castro ME, Madi K, Nunes T, et al. Pseudomelanosis duodeni associated with chronic renal failure. World J Gastroenterol. 2012; 18: 1414-1416.