
Special Article - Fall Prevention
Gerontol Geriatr Res. 2016; 2(3): 1018.
Effects of Virtual-Group Exercise at Home (V-GEAH) on Adherence and Fall Risks in Older Adults with a History of Falling
Machiko R. Tomita¹*, Fisher NA¹, Ramsey D², Stanton K¹, Bierdeman L¹, Kocher L³, Saharan S¹, Sridhar R4, Naughton BJ5 and Wilding G6
¹Department of Rehabilitation Science, University at Buffalo, USA
²Department of Health Professions Education, D’Youville College, USA
³Department of Industrial and Systems Engineering, University at Buffalo, USA
4Department of Computer Science and Engineering, University at Buffalo, USA
5Department of Medicine, University at Buffalo, USA
6Department of Biostatistics, University at Buffalo, USA
*Corresponding author: Tomita MR, Department of Rehabilitation Science, University at Buffalo, 505 Kimball Tower, 3435 Main Street, Buffalo, NY 14214, USA
Received: June 03, 2016; Accepted: June 27, 2016; Published: June 28, 2016
Abstract
The objective of this study was to investigate the adherence to and effectiveness of a Virtual-Group Exercise at Home (V-GEAH) program on reducing fall risks in community dwelling older adults, through a randomized controlled trial. Participants were 51 people aged 60-89 years with no cognitive deficits and had a fall within the past year. The intervention was solitary home exercise converted to group exercise at home, utilizing videoconference technology. The program offered progressive resistance and balance exercise 3 times a week for 24 weeks. Participants joined online group sessions using their computer with Internet, interacted with the health research team and exercise peers. Then, they followed an exercise instructor while being monitored for their safety. For72 V-GEAH sessions offered, adherence was excellent (84.0-93.3%) and no one dropped out. The treatment group improved in balance confidence, lower extremity strength (knee extension and flexion, ankle plantarflexion and dorsiflexion, and hip adduction), knee extension (quadriceps) endurance, and basic activities of daily living, more than the control group who were encouraged to walk. The number of falls reported by the treatment group was half of that of the control group. We conclude this video-conference exercise program was instrumental in raising motivation and accountability for continuing exercise, which were attributed to visual contacts with exercise peers and health care providers, easy and clear exercise instruction, gradual progressive exercise program, and participants’ learned computer skills enough to solve problems.
Keywords: Fall risks; Web conference technology; Adherence; Home exercise; Strength; Fear of falling
Abbreviations
V-GEAH: Virtual Group Exercise At Home; RCT: Randomized Controlled Trial; ADL: Activities of Daily Living; ABC: Activity- Specific Balance Confidence; ICC: Intratater Correlation Coefficient; FIM: Functional Independence Measure; GEE: Generalized Estimating Equations
Introduction
One in three community-dwelling older adults fall [1], of whom 22% incur additional falls within a year [2]. Fall related injuries are currently one of the most expensive medical conditions, accounting for 6% of medical expenditures for people 65 years of age and older [3]. Fall injury related health care costs are estimated to increase to $54.9 billion by 2023 in the U.S. alone [4]. Exercise is considered one of the most effective interventions to prevent further falls for older adults who have sustained a fall [5]. However, committing to regular exercise is known to be difficult. Reportedly, 25 to 50% of people who begin an exercise program typically drop out within 6 months and those who complete the programs have low to moderate adherence rates of approximately 66% [6]. Home-based exercise, especially demonstrates poorer adherence rates (≈25%) when compared to gym or a community-based group exercise [7,8], despite the advantages of not having to travel, privacy, flexibility to exercise at one’s convenience, and not being dependent on weather. Yet, poor adherence is primarily attributable to performing exercises alone, the lack of motivation, boredom, and safety concerns [9,10].
One way to improve home exercise adherence is the use of a supportive environment. Advancement in telecommunication systems enable people at home to interact with an exercise instructor in real time via their television screen. A study reported that a group of older adults who participated in a 15-week home-based Tai chi exercise program using DocBox [a] achieved higher adherence rates (69% vs. 38% for home-based exercise without the technology), reduced their number of falls, and improved balance and health measures, all of which were similar to the effects of Tai chi conducted in a community center [8]. Therefore, a virtual, home-based exercise program specifically tailored to older adults will improve adherence to group exercise program. Based on this rationale, the purpose of our study was to utilize commercially available, free of charge videoconference technology to convert long term home-based solitary exercise to group exercise, allowing peer interaction and the monitoring of participants for safety during home exercise. We named this virtual-group exercise at home (V-GEAH) program.
The specific hypotheses were:
1. Participants in the V-GEAH program would show a lower attrition rate (<25%) and a higher adherence rate (>66%) compared to the average of group exercise in past studies.
2. Participants in the V-GEAH program would reduce the number of falls and fall risks such as depression, weakness in lower extremity, and poor gait and balance, and increase balance confidence and function more than the control group.
At the posttest interview, participants evaluated the V-GEAH program using open-ended questions.
Materials and Methods
Development of V-GEAH program
We developed a Virtual-Group Exercise At Home (V-GEAH) program utilizing the internet and videoconferencing technologies. Participants used a desktop or laptop computer with a minimum dual core processor, a high speed connection (download speed =30 mbps), a large monitor (=17”) or a 32” TV screen as a monitor, and a Logitech HD webcam [b]. Each participant exercised at home alone, but was connected with up to six peers and a healthcare research group. A medical doctor’s segmented window was reserved for emergency use so that the participants in need of care and the physician could communicate during an exercise session. We used a video communication service called ooVoo [c] that provides free of charge video chats over the Internet. To use the webcam with multiple chat applications simultaneously, we installed a freeware program called ManyCam [d], and to record all sessions, we used Bandicam [e]. Training on how to use the system was provided in person to each participant, and then all participated in a beta testing (mock exercise session). During the session, if trouble occurred, they could contact ITs in the research group by phones to solve the problem.
Prior to the intervention, a 24-session progressive exercise program was developed and videotaped. The program exercise was for all lower extremity muscle groups, and was designed to allow for rest and recovery of the different muscle groups during each session so as to prevent fatigue. It intended to gradually improve strength and endurance of ankle, knee, and hip muscles, and also improve balance. The instructor was a certified fitness trainer and was familiar with older adults. The exercise program was developed by an exercise physiologist who developed a quantitative progressive exercise method [11], and a geriatric researcher who is knowledgeable about function of older adults with chronic conditions.
The program progressed on several levels: by adding exercise types (flexibility to balance), by intensifying exercises (different levels of Theraband ® [f] to ankle weights), and by increasing the number of repetitions/sets. New exercise types were added every 4 weeks. Within the 4-week interval, the program progressed by increasing repetitions (reps)/sets (1 set of 5 reps, 2 sets of 5, 1 set of 10 and 1 set of 12 reps). Examples of instructions are: (a) In an early stage, “Stand with your hands supported on a steady chair, push up on your toes and hold for 10 seconds and lean back on your heels, raising toes off the floor and hold for 10 seconds”; (2) In a midway stage, “Put appropriate weight directed by the exercise physiologist on each ankle, stand straight holding on to a stable chair, lift your right leg sideways and hold for 5 seconds, then relax, and switch to the other leg. Bring your right leg backwards while keeping knee straight, lift foot slightly off the floor, and do not lean forward and hold for 5 seconds. Switch to the other leg”; (3) in an early to advance stage, “Sit on a chair that is not too low. Keep your feet on the floor slightly apart. Lean forward over your knees; push off with both hands to stand up (for more advanced state, without using hands). When you sit down, don’t flop down; sit in a controlled manner”; and (4) In an advanced stage, “Put your hands on your hips, stand with one leg in front of you as if taking a big step or lunge. Take a giant step with an exaggerated knee bend such that the heel of your back foot comes off of the floor. Then, push back to the starting position with your front foot. Switch legs.”Each session lasted approximately 25 to 40 minutes, depending on the progression. We expected that this program design and progression would result in high compliance and culminate in reducing fall risk factors.
Study design
Human experimentation has been approved by a university Institutional Review Board (#426053-8). The research design was a Randomized Controlled Trial (RCT) with a 24-week intervention period. For the treatment group, four V-GEAH groups consisting of 6 to 7 participants per group started a V-GEAH program in October, January, April, and July to compensate for a seasonal effect. The control group was encouraged to walk inside or outside the home, in accordance with a federal recommendation [12]. Both groups were provided with a pedometer. The assessments were conducted at university labs 3 times: baseline, 12 and 24 weeks.
Participants
The original sample size needed was 50, 25 in each group, based on a power analysis of our previous study with an effect size (d) of .71 [14]. Expecting 20% attrition for the control group and 5% for the treatment group, 74 participants were recruited by a convenience sampling method using newspaper advertisements (Figure 1). Inclusion criteria were community-dwelling people aged 60 to 90 years, who fell in their home environment or a work place within the past year, resulting in a visit to a primary care physician or an emergency department. Exclusion criteria were having neurological disorders including Alzheimer’s disease and Parkinson’s diseases, cognitive impairment and, terminal illness, receiving physical and/or occupational therapy, non-ambulatory, and being scheduled to have any kind of surgery. All participants were required to obtain written permission from their primary care physicians to be in this study. Both groups were equivalent in all baseline variables of demographic characteristics, health status, and exercise behaviors (Table 1).
Variables
Control
M (SD)/ Frequency (%)
Treatment
M (SD)/ Frequency (%)
Differences
Demographic characteristics
Age (years)
74.0 (7.8)
72.3 (7.7)
t=.773 (.443)
Gender
Male
Female
4 (15.4%)
22 (84.6%)
2 (8.0%)
23 (92.0%)
Fisher’s Exact Test
(.668)
Living Status
Alone
With someone
12 (46.2%)
14 (53.8%)
14 (56.0%)
11 (44.0%)
Fisher’s Exact Test
(.579)
Home ownership
Own
Rent
Other
23 (88.5%)
2 (7.7%)
1 (3.8%)
23 (92.0%)
1 (4.0%)
1 (4.0%)
X2= 2.315
(p=.510)
Education
<12 years
High school
2 year college
BS/BA
MA/MS
Doctorate
0
8 (30.8%)
3 (11.5%)
5 (19.2%)
9 (34.6%)
1 (3.8%)
1 (4.0%)
4 (16.0%)
4 (16.0%)
10 (40.0%)
5 (20.0%)
1 (4.0%)
X2= 5.268 (p=.384)
Work status
Full time
Part time
Retired/not working
2 (7.4%)
5 (19.2%)
19 (70.4%)
1 (4.0%)
4 (16.0%)
20 (80.0%)
X2= 0.451 (p=.798)
Income
Very comfortable
Comfortable
Unconformable
Very uncomfortable
7 (26.9%)
13 (50.0%)
5 (19.2%)
1 (3.8%)
4 (16.0%)
17 (68.0%)
4 (16.0%)
X2= 2.444
(p=.486)
Health status
BMI (kg/m2)
26.2 (5.1)
27.4 (4.0)
t=0.953(.345)
Bodily pain
Yes
No
2 (7.7%)
24 (92.3%)
4 (16.0%)
21 (84.0%)
Fisher’s Exact Test
(0.419)
Number of illnesses
3.4 (1.6)
3.7 (2.0)
t=.502 (.618)
Number of medications
3.6 (2.5)
3.8 (3.5)
t=.311 (.757)
Number of medications
that may cause drowsiness
1.2 (1.3)
1.0 (1.7)
t=.443 (.659)
Vitamin D >800IU
Yes
19 (73.1%)
18 (72.0%)
Fisher’s Exact Test
(1.000)
Table 1: Baseline demographic and health characteristics of treatment and control groups at baseline.
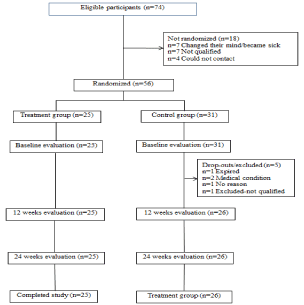
Figure 1: Consort flow diagram.
Measures
Fall risk factors assessed were balance confidence, gait, lower extremity strength and Activities of Daily Living (ADL). Subjective measures for balance confidence used the Activities-Specific Balance Confidence Scale (ABC) [15]. The ABC scale consists of whole numbers from 0% to100% for each of 16 items. The total score is divided by 16 to obtain the ABC score. Scores of 80% or greater are considered high physical functioning, whereas between 50-80% are deemed moderate, and less than 50% are low [16]. A score of less than 67% is indicative of future falls [15]. Depression was measured using the Center for Epidemiologic Studies-Depression. This instrument consists of 20 questions using an ordinal scale (0-3). The total scores range from 0 to 60, with 15 and above indicative of depressive symptoms [17].
Temporal gait parameters were acquired using motion capture techniques, by tracking retroreflective markers affixed to both shoes. Participants ambulated along a walkway at a self-selected pace, and gait velocity was monitored with photoelectric cells (Figure 2). Gait variables exported from Visual 3D software (Visual 3D) [g] included gait speed (m/s), step width (cm), and step length (cm). The mean of three trials and standard deviations for the above measures were used for analyses.
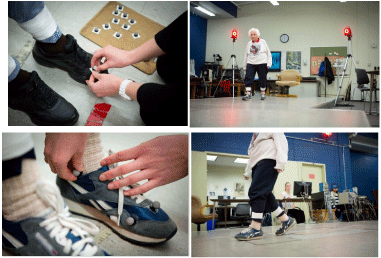
Figure 2: Reflective markers attached to shoes to capture motion for gait analysis.
Maximal voluntary isometric strength of the knee flexor/ extensors, hip flexor/extensors and ab/adductors were measured unilaterally using a strain gauge[h] and a standard exercise bench. A plantar/dorsiflexion force device with strain gauge was used to measure ankle plantar and dorsiflexion strength. The strain gauge quantifies the force of muscle contractions to give a numeric value. Two trials were performed for each leg/muscle group, with the highest force used for the analysis. The participants performed a total of 16 trials for each right and left leg. Participants were instructed to exert maximal isometric muscle force for 2-3 seconds in various positions depending on the muscle group being tested. Two trials were performed to measure strength.
Knee flexion (hamstrings) and endurance was measured by performing a maximal voluntary isometric contraction for 90 seconds or until fatigue was noticed or expressed. Endurance was calculated as the area under the fatigue curve. Participants were instructed not to perform a Valsalva maneuver during these tests.
The psychometrics of the equipment was established in the current study. The interrater and test-retest reliability for the standard exercise bench and strain gauge ranged from fair to excellent (Intrarater Correlation Coefficient, ICC, =.74 - .96) and between good and excellent (ICC =.75 - .995), respectively. Test-retest reliability for the plantar/dorsi- flexion force device was excellent (ICC = .91 - .96).
ADL were assessed using the Functional Independence Measure (FIM). The FIM TM contains 18 items composed of 13 motor tasks (eating, grooming, bathing, upper and lower body dressing, toileting, bladder and bowel management, bed to chair transfer, toilet transfer, shower transfer, locomotion and stairs) and 5 cognitive tasks (cognitive comprehension, expression, social interaction, problem, solving, and memory). Tasks are rated on a 7-point ordinal scale ranging from 1 (completely dependent) to 7 (completely independent) [18]. FIM has been mainly utilized for rehab purposes and scores have been validated for people with stroke, various levels of spinal cord injury, traumatic brain injury, and multiple sclerosis [19].
The number of falls was self-recorded in a log and verified by a monthly phone call.
Procedure
Written consent was obtained from all participants and written permission to participate in the study was obtained from their physicians. At the designated time for V-GEAH sessions, the healthcare research team initiated the program allowing predetermined and invited participants to join the ooVoo chat room. Participants talked with peer exercisers and the research team in segmented screens. Thereafter, participants were instructed to enlarge their monitor to a full screen for the exercise instruction. The research team monitored participants for their safety. After the session, again social interaction took place among participants and the research team. If participants wished to make up the missed session, YouTube was made available for them. (Figure 3) shows a monitoring screen in the research center during the session. The progress record was sent to each participant using lay language and figures such as % increase in strength in an e-mail attachment.
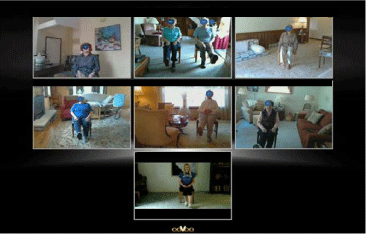
Figure 3: V-GEAH session in progress.
Statistical analysis
For hypothesis 1, the attrition rate was determined by the number of persons who dropped out of the program of the total number of people who were enrolled in the treatment and control groups separately. The adherence rate to the V-GEAH was determined by 2 methods: (1) attendance in 72 scheduled sessions, and (2) attendance in scheduled prescribed exercise sessions plus the number of makeup sessions using YouTube out of 72 total sessions. For hypothesis 2, fall occurrences during the intervention period of the 2 groups were compared using Mann-Whitney Tests. For fall risks, Generalized Estimating Equations (GEE) with a linear model using exchangeable structure for a working correlation matrix was used. First, we examined an interaction between the group orientation and time expressed by Wald chi-square and its p-value. Then, we examined the slopes of the two groups separately. If the result is significant, the group has changed in terms of an outcome measure over time. SPSS 23.0 [i] was used for statistical analyses and the significance level was set at .05 for all primary analyses.
Results and Discussion
Results for hypothesis 1
The attrition rate for the 24-week V-GEAH program was 0% which surpassed 9.1% from the study that utilized telecommunication [8] and a 25% average attrition rate based on the meta-analysis of exercise intervention [20]. The attrition for the control group in this study was 16.1%.
Of the total possible 72 sessions, crude adherence without makeup sessions was 84.4%. The rate was higher when makeup sessions were included, at 93.3%. These results were also better than in the above mentioned telecommunication study (69%) and community-based exercised programs (71%) [8], as well as 66% average adherence to exercise programs found in the meta-analysis of the literature [20]. In our study, only 5 sessions out of a total of 1,872 sessions (25 participants X 3 times/week x 24 weeks) were missed without participants’ prior notice.
Results for hypothesis 2
Over the 24-week study period the treatment group fell 8 times in total and the control group sustained 16 falls, of which difference was significant (Z=1.951, P=.026).
(Table 2) shows changes in fall risks for both groups at 3 separate time points. The results show that balance confidence measured by the ABC and ankle plantarflexion had a significant interaction (p=.015 and p=.007, respectively), indicating the two groups had different slopes over time. Balance confidence level was lower for the treatment group at baseline, but had improved and surpassed the control group. For ankle plantarflexion, the treatment group started a little higher than the control group, and ended up much higher.
Fall risk factors
Group
Baseline
12 weeks
24 weeks
GEE
M (SD)
M (SD)
M (SD)
Interaction & each slope
Balance confidence
Control
85.6 (10.9)
86.0 (9.8)
86.4 (8.9)
.015* .081
Treatment
81.0 (13.4)
83.9 (14.3)
86.7 (10.4)
.001***
Depression
Control
4.4 (4.9)
3.2 (3.6)
2.5 (3.2)
.878 .565
Treatment
5.3 (3.2)
3.6 (5.1)
2.3 (4.5)
.191
Strength
Knee
Control
11.4 (5.2)
12.2 (4.9)
12.9 (5.1)
.240 .474
Quadriceps (kg)
Treatment
13.0 (4.0)
14.8 (5.5)
15.7 (6.2)
.003**
Knee
Control
3.9 (2.6)
4.7 (2.7)
4.7 (2.8)
.100 .292
Hamstring (kg)
Treatment
5.5 (3.0)
6.1 (3.0)
7.2 (3.2)
<.001***
Ankle
Control
8.7 (4.2)
10.7 (3.5)
10.9 (2.9)
007** .560
Plantarflexion (kg)
Treatment
9.3 (4.4)
12.4 (5.4)
14.2 (8.4)
<.001***
Ankle
Control
4.6 (1.8)
4.7 (1.8)
5.4 (2.1)
.373 .625
Dorsiflexion (kg)
Treatment
5.0 (2.8)
5.6 (2.1)
6.2 (2.4)
<.001***
Hip Extension (kg)
Control
7.8 (3.8)
8.2 (3.6)
8.0 (3.0)
.498 .618
Treatment
7.3 (3.9)
8.4 (3.5)
8.1 (3.9)
0.153
Hip Flexion (kg)
Control
11.1 (5.4)
12.1 (4.9)
11.5 (5.5)
.361 .866
Treatment
12.7 (6.9)
12.7 (4.4)
14.4 (4.5)
0.13
Hip Abduction (kg)
Control
5.8 (2.5)
6.4 (2.7)
5.9 (2.3)
.274 .211
Treatment
7.4 (5.1)
7.1 (4.6)
6.6 (2.9)
.266
Hip Adduction (kg)
Control
5.7 (2.4)
6.0 (2.4)
5.9 (2.2)
.174 .600
Treatment
6.2 (2.3)
7.5 (3.1)
7.0 (2.3)
.002**
Endurance
Knee
Control
706.2(348.5)
749.0 (356.2)
814.0(383.5)
.287 .376
Quadriceps (kg.sec)
Treatment
821.4(312.1)
931.6 (303.3)
1002.6 (361.1)
.001***
Knee
Control
166.8(141.3)
199.1(117.8)
205.2 (146.2)
.952 .061
Hamstring (kg.sec)
Treatment
255.3(196.2)
287.2 (190.3)
307.6 (202.6)
.017*
Gait
Speed (m/s)
Control
1.11 (0.25)
1.08 (0.24)
1.09 (0.24)
.081 .305
Treatment
1.07 (0.25)
1.07 (0.25)
1.12 (0.29)
0.125
Step width(cm)
Control
10.6 (2.69)
10.3 (2.69)
10.5 (2.77)
.087 .065
Treatment
11.8 (3.00)
11.5 (3.06)
11.0 (2.67)
.012*
Step length (cm)
Control
59.7 (9.11)
58.9 (9.29)
59.1 (8.75)
.131 .432
Treatment
58.6 (9.29)
58.4 (9.64)
59.7 (10.47)
0.208
Function
FIM Motor
Control
87.7 (3.1)
88.0 (2.8)
87.9 (2.9)
.245 .580
Treatment
87.4(3.0)
88.2 (2.7)
88.2 (2.8)
.024*
FIM Cognition
Control
34.3 (1.0)
34.4 (1.2)
34.3 (1.2)
.509 .842
Treatment
34.2 (0.99)
34.6 (0.91)
34.6 (0.91)
0.071
*p= .05
**p= .01
***p= .001
Table 2: Change in fall risk factors.
Neither group was depressed at all at the 3assessment times, measured by the CES-D.
Regarding temporal spatial gait parameters (speed, step width, and step length,) the control group tended to decline while the treatment group was likely to improve, although without statistical significance except for step width. Walking with feet apart is associated with a way to prevent falls. The treatment group significantly reduced step width at 24 weeks from the baseline (p=.012).
For muscle strength and endurance, knees and ankles showed gradual significant improvements for both groups, but for all items, the treatment group consistently improved more (p<.01 for all but knee hamstring) compared to the control group (p>.05). Strength of hip was not significantly improved except for hip adduction for the treatment group (p=.002).
For function, FIM Motor and FIM Cognition were analyzed separately. The treatment group significantly improved in the motor domain (p=.024).
Results for V-GEAH program evaluation
The program evaluation by participants in open ended questions revealed that the participants perceived that they belonged to a group with common objectives, and they felt safe because experts were always present to support their behaviors (exercise). They felt that exercise instructions were easy to follow because the instructor explained and showed the steps with great clarity and the progress of exercise had the same pattern weekly and monthly. They felt encouraged to continue with their exercise. The reason they continued exercise and reported future absences was that they felt a need to; in other words, they thought that the peer and the research group would wonder about their absence. The reason for the frequent makeup of missed sessions was that they were afraid of not being able to catch up to the next progressive exercise level, if they missed a session. Another benefit of using this internet-based technology was that it enabled participants to attend live group sessions even when they were traveling or out of state, as long as they could access the Internet. However, 5% of participants thought the 6-month duration was very long while 77% said they will definitely miss the V-GEAH session.
Discussion
This study was able to achieve remarkably high adherence to a 24- week home exercise program in community-dwelling older adults, utilizing commercially available web conferencing technology and found the V-GEAH program was more effective to reduce fall risks than walking.
Two issues need to be noted in understanding study results. First is regarding walking. The control group was encouraged to walk in this study. At baseline they walked 3,494 steps/day, at 12 weeks, 4,139 steps/day, and at 24 weeks, 5302 steps/day. The treatment group walked 3,442 steps at baseline, 3,789 steps at 12 weeks, and 4,098 steps at 24 weeks. Therefore, on average, at 12 weeks the control group walked about 700 steps/day more and at 24 weeks 1,300 steps/day more than the treatment group a day. Since the control group increased walking steps they improved in knee and ankle strength but this improvement was not translated to improving balance confidence level or motor function, compared to the V-GEAH group. It was also apparent that having a pedometer was a facilitator of walking for many participants. This was especially true for the control group who were not provided with any other exercise but encouragement of walking. If the control group had walked the usually recommended 10,000 steps/ day, the result would have been different. This recommendation, however, has not been tested and validated for older adults with past falls. The best method is likely to be both types of exercise.
Congruent with the results of a meta-analysis examining the risk of falling in older adults [20] was that ankle strength deficits are associated with falls. In our study, ankle strength for the control group improved by19.6-25.3% by walking and the treatment group improved greater, 24.0 -53%. Therefore, fall prevention specific resistance exercise is more effective for strengthening ankles than walking and this is true for other muscle groups.
In a recent study in Japan, the authors stated that walking may be more effective than balance and leg exercise for fall prevention [21]. Although the conclusions of our study and theirs sound contradictory, it is important to acknowledge that different interventions were provided using the same names. “Walking” in our study was that with usual pace and theirs was brisk walking. For balance and strength exercise, we used quantitative progressive exercise while they used Tai chi and Otago based exercise. The common trait for the both studies was that the treatment group was provided with an intervention with more intensity than the control group. The future study should explore what type of exercise is effective for older adults with which conditions. More study is warranted on this subject.
The second is regarding gait. Temporal-spatial gait parameters tended to decline for the control group, whereas the treatment group progressed, but only stride width had statistical significance. It may be because the way the V-GEAH exercise was structured. We started with strengthening muscles and introduced balance exercise6 weeks later because we assumed strength should be built fast to prevent falls before they can do balance exercise. If balance exercise was introduced at the beginning, the effect may have been more apparent. Observing the rate of improvements in fall risks, it took 24 weeks for the effect of the intervention to be evident for many fall risks. Existing exercise studies do not pay attention to the order of exercise for a long term exercise program but to produce optimal outcomes, this may need to be explored.
Nevertheless, we successfully demonstrated that utilizing commercially available technology can overcome low adherence to a long term home exercise program. As technology continues to evolve, its applications to improve health behaviors become easier and more applicable. At the outset of this 2-year study, only a handful of participant’s had internet accessibility at download speeds more than 10 mbps, whereas stable high speed internet services was not available in some areas. One year later, the majority of new participant’s accessed it at 30 mbps and surrounding areas were covered by competing internet services. Considering only 2% of participants had no prior computer experience in this study, use of technology may no longer be regarded as an unfamiliar territory for communitydwelling older adults.
Videoconferencing technology use can be beneficial as it pertains to illnesses and conditions such as osteoporosis, low back pain, heart failure, hip fractures, end-stage renal disease, and osteoarthritis, all which have low adherence to home-based exercise [22-33]. For operative application of the V-GEAH to these conditions, we summarize important elements. (1) Exercise should be accompanied with patient monitoring by healthcare professionals to secure safety and immediate feedback; (2) Exercise instruction needs to be clear and simple, and its progression should be systematic so that participants can easily understand the pattern; (3) Training of technology use should be provided prior to the initiation of an exercise program so that participants have enough knowledge to solve common problems; (4) Socialization aspect is essential to make sessions interpersonal to develop a group atmosphere, as well as personal to develop accountably for participating in the program; (5) providing a written report of progress using lay language and figures (e.g., %) is important to encourage continuing participation. These are similar to the recent findings in a European study with patients with chronic back pain [34]. (6) Finally, we would like to emphasize the importance of interface, both technological and personal. Technologically, user interface should be intuitive and simple to use. Personally, people whom participants interact in the program (e.g., a research nurse, an exercise instructor, and an IT) should be perceived as caring, likable and/or approachable because the person can facilitate communication to develop a group atmosphere. An interesting situation in the V-GEAH program was that a pet cat of a participant recognized the exercise instructor’s voice and whenever the session was on, she always stayed with the participant; therefore on a monitor, which all peers could see. Her repeated appearance was noticed by the research nurse who decided to make her the exercise group pet. Then, group exercisers found a common topic. The repeated shared experience developed a sense of belonging. Although research literature rarely talks about personal influence in the use of healthcare technology, we recognize the importance of a human factor in terms of health communication to achieve high adherence to an exercise program.
Additionally, it should be reported that even though a screen was reserved during all V-GEAH sessions for a medical doctor in case of emergency, it was not used because an event to require him did not occur. The feature, we think, is an important one.
Limitations
This study may not be generalized to all older adults with past falls due to participants ‘characteristics. Participants in this study were more health conscious than average older adults who do not fall. Due to the convenience sampling method used to recruit participants, people who responded to flyers explaining the study may have been either aware of the importance of exercise, wanted to exercise, or desired to do more exercise. Of the 51 participants, only 1 person (2%) was diagnosed as prediabetic while the remainder was diabetes free. This contradicts the National Diabetes Fact Sheet, 2013, which says that 26.9% of Americans aged 65 years or older are diabetic [35]. If this figure was to be reflective of our sample, it would have been expected that 14 participants would have had diabetes. Therefore, our results may not be generalizable for older adults with diabetes or with other comorbidities. This situation is not unique only to this study. Most studies employing a convenience sampling method have the similar tendency, favoring study outcome. A recruitment method of participants who are both interested and uninterested in a targeted behavior in a study needs to be developed.
Final note is that if the V-GEAH method is used for diagnostic purposes, we advise that video conference technology needs to be maximally secure.
Conclusion
Utilization of web conference technology to convert solitary home-based exercise to group exercise was successful in terms of achieving zero attrition and great adherence to an exercise program, as well as reducing many fall risk factors and the number of falls in older adults with a history of falls.
Acknowledgement
This study was funded by the National Institute of Health; 1 R21 AG041457-01A1.
Suppliers
DocBox. https://www.docboxinc.com/press/20101001.asp.
Logitech HD webcam. https://www.staples.com/Logitech-HDWebcam- C270/product_354562?cid= PS: GooglePLAs:354562&ci_ src=17588969&ci_sku=354562& KPID=354562.
ooVoo. https://www.oovoo.com/home.aspx.
ManyCam. https://www.manycam.com/.
Bandicam. https://bandicam.en.softonic.com/.
Theraband. https://www.thera-band.com/store/products. php?ProductID=26.
Visual 3d. https://www.c0motion.com/products/visual3d/.
Strain gauge LCCA-250. https://www.omega.com.
IBM SPSS. https://www-01.ibm.com/software/analytics/spss/.
References
- Sherrington C, Whitney JC, Lord SR, Herbert RD, Cumming RG, Close JC. Effective exercise for the prevention of falls: a systematic review and metaanalysis. J Am Geriatr Soc. 2008; 56: 2234-2243.
- Shumway-Cook A, Ciol MA, Hoffman J, Dudgeon BJ, Yorkston K, Chan L. Falls in the Medicare population: incidence, associated factors, and impact on health care. Phys Ther. 2009; 89: 324-332.
- Komara FA. The slippery slope: reducing fall risk in older adults. Prim Care. 2005; 32: 683-697.
- Carroll NV, Slattum PW, Cox FM. The cost of falls among the communitydwelling elderly. J Manag Care Pharm. 2005; 11: 307-316.
- Heath JM, Stuart MR. Prescribing exercise for frail elders. J Am Board Fam Pract. 2002; 15: 218-228.
- Allen K, Morey MC. Physical activity and adherence. Bosworth H, editor. In: Improving Patient Treatment Adherence. Springer Science +Business Media LLC. 2010; 9-38.
- Lin MR, Wolf SL, Hwang HF, Gong SY, Chen CY. A randomized, controlled trial of fall prevention programs and quality of life in older fallers. J Am Geriatr Soc. 2007; 55: 499-506.
- Wu G, Keyes L, Callas P, Ren X, Bookchin B. Comparison of telecommunication, community, and home-based Tai Chi exercise programs on compliance and effectiveness in elders at risk for falls. Arch Phys Med Rehabil. 2010; 91: 849-856.
- Boyd R, Stevens JA. Falls and fear of falling: burden, beliefs and behaviours. Age Ageing. 2009; 38: 423-428.
- Friedman SM, Munoz B, West SK, Rubin GS, Fried LP. Falls and fear of falling: which comes first? A longitudinal prediction model suggests strategies for primary and secondary prevention. J Am Geriatr Soc. 2002; 50: 1329- 1335.
- Fisher NM, Pendergast DR. Application of quantitative and progressive exercise rehabilitation to patients with osteoarthritis of the knee. J Back Musculoskelet Rehabil. 1995; 5: 33-53.
- Centers for Disease Control and Prevention. Take a stand on falls.
- Tomita MR, Tsai BM, Fisher NM, Kumar NA, Wilding G, Stanton K, et al. Effects of Multidisciplinary Internet-based Program on Management of Heart Failure. Journal of Multidisciplinary Healthcare. 2009; 2: 13-21.
- Powell LE, Myers AM. The Activities-specific Balance Confidence (ABC) Scale. J Gerontol A Biol Sci Med Sci. 1995; 50A: M28-34.
- Myers AM, Fletcher PC, Myers AH, Sherk W. Discriminative and evaluative properties of the activities-specific balance confidence (ABC) scale. J Gerontol A Biol Sci Med Sci. 1998; 53: M287-294.
- Lajoie Y, Gallagher SP. Predicting falls within the elderly community: comparison of postural sway, reaction time, the Berg balance scale and the Activities-specific Balance Confidence (ABC) scale for comparing fallers and non-fallers. Arch Gerontol Geriatr. 2004; 38: 11-26.
- Radloff, LS. The CES-D Scale, A self-report depression scale for research in the general population. ApplPsychol Meas. 1977; 1: 385-401.
- The FIM Instrument. https://www.udsmr.org/.
- Rehab Measures: Functional Independence Measure. https://www. rehabmeasures.org/Lists/RehabMeasures/DispForm.aspx?ID=889.
- Schwenk M, Jordan ED, Honarvararaghi B, Mohler J, Armstrong DG, Najafi B. Effectiveness of foot and ankle exercise programs on reducing the risk of falling in older adults: a systematic review and meta-analysis of randomized controlled trials. J Am Podiatr Med Assoc. 2013; 103: 534-547.
- Okubo Y, Osuka Y, Jung S, Rafael F, Tsujimoto T. Walking can be more effective than balance training in fall prevention among community-dwelling older adults. Geriatr Gerontol Int. 2015.
- Miller KK. Adherence with Home Exercise Programs 1-6 months after Discharge from Physical Therapy by Individuals Post-stroke [thesis]. Indiana University, Indianapolis, IN: 2008; 24.
- Kolt GS, McEvoy JF. Adherence to rehabilitation in patients with low back pain. Man Ther. 2003; 8: 110-116.
- Iversen MD, Fossel AH, Katz JN. Enhancing function in older adults with chronic low back pain: a pilot study of endurance training. Arch Phys Med Rehabil. 2003; 84: 1324-1331.
- Medina-Mirapeix F, Escolar-Reina P, Gascon-Canovas JJ, Montilla-Herrador J, Collins SM. Personal Characteristics Influencing Patients’ Adherence to Home Exercise During Chronic Pain: a Qualitative Study. J Rehabil Med. Apr 2009; 41: 347-352.
- Milroy P, O’Neil G. Factors Affecting Compliance to Chiropractic Prescribed Home Exercise: a Review of the Literature. J Can Chiropr Assoc. 2000; 44:141-148.
- Forkan R, Pumper B, Smyth N, Wirkkala H, Ciol MA, Shumway-Cook A. Exercise adherence following physical therapy intervention in older adults with impaired balance. Phys Ther. 2006; 86: 401-410.
- Iversen MD. Physical Therapy for Older Adults with Arthritis: What is Recommended?. Int. J. Clin. Rheumatol. 2010; 5: 37-51.
- Marks R, Allegrante JP. Chronic osteoarthritis and adherence to exercise: a review of the literature. J Aging Phys Act. 2005; 13: 434-460.
- Pisters MF, Veenhof C, van Meeteren NL, Ostelo RW, de Bakker DH, Schellevis FG, et al. Long-term effectiveness of exercise therapy in patients with osteoarthritis of the hip or knee: a systematic review. Arthritis Rheum. 2007; 57: 1245-1253.
- Roddy E, Zhang W, Doherty M, Arden NK, Barlow J, Birrell F, et al. Evidencebased recommendations for the role of exercise in the management of osteoarthritis of the hip or knee--the MOVE consensus. Rheumatology (Oxford). 2005; 44: 67-73.
- Ling KW, Wong FS, Chan WK, Chan SY, Chan EP, Cheng YL, et al. Effect of a home exercise program based on tai chi in patients with end-stage renal disease. Perit Dial Int. 2003; 23 Suppl 2: S99-99S103.
- Schechter CB, Walker EA. Improving Adherence to Diabetes Selfmanagement Recommendations. Diabetes Spectrum. 2002; 15: 170-175.
- Palazzo C, Klinger E, Dorner V, Kadri A, Thierry O, Boumenir Y, et al. Barriers to home-based exercise program adherence with chronic low back pain: Patient expectations regarding new technologies. Ann Phys Rehabil Med. 2016; 59: 107-113.
- Centers for Disease Control. National Diabetes Fact Sheet, 2013. https://www. cdc.gov/diabetes/pubs/factsheet11/fastfacts.htm.