
Case Report
Austin Gynecol Case Rep. 2017; 2(1): 1011.
Heterotopic Pregnancy following Ovulation Induction: A Case Report
Kouach J¹, Moukit M¹*, Ait El Fadel F¹, El Fazazi H¹, Guelzim K¹, El Hassani ME¹, Babahabib A¹, Moussaoui RD¹ and Dehayni M²
¹Department of Obstetrics and Gynecology, Military Training Hospital Mohammed V, Morocco
²Pole of Gynecology and Visceral Surgery, Military Training Hospital Mohammed V, Morocco
*Corresponding author: Mounir Moukit, Department of Obstetrics and Gynecology, Military Training Hospital Mohammed V, Hay Riyad, 10100, Rabat, Morocco
Received: January 23, 2017; Accepted: February 17, 2017; Published: February 20, 2017
Abstract
Clomiphene Citrate which increases the rate of twinning could be associated with a heterotopic pregnancy rate of 1/900. We present the case of a 25-yearold Moroccan woman who developed a simultaneous extra- and intrauterine pregnancy after ovulation induction with Clomiphene Citrate. An urgent minilaparotomy was performed confirming a preruptured ectopic pregnancy in the right fallopian tube. Preservation of the intrauterine pregnancy was obtained until 41 weeks with vaginal delivery of a healthy boy.
Keywords: Heterotopic pregnancy; Clomiphene citrate; Transvaginal ultrasound; Surgery
Introduction
The concept of ultrasound confirmation of an Intrauterine Pregnancy (IUP) to exclude the possibility of an Extrauterine Pregnancy (EP) is well known because Heterotopic Pregnancy (HP) is extremely rare. However, with increasing use of Assisted Reproductive Techniques (ART) and ovulation induction, more cases have been reported in the literature. We report a case of HP following ovulation induction with Clomiphene Citrate, which was successfully diagnosed and managed in our department.
Case Report
A 25-year-old Moroccan woman was a case of primary infertility for two years and ultrasound findings of polycystic ovary syndrome. Hysterosalpingography and her husband spermogram were normal. She received ovulation induction with Clomiphene Citrate (100 mg/ day) starting on day 2 of the cycle and continued with recombinant FSH on day 7. Transvaginal ultrasound on day 12 showed 2 good size follicles in the right ovary; the left ovary contained one good size follicle in addition to other small follicles less than 10 mm. Endometrium was 12 mm thick. She was given HCG on day 12 and was advised for natural intercourse on day 13. Her next presentation was at 6 weeks of amenorrhea with a chief symptom of lower abdominal pain. On admission, patient was conscious, coherent with pulse 108/min, blood pressure 110/80 mmHg; mild tenderness was found on deep palpation of the right lower abdominal quadrant. Pelvic examination revealed an enlarged uterus corresponding to 6 weeks of pregnancy, with no bleeding. Transvaginal ultrasound showed an intrauterine gestational sac with fetal pole and visible fetal heartbeat. A small amount of free fluid was seen in the pouch of Douglas. Given her history of fertility treatment and her physical examination findings, adnexal areas were evaluated with particular detail. A second gestational sac with fetal pole and cardiac activity, adjacent to the right ovary, was visualized, suggestive of heterotopic pregnancy (Figure 1). Her haemoglobin was 10.1 g/dL with a normal white blood cell count and platelet count. Patient was consented for an operative laparotomy few hours later. Per operatively, a total of 80 ml of hemoperitoneum was aspirated. The uterus was enlarged according to the gestational age; left annex and right ovary were normal with a preruptured ectopic pregnancy in the ampullary portion of the right fallopian tube. Enucleation of the pregnancy was performed with right salpingectomy. Nicardipine (Loxen®) was used for tocolysis. The material was sent for histological examination confirming chorionic villi. The intrauterine pregnancy was followed up till 41 weeks and she was induced (one dose of Misoprostol) with vaginal delivery of a healthy baby boy.
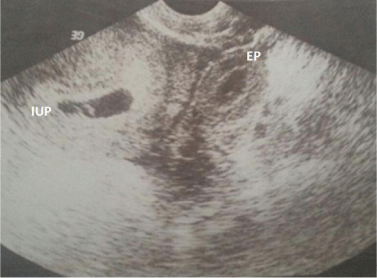
Figure 1: Transvaginal ultrasound revealing simultaneous Intrauterine (IUP)
and Ectopic Pregnancy (EP).
Discussion
Heterotopic pregnancy is a rare form of twin pregnancy defined as the simultaneous presence of intra- and extrauterine pregnancy. The estimated incidence is 1 per 30000 pregnancies [1]. It mostly happens with known risk factors notably assisted reproductive techniques, ovulation induction, and previous history of pelvic inflammatory diseases or ectopic pregnancy. The risk factor we have found in our patient was ovulation induction by Clomiphene Citrate. This drug is used to induce ovulation in selected populations with oligo or anovulation as a strategy to increase follicles number and development, and could be associated with HP in up to 1/900 of the cases [2]. Maheswari and Panicker reported a case of triplet heterotopic pregnancy after ovulation induction with Clomiphene Citrate [3]. It is interesting that in our case, as well as other cases reported in the literature [4,5], the drug had been given from days 2 to 6 of the cycle, a time when the resultant FSH surge is more likely to enhance maturation of multiple follicles. In some previous reports, the drug had been given from days 5 to 9 of the cycle, when it is more likely to result in maturation of the dominant follicle only [6,7]. Preoperative diagnosis of HP remains a major challenge. Around 50% of cases are asymptomatic and diagnosed very late with significant morbidity and sometimes mortality. When symptomatic, the clinical features are abdominal pain, vaginal bleeding, hypovolemic shock, and adnexal mass. High-resolution transvaginal ultrasonography is the most important aid in the diagnosis. Simultaneous visualization of intra and extrauterine gestational sacs confirms the diagnosis of heterotopic pregnancy. In a review of the literature (112 cases of HP), 46 were diagnosed by ultrasound while 66 were diagnosed during surgery [8]. According to reviews, in 77 to 85% of cases in whom diagnosis was via ultrasonography, diagnosis was made between 5 and 8 weeks of gestation [7], as was in our patient. Plasmatic beta human chorionic gonadotropin (beta-hCG) level is often difficult to interpret because the IUP causes the beta-hCG level to rise appropriately. Consequently, it was not performed in this case. The standard treatment for HP is surgery by laparoscopy or laparotomy depending upon the condition of the patient. Laparoscopic surgery is an option if the patient is hemodynamically stable; moreover, emergency laparotomy is the only choice if the hemodynamic status is compromised. In our case, lack of laparoscopic equipment in the operating room for emergency, minilaparotomy was performed for rapid treatment. The main aim of the surgery should be the preservation of the intrauterine pregnancy with minimal manipulation of the uterus. Intrauterine fetal outcome after surgical management of the EP depends on many factors: gestational age of diagnosis, operative time, quality of anesthesia, and surgery (minimal uterine manipulation). The use of prophylactic tocolysis still debatable by several authors. In the present case, intravenous Nicardipine (Loxen®) was prescribed during and after surgery for prevention of uterine contractions. Medical treatment can be used safely and effectively to manage patients who are clinically stable and where a HP is recognized relatively early in gestation. The successful management of six cases of HP using Potassium Chloride (KCl) injection into the tubal EP has been reported [9]. However, since the risks of continued growth and rupture still exist with such nonsurgical management, repeated ultrasounds examination and close monitoring of clinical symptoms are essential. A literature review of HP treated with KCL injection noted that 55% of cases failed this therapy and required surgical intervention [10]. Expectant management could be considered as a form of treatment in a symptom-free patient where the ectopic tubal embryo has a limited craniocaudal length with no heart activity [11].
Conclusion
This case suggests that heterotopic pregnancy must always be considered in patients presenting with pelvic pain even in a confirmed intrauterine pregnancy, particularly if ovulation induction or assisted reproductive techniques have done. It also demonstrates that surgical approach with prophylactic tocolysis should be preferred to preserve the intrauterine ongoing pregnancy.
Acknowledgment
We are thankful to the patient who permitted us to present his history in this report.
References
- Avitabile NC, Kaban NL, Siadecki SD, Lewiss RE, Saul T. Two Cases of Heterotopic Pregnancy: Review of the literature and sonographic diagnosis in the emergency department. J Ultrasound Med. 2015; 34: 527-530.
- Shastri KR, Anand NI, Ganatra BM. A rare case of heterotopic pregnancy in natural conception with ectopic pregnancy. Indian Journal of Obstetrics and Gynecology Research. 2015; 2: 174-175.
- Maheswari S, Panicker S. Triplet heterotopic pregnancy following ovulation induction with Clomiphene citrate: a case report and review of literature. Int J Reprod Contracept Obstet Gynecol. 2013; 2: 743-745.
- McClure N, McClelland R, Winter H, White R. Heterotopic pregnancy. J Obstet Gynecol. 1991; 11: 101-103.
- Selo-Ojeme DO, GoodFellow CF. Simultaneous intrauterine and ovarian pregnancy following treatment with Clomiphene citrate. Arch Gynecol Obst. 2002; 266: 232-234.
- Naki MM, Tekcan C, Uysal A, Guzin K, Yucel N. Heterotopic pregnancy following ovulation induction by Clomiphene citrate and timed intercourse: a case report. Arch Gynecol Obstet. 2006; 274: 181-183.
- Mehrabian F, Robati BK. Heterotopic abdominal pregnancy following ovulation induction with Clomiphene citrate. Iran J Reprod Med. 2010; 8: 51- 54.
- Tandon R, Goel P, Saha PK, Devi L. Spontaneous heterotopic pregnancy with tubal rupture: a case report and review of the literature. J Med Case Reports. 2009; 3: 8153.
- Scheiber MD, Cedars MI. Successful non-surgical management of a heterotopic an abdominal pregnancy following embryo transfer with cryopreserved-thawed embryos. Hum Reprod. 1999; 14: 1375-1377.
- Goldstein JS, Ratts VS, Philpott T, Dahan MH. Risk of surgery after use of potassium chloride for treatment of tubal heterotopic pregnancy. Obstet Gynecol. 2006; 107: 506-508.
- Baxi A, Kaushal M, Karmalkar HK, Sahu P, Kadhi P, Dava B. Successful expectant management of tubal heterotopic pregnancy. J Hum Reprod. 2010; 3: 108-110.