
Special Article - Long-term Care Staffing Policies and Programs
Gerontol Geriatr Res. 2017; 3(1): 1029.
Development of a Sensory Stimulation Care Integrated in Daily Practice for Nursing Home Residents with Moderate to Severe Dementia: An Action Research Approach
Kwong EWY¹*, Lai CKY², Tse MMY², Liu JYF² and Leung S³
¹School of Nursing, Tung Wah College, China
²School of Nursing, The Hong Kong Polytechnic University, China
³Alice Ho Miu Ling Nethersole Nursing Home, China
*Corresponding author: Enid WY Kwong, School of Nursing, Tung Wah College, Wyllie’s Road, Kowloon, Hong Kong, China
Received: May 19, 2017; Accepted: June 12, 2017; Published: June 19, 2017
Abstract
Purpose: An action research design was adopted in this study to elicit the process of change in care staff’s Sensory Stimulation (SS) care to nursing home residents with later dementia and to finally develop a sensory stimulation care integrated to daily practice.
Methods: Three nursing home residents with moderate to severe dementia and their family caregivers, and the care staff who provided direct care to nursing home residents with later dementia from a nursing home participated in this study. Two action research cycles of the SS care integrated to daily practice were carried out by the care staff members. There were two rounds of interviews with the family members and the care staff conducted after the implementation of the SS care. The data were collected between March and July 2015.
Results: In triangulation of the data collected from the care staff and the family members, four main themes were identified after the two cycles of implementation. They were behavioral (Reduction in agitated behavior, Decrease in suspicion), psychological (Increase in positive emotional responses) and social changes (Increased social interaction with care staff and family members, Improved motivation to participate in activities) of the residents and also increased job satisfaction of the care staff. At the end of the second cycle, the SS care integrated in daily practice was finally developed.
Conclusion: Overall, the finalized SS care was well-accepted by the care staff and the family members but availability of sufficient resources and manpower should be ensured for the sustainability of this SS care.
Keywords: Alzheimer disease; Nursing homes; Sensory stimulation care
Introduction
Care to nursing home residents with moderate to severe dementia
In 2011, 47% of all nursing home residents in the United States had a diagnosis of dementia [1],while in Hong Kong 31.6% of institutionalized people aged 60 or above were identified as suffering from dementia in 2009 [2], a figure projected to nearly by double between 2009 to 2039 in Hong Kong [3]. The majority of nursing home residents with dementia are at the moderate to severe stage of the disease, in which Behavioural and Psychological Symptoms Of Dementia (BPSD) are prevalent [4]. As the disease progresses, the residents become less aware and responsive as the severity of their dementia increases and their cognitive function decreases [5].
Nursing home residents with moderate to severe dementia usually lack adequate stimulation and human social interaction [6], which leads to an increase in their BPSD [4] and a decrease in their awareness and responsiveness [7]. Together with the BPSD, an increase in disabilities and morbidity among the residents will lead to more and/or prolonged hospitalizations and higher healthcare costs [8]. Staff caregivers in nursing homes will also have to spend more time managing the BPSD of these residents and will be more likely to experience distress in their care giving [9]. Their interaction with the residents may decrease, while their frustration with their job will increase [10], leading to burnout and a high staff turnover rate. This would negatively affect the quality of the care that is delivered to the residents [9].
Sensory stimulation-oriented care
Given this situation, there is an urgent need to improve the quality of the care delivered to residents with moderate to severe dementia. A non-pharmacological approach should be the first line of care [11]. A sensory stimulation-oriented approach that makes no appeal to intellectual abilities is feasible for people at the later stages of dementia [12]. Session-based Multisensory Stimulation (MSS) or Snoezelen in a room has been commonly used on older people with moderate to severe dementia [13-17] and on patients with dementia of all stages with BPSD, [18-21] in order to reduce their BPSD. In a recent review [22] of original studies of various designs and employing various experimental protocols to examine the impact of MSS on people with dementia [15,19,21,23,24], it was concluded that, in general, MSS has a positive effect on the behavior and mood of patients and/or on staff-patient communication, but that the effect of the stimulation only lasted as long as it was provided. Another review [25] of MSS for dementia patients, which included only two Randomized Controlled Trials (RCTs) [14,26], reported that MSS had no significant effects on the patients [14], with the exception of some short-term effects on behavior and mood from an MSS care programme that had been integrated into morning daily care [26].
Integrating sensory stimulation care in daily care
Indeed, psychosocial treatments, including a stimulationoriented approach to dealing with dementia, may not provide lasting effects; thus, those that can be embedded in daily care are practical and beneficial [27]. vanWeert reported the same trial in two studies [26,28] testing the effect of MSS integrated in daily care. There was more improvement in several specific types of behavior, in the mood of the residents [26], and in communicational interaction between the residents and care staff within the sessions [28] among those in the experimental group than in the control group, who were provided with the usual care. In short, the immediate and short-term effect of providing Sensory Stimulation (SS) to older people in the later stages of dementia is promising. Therefore, SS activities which are integrated into daily care may not only fulfill the unmet needs of people with dementia for environmental stimulation, but also for daily social interaction [29]. Thus, the effect on the residents is likely to be long-lasting.
As integrating sensory stimulation care in daily practice involves changing the care practices of staff in nursing homes, the staff are most likely to be fear and uncertain with changes, resulting in their resistance to such changes. Thus, our research team designed such care for care staff to provide while managing care staff’s change in their daily practice through action research approach.
Study Objectives
1. Elicit the process of changing care staff’s practice in sensory stimulation care
2. Development of a sensory stimulation-oriented care which is integrated in daily practice
Methods
Study design
We adopted action research for this study. Action research is a process of self-reflection and evaluative inquiry conducted by participants who are “actors” engaging in an “action” to change an “action” by improving or refining it. Unlike other research methodologies, the major characteristics of action research are participation and democratic impulse [30] Participants perceive the need to change and are willing to play an active part in the change, and they, not the researchers, will lead the change. The process of action research is a bottom-up approach that allows direct communication and open discussion among the participants (care staff participants and family caregiver participants) to enhance their understanding of the change. It also allows them to become involved in identifying problems and planning, implementing, and evaluating the change, and provides a sense of ownership to the participants. All of these are principles for managing changes in organizations. The participants will ultimately decrease their resistance to change, resulting in increased acceptance of the change [30,31]. A number of authors have recognized the potential of action research in the development of care practices through changes [31,34], as well as in the implementation of research findings [35,36].
Setting and sample
We used purposive sampling, residents and their family members, and various types of care staff from a nursing home in Hong Kong. The nursing home (1) was operated by a Non-Governmental Organization (NGO), (2) perceived a need for a change in care of residents with later stage of dementia and (3) was willing to play an active role in improving the care. There were three resident participants who were aged 65 or above, suffered from moderate to severe dementia as diagnosed by medical officers, and at stage 5 or 6 of the Functional Assessment Staging Test (FAST), but with no additional diagnosis of a psychiatric nature (Table 1). Three family member participants were the primary caregivers of the three resident participants, and they visited the resident participants at least twice a week. The care staff participants were professional nurses, health care workers, personal care workers or service assistants who had opportunities to care of these three residents. All of the participants voluntarily took part in the study. There were only three resident participants in this study because the nursing home wanted to preliminarily try this programme to see the acceptance of the residents and the care staff and hoped to develop this programme for future adoption.
Cases
Age
Gender
Marital status
Behavior associated with dementia
1
98
Female
Widow
-Suspicious, used to complain about being beaten up and having her things stolen.
- She had become more withdrawn in recent years.
-Easily irritated.
2
85
Female
Widow
-Always complained of tiredness, usually stayed in bed.
3
92
Female
Widow
-Being isolated and reluctant to join in group activities.
Table 1: Profile of the residents.
Ethical consideration
This research was carried out in accordance with The Code of Ethics of the World Medical Association (Declaration of Helsinki). Ethical approval to conduct this study was obtained from the Ethics Review Sub-Committee of the University of the first author in this paper (HSEARS20140413001). Written, informed consent to participate in this study was obtained from the three primary family caregivers of the three residents with moderate to severe dementia for their own participation and their three residents’ participation, and also from the care staff in the nursing home. The participants had the right to refuse the participation in this study, response to any questions to be asked and also quit the study anytime without any penalty. Confidentiality and anonymity were assured.
Procedures
Two action research cycles to plan, implement and evaluate the sensory stimulation care which was integrated to daily practice were carried out. The details of the procedures were described below (Figure 1).
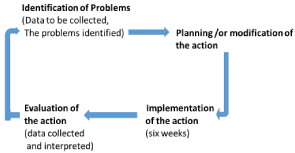
Figure 1: The Action Research Cycle.
A. The first action research cycle: An action research cycle involves several cyclic steps which are identification of problem, planning, action, evaluation (data collection and analysis) and selfreflection. This study had two action research cycles implemented. There were several stages for each cycle, which was described below.
The data collected for identification of the problems of caring residents with later dementia: The nursing home in this study delivers care to residents who are frail and have physical and/or cognitive impairment, and require a moderate to high level of care. The first author and the trained RA using the interview guidelines conducted three focus group interviews with a professional group (one registered nurse, two enrolled nurses),a non-professional group (one health workers, two personal care workers and one service assistant) and family member group (three family caregivers of the three resident participants). In the interviews, the care staff participants discussed the care currently delivered to residents with moderate to severe dementia, the observed benefits, the difficulties/barriers involved, expectations for the care they delivered, and their suggestions for improvements to the current approach to care. With the agreement of the participants, all the interview contents were audio-recorded were transcribed. Moreover, three hours of field observation were carried out by the trained RA to observe the residents’ responses to sensory stimulation and how care staff communicatively interacted during daily care with those residents who suffer from moderate to severe dementia.
Forming the action team: An action team was assembled that included one representative from registered nurses, one from enrolled nurses, one from health workers, two from personal care workers, one from the service assistants and the first author of this study. This action team was responsible for reviewing and interpreting the results, identifying the problems and issues regarding the SS care and then planning, evaluating and modifying the care in each action research cycle.
The problems identified: Based on the results from the data collected in the focus group interviews and the field observation, the action team identified that (1) personalized care to residents with moderate to severe was an area that needs to be improved, (2) promoting sensory stimulations and social interactions to the residents with moderate to severe dementia was necessary for improving the care, (3) the non-professional care staff including HWs, PCWs and service assistants had insufficient knowledge and skills in dementia care, communication with residents with dementia, and SS care.
Planning the actions: With the problems identified, the action team discussed how to plan the actions to manage the problems. The team agreed to increase sensory stimulation and social interactions with residents with moderate to severe dementia. The first author shared with the team members about the research results on sensory stimulations to demented older people and the preliminary idea about integrating sensory stimulations to daily care, to have a continuous effect. The team members tentatively supported this idea. The members discussed the amount of time and manpower that would be needed, the knowledge and skills of the care staff, the nature of the sensory stimulus, and ways of integrating SS into daily care.
The action team held a meeting to inform all care staff in the nursing home about the integration of SS care into daily practice. Many staff members were concerned about the amount of time and manpower required to deliver this care. They were worried that they did not possess enough knowledge and skills to give such care, and that the paperwork involved would increase their workload. The action team emphasized that the care staff was allowed to continuously comment on and modify the care until it appeared feasible and acceptable to them. Finally, in the meeting, it was decided that such care would be provided to three residents with moderate to severe dementia in the first phase to see the comments from the care staff and their family members. The team further explained what they would do to prepare care staff to implement this care.
The team finally agreed on a nursing process and preferencebased approach to assess, plan, act upon, and evaluate the sensory stimulus given to individual residents during the daily care. Therefore, the care protocol for the care staff to use was designed. It is included four steps namely, assessment of residents’ preferences in food/drink, activities, hobbies etc and planning, implementing, and evaluating the SS integrated in daily care. The protocol guides different types of care staff to carry out different tasks at the required time in each step. Moreover, a list of suggested sensory stimuli integrated into daily practice was drawn up, referencing previous studies and Chinese culture and custom, for the care staff to use in planning the sensory stimulation activities. A communicative interaction guide were designed based on the previous studies [33-34], and the results from the focus group interview with the staff members and the family members for care staff’s reference to communicate with the residents with dementia while performing the SS activities which are planned. Through referencing previous studies [20,30,32], the team designed all of the required forms that are simple and user friendly.
In order to enhance staff members’ knowledge and skills on dementia care and SS care, the first author conducted the two-hour seminar for the care staff, including nurses, health workers, personal care workers, and service assistants. Topics discussed in the seminar included an introduction to dementia, skills for communicating with residents with dementia, the importance and effectiveness of sensory stimulation, and knowledge and skills on integrating sensory stimuli into daily care. Besides, the protocol, the list of suggested sensory stimuli, the communicatively interaction guide and the required forms were demonstrated how to use in the implementation of the SS care.
Action implementation of the SS care integrated in the daily care: A group of care staff including a registered nurse, an enrolled nurse, a health worker, two personal care workers and one service assistant was assigned to deliver the SS care which was integrated in daily practice. Adopting the care protocol, the nurses or the health workers assessed each resident participant’s previous and current preferences with regard to activities, food, drink, materials, and people by observing the residents and questioning their family caregivers and other care staff members. Based on this assessment, they planned the SS activities and integrated them into daily care.
The planned activities were wide-ranging, and included the ‘paigow’ card game; the red card game, mahjong, limb massage, movie appreciation, personal grooming, and ‘yum cha’ (going out to eat dim sum) and visiting a wet market. Most of the activities were planned for all three residents, while four activities (namely, mahjong, the paigow card game, the red card game, and visiting a wet market) were planned for designated cases, in accordance with the preferences of the participants. A summary of the SS activities is given in Table 1. According to the planned activities, the health worker, the personal care workers and the service assistant carried out the activities for the residents. The three residents were stimulated in terms of their sense of vision, smell, hearing, taste, and/or touch and their pleasant memories were recalled through their participation in the SS activities. Moreover, the care staff prompted the residents to interactively communicate with the activities during the implementation of the activities.
The implementation of this SS care lasted six weeks. The nurses or health workers conducted the evaluation once every two weeks. They collected feedback from the two personal care workers and the service assistant on the residents’ acceptance and responses to the SS activities which they provided. Three evaluations indicated that the residents well accepted the SS activities so they were not modified during this 6-week implementation.
Evaluating the action: After the SS care had been implemented for six weeks, an action research evaluation was conducted. In the evaluation stage, the first author together with the trained RA using the interview guideline conducted three face-to-face individual interviews with three family caregiver participants. Moreover, theyalso conducted two focus group interviews with the group of care staff (one registered nurse, one enrolled nurse, one health worker, two personal care workers and one service assistant) who were responsible for provision of the SS care to the resident participants and the group of other care staff (one registered nurse, one enrolled nurse, two health care workers, two personal care workers and one service assistant ) who had opportunities to provide other daily care activities to the resident participants. In the interview, the participants were encouraged to voice their observations on the residents, views on the SS care and suggestions to improve it. Upon their agreement, the interviews were all audio-recorded for transcriptions and data analysis.
Self-reflection modification of the action: The action team interpreted the results and discussed the modification of the SS care. With the agreement of all of the members, the limb massages were increased to three times a week and the yum cha activity to once a week because the residents liked these activities most and the nursing home could afford the manpower for this change. Moreover, some other residents without dementia were invited to join the mahjong games, card games, and paigowpoker games because the atmosphere became more joyful as the number of participants increased. The family caregivers were also encouraged to join the activities along with the changes.
B. The second action research cycle
The modified SS care was then implemented again in the 2nd cycle as the 1st cycle. The 2nd cycle of the implementation also lasted for six weeks. Upon completion of the second cycle of the implementation, individual and two focus group interviews were conducted again as in the first cycle. Overall, the results on resident participants in the second round of interviews were similar as those in the first round of interviews. Although the participants did not offer any other feedback on improving the SS care in these second round of interviews, the care staff emphasized that if full implementation of this care to all residents with moderate to severe dementia in the nursing home, sufficient manpower and resources should be ensured for its successful implementation.
Data analysis
Nvivo software (version 10) was adopted to conduct qualitative content analysis of the data collected from two rounds of focus group interviews and individual face-to-face interviews for identification of the sub-themes and themes from the interview and the field observation data in this study. The first author and the RA independently reviewed all of the data. Both of them then met to came up with a framework for analyzing the interview data. Based on the framework, they identified codes and developed sub-themes and themes independently and then let the research team members review the whole data analysis. The discrepancies were identified and discussed to finalize the sub-themes and themes. The sub-themes, themes and representative verbatim were translated in English and then backward translated were done to confirm the accuracy of the translation.
Results
All three residents were female, widowed, and in the category of the oldest-old (aged between 85 and 98 with the mean age of 92. They all had behavior associated with dementia (Table 2). All three family caregivers were the daughters of the three residents. They were housewives and visited their mothers frequently ranged from once every day to three times a week.
Multiple sensory stimulation activities
Frequency for the activities to be carried out
Primary senses to be stimulated
Cases
Red card game
(Traditional Chinese game)
Twice a week, 1 hour per session
Vision, hearing
Case 1
Paigow poker
(Traditional Chinese gambling game)
Twice a week, 1 hour per session
Vision, hearing
Case 2
Visits to a wet market (This resident participant had been a fish monger in the market.)
Once every two weeks, 30 minutes per session
Vision, Olfaction, Hearing
Case 2
Mahjong
Twice a week, 1 hour per session
(before sleep)
Vision, Hearing
Case 3
Limb massage
Two times a week, 30 minutes per session
Olfaction, Touch
All
Movie appreciation
Once every week, 30 minutes
Vision, Hearing
All
Yum cha
(Chinese dim sum)
Once every two weeks, 3 hours per session
Vision, Hearing, Taste
All
Personal grooming (Applied moisturizer and balm on the residents after the morning shower, and massaged their limbs.)
Every morning after a shower
Olfaction, Touch
All
Table 2: Sensory stimulation activities integrated to daily practice.
Through the triangulation of the data from the care staff and the family members, the themes and sub-themes were identified (Table 3). Overall, they found positive changes of the resident participants in behavior (reduction in agitated behavior, decrease in suspicion), psychological wellbeing (increase in positive emotional responses) and social wellbeing (Increased social interaction with care staff and residents, improved motivation to engage in activities) from the SS care. The care staff also reported that having more connection with the residents, having appreciation from the residents, receiving appreciation from family members for their good care delivered, having good support from the family members and improved wellbeing of the residents are their driving force behind their good care delivered.
Themes
Sub-themes
Verbatim of family member
Verbatim of care staff
1. Behavioural change of residents
1.1. Reduction in agitated behavior
My mom (Case 1) used to scold others a lot�. Maybe it is the effect of the program, but no negative things have happened recently to provoke her. I seldom see her scolding others like she did before�.
- She (Case 1) used to babble a lot, scolding herself and xx (another resident), frequently talking to herself, but this has decreased greatly.
- Her (Case 2) temper has improved a lot. She doesn’t scold others as much as before�.
- Case 3 has a better temper now. Before she would scold us when we woke her up for mealtimes. Now, she will let us feed her several spoonfuls without losing her temper�.
1.2. Decrease in suspicion
I found that she (Case 3) complained less about being beaten by others. Before, she dressed up and sat in the common area and said that she wanted to see who would come out to beat her up� She also said that someone would bring her to mainland China �and also that someone wanted to harm us (herself and her family members)� Now, she has become less abusive when talked to�.
When she (Case 2) sits there and rests � she shares her food with others, and doesn’t accuse others of beating her up and/or stealing things from her�.
2. Psychological change of residents
Increase in positive emotional responses
- She (Case 1) appeared happier after she started playing red card game. Whenever she talks about it, she smiles�.
- My mom (Case 2) is more calm, she smiles when we talk about the paigow card game�.-
- My mom (Case 3) is happier, as she can go out to yum cha and engage in different activities. �.
It is obvious that their mood is more stable after participating in the activities. Maybe these activities occupy their time.... They are more cheerful now as there are more activities to engage them. It’s better than just sitting there all day long.
3. Social change of residents
3.1. Increased social interaction with care staff and residents
Unlike before, I had to ask her many times, now she (Case 3) actively tells me what she wants to eat and asks me to get it for her. She told me that she wanted “Phoenix talons” when we went to yum cha
When she (Case 2) sit there and rests, she chats with the neighbouring residents. Previously, she did not talk to the residents in her bedroom, but now communicates verbally with them�. When I asked her (Case 2) which part of the wet market she wanted to go to, she actively shared with me what snacks and fruits she wanted to buy�. Now, she (Case 2) sits and stays alert, and initiates conversations with the staff. She even asks about the schedule of different activities and actively shares which activities she had joined in before
3.2.Improved motivation to participate in activities organized by the nursing home
Case 2 has the greatest improvement. Before the SS activities, she usually stayed in bed and complained of tiredness�. Now, she proactively asks when we will have card games, when we will go for yum cha, and when we will go to the wet market� When they are happy, we feel contented. They do not only become more cheerful, but also tend to refuse less when we try to engage them in some other activities, such as taking part in physical exercise.
4. Increased job satisfaction of care staff
4.1 Having more connection with the residents
When I massaged them, we had more interactions than before. Like Case 2, after helping to massage her, she said thank you. This interaction is meaningful and makes me feel more connected with her.
4.2 Having appreciation from the residents
She (Case 2) shared food with me; after going out with her, she said I should have bought you some biscuits. She is more proactive in showing her appreciation.
4.3 Receiving appreciation from family members for the good care delivered
They (family caregivers) say that we (the team) are hard working. They are very understanding. This make us happy because they (the family caregivers) gave us positive feedback�. The family caregivers told us what they had observed us doing for the residents, they were moved and burst into tears. They said that the way that we care for the residents is very touching
4.4. Having good support from the family members
When I called the family caregivers to ask them to join the yum cha activity for the residents, they (family caregivers) had some other commitments planned already, but they still tried to re-arrange their own schedules in order to join the activity�. They try their best to match our activity schedule�. I realize that the family caregivers try to cooperate with us. They give us good support and compromised a lot�. It’s a win-win situation
4.5 Improved wellbeing of the residents
When we see them become happier and more responsive, we feel very glad and satisfied�. I feel that the effort that we put in has not been wasted. It is rewarding�. It is a bonus to see their responses and their improvements meeting our expectations
Activities were organized three or four times out of five days, and the staff members are very responsible. I asked one of them if that would be too much for a burden for her (the staff caregiver). she admitted that it was, but said that she saw that the residents had improved, so she would strive hard to run the activities.
Table 3: Themes and sub-themes identified from the 1st and 2nd round of the interviews with family members and care staff.
Discussion
Development of the SS care integrated to daily practice
Through this action research study, the process of changing the care staff’s practice in sensory stimulation care in the nursing home has been discussed above in details. This bottom-up approach allowed the care staff took the lead to change their practice and finally develop this new model of care. They had the opportunities to plan, act, evaluate and modify the SS care which allowed them to have sense of ownership in this change. Moreover, through the training and provision of the SS care, the care staff was empowered in the areas of interactively communication and sensory stimulation in dementia care. At this end of the second action research cycle, the SS care was finally developed. This study has found the preliminary impact of the SS care integrated in daily practiceon the residents and the care staff. It also further added evidence in the contribution of action research to changing care practice and developing new practice as reported in the previous studies [31-34].
Changes in the behavior and psychosocial wellbeing of the residents
The family members and care staff observed some positive changes in behavior and psychosocial wellbeing. Kitwood and Bredin emphasized the importance of personhood in developing care practices for people with dementia [37]. Personhood is the key concept of this programme, with the SS activities being individually planned according to the residents’ preferences, habits, and interests. Personhood is further addressed by giving the residents choices of different activities. For example, the residents were allowed to choose the scent of the massage oil and body balm. The residents were thus willing to participate in these personalized activities, which were tailor-made for them.
In response to the stimulation, a decrease in agitated behavior and suspicion coupled with positive emotional responses from the residents were observed in this study, a finding supported by previous studies [15,17-21,23,24, 26]. The SS activities created pleasurable experiences that improved the mood of the residents and also reduced their level of agitation. The residents were more calm and relaxed during the period of receiving the SS care. Hansen suggested that massage and touch are effective supplements to other treatments in reducing behaviors’ associated with dementia, such as anxiety, agitated behavior and depression [38].
It was also observed that the residents had more social connection with staff caregivers, family caregivers, and other residents in this study. This finding is similar to that of previous studies, which found increased verbal communication from participants with dementia. Those staff care givers had more opportunities to interactively communicate with the residents while they implemented the MSS activities [17,28]. In addition, the activities were of a nature that allowed the family and staff caregivers to find topics to interactively communicate with the residents, especially when they involved outings such a visits to a wet market or going to yum cha. These were highly stimulating activities that engaged the attention of the residents and prompted them to talk about activities that they had liked before. Recalling pleasant memories of past events caused them to initiate conversations with the people around them, including staff and family caregivers and other residents. These were likely the reasons why the residents formed more social connections. The residents’ mood improved, and they became less agitated. Being calmer and more relaxed also made them more approachable, which facilitated social interactions with the people around them.
The SS activities for example, majhong, red card games, paigow poker required the participants to pay attention and use their minimal cognitive resources. The residents had liked these activities very much when they were young. It was observed that they were able to play these games and enjoyed them very much, regardless of the cognitive demands on them. This suggests that older people with moderate to severe dementia can maximize their cognitive functions when they participate in activities that they had often engaged in and enjoyed in the past.
Changes in the care staff
The SS care is a personalized approach of care so it likely increases care staff’s workload. The care staff admitted that their workload was increased but they still could deliver the good SS care to the residents. The driving force behind their good work was improved wellbeing of the residents, having more connection with and appreciation from the residents and receiving appreciation and good support from the family members. Improved wellbeing of the residents let the care staff believe that the SS care is beneficial to the residents. As the care staff had been well trained before implementing the care, they were able to effectively initiate conversions with the residents and carry out the SS activities causing them to be well accepted by the residents. As the residents liked the activities, they were grateful to the care staff for providing the enjoyable SS activities. In addition, the residents showed better compliance with the staff members’ instructions to participate in other activities, physical exercise which much reducing the tension between care staff and the residents.
The staff caregivers received appreciation and support from the family caregivers for their good work. The family members were involved in some activities such as yum cha, and card games when they accompanied the residents. This participation allowed them to more closely observe and more actively interact with the care staff, which gave the family caregivers a better understanding of how the care staff delivered care to the residents. When they observed improvements in the residents’ behavior and psychosocial wellbeing, they recognized and appreciated the staff members’ efforts and good work and also well cooperated with the care staff.
All these discussed above led to a virtuous cycle. Observing the benefits of the SS care to the residents and care staff, the care staff made great efforts to carry out the SS activities, which resulted in more improvement to the wellbeing of the residents and more appreciation from the residents and family members. The accumulation of this improvement and the appreciation will most likely motivate care staff to continuously provide quality care to nursing home residents.
Acceptance of residents, family members, and care staff
This SS care was well received by the residents who enjoyed the SS activities and the family members accepted this care because of their observed positive changes of their mothers in behavior and psychosocial wellbeing. In the case of the care staff, they accept it on the condition that sufficient resources are provided, although they found this care to be good for the residents and themselves. Personalized care requires more resources in time, materials, and manpower for delivery. Inadequate resources in some nursing homes will most likely constrain their ability to sustain such care. To ease the use of resources, it is recommended that nursing homes mobilize family caregivers and/or volunteers to assist in carrying out the SS activities, but that these individuals should be well trained beforehand.
Implications for practice
Although there were only three residents as the study participants in this study, the contribution of an action research approach to changing care staff’s practice and development of the SS care was illustrated. The benefits of the SS care to residents and staff caregivers have been noted in this study. If the sensory stimulation and social interactions are integrated into daily care and continuously implemented, it is believed that such care will continuously benefit both the residents and care staff. This care model is thus highly recommended for nursing homes’ consideration to adopt not only for SS care but also for changing other care practices.
Limitation
The major limitation is the small sample size from a nursing home that largely decrease the transferability of the study findings. It is thus strongly recommended to conduct a feasibility test with more elderly participants with both genders from more nursing homes to test the feasibility and staff acceptance of this SS care and also its preliminary effect.
Conclusion
The sensory stimulation care integrated to daily practice for nursing home residents with moderate to severe dementia was developed through an action research approach. Preliminary evidence has been provided that it has a positive impact on the residents and the care staff and was also overall accepted by the residents and their family caregivers and the care staff in the nursing home. As personcentered care is the emphasis of this type of care, it is necessary to consider strategies to ensure sufficient resources and manpower for its sustainability. Although this sensory stimulation care was only carried out to three residents in this action research, the process and outcomes of this change can be taken as preliminary work for designing future quantitative studies with large sample size to test the effect of this SS care integrated to daily practice.
Role of the Funding Source
This study was funded by Departmental Research Fund, School of Nursing, and the Hong Kong Polytechnic University. This funding was used by the research team to carry out this study. However, the funding source had no involvement in study design, the data collection, data analysis and interpretation of data, writing of the report and in the decision to submit the article for publication.
Acknowledgement
Our research team acknowledges the contribution of Ms Poman Wong who is our research assistant to data collection and data analysis for this paper.
References
- Alzheimer’s Association. 2012 Alzheimer’s disease facts and figures. Alzheimer’s Dement. 2012; 8: 131-168.
- Census & Statistics Department. Thematic household survey report no. 40: social-demographic profile, health status and self-care capability of older persons. Hong Kong: Census & Statistics Department. 2009.
- Yu R, Chau PH, McGhee SM, Cheung WL, Chan KC, Cheung SH, et al. Trends in prevalence and mortality of dementia in elderly Hong Kong population: projections, disease burden, and implications for long-term care. Int J Alzheimers Dis. 2012: 1-6.
- Finkel SI, Burns A, Cohen G. Overview. Int Psychogeriatr. 2000; 12: S13-18.
- Verhey FRJ, Rozendaal N, Ponds RWHM, Jolles J. Dementia, awareness and depression. Int J Geriatr Psych. 1993; 8: 851-856.
- Kwong EWY, Lai LKY, Tse M, Liu J, Wong, A. Care for nursing home residents with moderate to severe dementia: perception of formal and informal caregivers. Hong Kong College of Gerontology Nursing, the 7th Scientific Meeting Cum 16th AGM. 2013.
- Clare L. Awareness in people with severe dementia: review and integration. Aging Ment Health. 2010; 14: 20-32.
- Cerejeira J, Lagarto L, Mukaetova-Ladinska EB. Behavioral and psychological symptoms of dementia. Front Neurol. 2012; 3: 1-21.
- Ballard C, Neill D, O’Brien J, McKeith IG, Ince P, Perry R. Anxiety, depression and psychosis in vascular dementia: prevalence and associations. J Affect Disorders. 2000; 59: 97-106.
- Brodaty H, Burns K. Nonpharmacological management of apathy in dementia: A systematic review. Am J GeriatPsychiat. 2012; 20: 549-564.
- van de Glind EMM, van Enst WA, van Munster BC, OldeRikkert MGM, Scheltens P, Scholten RJPM, et al. Pharmacological treatment of dementia: a scoping review of systematic reviews. Dement GeriatrCognDisord. 2013; 36: 211-228.
- American Psychiatric Association. Practice guideline for the treatment of patients with Alzheimer’s disease and other dementia. Am J Psychiat. 2007; 164: S5-56.
- Baker R, Bell S, Baker E, Holloway J, Pearce R, Dowling Z, et al. A randomized controlled trial of the effects of multi-sensory stimulation (MSS) for people with dementia. Brit J Clin Psychol. 2001; 40: 81-96.
- Baker R, Holloway J, Holtkamp CCM, Larsson A, Hartman LC, Pearce R, et al. Effects of multi-sensory stimulation for people with dementia. J AdvNurs. 2003; 43: 465-477.
- Milev RV, Kellar T, McLean M, Mileva V, Luthra V, Thompson S, et al. Multisensory stimulation for elderly with dementia: A 24-week single-blinded randomized controlled pilot study. Am J Alzheimers Dis Other Demen. 2008; 23: 372-376.
- Anderson K, Bird M, MacPherson S, McDonough V, Davis T. Findings from a pilot investigation of the effectiveness of a Snoezelen room in residential care: should we be engaging with our residents more? GeriatrNurs. 2011; 32: 166-177.
- Marques A, Cruz J, Barbosa A, Figueiredo D, Sousa LX. Motor and multisensory care-based approach in dementia: long-term effects of a pilot study. Am J Alzheimers Dis Other Demen. 2013; 28: 24-34.
- vanDiepen E, Baillon SF, Redman J, Rooke N, Spencer DA, Prettyman R. A pilot study of the physiological and behavioural effects of Snoezelen in dementia. Br J OccupTher. 2002; 65: 61-66.
- Baillon S, Van Diepen E, Prettyman R, Redman J, Rooke N, Campbell R. A comparison of the effects of Snoezelen and reminiscence therapy on the agitated behaviour of patients with dementia. Int J Geriatr Psych. 2004; 19: 1047-1052.
- Minner D, Hoffstetter P, Casey L, Jones D. Snoezelen activity: the good shepherd nursing home experience. J Nurs Care Qual. 2004; 19: 343-348.
- Ward-Smith P, Llanque SM, Curran D. The effect of multisensory stimulation on persons residing in an extended care facility. Am J Alzheimers Dis Other Demen. 2009; 24: 450-455.
- Sanchez A, Millan-Calenti JC, Lorenzo-Lopez L, Maseda A. Multisensory stimulation for people with dementia: a review of the literature. Am J Alzheimers Dis Other Demen. 2013; 28: 7-14.
- Cornell A. Evaluating the effectiveness of Snoezelen on women who have a dementing illness. Int J PsychiatrNurs Res. 2004; 9: 1045-1062.
- Staal JA, Sacks A, Matheis R, Collier L, Calia T, Hanif H, et al. The effects of Snoezelen (multi-sensory behavior therapy) and psychiatric care on agitation, apathy, and activities of daily living in dementia patients on a short term geriatric psychiatric inpatient unit. Int J Psychiat Med. 2007; 37: 357-370.
- Chung JC, Lai CK, Chung PM, French HP. Snoezelen for dementia. Cochrane Database Syst Rev. 2002.
- Van Weert JCM, Van Dulmen AM, Spreenwenberg PMM, Ribbe MW, Bensing JM. Behavioral and mood effects of snoezelen integrated into 24- hour dementia care. J Am Geriatr Soc. 2005; 53: 24-33.
- Vernooij-Dassen M, Vasse E, Zuidema S, Cohen-Mansfield J, Moyle W. Psychosocial interventions for dementia patients in long-term care. Int Psychogeriatr. 2010; 22: 1121-1128.
- vanWeert JCM, van Dulmen AM, Spreeuwenberg PMM, Ribbe MW, Bensing JM. Effects of snoezelen, integrated in 24 h dementia care, on nurse-patient communication during morning care. Patient EducCouns. 2005; 58: 312-326.
- Cohen-Mansfield J. Use of patient characteristics to determine nonpharmacologic interventions for behavioural and psychological symptoms of dementia. IntPsychogeriatr. 2000; 12: 373-380.
- Munten G, van den Bogaard J, Cox K, Garretsen H, Bongers I. Implementation of evidence-based practice in nursing using action research: a review. Worldviews Evid Based Nurs. 2010; 7: 135-157.
- French. Evidence-based nursing: a change dynamic in a managed care system. J NursManag. 2000; 8: 141-147.
- Ullrich S, McCutcheon H, Parker B. Reclaiming time for nursing practice in nutritional care: outcomes of implementing protected mealtimes in a residential aged care setting. J ClinNurs. 2011; 20: 1339-1348.
- Rowley J, Taylor B. Dying in a rural residential aged care facility: an action research and reflection project to improve end-of-life care to residents with a non-malignant disease. Int J NursPract. 2011; 17: 591-598.
- Lea E, Andrews S, Hill K, Haines T, Nitz J, Haralambous B, et al. Beyond the ‘tick and flick’: facilitating best practice falls prevention through an action research approach. J ClinNurs. 2012; 21: 1896-1905.
- MacGuire JM. Putting nursing research findings into practice: research utilisation as an aspect of management of change. J AdvNurs. 1990; 15: 614- 620.
- Dyess SM, Boykin A, Bulfin MJ. Hearing the voice of nurses in caring theorybased practice. NursSci Quart. 2013; 26: 167-173.
- Kitwood T. The technical, the personal, and the framing of dementia. SocBehav. 1988; 3: 161-179.
- Hansen NV, Jorgensen T, Ortenblad L. Massage and touch for dementia. Cochrane Database Syst Rev. 2006.