
Special Article - Geriatric Care Nursing
Gerontol Geriatr Res. 2021; 7(3): 1058.
A Comparison between Independently Living Elderly Individuals and Residents in 25 German Nursing Homes Following the Group-Living Principle
Simon A*
School of Health Sciences & Management, Baden-Wuerttemberg Cooperative State University, Stuttgart, Germany
*Corresponding author: Anke Simon, School of Health Sciences and Management, Baden-Wuerttemberg Cooperative State University, Stuttgart, Germany
Received: May 21, 2021; Accepted: June 18, 2021; Published: June 25, 2021
Abstract
Objective: The purpose of this study was to analyses the subjective Quality of Life (QoL) perceived by older people in German nursing homes following the group-living principle.
Methods: The Nottingham Health Profile (NHP), a health-related QoL measuring instrument, was employed in 25 nursing homes (n=404 participants). A comparison with a national German representative subsample of independently living elderly individuals (age group over 75) was conducted. Psychometric properties and appropriateness were analyzed.
Results: Our findings indicate an acceptable perception of residents’ QoL. The mean NHP scale scores show that except for the NHP subscale physical ability, the perceived QoL of residents in group-living nursing homes reached nearly the same level as that of independently living elderly individuals (national German reference values, age group over 75 years). QoL-related results on life satisfaction and feeling of happiness confirm the NHP findings. The protocol from a preliminary pilot study could be replicated according to good scientific practice.
Conclusions and Implications: The report presents the first major investigation in the field of subjective quality of life in group-living nursing homes. The study focused on people over 75 years of age with age-specific reduced physical and mental abilities. The NHP should also be considered a reliable, valid and appropriate instrument for older people. Due to the lack of research on residents’ perspectives, further studies should establish age-specific and care setting specific reference data for nursing home residents. In particular, more research is needed to answer the question of which care setting best meets people’s essential needs in older age.
Keywords: Quality of life; Empirical study; Nursing homes; Group-living principle
Abbreviations
Diff: Difference between Mean Values; EL: Energy Loss; ER: Emotional Reaction; EQ-5D: Euro Qol-5 Dimension; f: Female; FH: Feeling of Happiness; HUI: Health Utility Index; LS: Life Satisfaction; M: Mean Value; m: Male; NHP: Nottingham Health Profile; OECD: Organization for Economic Cooperation and Development; P: Pain; PM: Physical Mobility; QoL: Quality of Life; S: Sleep; SD: Standard Deviation; SF-36: Short Form Survey 36; SF-6D: Short-Form Survey Six-Dimension; SH: Status of Health; SI: Social Isolation; a: Internal Consistency (Cronbach’s alpha); rtt: Split-Half-Reliability (Spearman- Brown).
Background
Group-living care settings have evolved as a reaction to critical public opinion regarding the hospital-like environment of traditional nursing homes. The concept originated in Sweden and was later introduced in other countries, such as the Netherlands [1], Great Britain [2], France [3], and Japan [4]. Although group-living, home-like nursing homes have been established as an alternative to traditional nursing homes (settings) for many years, there is no generalized definition of the term “group-living nursing home”, but common principles and concepts related to this model include:
• Archetypical nursing homes consist of several group-living units with up to 15 residents living together in each unit.
• Nursing homes provide home-like environments as much as possible.
• An individual space, either a small private apartment or a one-room unit, is provided for each resident. Additional large dayrooms/lounge kitchen areas serve as a shared space, where the majority of daytime is spent together with other residents.
• The idea of ‘active ageing’ is implemented, allowing as much privacy and independence as possible. Comparable to the residents’ former homes, no centralized food and no centralized washing service are provided.
• A mixed care team (an educated care-giver per unit and nursing staff and voluntaries per nursing home) compensates for declining ability and vitality in the residents and lowers the burden for family care.
• A mix of residents (with psychogeriatric complaints, i.e., dementia, and with somatic, physiological ailments) live together.
In public opinion, conventional nursing homes are often associated with single-sided thoughts, such as the last stage before death, poor Quality of Life (QoL) and loss of independence. The implemented German standard assessment instrument for external mandatory evaluation of nursing homes, based on the German Care Transparency Act (§ 115 Abs. 1a SGB XI), mainly focuses on the evaluation of objective quality indicators, primarily structure and process quality attributes. Critical discussions among health scientists, health professionals and health politicians about methodological issues and the lack of outcome criteria led to a recent revision that was introduced in December 2019 [5-9]. Although the newly revised German assessment instrument covers essential outcome quality criteria such as the prevention of mobility loss, independent maintenance of daily activities, and unintended weight loss, and solves most of the mentioned issues, the viewpoint of the residents is still not included.
Current research proposes the implementation of quality of life measurements to cover residents’ viewpoints on care [5,10-16]. To date, only a few studies investigating subjective quality of life in older people can be found. They mainly focus on older, multi-morbid patients without dementia [5,17,18], address patients with dementia partly in special settings [14,15,19-23], and consider care-related measures for nursing home residents [10,16,24]. According to our research, there is still a complete lack of studies on group-living nursing home residents in Germany and elsewhere, apart from one preliminary pilot study published in 2013. In Simon et al. [25], we researched certain quality of life measurements according to the following criteria: a) dimensions that included aspects of physical and mental well-being, social relations and daily life appropriate for the tar-get group of nursing home residents [26], b) validation as paper & pencil questionnaires and face-to-face interviews, and c) the availability of nation-wide age-specific reference values. The selection process included generic profile-based instruments (i.e., Short Form Survey 36/SF-36 and Nottingham Health Profile/NHP) and preference-based measures with a single-dimension index score (i.e., Short Form Survey Six Dimension/SF-6D, Health Utility Index/HUI, EuroQol-5 Dimension/EQ-5D). During the preliminary investigation in 2013, a questionnaire appropriate for elderly individuals could be validated. Descriptive findings in seven nursing homes indicated an acceptable quality of life.
The study presented here has two objectives. Our main intention is to measure residents’ subjectively perceived quality of life in group-living nursing homes. The second aim of our investigation is to replicate our preliminary study results as well as to implement a research protocol [25] according to good scientific practice.
Quality of life was assessed by using the Nottingham Health Profile [27]. The NHP is one of the most commonly used generic scales for measuring health-related quality of life and has already been used in nursing home studies with frail elderly individuals [18,28]. The 38 items, formulated as direct statements, aim to identify self-assessed QoL impairments in six dimensions: physical mobility, pain, sleep, social isolation, emotional reaction, and energy level. Gunzelmann et al. [29] confirmed the psychometric validation of the German NHP version [30]. The authors provided age-specific reference values as a representative subsample.
Methods
Participants and data collection
This exploratory cross-sectional study included 25 group-living nursing homes in Germany and was conducted in January 2018. The care provider (private, non-profit organization) is one of the first to introduce group-living nursing homes in Germany. All 25 nursing homes in our sample homogenously follow the cooperative groupliving policy (as mentioned above). There-fore, the investigation was conducted in a standardized setting regarding aspects such as homogenous philosophy of care, similar building features and domestic characteristics, 10 to 14 residents per unit, standardized care concept and qualified mix of staff.
According to our study protocol [25], the inclusion criteria for selecting residents were as follows: living in nursing homes for more than three months and willingness and physical and mental ability to participate in the study. Residents with cognitive impairment, i.e., dementia, were not excluded for ethical reasons. Naturally, many of the residents in nursing homes suffer from various stages of dementia in different stages. They do, however, have the human right to freedom of expression. Nevertheless, nursing home head nurses pre-selected the target population regarding the general ability to understand and answer quality of life and health-related questions. As proposed in the preliminary pilot study, patients with severe depressive symptoms were excluded [25].
Data acquisition was accomplished by face-to-face interviews. Due to the special setting of nursing homes with bodily and cognitively impaired older people (including residents with dementia), we replicated our study design’s introduction procedure [25], comprising four well-prepared steps: (1) all investigators underwent a short training session on qualitative re-search methods and the interview guideline; (2) organized groups (two to three interviewers assigned to each nursing home) visited the related group-living units for two days; and (3) to gain natural contact with the residents, the investigators were introduced to the residents by the head care-giver very early with the start of the morning shift, i.e., they helped prepare breakfast and ate with the residents, assisted with the morning toilette and bed making; and (4) the investigators spent the entire two days together with the nursing home residents to create a familiar atmosphere. In this way, time pressure and uncomfortable situations could mainly be avoided. The nursing home residents and investigators decided freely when and where to perform the interview. The length of the interview was not limited. The investigators were allowed to explain the statements and scales if necessary or to read them aloud.
Questionnaire
The measurement tool was administered as a self-reported questionnaire [25]. A German version of the NHP [27] validated by Kohlmann et al. [30] and by Gunzelmann et al. [29] was used for the population of independently living people. The scale consists of 38 QoL items related to six dimensions using a binary (yes or no) scale. Residents confirmed each statement with “yes” (when there was a complaint or limitation, entered as 1) and denied it with “no” (when there was no complaint or limitation, entered as 0) regarding his or her (living) situation at the time of the interview. Following the calculation instructions [30], each ‘yes’ was weighed according to its importance in the dimension and scored between 0 (maximum quality of life) and 100 (no quality of life). The dimensions’ score was not calculated when the resident was unable to completely respond to the related items.
To compare our obtained data with the German reference values, we used a representative subsample of independently living people older than 75 years [25,29]. Furthermore, we added two QoL-related scales to the original pilot study protocol: the OECD life satisfaction scale (2017; single item scale from a minimum score of 0 to a maximum score of 10) and the feeling of happiness scale by Inglehart et al. [31] (Likert scale from 1 - not happy at all to 4 - very happy) and compared our findings with reference data provided by the OECD Better Life Index and the World Value Survey.
Following the original pilot study protocol, we included sociodemographic and health-related variables: age, sex, marital status, length of stay, current state of health (five-point Likert scale from 1 - very poor to 5 - very good), grade of dependency (German assessment standard Pflegegrad) and the AMT4 (shortened version of the Abbreviated Mental Test by Swain and Nightingale [32]).
Statistical analysis
The Statistical Package for the Social Sciences (SPSS), version 23, was used for all analyses. The descriptive results comprise the mean, standard deviation, frequency and percentage. Possible differences between the subsample residents older than 75 years of age and the German reference data of independently living older people were sex-specifically verified using the t-test. The NHP reliability analyses (internal consistency, split-half reliability) and the inter-correlation of the scales were replicated and reported according to our pilot study protocol [25]. Significance was set at the 5% level (p<0.05).
Results
Study population
Out of a total of 1577 residents in 25 nursing homes, 615 were physically and cognitively able to answer the questionnaire. A total of 404 of these residents participated in the study (response rate 66%). Reasons for declining were mainly due to a lack of interest, insufficient time, and absence during the time of interviews. Table 1 shows the baseline characteristics of the participating residents. Seventy-eight percent of the participants were female; the mean age was 84.6; the majority were widowed (76.7%). Approximately two-thirds of the respondents had lived in the nursing home for more than one year. Thirty-three percent of those tested had an impaired cognitive status. Most participants had been categorized as grade 2 or 3 de-pendency.
Characteristics
Participants
Sex
Male
87 (21.5%)
Female
317 (78.5%)
Age
Average
84.6
Standard Deviation
7.8
Range
47-102
Marital Status
Married/Living Together
39 (9.7%)
Married/Living Apart
2 (0.5%)
Single
37 (9.2%)
Divorced
11 (2.7%)
Widowed
310 (76.7%)
Not Available
5 (1.2%)
Length of Stay
<1 Year
146 (36.1%)
1-2 Years
101 (25.0%)
>2 Years
157 (38.9%)
Grade of Dependency
None
19 (4.7%)
Grade 1
6 (1.5%)
Grade 2
153 (37.9%)
Grade 3
172 (42.6%)
Grade 4
48 (11.9%)
Grade 5
3 (0.7%)
Not Available
3 (0.7%)
Cognitive Status
Not Impaired
269 (66.6%)
Impaired
135 (33.4%)
Table 1: Baseline characteristics of the participants.;
Quality of life
The mean NHP score over all scales (166.54, SD 94.04) was calculated first, followed by the mean scores of the six individual NHP scales. Figure 1 shows the nursing home residents’ subjective quality of life scores ranging between 0 (maximum quality of life) and 100 (no quality of life). As seen in Figure 1, the NHP scale social isolation scored the lowest (15.49), followed by the sub-scale emotional reaction (17.24), indicating residents’ high quality of life in those areas. In contrast, the NHP scale physical mobility had the highest score (45.66) and was thus perceived as the worst subjective QoL area. The NHP scales pain, sleep and energy loss show a score between those of the previous scales. Third, we compared our findings with those of the German reference group over 75 years of age, drawn from the abovementioned NHP national dataset. The national reference data set included only older people living independently (the sample does not include older people living in an institution). The comparative findings are shown in Table 2. The t-test identified only a few significant differences between elderly individuals living independently and group-living nursing home residents. The highest disparity was found in physical mobility. Nursing home residents were more affected by physical impairments and loss of mobility (mean score 46.02 for females, 44.17 for males) than independently living older people (mean score 27.01 for females, 22.22 for males). Women in nursing homes scored higher on pain (mean 27.78 versus 21.41) and on sleep than women living independently (mean 33.80 versus 27.90). No significant differences could be encountered for the NHP scale energy loss. Minor differences were found for both sexes’ emotional reaction scales and for men’s social isolation perception. The subsample of German reference data of independently living elderly individuals showed moderate sex differences, as do our findings presented here. In accordance with our NHP results, QoLrelated scale scores on life satisfaction and happiness reached the German reference levels only with slight differences (below as well as above).
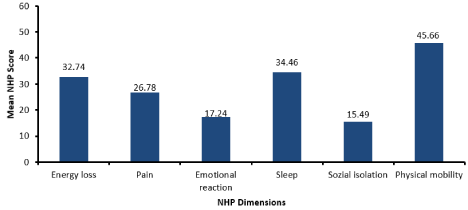
Figure 1: Descriptive results of the NHP scales.
NHP Scales
Group-Living Nursing Home Residents
German Reference Values from Older
People Living IndependentlyDiff.
t
M
SD
n
M
SD
n
Energy Loss
m
28.12
28.62
64
33.33
40.82
45
-5.21
-1.359
f
34.27
29.64
284
34.98
36.86
81
-0.71
-0.485
Pain
m
22.92
26.26
60
21.94
29.33
45
0.98
0.229
f
27.78
27.8
252
21.14
27.92
81
6.64
3.688***
Emotional Reaction
m
17.19
15.95
64
11.11
21.32
45
6.08
2.945**
f
16.94
17.18
284
14.04
22.04
81
2.9
2.556*
Sleep
m
34.69
25.76
64
31.56
32.89
45
3.13
0.671
f
33.8
26.28
284
27.9
31.25
81
5.9
3.749***
Social Isolation
m
16.88
20.84
64
8.89
17.35
45
7.99
2.863**
f
14.79
20.2
284
12.59
18.01
81
2,20
1.739
Physical Mobility
m
44.17
22.25
60
22.22
27.94
45
21.95
6.814***
f
46.02
21.85
281
27.01
27.84
81
19.01
13.648***
M: Mean; SD: Standard Deviation; Diff: Difference between Mean Values; m: male; f: female.
***: P =0.001 (2-sided); **: P =0.01 (2-sided); *: P =0.05 (2-sided).
Table 2a: Comparison between group-living nursing home residents and German reference values from individuals over 75 years of age.
Qol Related Scales
Group-Living Nursing Home Residents
German Reference Values Better Life IndexB
Diff
t
M
SD
n
M
SD
n
Life satisfaction
7.07
0.704
389
7
-
12.414
0.07
0.26
World Value SurveyW
Feeling of happiness
m
2.78
0.701
64
3.05
0.716
65
0.27
-3.068**
f
2.73
0.722
284
2.79
0.643
75
0.06
-1.344
M: Mean; SD: Standard Deviation; Diff: Difference between Mean Values; m: male; f: female; ** p =0.01 (2-sided).
BSex differentiation and SD not available [33].
WAge group over 75 years selected and calculated based on the World Value Survey SPSS data set [34].
Table 2b: Comparison between group-living nursing home residents and German reference values from better life.
Reliability of the NHP for group-living nursing home residents
Table 3 shows the mean and standard deviation as well as Cronbach’s alpha and the split-half reliability of the NHP for the 404 home residents. All scales can be regarded as sufficient, as we obtained high values for Cronbach’s alpha and the split-half reliability.
Scale
M
SD
a
rtt
Energy loss
32.74
29.8
0.84
0.83
Pain
26.78
27.37
0.9
0.96
Emotional reaction
17.24
17.44
0.76
0.8
Sleep
34.46
26.17
0.84
0.85
Social isolation
15.49
20.64
0.77
0.83
Physical mobility
45.66
22.57
0.82
0.93
M: Mean; SD: Standard Deviation; a: Internal Consistency (Cronbach’s alpha); rtt: Split-Half Reliability (Spearman-Brown).
Table 3: Psychometric data for the items of the NHP for group-living elderly individuals.
Table 4 shows the inter-correlations for all NHP scales. In general, positive correlations appear between all NHP scales. The highest inter-correlations were found between physical mobility and pain and between emotional reaction and energy loss.
EL
P
ER
S
SI
PM
SH
LS
FH
Energy Loss (EL)
-0.193**
-0.269**
-0.236**
Pain (P)
0.329**
-0.272**
-0.191**
-0.132*
Emotional Reaction (ER)
0.399**
0.272**
-0.187**
-0.462**
-0.374**
Sleep (S)
0.277**
0.370**
0.364**
-0.146**
-0.214**
-0.110*
Social Isolation (SI)
0.263**
0.171**
0.445**
0.218**
-0.208**
-0.386**
-0.329**
Physical Mobility (PM)
0.438**
0.457**
0.182**
0.265**
0.179**
-0.256**
-0.178**
-0.113*
** P =0.01 (2-sided); * P =0.05 (2-sided).
SH: Status of Health; LS: Life Satisfaction; FH: Feeling of Happiness.
Table 4: Inter-correlations of NHP scales and further relations.
Correlation analysis showed a statistically significant moderate inverse relation between the NHP score and the currently perceived status of health (r -0.283, p ≤0.01). The highest correlation was found between the perceived status of health and the NHP scale pain (r -0.272, p ≤0.01), followed by the NHP scale physical mobility (r -0.256, p ≤0.01). The NHP score also correlated positively with the residents’ feelings of happiness (r 0.295, p ≤0.01) and life satisfaction (r 0.393, p ≤0.01). No statistically significant relation could be found between the NHP score and age. Residents with cognitive impairments (positive AMT4 test) generally estimated their quality of life to be higher than others (NHP score 135.48, p ≤0.001, eta 0.243/eta2 0.059).
Discussion and Limitations
The present study describes the subjective quality of life in groupliving nursing home residents. Home-like living, social interactions and domestic activities are important characteristics of group-living nursing homes. According to our main objective, the present study con-ducted face-to-face interviews employing the Nottingham Health Profile (NHP). The mean NHP scale score over all dimensions suggests an adequate perception of quality of life. Among the six different NHP scales, social life and emotional well-being scored best regarding subjective quality of life, whereas physical mobility showed the lowest perception of quality. We regard deteriorated physical mobility as one of the main reasons for living in a nursing home. Several other studies have yielded similar findings investigating mobility in older people [33,34]. The comparison with reference values from independently living older people in Germany revealed further results. Although a few significant differences between the two subsamples of persons older than 75 years could be found, our findings indicate that with the exception of the NHP scale physical mobility, the perceived quality of life of group-living nursing home residents and independently living elderly individuals over 75 years of age are nearly identical. Accordingly, our present findings from 25 nursing homes confirm those of the preliminary pilot study conducted in seven nursing homes in 2013. Further QoL-related scales, specifically the residents’ perceived life satisfaction and feeling of happiness, support the NHP results.
Previous study findings, although not directly related to group-living settings, indicate that active conduct of life and social interactions in older age have a decisive impact on QoL [35-37].
Subjective quality of life is an essential criterion for the evaluation of nursing homes and geriatric care. Furthermore, patient-outcome research on the (assumed) value of innovative care models and ‘new living and care arrangements’, such as group-living principles substituting former institutional care, is an important resource for health policy-makers and public health researchers. In addition to objective quality indicators, appropriate measurements of residents’ perspectives are necessary to comprehensively evaluate the impact of innovative home care settings. Hence, our second objective was to replicate the previous study protocol, aiming to validate the scales implemented at the time. A recent meta-analysis by Camerer et al. [38] revealed that many studies in the social sciences could not be replicated (replication crisis). The verification of study designs is a very important part of good scientific practice. However, the psychometric quality of the NHP instrument turned out to be sufficient (satisfactory internal consistency and split-half reliability). The questionnaire was appropriate for nursing home res-idents with age-specific mental and functional impairments. The NHP sub-scales showed various intercorrelations. Consistent with our pilot study design [25] and with the findings from the nation-wide sample of independently living people [29], we found a relatively high correlation between physical mobility and pain. As shown in the same study, we could also replicate the significant correlations between energy loss, emotional reaction and social isolation, suggesting that energy loss not only results from physiological ageing but also can be under-stood as linked to social and emotional well-being [39-43].
Despite the common assumption that nursing home residents are unable to understand and answer complex questions properly [5], the participants in our study responded well to the interviews. The majority of NHP items were easy to understand, as the two response choices (yes or no) were easy to handle for the interviewees. Naturally, many nursing home residents found it hard to manage paper & pencil tests due to impaired vision or hearing, difficulties concentrating and other dementia-related ailments. Reading the questionnaire out loud in a face-to-face interview proved to be most practical. Additionally, we could avoid the need for supportive assistance from nursing home staff (often required with self-administered paper & pencil questionnaires) to prevent possible biases on the effect of social desirability responses.
On average, the interview was completed within 40 minutes. However, some interviews took approximately two hours because some residents found pleasure in telling the researchers about their lives.
The negatively formulated NHP statements worried some of the participants. In these cases, the interviewees received close attention and further explanations of the statements.
Naturally, the cross-sectional design of the present study (at a specific point in time) exhibits some limitations. The preselection of the samples according to resident eligibility may limit the subsequent interpretation as well as the relevance of the data. Additionally, the fact that the personal characteristics of residents in group-living settings might differ from those of regular nursing home residents limits the comparability of the data.
The Nottingham Health Profile is one of the most frequently used generic instruments in the area of health-related quality of life measurement. It appears to be particularly appropriate for the questioning of older people, as the items are short and answering is relatively easy. Nevertheless, the NHP concept focuses generally on negative criteria in measuring subjective quality of life, albeit from a holistic point of view, and positive aspects could enrich the outcome of the questionnaire. Moreover, some items in the dimension social isolation might trigger relatively strong emotional reactions (with regard to the findings in our pilot study in 2013 and as reported by Warnke et al. [18]). Accordingly, the NHP scale, particularly the subscale social isolation, is not recommended for evaluating subjective quality of life in residents with depressive symptoms, as they are often related to dementia.
Although the NHP covers areas of particular importance to older people, such as loss of energy, pain, sleeping disorders, social isolation, mobility and emotional health, it might be useful to enhance the instrument with subscales focusing on specific QoL aspects that are related to nursing care settings [37].
Conclusion and Implications
To our knowledge, this investigation provides unique evidence about the subjective quality of life in group-living nursing homes. The study presented here (1) addresses elderly people with agespecific reduced physical and mental abilities; (2) includes cognitively impaired participants; and (3) encompasses 25 nursing homes in the first major study in the research field of subjective quality of life in German group-living nursing homes. Moreover, the previous pilot study protocol and the preliminary results could be successfully replicated.
The presented findings intend to start a discussion: in many countries, traditional hospital-like nursing homes are evolving. New initiatives aim at improving the notion of nursing home care to better meet people’s needs, improve the quality of care and eventually enhance quality of life. To varying degrees, many of these activities focus on aspects of home-like nursing environments, such as traditional nursing homes with enhanced activities, group-living nursing homes, combination care homes (residential and nursing homes under one roof), small group nursing homes, and nursing homes in rural farm settings.
Therefore, we recommended a nationwide scientific evaluation programme on subjectively perceived outcome quality to provide representative reference values and to compare various care settings.
Due to the lack of research on residents’ perspectives on QoL, further studies should follow to establish age-specific and care settingspecific reference data for nursing home residents. In particular, more research is required to answer the question of which care setting best meets the essential needs of older people. We welcome participatory efforts.
Declarations
Acknowledgements
We thank the participating residents and nursing staff of the 25 nursing homes. We are also indebted to the students (School of Health Sciences & Management, year 2015) for helping with the field work. Kaspar Pfister and Michael Barkow provided administrative support, and we thank them both.
Authors’ contributions
AS designed the study, carried out the study, performed statistical analysis and wrote the manuscript.
Ethical approval and consent to participate
The study was conducted in full accordance with the ethical standards of the institutional and national research committee and to the World Medical Association Declaration of Helsinki, the guidelines and recommendations for ensuring Good Epidemiological Practice (GEP), and the international code for market and social research (ICC/ESOMAR). Informed consent was obtained from all individual participants included in the study.
Funding
The study was supported by a grant for travel and analysis expenditures from the Nursing Home Management Organization (a non-profit company).
References
- WJ Eerden van der and GMM Jones. “Dutch large-scale dementia-care environments: a village within the community”. Care Services Management. 2011; 5: 137-146.
- J Lindesay, K Briggs, M Laves, A Macdonald and J Herzberg. “The Domus philosophy: a comparative evaluation of a new approach to residential care for the demented elderly”. Int J Geriatr Psychiatry. 1991; 6: 727-736.
- J Ritchie, A Colvez, J Ankri, B Ledesert, H Gardent and A Fontaine. “The evaluation of long-term care for the dementing elderly: a comparative study of hospital and collective non-medical care in France”. Int J Geriatr Psychiatry. 1992; 7: 549-557.
- Y Funaki, F Kaneko and H Okamura. “Study on factors associated with changes in quality of life of demented elderly persons in group homes”. Scand J Occup Ther. 2005; 12: 4-9.
- M Hassler and K Wolf-Ostermann. “Wissenschaftliche Evaluation zur Beurteilung der Pflege-Transparenzvereinbarungen für den ambulanten (PTVA) und stationären (PTVS) Bereich”. 2010.
- J Möller and G Zieres. “Zur Transparenz der Qualität von Pflegeeinrichtungen. On quality and transparency of care facilities”. Gesundh ökon Qual manag. 2010; 15: 39-44.
- S Sünderkamp, C Weiß and H Rothgang. “Analyse der ambulanten und stationären Pflegenoten hinsichtlich der Nützlichkeit für den Verbraucher”. Pflege. 2014; 27: 325-336.
- A Przylog, MA Stroka, S Engel and R Linder. “Bieten Pflegeheime mit besseren Pflegenoten auch eine bessere Qualität? Empirische Analyse auf Ba-sis von GKV-Routinedaten”. Zeitschrift für Gerontologie and Geriatrie. 2016; 49: 308-316.
- K Wingenfeld and D Engels. “Entwicklung und Erprobung von Instrumenten zur Beurteilung der Ergebnisqualität in der stationären Altenhilfe. Abschlussbericht”. Bundesministeriums für Gesundheit und des Bundesministeriums für Familie, Senioren, Frauen und Jugend, Bielefeld, Köln, IPW. 2011.
- S Becker, A Kruse, J Schröder and lU Seid. “Das Heidelberger Instrument zur Erfassung von Lebensqualität bei Demenz (H.I.L.DE)”. Z Gerontol Geriat. 2005; 38: 108-121.
- H Brandenburg and H Günther. Gerontologische Pflege. Bern: Hogrefe. 2015.
- B de Boer, JPH Hamers, SMG Zwakhalen, FES Tan and H Verbeek. “Quality of care and quality of life of people with dementia living at green care farms: a cross-sectional study”. BMC geriatrics. 2017; 17: 155.
- C Grabowski, AJ O’Malley, CC Afendulis, DJ Caudry, A Elliot and S Zimmerman. “Culture change and nursing home quality of care”. Gerontologist. 2014; 54: S35-545.
- JS Kok, MMA Nielen and EJA Scherder. “Quality of life in small-scaled homelike nursing homes: an 8-month controlled trial”. Health and quality of life outcomes. 2018; 16: 38.
- R Palm, D Trutschel, CGG Sorg, MN Dichter, B Haastert and B Holle. “Quality of Life in People with Severe Dementia and Its Association with the Environment in Nursing Homes: An Observational Study”. Gerontologist. 2019; 59: 665-674.
- M Vaarama, R Pieper and A Sixsmith. “The general framework and methods for the care keys research”. In Care-related quality of life in old age: concepts, models, and empirical findings, New York, Springer, Vaarama M; Pieper R; Sixsmith A. 2008: 3-18.
- M Holzhausen. Lebensqualität älterer Menschen. Konstruktion eines neuen individualisier-ten Messverfahrens, Bern: Hans Huber. 2009.
- A Warnke, G Meyer, U Bott and I Muelhausen. “Validation of a quality of life questionnaire measuring the subjective fear of falling in nursing home residents”. Z Geront Geriat. 2004; 37: 459-466.
- S Auer, U Kienberger, P Pascher, M Geck, B Hofmann, C Viereck, et al. “Small scale group living versus traditional nursing home for persons with dementia”. Pflegewissenschaft. 2017; 19: 156-165.
- TP Ettema R-M Droes, J de Lange, GJ Mellenbergh and MW Ribbe. “A review of quality of life instruments used in dementia”. Qual Life Res. 2005; 14: 675-686.
- HJ Gertz and M Berwig. “Ist die Lebensqualität von Demenzpatienten messbar”? Nervenarzt. 2008; 79: 1023-1035.
- R Logsdon, LE Gibbons, SM McCurry and L Teri. “Assessing quality of life in older adults with cognitive impairment”. Psychosom Med. 2002; 64: 510-519.
- A Sixsmith, M Hammond and G Gibson. “Quality of life and dementia”. In Care-related quality of life in old age: concepts, models, and empirical findings, New York, Springer. 2008: 217-233.
- T Schaal, T Schönfelder, J Klewer and J Kugler. “Quality of care in German nursing homes. A longitudinal study regarding quality assenssments from 2009 to 2013”. Heilberufe Science. 2015; 6: 3-9.
- A Simon, M Berwig and S Heinrich. “Quality of life in Nursing Homes following the Group-Living Principle. A pilot study measuring the quality of life from the subjective perspective of dependent-living elderly”. Z Gerontol Geriat. 203; 46: 556-562.
- R Rupprecht. “Lebensqualität”, In Gerontologie. Medizinische, psychologische und sozialwissenschaftliche Grundbegriffe, Stuttgart, Kohlhammer. 2006: 242-247.
- SM Hunt and J McEwen. “The development of a subjective health indicator”. Social Health Illn. 1980; 2: 231-246.
- A Noro. “Long-term institutional among Finnish elderly population: trend and potential dis-charge”. Stakes, Helsinki. 1998.
- T Gunzelmann, A Hinz and E Brähler. “Subjective health in older people”. GMS Psycho-Social-Medicine. 2006; 3: 1-10.
- T Kohlmann, M Bullinger and I Kirchberger-Blumstein. “The German version of the Nothingham Health Profile (NHP). Methodological issues of translation and psychometric validation”. Soz Präventivmed. 1997; 42: 175-185.
- R Inglehart, C Haerpfer, A Moreno, C Welzel, K Kizilova, J Diez-Medrano, et al. “World Values Survey: Round Six - Country-Pooled Datafile Version”. 2014.
- DG Swain and PG Nightingale. “Evaluation of a shortened version of the Abbreviated Mental Test in a series of elderly patients”. Clin Rehabil. 1997; 11: 243-248.
- MA Wirtz, M Morfeld, E Brähler and H Glaesmer. “Association of Physical Morbidity and Health-Related Quality of Life in a Representative Sample of Older German People”. European Journal of Health Psychology. 2018; 25: 140-151.
- ET Yümin, TT Simsek, M Sertel, A Öztürk and M Yümin. “The effect of functional mobility and balance on health-related quality of life (HRQoL) among elderly people living at home and those living in nursing home”. Arch Gerontol Geriatr. 2011; 52: 180-184.
- S Graefe, S van Dyk and S Lessenich. “Being old is occurring later. Agerelated norms and self-concepts in the second half of life”. Z Gerontol Geriat. 2011; 44: 299-305.
- G Livingston, A Sommerlad, V Orgeta, SG Costafreda, J Huntley, D Ames, et al. “Dementia prevention, intervention and care”. Lancet. 2017; 390: 2673- 2734.
- D Xu, H Mou, J Gao, W X, J Ling and K Wang. “Quality of life of nursing home residents in mainland China: The role of children and family support”. Arch Gerontol Geriatr. 2019; 83: 303-308.
- C Camerer, A Dreber, F Holzmeister, T-H Ho, J Huber, M Johannesson, et al. “Evaluating the replicability of social science experiments in Nature and Science between 2010 and 2015”. Nature Human Behaviour. 2018.
- J Möller, H Panhorst and G Zieres. “Qualitätsberichterstattung für ambulante Pflegedienste. Anspruch und Realität. Public reporting on professional nursing home care demand and reality”. Gesundh ökon Qual manag. 2010; 15: 185-191.
- M Vaarama, R Pieper and A Sixsmith. Care-related quality of life in old age: concepts, models, and empirical findings. New York: Springer. 2008.
- WD Oswald, et al. Gerontologie. Medizinische, psychologische und sozialwissenschaftliche Grundbegriffe, Stuttgart: Kohlhammer. 2006.
- LD Sharples, CJ Todd, N Caine and S Tait. “Measurement properties of the Nottingham Health Profile and Short Form 36 health status measures in a population sample of elderly people living at home: Results from ELPHS”. Br J Health Psychol. 2000; 5: 217-233.
- OECD. “Better Life Index”. 2017.