
Special Article - Long-Term Care Staffing Policies and Programs
Gerontol Geriatr Res. 2016; 2(5): 1025.
A Quality of Care Evaluation of a Care Delivery Model for Resident Care
Kobayashi KM*
Department of Sociology and the Institute on Aging and Lifelong Health, University of Victoria, Canada
*Corresponding author: Karen M Kobayashi, Department of Sociology and the Institute on Aging and Lifelong Health, University of Victoria, Associate Professor and Research Affiliate, Victoria, BC V8W 3P5, Canada
Received: October 06, 2016; Accepted: November 08, 2016; Published: November 10, 2016
Abstract
Residential care facilities are an important option for adults who require 24 hour nursing care. Providing Quality of Care (QoC) to older adults in these settings is an ongoing challenge given the increasingly complex needs of this population and the escalating economic constraints within which health authorities operate. While the implementation of the residential care delivery model has contributed to some improvements in quality of care, it has also highlighted key challenges that are both interpersonal and organizational in nature. Specifically, gaps in leadership, teamwork, mentorship, and communication, as well as staffing mix, staffing consistency, resident complexity, and competing policy and program initiatives and directives. The implementation of a major change in the way that care is delivered impacts residents, family members, and staff and may in turn, impact their perceptions of change in quality of care. When evaluating a model, therefore, it is important to include the voices of those most affected in their dayto- day lives by the change. A key strength of this study is the opportunity to draw insights and lessons from a vast array of both qualitative and quantitative data from multiple sources. In addition to studying existing quantitative indicators of QoC, such an evaluation requires the collection and analysis of qualitative data from multiple sources. Finally, this study underscores the importance of acknowledging the centrality of quality of care to the promotion of quality of life for residents, family members, and staff in long term care settings.
Keywords: Long term care; Quality of care; Consistent Staff; Nurses
Background
In Canada as in many developed countries, residential care facilities are an important option for adults who require 24 hour nursing care. Providing Quality of Care (QoC) to older adults in these settings is, and will continue to be, an ongoing challenge given the increasingly complex needs of this population and the escalating economic constraints within which health authorities operate. Indeed, creating efficiencies and cost savings while preserving QoC in a person-centered environment has proven to be a difficult balancing act. Although we know that appropriate staff mix and availability are associated with better resident outcomes [1,2], the actual parameters that define “adequate” and “appropriate” remain elusive [3].
Health Authorities provide subsidized care for adults who are unable to live safely or independently at home due to complex health care needs. Funding models and costs of care and service that residents fund through various co-payment models also differs across Canada, and within provinces. Within Canada, the average age of individuals living in institutional, residential care settings is typically between 80 and 85 years and approximately 60-65% of the population is female [4]. The staff that provides direct care in residential care facilities includes unregulated Health Care Assistants (HCA); as well as professional staff such as: Licensed Practical Nurses (LPN), Registered Nurses (RN) and/or Registered Psychiatric Nurses (RPN). Other allied health care professionals who provide care include: therapists (occupational, physical, music, recreation), social workers, and spiritual care counselors.
In some jurisdictions, there is currently no provincial legislation regarding: (1) the minimum number of direct care hours per day that must be provided to older adults in residential care settings; or (2) the qualifications required for staff who are delivering such care [1]. The absence of such standards for staffing inevitably has an impact on the QoC delivered and received in residential care facilities [5]. Defining and improving quality of care has been a longstanding focus of health authorities, the Office of the Seniors Advocate, those who work within Long Term Care Facilities (LTC), as well as researchers.
Studies conducted in acute care settings suggest that as the number of RNs increase, certain patient outcomes improve such as: decreases in mortality, infection and pressure ulcer rates [3,6]. Literature examining the relationship between nurse staffing levels and quality of care in residential care facilities is slowly growing, but remains predominantly based on US or European experiences [7]. In an attempt to address this knowledge gap, executive leadership in a Western Canadian health authority redesigned and implemented a new residential Care Delivery Model (CDM) in 2011. The goal of the model was to both standardize access to care and improve quality of care.
The care delivery model consists of three specific and inter-related aspects: (1) staffing mix (registered nurses, licensed practical nurses, and health care assistants); (2) funding methodology (how much funding and for what); and (3) the provision of 3.0 direct care nursing hours (number of care hours provided by direct care staff (inclusive of RNs, LPNs and HCAs, per resident per day). A concomitant set of principles, guidelines and standards were developed that focused on the provision of quality care within the parameters set out in the model. Specifically, the RN leadership role was delineated further, emphasizing the coordination and overseeing of residents’ care, while LPNs and HCAs focused on the provision of clinical care and addressed daily care needs.
Staffing mix
The major staffing changes included a reduction in RNs and an increase in LPNs, while HCAs remained relatively constant or increased slightly. Within the owned and operated sites, before the implementation (2009/10 figures), RNs made up 20% of the care staff while LPNs comprised 11% and HCAs 69%. After the model was implemented (based on 2012/13 figures), RNs made up 9% of care staff, LPNs 25% and HCAs 66%. The staff mix ratios varied substantially across the three study sites with one facility experiencing the greatest reduction in RNs (from 24% to 8%) and an accompanying substantial increase in LPNs (from 6% to 24%).
Funding
A further goal of the CDM was to standardize the approach to funding, with higher average expenditure per resident per day to improve quality of care. The standardized approach was implemented in order to offer residents comparable access to care across the region. This increase in compensation varied across facilities from 2 to 12% from 2009/10 to 2012/13. The largest increases in funding were seen at the contracted (HSP) care provider facilities.
Direct care nursing hours
Table 1 shows the total direct care hours, broken down by the three types of care providers. Facilities A and B, as well as the O&O sites met the goal of an increase in total DCHs of 3.0 after the model implementation while Facility B fell just slightly short. The HSPs increased their total hours (particularly from HCAs), but were still not meeting the 3.0 DCH goal as of 2012/13.
Direct Care Hours
DCH
RIN
LPN
HCA
Total DCHs
2009/10
2012/13
2009/10
2012/13
2009/10
2012/13
2009/10
2012/13
Facility A
0.44
0.32
0.25
0.57
2.16
2.16
2.85
3.05
Facility B
0.46
0.35
0.51
0.62
1.63
1.99
2.6
2.96
Facility C
0.65
0.24
0.16
0.73
1.87
2.04
2.68
3.01
All O&O
0.56
0.28
0.32
0.74
1.94
2.02
2.82
3.04
HSP
0.34
0.32
0.31
0.35
1.54
1.88
2.19
2.55
Table 1: Direct Care Hours by Care staff in 2009/10 and 2012/13.
Related to standardizing care, an important goal was to evaluate the impact of a change in health human resource allocation utilizing quality of care measures and fiscal indicators. In summary, the overall aim of the CDM was to encourage a broader range of staff and skills to support a more socially-informed model of care; that is, to provide more direct assistance to residents to complete their basic activities of daily living.
Research Question
A collaborative partnership between academic researchers and knowledge users was forged between health authority clinical experts, decision makers, and researchers affiliated with a centre for aging-related research at a university in Western Canada. The team collaboration worked together to answer the main research question: Does the implementation of a Residential Care Delivery Model (i.e., changing the nursing staff mix, changing the funding methodology, and changing the direct care hours) affect the quality of care delivered and received in residential care facilities operated by the health authority?
Methods, Research Design and Data
The measurement of QoC is complex [8]. To interrogate this multi-dimensional concept, numerous data sources were considered, and a mixed methods research design was used. This three-year study collected both qualitative and quantitative data from a range of sources. To uphold confidentiality and anonymity, all quantitative data were secondary and were compiled at the aggregate-level for the research team by designated staff at the health authority. These data sources included provincial performance measures (e.g. unscheduled hospital transfers) and the standardized Resident Assessment Instrument Minimum Data Set 2.0 (RAI-MDS). Qualitative data were obtained from in-person interviews with a broad range of stakeholders, including management, nurse leaders, direct care workers, residents and families.
Three health authorities owned and operated residential care facilities, hereafter referred to as Facilities A, B, and C, were purposively selected for inclusion in the study. The selection criteria were based on geographic representation (north, south and east areas within the health authority), facility size (i.e., approximately 100 residents), and CDM implementation in 2011. Each of the three facilities was located in an urban area. All three buildings were older, single floor dwellings with primarily multiple bed rooms, interconnecting hallways between neighborhoods (i.e., units), and large dining rooms.
All older adults age 65+ moving in to residential care receive an assessment based on the internationally recognized Resident Assessment Instrument - Minimum Data Set 2.0 (RAI-MDS 2.0). Residents are assessed at intake (entry point) and then ideally at quarterly intervals, or when there is a change in a resident’s health and care trajectory, to assist in the creation of an appropriate care plan, as well as to track changes in the residents’ health over time [9]. With a focus on measuring and improving the quality of care for residents, various quality indicators within the RAI have been identified and validated as proxy measures for quality of nursing home care [10,11] (i.e., restraint use, falls, pressure ulcers, experience of pain) [12,13].
Of the numerous RAI-MDS indicators for which there were data, we selected only those indicators that were deemed to be more sensitive to nursing care and eliminated those that we identified as not being directly affected by changes to the staffing mix. The selection of the indicators was supported by the literature [13,14] and the ‘lived experiences’ described by a diverse Advisory Panel of experts from the practice field. The final indicators selected from RAI-MDS included pressure or stasis ulcer any stage, infection rates (wound, urinary, respiratory), frequent pain of moderate intensity, fractures from falls, antipsychotic drug use in absence of psychotic and related conditions and verbal or physical abuse affecting others.
In gathering the qualitative data, researchers visited each site to introduce the study and request participation. In addition, pamphlets explaining more about the study were left at each site for staff to review. Family members were informed of the study through regularly scheduled meetings called Family Council meetings, while eligible residents were recruited by facility staff (typically a social worker or recreation therapist). Prior to conducting the interviews, ethics approval was received jointly from the University of Victoria Human Subjects Ethics Review Committee and the health region’s ethics approval committee.
The qualitative data were collected in both group, and one-onone interview settings using a semi structured interview guide with allowance for open-ended discussion from participants. A nonrandom, convenience sampling technique was employed. Residents, family members, direct care staff, allied health personnel and senior and site leadership members (i.e., directors, managers) were invited to share their experiences of the CDM. Almost all interviews were completed at the facilities though one occurred in a family member’s home, and another took place in a community location. Face to face interviews were conducted individually or in the same occupation groups in an attempt to address potential power imbalances. A small number of interviews were conducted over the telephone. A total of 116 interviews were completed with 160 participants at two time periods (summer 2012 and 2013). Due to attrition, scheduling conflicts, etc., most care staff was only interviewed once, while site leadership members (Residential Care Coordinator, Clinical Nurse Educator, manager, director) were able to be interviewed at both time periods. All interviews were recorded and then professionally transcribed (Table 2).
Interview Participants
Total Number
Nurse Leaders
23
Registered Nurses
7
Licensed Practical Nurses
16
Health Care Aides
32
Recreation Therapist
6
Social Worker
2
OT/PT
6
Residents
32
Family Members
28
Other
8
TOTAL
160
Table 2: Interview Participants.
Data Analysis
As noted, the main quantitative information was aggregated RAI data provided to the research team. This information dated back a year and a half before the implementation to three years after (June 2009 to June 2014) for the three study sites (Facilities A, B, C). In addition, we received combined average data from the other Owned and Operated (O&O) and contracted sites (HSP). The data were first observed on a quarterly basis to discern if there were any noticeable pre-post implementation trends. Monthly data were then provided and analyzed by calculating rolling six-month averages to smooth out any peaks or substantial dips (see Tables x-x in results section).
Qualitative analysis occurred concurrently with data collection. The first level analysis was undertaken by a member of the research team in a process of reading through the transcripts to develop preliminary themes. All transcripts were entered and coded using NVIVO 10, a software program that was used to “code” - organize and retrieve - excerpts of the data [15].
Emergent findings at phase one were used to inform and direct further interviews, not replacing the original interview schedule, but refining questions and adding probes. The second level analysis was conducted in multiple team meetings, where members were engaged in in-depth discussions about emergent themes. To enhance and support the analysis of all the data, an Advisory Panel (AP) of interdisciplinary team members working in various capacities within the residential care sector (who were not team members of the three study sites) was established to contribute to the processes of data interpretation and validation and to provide oversight to the project. The panel met seven times over the course of the three-year study period.
Throughout the analysis, health authority team members provided important critical perspectives on contextual issues, giving broader insights, and confirming and questioning emergent ideas. This process helped challenge fixed assumptions or biased conclusions on the part of both academic and health authority team members. Ongoing discussion took place at monthly team teleconference meetings and informal meetings after phase 1 of data collection and through phase 2, which allowed for further reflection and refinement of the themes.
Results and Discussion
In this section, the results are discussed, first reviewing the quantitative findings and then the insights gleaned from qualitative interviews.
Quantitative findings and discussion
RAI-MDS 2.0: In an attempt to measure care objectively, Quality of Care Indicators (QIs) based on available evidence and expert consensus have been identified within the RAI-MDS 2.0, and validated as proxy measures for quality of care within long term care facilities [11]. Nine nurse-sensitive indicators of QoC were selected by the research team in consultation with the AP members and based upon the research literature. These included pressure ulcers (any stage), UTIs, respiratory infection, wound infection, aggressive behavior, verbal and/or physical abuse, antipsychotic use, pain (moderate+ intensity), and fracture within past 180 days. Several of these indicators are consistent with the indicators used by the Canadian Institutes of Health Information (CIHI) in a recent report (2014?). CIHI divides the indicators into three themes: Appropriateness and Effectiveness of Care, Safety, and Health Status. Their web tool, Your Health System, unveiled in June 2015, allows the public to compare over 1000 LTC facilities across Canada with data from 2009/10 to 2013/14.
The following observations were made from the analysis of the RAI-MDS 2.0 data. While variation across time is evident at all three facilities (A,B&C), the indicators with the greatest amount of variability included urinary tract infections and pressure ulcers. Urinary Tract Infections saw the most variation at Facility A with several peaks and a higher rate after the implementation. At Facility B, the UTI percentage has returned to pre-implementation rates while Facility C rates increased post-implementation, but have been decreasing over the past two years (Figure 1).
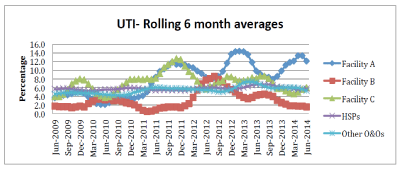
Figure 1: Urinary Tract Infections (rolling 6 month averages).
For pressure ulcers (any stage), Facility A saw no change in this indicator, while data from Facility B indicated that there was a decrease in ulcers post-implementation, and Facility C saw an increase 12 months post-implementation, followed by a recent reduction (Figure 2).
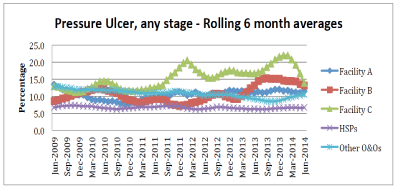
Figure 2: Pressure Ulcer, any Stage (rolling 6 month averages).
Antipsychotic use decreased in Facility B, while Facility A saw an increase in the months prior to CDM implementation, and no change following implementation, while Facility C saw an increase in the months prior to implementation, and a continued increase throughout implementation with a leveling off post-implementation.
Regarding physically or verbally abusive behavior, all three facilities reported slight variations across time, but all facilities as well as the other owned and operated sites were relatively stable by the end of the time frame (15-20%). In Facility B and C, there was no change in reported pain. In Facility A, an increase in this indicator began months prior to the CDM, peaking at two years’ post CDM, and then declined. One of the interesting aspects of the Pain graph is that it “mimics” changes in other key nurse sensitive indicators related to infection (UTI and Respiratory infection, and aggressive behavior). The indicators with the lowest/minimal variation include fractures, respiratory and wound infection, and aggressive behavior.
Although RAI indicators did not show substantial changes over the three-year period, some fluctuation occurred, with most of it leveling off to pre-implementation rates. An additional performance measure, “Unscheduled Trips to the ER” was also examined. The three facilities averaged approximately 5 transfers per 100 residents per quarter, peaking to 9 in the fall of 2011 and then decreasing to 6.1 in 2013. Other owned and operated facilities reported 6.2 transfers in 2012 and 8.3 in 2013. Given the nature of the data we cannot conclude that the CDM was causally linked to this short-term increase in transfers to the emergency room or, for example, that the data actually reflect changes in resident health over that time period.
Despite an increase in direct care hours, questions remain about the impact on staff during and as a result of the change. In the qualitative interviews staff expressed feelings of stress, fatigue, and in some cases, moral distress. The CDM changes, although perhaps not necessarily directly responsible for these effects, appeared to increase the intensity of these feelings at two of the three study sites. One of the most interesting findings in this study relates to the divergence between the quantitative RAI indicators, and the qualitative insights from staff about quality of care, team functioning.
Relatedly, some AP members and interview participants questioned the quality of the RAI data due to lack of consistent staff, and staff not completing forms in a timely and thorough manner. Participants in the study cautioned against relying on the RAI as a measure of quality care. They also expressed concern that the categories provided on the standardized assessment tool were not necessarily meaningful for each resident and that indicators could be misleading. An important sub-question that emerged from these discussions was how staff members could be supported in collecting these data since they may not recognize the value of completing the assessments in a broader context.
I believe it’s about relationships... And then to measure, I mean, there is nurse sensitive outcomes that you know I’m thinking about infection and wounds and pressure sores and things like that. I think we do measure those, but it’s that intangible about what is the relationship like and the resident feeling valued (Director).
As noted in the quote above, the RAI indicators and other quantitative measures provide some insight into quality of care; however, they are not able to provide insights into the experience of giving or receiving care or the lived experience of staff working within the new CDM. The face-to-face interviews allowed participants to share their thoughts on the model and how it affected their day-today experiences as well as their impressions of care quality.
I know statistics will tell a story. I’m not sure they tell the whole story. In fact I know they don’t tell the whole story (Manager).
Qualitative findings and discussion
In speaking with care staff, the importance of interpersonal and organizational contexts came to light. Specific interpersonal concepts that were highlighted included leadership, teamwork, mentorship, and communication, while organizational issues that emerged were staffing mix, consistency in staff, complexity of residents, and competing program implementation. Both of these contexts – the interpersonal and the organizational – play an important role in the provision of high quality care.
Strong leadership
When a significant change is implemented, the importance of formal leaders (i.e., managers, Residential Care Coordinators and Clinical Nurse Educators) having expertise in change management, communication, and an understanding of the salience of their leadership in complex change management cannot be underestimated. A significant aspect of the CDM shift was gauging the readiness of team members to understand how the change would impact their roles at a micro level, specifically responding to the question, “What will my day look like?”
There is a pressing need to focus on the nature of local leadership, and support for leadership. In particular, the relationships and skill sets between all levels of management and direct care staff must be better understood. Our findings show that a collaborative and more inclusive model of leadership appears to work better than hierarchical or laissez-faire models. Opportunities for open dialogue, staff inclusion, engagement and investment in solution finding and implementation are hallmarks of such a model. Servant leadership1 is an example of a leadership model followed by one site that encouraged an environment in which staff felt supported and empowered and a common sense of purpose.
The concept of leadership and leading others and pulling the team together and being the leader without doing something, something task oriented, was a big step. It was a huge step. I’m not sure how much was invested in terms of leadership training for RNs. There have been snippets of it, but not a huge amount and I think that that’s one area that we’ve certainly tried to do it on site…. It’s hard to be part of the team if your leader is not leading. If nobody is leading the team right; everybody is doing their own thing. (Manager).
Teamwork and consistent staff
Direct care staff members do not work in isolation – it is their interactions with residents, each other, and other individuals in the ‘Microsystems’ of their facilities that determine quality outcomes. As such, this study confirmed that strong teams, as reflected in skilled leadership, consistent staff and shift rotations that support continuity of care (for example, limiting part-time scheduling or rotations that move staff between resident cohorts at frequent intervals) are key to building relationships between staff, residents, and family, a cornerstone of “quality of life” [16]. Effective leadership builds trust and creates an environment where staff, residents, and family feel supported.
In addition to the aforementioned factors, teamwork that includes aspects of mentorship, trust, and open communication appears to have greater resiliency in times of significant change. A resilient team is easier to create and maintain when staffing is consistent and staff turnover is low [17].
Mentorship
Mentorship and workplace education were strongly related to staff morale as well as teamwork. With a collaborative nursing model, the norm of helping and doing things together led more naturally into mentoring relationships.
…if you empower your people…. they’ll deliver good care. And you know they’ll pass that on to the care aides so that we are a strong team (RN).
This was not however the norm at all facilities, and mentorship seemed to be a missing component in some poorly functioning units, particularly at facilities where the influx of mostly new LPN graduates required a great deal of support. Where active resentments and resistance to the LPN influx was strong, these LPNs did not often find the support they required.
So knowing that resentment is there, I don’t know how much mentoring is going on, and again lots of staff changes so you’re mentoring one person and that person is gone and a new person is coming in. So, I think it’s very difficult to keep that ongoing relationship and mentoring when the staff is changing so frequently. (Volunteer coordinator).
Mentorship is key for those who need support to function to full capacity and to contribute as an important team member. However, mentorship requires time and resources, both of which can be scarce in long term care settings:
It took huge amounts of resources and support to get the LPNs to the level of knowledge and experience that they could function fairly independently… Does the LPN know as much as the nurse? No, she doesn’t and she doesn’t think the same way. She doesn’t think in a broad sense, more encompassing, all-encompassing sense, is much more focused or he is more, ah, focused on specific things related to what the resident needs. And it’s that broader knowledge and expertise that you need as well (Manager).
Role clarity and skill mix
The distinction between staff mix and staff knowledge and skills was also an important theme. With a revised staff mix reflected in a decrease in RNs alongside a shift in their roles, and an increase in LPNs and HCAs - there are more “hands” to provide care. However, through the interviews it was also deemed important to know and understand the expertise and clinical skills of the staff so that onsite, continuing education and mentorship could facilitate the development of the skills and knowledge of less experienced and/or less confident staff members. Indeed, it is the staff mix and integration of various knowledge sources that influences teamwork in terms of communication and the way(s) in which work flows over the course of a day.
In times of change, role clarity is needed; in particular, highlighting the importance of each position in working together to care for the resident. This is a foundational element of good teamwork and leadership. Role clarity is particularly important if the day-to-day work changes dramatically. Not only is it important for individual staff members to understand the change in their role, it is equally important for other team members to understand the changes in roles as well.
While the total hours of care were increased on evening shifts, staff expressed concern regarding increased resident activity in the evening/night, that is, frequent bell ringing, residents who were wandering, and others who were loud and disturbing others and/ or climbing out of bed. Some potential safety and risk issues were identified, however, in relation to the shift in staff mix. In the context of staffing, some team members noted that changes in the number of RNs assigned to the night shift reduced the number of staff who was trained to deal with complex medical situations:
If everything goes well then two people can manage it quite easily. You get a couple of sick people, it’s a bit of a challenge. You get someone who wanders, again even a greater challenge. Someone who suddenly gets sick in the middle of the night and you have to send to the ER (RN).
And so with more and more acute interventions, IVs, PICC lines, you name it. That for me, my barometer is we have one RN on nights for 110 residents. If you add this person with those needs to the mix, how safe is it? And you know sometimes it just isn’t, and if you know it does not going to be safe on a long-term basis… (Manager).
Organizational change
A major organizational change benefits from staff involvement starting at the earliest stages. Co-creating new role descriptions in partnership with team members may assist staff in understanding the change, the impact of the change, and may help to provide a sense of influence/control over their work environments. It needs to be recognized that staffing changes may represent a significant culture shift for some staff members. Disruption to staff morale may be mitigated by conducting an ‘environmental scan’ at facilities to identify readiness and any existing education and/or support for teams or leaders implementing the change. In addition, major change requires time to create new roles, systems of organization, and communication strategies.
So having the staffs who are going through the transition, the RNs and the LPNs, having them involved every step of the way was so important. What do you think this is going to look like and how can we support you? (Residential Care Coordinator - RCC).
Timing and context
Providing quality care is facilitated by continuity of care and effective teamwork, however, factors outside the control of managers and leadership impacted the ability to maintain these important attributes. Single Certification was one such factor. This initiative was a negotiated Memorandum of Understanding developed between the Facilities Bargaining Association and the Health Employers Association that provided an opportunity for staff who may have been experiencing job impacts due to restructuring to bid into positions anywhere within the Health Authority, versus the previous limited geographic “bumping” that occurred. This bumping and movement of staff made it difficult for teams to form cohesive groups at certain facilities.
It is important to understand, and, as much as possible, identify and mitigate the impact of confounding factors (i.e., layered change initiatives) that may increase staff, resident and family anxiety. For example, if another large initiative(s) is occurring at the same time and “adaptations” have to be made at facilities, clear and frequent communication to residents, families, and staff is required. Related to this point is the need to ensure enough lead-time to allow change to be evaluated and supported.
… When you’re just trying to meet your own basic workload and then all these other things [policies and guidelines] are thrown on you. And I understand they are for the betterment of care, but you need to give us time. We need time (LPN).
Measuring Quality of Care (QoC)
QoC does not mean the same thing across different care contexts; that is, the definition from home care or acute care cannot be easily applied in or transposed to LTC settings. To illustrate this point, results from this study challenge organizations, policymakers and academics to recognize residents’ social needs as an integral part of quality of care and to make these a priority.
Tensions between quality of care and Quality of Life (QoL) surfaced in the interviews; it became apparent that the metrics for measuring quality of care (e.g., ulcers, wound infections, antipsychotics use, etc.) were not those that care staff, residents or families identified as most important necessarily. Under quality of life, staff articulated the importance of knowing the resident, understanding the uniqueness of each individual and his/her relationships as being more highly valued than standardized quality of care measures. Quality of life was viewed as an integral aspect and dimension of quality of care in residential care.
This study not only confirmed the importance of care relationships as a factor in constructing a sense of well-being or Quality of Life (QoL) for residents, but also underscored that these relational aspects of care were a driving force behind staff’s job satisfaction. At present, resident quality of care information is gathered primarily through the standardized process RAI-MDS tools. This study highlights the fact that the quantitative assessment data alone do not provide a broad enough understanding of the aspects of quality of care from which to base resident care decisions in LTC settings.
Limitations
The introduction of Single Certification at the same time as the CDM constrained our ability to make conclusive statements about the full impacts of the CDM. In particular, Single Certification made it difficult to predict staff movement, impact on teams, and consequently left teams and leadership in limbo at times to mitigate the impact. In essence, any variable or factor outside the control of the residential program in the health authority may promote a significant level of disruption for staff, residents and families at the time the CDM was introduced. Thus, there is a need to take into account other initiatives or changes to health care protocols/practice guidelines that are being introduced simultaneously.
It’s not the Care Model that’s not working, but it’s just it’s so many other things – external/internal factors that influence this Care Model; the success of this Care Model and slow down the success. And I mentioned it to you before that Single Cert is a huge negative impact (Manager).
Conclusion
This research project examined an important question regarding how a care delivery model affected quality of care for residents. However, at the end of the day further questions emerged that require attention. Future research in this area should aim to develop a deeper understanding of what makes an effective leader during a time of transition, looking in particular at the mechanisms and models that are helpful in supporting care teams and leaders during times of change. The validity of specific quantitative data generated from standardized assessment instruments such as the RAI-MDS indicators was seriously questioned by participants, and …to accurately measure quality improvements in residential care was also seriously questioned by some participants, a finding that is supported in the literature [18,19]. As such, it is important to identify what measures do exist in these instruments or others that have sufficient sensitivity to provide evidence of clear improvements in quality of care and/or quality of life. The updated RAI 3.0, for example, actually includes questions requiring a response from the resident. Further, if improved quality of life is the goal after changes to service delivery are made, what might a revised model of care look like, i.e., what services need to be provided in residential care and what impact might these have on resident length of stay, service delivery, or resident, family, and staff satisfaction?
While the implementation of the residential care delivery model has contributed to some improvements in quality of care, it has also highlighted a number of key challenges in that are both interpersonal and organizational in nature. Specifically, these are linked to gaps in leadership, teamwork, mentorship, and communication, as well as issues with staffing mix, consistency in staffing, complexity of residents, and competing policy and program initiatives and directives. There is a need to recognize then that the implementation of a major change in the way that care is delivered will impact residents, family members, and staff and may in turn, impact their perceptions of change in quality of care. When evaluating a model, therefore, it is important to include the voices of those most affected in their day-to-day lives by the change. A key strength of this study is the opportunity to draw insights and lessons from a vast array of both qualitative and quantitative data from multiple sources. In addition to studying existing quantitative indicators of QoC, such an evaluation requires the collection and analysis of qualitative data from multiple sources. Finally, this study underscores the importance of acknowledging the centrality of quality of care to the promotion of quality of life for residents, family members, and staff in long term care settings.
References
- Office of the Ombudsperson. The Best of Care: Getting it Right for seniors in British Columbia (Part 2). Public Report No. 47 to the Legislative Assembly of British Columbia. 2012.
- Harrington C, Choiniere J, Goldmann M, Jacobsen FF, Lloyd L, McGregor M, et al. Nursing Home Staffing Standards and Staffing Levels in Six Countries. Journal of Nursing Scholarship. 2012; 44: 88-98.
- Canadian Nurses Association. Nursing Staff Mix: A Literature Review, Ottawa: ON, 20pp. 2004.
- Office of the Seniors Advocate. Seniors Housing in BC. 2015.
- McGregor M, Baumbusch J, Abu-Laban R, McGrail K, Andrusiek D, Globerman J, et al. A Survey of Nursing Home Organizational Characteristics Associated with Potentially Avoidable Hospital Transfers and Care Quality in One Large British Columbia Health Region. Canadian Journal on Aging. 2011; 30: 551-561.
- Aiken L, Sloane D, Van den Heede, Griffith P, Busse R, Diomidous M, et al. Nurse staffing and education and hospital mortality in nine European countries: A retrospective observational study. The Lancet. 2014; 383: 1824-1830.
- Spilsbury K, Hewitt C, Stirk L, Bowman C. The relationship between nurse staffing and quality of care in nursing homes: A systematic review. International Journal of Nursing Studies. 2011; 48: 732-750.
- McGregor M, Ronald L. Residential Long-Term Care for Canadian Seniors: Nonprofit, For-Profit or Does it Matter? IRPP Study, No. 14, Montreal: Institute for Research on Public Policy. 2011.
- Office of the Seniors Advocate. Placement, Drugs and Therapy… We can do better. 2015.
- McLean, A. The person in dementia: A study of nursing home care in the US. Peterborough, ON: Broadview Press. 2007.
- Rolland Y, Barreto P de Souto. Research Can Improve Care in the Nursing Home. Journal of the American Medical Directors Association. 2013; 14: 233-235.
- Estabrooks C, Knopp-Sihot J, Norton P. Practice sensitive quality indicators in RAI-MDS 2.0 nursing home data. BMC Research Notes. 2013; 6: 460.
- Canadian Institute for Health Information. When a nursing home is home: How do Canadian nursing homes measure up on quality? Ottawa, ON: CIHI. 2013.
- Donald F, Martin-Misener R, Carter N, Donald E, Kaasalainen S, Wickson-Griffiths A, et al. A systematic review of the effectiveness of advanced practice nurses in long-term care. Journal of Advanced Nursing. 2013; 69: 2148-2161.
- Richards L. Data alive! The thinking behind NVivo. Qualitative Health Research. 1999; 9: 412-428.
- Kane RA. Long-term care and a good quality of life bringing them closer together. The Gerontologist, 2001; 41: 293-304.
- Trastek V, Hamilton N, & Niles E. Leadership Models in Health Care – A Case for Servant Leadership. Mayo Clinic Proceedings. 2014; 89: 374-381.
- Kontos P, Miller K, & Mitchell G. Neglecting the importance of the decision making and care regimes of personal cupport workers: A critique of standardization of care planning through the RAI/MDS. The Gerontologist. 2009: 50: 352-362.
- Tellis-Nayak V. A Person-Centered Workplace: The Foundation for Person-Centered Caregiving in Long-Term Care. Journal of the American Medical Directors Association. 2007; 8: 46-54.