
Special Article - Geriatric Medicine
Gerontol Geriatr Res. 2016; 2(4): 1022.
Improved Survival in Patients Older than 80 Years with Multiple Rib Fractures: Impact of Geriatric Trauma Co- Management
Singh M¹*, Butterfield K², Monteiro JFG³, George A4, Heffernan DS4, Mc Nicoll L³ and Gravenstein S1,3
¹Department of Internal Medicine, School of Medicine at Case Western Reserve University, USA
²Pharmacy Quality Alliance, USA
³Department of Medicine, Rhode Island Hospital, USA
4Department of Surgery, Warren Alpert School of Medicine at Brown University, USA
*Corresponding author: Mriganka Singh, Division of Geriatric Medicine, University Hospitals Cleveland Medical Center, UH Hanna House B-15 11100 Euclid Avenue, Mailstop: HAN6095 Cleveland,OH-44106
Received: August 17, 2016; Accepted: October 14, 2016; Published: October 17, 2016
Abstract
Traumatic rib fractures in the elderly result in significant adverse outcomes. Geriatric co-management programs have been proven effective in hip fracture patients but there are no studies in traumatic multiple rib fracture patients.
Objectives: To compare outcomes, particularly overall mortality, in older trauma patients with multiple rib fractures in a Geriatric Trauma Co-Management (GTC) program versus usual care.
Design: A retrospective cohort study.
Setting: An eleven bed trauma critical care unit within a 719 beds level 1 trauma center.
Participants: Three hundred and ninety five patients aged 65 and older admitted to the trauma service with multiple rib fractures with or without other injuries from September 2012 to November 2014. Among these, 149 (39.0%) received care with GTC.
Measurements: Baseline demographic and outcome measures were obtained from the trauma registry.
Results: Baseline characteristics were similar for both groups except that the GTC patients were older by 3 years, had falls more often as the mechanism of injury, and had greater comorbidities (Charlson of 2.8 vs 2.1). Overall mortality (inpatient and hospice discharge), was lower in the co-management group (8.7%) when compared with usual care (15.0%), (adjusted OR 0.4; p = 0.029), which represented a 41.0% reduction and 9 fewer deaths. Survival differences met significance among patients > 80 and those with lower Injury Severity scores.
Conclusion: Among older trauma patients with multiple rib fractures, survival may be improved with geriatric trauma co-management.
Keywords: Geriatric trauma; Rib fractures; Co-management; Mortality
Introduction
Elderly chest trauma patients have higher mortality and morbidity due to multi-morbidity and limited physiologic reserve [1- 3]. Given the prevalent mechanisms of injury, older patients are more likely to sustain blunt trauma especially in the chest. Rib fractures can be found in about 10% of all trauma patients but the elderly are especially prone to fracturing a rib with an incidence as high as 60 per 100,000 persons per year [4]. There is an associated 12.0% overall mortality and about 33.0% will develop pulmonary complications as shown by a study on trauma patients with rib fractures by Ziegler et al. [5]. However, in the elderly trauma patients with rib fractures, the mortality and thoracic morbidity rates are twice as high compared to younger patients with similar injuries [1]. For each 1-year increase in age over 65, the odds of dying after trauma increases by 6.8% [6]. Each additional rib fracture increases the mortality rate by 19.0% and the risk of pneumonia by 27%1. Preexisting co-morbidities and overall injury severity are known to predict outcomes in the elderly [6,7]. The effect of pre-existing co-morbidities on mortality is most pronounced for patients with four or fewer rib fractures, exhibiting an inverse relationship to the number of rib fractures.
The increasing number of elders in the U.S. is driving the growth in the number of older trauma patients. Previous work has shown that aggressive management of older trauma patients may be justified given positive long term outcomes [8]. Consequently practice management guidelines on geriatric trauma developed by the Eastern Association for the Surgery of Trauma, [9] proposed the following: a lower threshold for trauma activation for injured patients aged 65 years or older who are evaluated at trauma centers, aggressive triage, correction of coagulopathy, and limitation of care when clinical evidence predicts an overwhelming likelihood of poor long-term prognosis.
Geriatric co-management has improved outcomes in elderly hip fracture patients [10] as has a geriatric trauma consultation [11,12]. However, reports on a co-management model for geriatric trauma in general or specifically for geriatric trauma with multiple rib fractures are lacking.
We developed the Geriatric Trauma Co-management (GTC) program based on the principles of comprehensive geriatric assessment and an operational model similar to the geriatric hip fracture program; [13] with the goal of preventing complications related to multi-morbidity and also new onset complications in the acute setting. Our primary specific aim was to compare overall mortality (defined as inpatient mortality and hospice discharges) among patients with multiple rib fractures managed by the GTC program versus usual care. Our secondary aim was to compare secondary outcomes such as length of stay (LOS), discharge disposition and readmission rates among patients with multiple rib fractures managed by the GTC program versus usual care. In addition, we further assessed the impact of age and injury severity on mortality.
Methods
Study design and setting
This was a retrospective cohort study performed in an academic tertiary care 719 bed hospital which was also a certified level I trauma care center managed by a trauma surgery specialty group. Trauma patients with multiple rib fractures are initially managed in the eleven-bed Trauma Intensive Care Unit (TICU) followed by transfer to either a step down unit or general trauma unit. This study was approved with waived consent by the institutional review board of Rhode Island Hospital.
Patient selection
We included patients aged 65 and older with multiple rib fractures with or without other injuries admitted to the trauma service in the trauma intensive care unit from October 2012 to November 2014. Multiple rib fractures were defined as the presence of 2 or more rib fractures. Referral to the GTC was at the discretion of the trauma team. Patient participation was voluntary, thus not all patients meeting this criteria participated in the GTC.
Study procedures
The GTC was headed by a lead geriatrician with a focus on teambased, interdisciplinary care coordination involving nursing, physical therapy, social work and clinical pharmacy. The trauma surgery team decided which patients could benefit from GTC and placed the referral.
Geriatric Trauma Co-management Clinical Intervention: After GTC referral, an initial evaluation was done based on the principles of comprehensive geriatric assessment and the patients were followed daily by the geriatrician addressing common geriatric syndromes (e.g., prevention and management of delirium, evaluation and workup for traumatic falls), medication management, pain management, co-management of co-morbidities (e.g., congestive heart failure, hypertension, renal disease, dementia, lung disease) and managing preventable complications such as delirium and constipation. The trauma surgeons took primary responsibility for surgical and critical care issues such as ventilator management, hemodynamic stability, sepsis, fractures, trauma and surgical wounds. An individualized care plan was developed daily in collaboration with the surgery team.
Usual Care: Trauma patients older than 65 yrs with multiple rib fractures were admitted to the trauma ICU from the trauma bay. In addition to trauma evaluation and management of injuries, the management of comorbidities and medical complications was done by the trauma team.
A geriatric trauma co-management committee was formed, which comprised of geriatricians, a geriatric trauma surgeon, trauma nurses and trauma mid-level providers. The committee met monthly and developed geriatric protocols (bowel and delirium in TICU), as well as geriatric-specific educational resources for resident education. Education on the principles of geriatrics and their application to the clinical setting in trauma care was imparted to the trauma residents by both formal and informal talks. A series of geriatric talks were given as formal didactics year round by geriatric faculty members in addition to informal patient specific bedside teaching during morning rounds and morning report.
Data collection
Data for our study was collected from the trauma registry at a major teaching hospital in New England. Baseline demographic measures included, but were not limited to age, gender, race, functional status, injury mechanism, mean Injury Severity Score (ISS) score, [14,15] Abbreviated Injury Scale (AIS) scores, [15] number of trauma diagnosis and number of comorbidities (cancer, congestive heart failure, diabetes mellitus, hypertension and respiratory diseases). Injury type was classified according to the AIS; the most widely used anatomical injury rating scale [16]. The AIS ranks and compares injuries by severity according to 6 body regions with relative severity ranked on a scale of 1 (minor) to 6 (incompatible with life). The 6 body regions used in the AIS are head, face/neck, chest, abdomen/pelvis, extremities and external. Injury severity was measured by the Injury Severity Score (ISS). Derived from the AIS, the ISS allows comparison of injury severity among heterogeneous injuries. The ISS is the sum of the squares of the highest AIS grades in each of the three most severely injured body regions and the scores range from 1 (least severe) to 75 (most severe). We grouped the ISS scores in the mild to moderate (0-15), severe (16-24) and very severe (=25) ranges [3].
Primary outcome
The primary outcome of overall mortality was defined as death in the hospital (during the current hospitalization) as well as discharge to a hospice in-patient facility with the presumption that death would be imminent. We further analyzed mortality stratified by age categories (65-70, 71-75, 76-80, 81-85, = 86) and by injury severity based on ISS ranges (0-15, 16-24, =25) [3].
Secondary outcomes
Secondary outcomes that were analyzed included readmission rates, total hospital length of stay, trauma Intensive Care Unit (ICU) length of stay, discharge disposition, complications and patients requiring surgery. Readmission was defined as admission to the discharging hospital within 30 days of discharge. Discharge disposition was defined as home, skilled nursing facility, assisted living facility or hospice. Complications were defined as cardiac arrest, drug/alcohol withdrawal, acute renal failure, pneumonia, urinary tract infection, and sepsis. The drug/alcohol withdrawal complication was defined as presence of drug withdrawal from sedative/hypnotics like benzodiazepines or opiates as well as alcohol.
Statistical analysis
The analysis was conducted in SAS© software (Version 9.3, SAS Institute Inc., Cary, NC), where chi-square and Student’s t-tests were used for bivariate analysis. Multivariate logistic regression was used to control for the effect of age, ISS, LOS, number of comorbidities, trauma diagnosis, major functional dependence and injury mechanisms on overall mortality between GTC and usual care.
Results
Baseline and hospital data
There were 395 trauma patients with multiple rib fractures admitted to the trauma service during the 36 months (i.e., October 2012 to November 2014) study period (Table 1), of which 149 (38%) were referred for co-management in the GTC. Patients more than 85 years old comprised 34.2% of the cases in the GTC group. Compared to the usual care group, the patients in the GTC group were in general older by an average of 2.9 years (81.2 vs 78.3; p-value=0.01), were more likely to have sustained a fall as the mechanism of injury and had a significantly higher number of co-morbidities (Charlson 2.8 vs 2.1; p-value<0.001). The mean ISS score was 12.3 (GTC) and 12.9 (usual care group) and the difference was not significant (p-value=0.6962). The two groups also did not differ significantly in the mean AIS scores for all the 6 body regions or in the number of trauma diagnoses (3.2 vs 3.5; p-value=0.4124). The majority of cases in both groups (80.5% vs 71.1%) were in the ISS score range of 0-15.More patients in the usual care group were admitted from home compared to the GTC group and the difference was statistically significant (93.9% vs 85.9%). The GTC group had a significantly higher number of patients admitted from assisted living facilities (10.1% vs 3.3%).
Study group
GTC
(n=149)
Usual carea
(n=246)
Full sample
(n=395)
Age, mean (SD)**
81.2 (8.8)
78.3 (8.6)
79.4 (8.8)
Age categories, no. (%)
65-70
24 (16.1)
60 (24.4)
84 (21.3)
71-75
22 (14.8)
44 (17.9)
66 (16.7)
76-80
18 (12.1)
37 (15.0)
55 (13.9)
81-85
34 (22.8)
46 (18.7)
80 (20.3)
Over 85
51 (34.2)
59 (24.0)
110 (27.8)
Gender, no. (%)
Male
67 (45.0)
128 (52.0)
195 (49.4)
Race, no. (%)
White
139 (93.9)
228 (92.7)
367 (92.9)
Day of the week, no. (%)
Weekend
37 (24.8)
77 (31.30)
114 (28.9)
Injury mechanism, no. (%)
Fall
115 (77.2)
168 (68.3)
283 (71.6)
ISS Score, mean (SD)
12.3 (6.5)
12.9 (7.3)
12.7 (7.0)
ISS Categories, no. (%)
0-15
120 (80.5)
175 (71.1)
295 (74.7)
16-24
22 (14.8)
54 (22.0)
76 (19.2)
25 or more
7 (4.7)
17 (6.9)
24 (6.1)
AIS Scores, mean (SD)
Head
2.6 (0.7)
2.8 (0.7)
2.8 (0.7)
Face/Neck
1.5 (0.7)
1.9 (0.5)
1.8 (0.5)
Chest
2.8 (0.5)
2.8 (0.6)
2.8 (0.6)
Abdomen/pelvis
2.2 (1.9)
2.2 (2.1)
2.2 (0.5)
Extremities
2.1 (2.0)
2.2 (2.1)
2.2 (0.5)
External
1.0 (1.0)
1.1 (1.0)
1.1 (0.3)
DNI DNR
20 (13.4)
24 (9.8)
44 (11.1)
No. of Trauma Dx, mean (SD)
3.2 (2.3)
3.5 (2.7)
3.4 (2.6)
No. of comorbidities, mean (SD)***
2.8 (1.6)
2.1 (1.5)
2.3 (1.6)
Comorbidities, no. (%)
Cancer
6 (4.0)
2 (0.8)
8 (2.0)
CHF
15 (10.1)
21 (8.5)
36 (9.1)
Diabetes
36 (24.2)
48 (19.5)
84 (21.3)
Hypertension
117 (78.5)
154 (62.6)
271 (68.6)
Respiratory
23 (15.4)
23 (9.4)
46 (11.7)
Admission Location*
Home, no. (%)**
128 (85.9)
231 (93.9)
359 (90.9)
ALF, no. (%)**
15 (10.1)
8 (3.3)
23 (5.8)
SNF/Acute Rehab, no. (%)
6 (4.0)
7 (2.9)
13 (3.3)
Notes: * – p<0.05; ** - p<0.01; *** - p<0.001; a - care provided by the trauma team.
Abbreviations: AIS: Abbreviated Injury Scale; ALF: Assisted Living Facility; CHF: Congestive Heart Failure; Dx: Diagnosis; DNR/DNI: Do Not Resuscitate/Do Not Intubate; GTC: Geriatric Trauma Co-Management Program; ISS: Injury Severity Score; SD: Standard Deviation; ALF: Assisted Living Facility; SNF: Skilled Nursing Facility.
Table 1: Baseline Characteristics of Analytical Study Sample.
Primary outcome
Table 2 shows our primary outcome of overall mortality. In the GTC group, overall mortality was lower by 40.7%, translating to nine fewer deaths. The outcome was also statistically significant with an odds ratio of 0.4 (p-value=0.0285), after adjusting for ISS score, age, number of trauma diagnoses, number of comorbidities, injury mechanism, LOS, and gender. As expected, mortality rate was highest in the ISS=25. For ISS (0-15) there was 37.5% (p-value= 0.0373) reduction in mortality. In the ISS (16-24) category, there was a 9.0% (p-value= 0.0791) difference with a increase in mortality in the GTC group. Mortality in the ISS (>25) range category was 47.9% lower (p-value = 0.3723) in the GTC group (Figure 1).
Outcomes
Unadjusted
Adjusteda
No. (%)
OR (95% CI)
n=
P-value
OR (95% CI) n=
P-value
Overall Mortalityb
Usual carec
37 (15.0)
1 [Reference]
1 [Reference]
GTC
13 (8.7)
0.54
( 0.28-1.05)
0.0705
0.40
(0.18-0.91)
0.0285
Notes: a- Results from logistic regression model with indicators of study group and controls for Geri-Consult,Age, Number of comorbidities, major psych, dependent health status, length of stay, injury from fall, injury from bike, Trauma Diagnosis, ISS score. b- Overall Mortality- Patients who expired or were discharged to hospice. c- Care provided by the trauma team.
Abbreviations: OR: Odds Ratio; CI: Confidence Interval; GTC: Geriatric Trauma Co-Management Program.
Table 2: Main outcome.
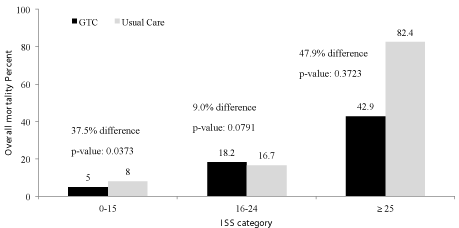
Figure 1: Overall mortality by ISS Category.
Notes: b- Overall Mortality – Patients who expired or were discharged to
hospice. c - Care provided by the trauma team.
Abbreviations: GTC: Geriatric Trauma Co-Management Program; ISS: Injury
Severity Score.
Secondary outcomes
There was no significant difference between the secondary outcomes of readmission and length of stay (ICU and total hospital). Individuals who received care in the GTC group were significantly (p-value <0.0001) more likely to be discharged to skilled nursing facility than those who received usual care (Table 3).
Outcomes
Study group
GTC
(n=149)
Usual carea
(n=246)
Full sample
(n=395)
Readmission, no. (%)
2 (1.3)
4 (1.7)
6 (1.5)
Length of stay, mean (SD)*
6.9 (5.3)
5.7 (5.6)
6.2 (5.5)
ICU Length of stay, mean (SD)
4.6 (3.4)
4.7 (5.7)
4.7 (4.8)
Discharge Location, no. (%)
Home**
37 (24.8)
104 (42.3)
141 (35.7)
SNF/Acute Rehab***
97 (65.1)
99 (40.2)
196 (49.6)
Assisted Living
1 (0.7)
3 (1.22)
4 (1.0)
Hospice
4 (2.7)
18 (7.3)
22 (5.6)
Complications, no. (%)
Cardiac arrest
1 (0.7)
3 (1.2)
4 (1.0)
Drug/alcohol withdrawal
4 (2.7)
5 (2.0)
9 (2.3)
ARF
0 (0.0)
1 (0.4)
1 (0.25)
PNA
3 (2.0)
7 (2.9)
10 (2.5)
UTI
20 (13.4)
18 (7.3)
38 (9.6)
Sepsis
2 (1.3)
6 (2.4)
8 (2.0)
Surgery
15 (10.1)
29 (11.8)
44 (11.1)
Notes: * - p<0.05; ** - p<0.01; *** - p<0.001.
Abbreviations: GTC: Geriatric Trauma Co-Management Program; ARF: Acute Renal Failure; PNA: Pneumonia; UTI: Urinary Tract Infection; ICU: Intensive Care Unit; SD: Standard Deviation; SNF: Skilled Nursing Facility.
Table 3: Secondary outcomes.
Discussion
Mortality in trauma correlates with age; comorbidities and grading of injuries. A study by Finelli et al. [17] demonstrated an agedependent increase in mortality for all ISS groups, all mechanisms of injury and all body regions. It is no surprise then that chest trauma in older patients is more likely to result in death and significant complications than in similarly injured young patients [18-20]. Rib fractures in particular, which are a marker of injury severity [21-25] and indicate associated severe traumatic injuries, [5,22-24] should receive special attention in the elderly as shown by previous work [2, 25]. Overall mortality in older trauma patients with rib fractures in our study was 10.1% which was close to the reported range (11-17%) from previous studies [1,5,19,26-28].
To cater to the specialized needs of the older trauma patient various approaches relating both to trauma care and medical management have been tried. Research by Clement et al. [29] has suggested that early medical/physician intervention may avert deaths in the older trauma patient due to medical complications arising late in the admission and unrelated to the initial trauma insult.
We found a significant reduction in overall mortality in the geriatric trauma co-management group for older trauma patients with rib fractures. There was no significant difference in the AIS scores of the five body regions between the two groups possibly implying that the pattern of injury may not have played a significant role in accounting for the difference in mortality between the groups. Similar to other studies, [3,30] we found that our subjects with the highest mortality also presented with the most severe ISS scores (ISS = 25).
Our study on the co-management model of care for older trauma patients with multiple rib fractures demonstrates that overall mortality can be improved by as much as 22.0% with such an intervention. This echoes findings from a study by Fallon et al. [10] which reported a reduction in mortality in older trauma patients who were seen by a geriatric consult service at a level 1 trauma center. We speculate that the improved survival may have been the result of a proactive approach to medication management, co-morbid disease management and prevention of complications. The existing literature remains controversial on the role of preexisting co-morbidities, in part because of a wide variety of age definitions for geriatric trauma, statistical methodologies, and outcome measures.
Labib et al. [30] concluded that pre-existing co-morbidities are not independent risk factors of mortality in geriatric trauma patients, whereas others have reported that not only do pre-existing conditions increase the odds of experiencing a complication to over three fold, [31] but age and pre-existing conditions are independent and additive risk factors of mortality after trauma, (31) with similar findings in the elderly rib fracture patient populations [1,21,33-34] Studies suggest that the greatest effect of pre-existing conditions on mortality is at an intermediate level of injury [6]. Our study was inadequately powered to demonstrate relative benefit from GTC for individuals with moderate or severe injury severity.
As seen in Figure 2, the mortality rate seems to be similar across all age ranges in the GTC but increases sharply in patient’s aged 81 and older in the usual care group. This trend is similar to the finding in the study by Finelli et al. [17] which showed that trauma patients older than 74 years had twice the odds of mortality compared to those 65-74 years of age. There was a significant improvement in mortality in ISS score range (0-15) in the GTC group. In the severe ISS score range (>25) we observed nearly 50% less mortality but our sample size was insufficient to reach significance. Given the beneficial effect of the GTC model for patients across all age subgroups and in ISS ranges (0-15) and perhaps in ISS>25, we think the greatest net clinical benefit from GTC might be realized by the trauma patients older than 80 years with low ISS scores, as this represents the patients most frequently seen.
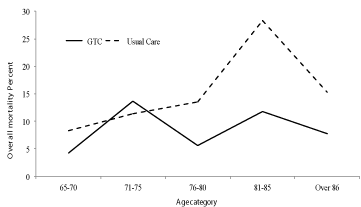
Figure 2: Overall Mortality by Age.
Notes: b- Overall Mortality- Patients who expired or were discharged to
hospice. c - Care provided by trauma team.
Abbreviations: GTC: Geriatric Trauma Co-Management Program.
Our disposition data see in Table 3 revealed that the patients in the GTC group were significantly more likely to be discharged to a Skilled Nursing Facility (SNF). There were significantly more patients admitted from assisted living facilities and nursing homes under the GTC group. We think that the higher rates of discharges to skilled rehabilitation facilities in the GTC group may be reflective of a higher premorbid functional dependence, worsened by deconditioning acquired during hospitalization. Association of lower pre-injury ADL function with greater care needs at discharge as shown by Dunham C et al. supports our finding [35]. Significantly higher number of comorbidities in the GTC group also likely drove the need for ongoing medical surveillance and care at rehab facilities.
Our study had limitations. Our retrospective design can introduce bias. It was underpowered to detect improvement in mortality across all injury severity ranges or to show significant improvements in other outcomes. In terms of mortality outcomes, we did not analyze for a change in patient/family preference for aggressiveness of care and cannot say if that could have impacted mortality rates between the groups. We did not measure premorbid functional status or incident/ prevalent delirium which could likely have impacted discharge dispositions in the two groups.
Conclusion
In conclusion, after adjusting for covariates, the GTC care model can reduce mortality in the older trauma patient with multiple rib fractures. Hence, using a GTC model for older trauma patients with multi-morbidity may improve patient outcomes, with possibly the greatest impact on the patient subset older than 80 years of age and those with lower ISS scores. More research is needed to explore the effect of this care model on other patient and hospital centered outcomes, and a larger sample size is needed to establish benefit with more severe injuries.
Acknowledgement
Author contributions: Study concept and design: Singh, Butterfield, McNicoll, Heffernan; Data acquisition: Singh, George; Data Analysis: Butterfield, Monteiro; Data interpretation: Singh, Butterfield, Monteiro, McNicoll, Heffernan; Manuscript preparation: Singh, Butterfield, Monteiro, McNicoll; Manuscript review: Singh, Butterfield, Monteiro, George, Heffernan, McNicoll, Gravenstein.
References
- Bulger EM, Arneson MA, Mock CN, Jurkovich GJ. Rib fractures in the elderly. Journal of Trauma. 2000; 48: 1040-1047.
- Bergeron E, Lavoie A, Clas D, Moore L, Ratte S, Tetreault S, et al. Elderly trauma patients with rib fractures are at greater risk of death and pneumonia. Journal of Trauma Injury, Infection and Critical Care. 2003; 54: 478-485.
- Hashmi A, Ibrahim-Zada I, Rhee P, Aziz H, Fain MJ, Friese RS, et al. Predictors of mortality in geriatric trauma patients: A systematic review and meta-analysis. Journal of Trauma Acute Care Surgery. 2014; 76: 894-901.
- Palvanen M, Kannus P, Niemi S, Parkkari J, Vuori I. Epidemiology of minimal trauma rib fractures in the elderly. Calcif Tissue Int. 1998; 62: 274-277.
- Ziegler DW, Agarwal NN. The morbidity and mortality of rib fractures. J Trauma. 1994; 37: 975-979.
- Grossman MD, Miller D, Scaff DW, Arcona S. When is an elder old? Effect of preexisting conditions on mortality in geriatric trauma. J Trauma 2002; 52: 242-246.
- Richardson JD, Adams L, Flint LM. Selective management of flail chest and pulmonary contusion. Ann Surgery. 1982; 196: 481-487.
- Battistella FD, Din AM, Perez L. Trauma patients 75 years and older: long term follow-up results justify aggressive management. J Trauma. 1998; 44: 618-623.
- Calland JF, Ingraham AM, Martin N, Marshall GT, Schulman CI, Stapleton T, et al. Eastern Association for the Surgery of Trauma. Evaluation and management of geriatric trauma: an Eastern Association for the Surgery of Trauma practice management guideline. J Trauma Acute Care Surg. 2012; 73: S345YS350.
- Friedman SM, Mendelson DA, Bingham KW, Kates SL. Impact of a comanaged Geriatric Fracture Center on short-term hip fracture outcomes. Arch Intern Med. 2009; 169: 1712-1717.
- Lenartowicz M, Parkovnick M, McFarlan A, Haas B, Straus SE, Nathens AB, et al. An evaluation of a proactive geriatric trauma consultation service. Annals of Surgery. 2012; 256: 1098-1101.
- Fallon WF, Rader E, Zyzanski S, Mancuso C, Martin B, Breedlove L, et al. Geriatric outcomes are improved by a geriatric trauma consultation service. The Journal of Trauma Injury, Infection and Critical Care. 2006; 61: 1040- 1046.
- Friedman SM, Mendelson DA, Kates SL, MCcann RM. Geriatric Co- Management of Proximal Femur Fractures: Total Quality Management and Protocol- Driven Care Result in Better Outcomes for a Frail Patient Population. JAGS. 2008; 7: 1349-1356.
- Baker SP, O’Neill B, Haddon W, Long WB. The injury severity score: A method for describing patients with multiple injuries and evaluating emergency care. J Trauma. 1974; 14: 187-196.
- Linn S. The injury severity score--importance and uses. Ann Epidemiol. 1995; 5: 440-446.
- MacKenzie EJ. Injury severity scales: Overview and directions for future research. Am J Emerg Med. 1986; 2: 537-549.
- Finelli FC, Jonsson J, Champion HR. A case control study for major trauma in geriatric patients. J Trauma. 1989; 29: 541-548.
- Svennevig JL, Bugge-Asperheim B, Geiran OR. Prognostic factors in blunt chest trauma: Analysis of 652 cases. Ann Chir Gynecol. 1986; 75: 8-14.
- Shorr RM, Rodriguez A, Indeck MC, Crittenden MD, Hartunian S, Cowley RA. Blunt chest trauma in the elderly. J Trauma. 1989; 29: 234-237.
- Cameron P, Dziukas L, Hadj A, Clark P, Hooper S,. Rib fractures in major trauma. Aust NZJ Surg. 1996; 66: 530-534.
- Stawicki SP, Grossman MD, Hoey BA, Miller DL, Reed JF. Rib fractures in the elderly: A marker of Injury Severity, JAGS. 2004; 52: 805-808.
- Wu CL, Jani ND, Perkins FM. Thoracic epidural analgesia versus intravenous patient controlled analgesia for the treatment of rib fracture pain after motor vehicle crash. J Trauma. 1999; 47: 564-567.
- Bollinger CT, Van Eeden SF. Treatment of multiple rib fracture: randomized controlled trial comparing ventilatory with non-ventilatory management. Chest. 1990; 97: 943-948.
- Wisner DH. A stepwise logistic regression analysis of factors affecting morbidity and mortality after thoracic trauma: effect of epidural analgesia. J Trauma. 1990; 30: 799-805.
- Simali M, Turut H, Topcu S. A comprehensive analysis of traumatic rib fractures: Morbidity, mortality and management. Eur J Cariothoracic Surg. 2003; 24: 133-138.
- Lee RB, Bass SM, Morris JA Jr. Three or more rib fractures as an indicator for transfer to a level I trauma centre: apopulation-based study. J Trauma. 1990; 30: 689-694.
- Poole GV, Myers RT. Morbidity and mortality rates in major blunt trauma to the upper chest. Ann Surg. 1981; 193: 70-75.
- Wilson RF, Murray C, Antonenko DR. Non penetrating thoracicinjuries. Surg Clin North Am. 1997; 57: 17-36.
- Clement ND, Tennant C, Muwanga C. Polytrauma in the elderly: Predictors of the cause and time of death. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine. 2010, 18: 26.
- Labib N, Nouh T, Winocour S. Severely injured geriatric population: morbidity, mortality and risk factors. J Trauma. 2011; 71: 1908-1914.
- Richmond TS, Kauder D, Strumpf N. Characteristics and outcomes of serious traumatic injury in older adults. JAGS. 2002, 50: 215-222.
- Hollis S, Lecky F, Yates DW, Wood M. The effect of pre-existing medical conditions and age on mortality after injury. Journal of Trauma. 2006, 61; 1255-1260.
- Millham FH, LaMorte WW: Factors associated with mortality in trauma: Reevaluation of the TRISS method using the National Trauma Data Bank. J Trauma. 2004: 56; 1090-1096.
- Bergeron E, Rossignol M, Osler T. Improving the TRISS methodology by restructuring age categories and adding comorbidities. J Trauma. 2004; 56: 760-767.
- Dunham CM, Chance EA, Hileman BM et al: Geriatric Preinjury activities of daily living function is associated with Glasgow coma score and discharge disposition: a retrospective, consecutive cohort study. J Trauma Nurs. 2015; 22: 6-13.