
Case Report
Austin Head Neck Oncol. 2017; 1(1): 1003.
Ovarian Metastasis from Schmincke-Regaud’s Tumor
Ennaji M¹*, Willemse E¹, Veys I², Larsimont D², Andry G¹ and Digonnet A¹
¹Department of Head and Neck Surgery, Jules Bordet Institute (ULB), Brussels, Belgium
²Department of Mammo-Pelvic Surgery, Jules Bordet Institute (ULB), Brussels, Belgium
³Department of Pathology, Jules Bordet Institute (ULB), Brussels, Belgium
*Corresponding author: Meriem Ennaji, Department of Head and Neck Surgery, Jules Bordet Institute (ULB), Brussels, Belgium
Received: July 27, 2017; Accepted: August 30, 2017; Published: September 06, 2017
Abstract
Nasopharyngeal Carcinoma (NPC) has an established potential for distant metastasis however it is generally localized at diagnosis. Metastatic sites are usually multifocal and involve the bones, lungs and distant lymph nodes [1]. To the best of our knowledge, this is the first report of a nasopharyngeal carcinoma that metastasized to the ovary.
In the present study, the case of a 57-year-old female patient with a history of nasal obstruction and epistaxis is presented. Following a series of examinations and a biopsy of the cavum, the patient was diagnosed with an undifferentiated carcinoma of the nasopharynx (cT2bcN1M0). Subsequently, the patient received a concurrent Chemoradiation Therapy (CRT). She was in complete remission after the treatment.
Fourthy one months after primary diagnosis, during her regular follow up examination, a voluminous hypermetabolic lesion was discovered in the left ovary through Positron Emission Tomography-Computed Tomography (PETCT). The histological results confirmed the evidence of an ovarian metastasis from Undifferentiated Carcinoma of the Nasopharyngeal Type (UCNT).
The aim of this report is to present the unusual case of ovarian metastasis from nasopharyngeal carcinoma, an extremely rare event but worth considering in patients presenting an ovarian lesion at imaging and a history of primary or recurrent nasopharyngeal carcinoma.
Keywords: Nasopharyngeal carcinoma (NPC); Undifferentiated carcinoma of the nasopharyngeal type (UCNT); Epstein- barr virus (EBV); Positron emission tomography-computed tomography (PET-CT)
Abbreviations
NPC: Nasopharyngeal Carcinoma; CRT: Chemoradiation Therapy; PET-CT: Positron Emission Tomography-Computed Tomography; UCNT: Undifferentiated Carcinoma of the Nasopharyngeal Type; WHO: World Health Organization; EBV: Epstein - Barr virus; EBER: In-Situ- Hybridization for EBV-DNA; MOC: Multidisciplinary Oncologic Consultation; TPN: Total Parenteral Nutrition
Introduction
Nasopharyngeal Carcinoma (NPC) is a tumor arising from the epithelial cells that cover the surface and line the nasopharynx. It was first described as a distinct entity by Regaud and Schmincke in 1921 [2-3].
The World Health Organization (WHO) classifies nasopharyngeal carcinoma in three types: keratinising squamous cell carcinoma (Type I), non-keratinising differentiated carcinoma (Type II) and non-keratinising undifferentiated carcinoma (Type III) [4].
The undifferentiated tumor (type III), also called Schmincke’s tumor or lymphoepithelioma is the most common type of NPC. It is also more prevalent in North African and Chinese populations [5]. Consumption of salted fish is one of the factors leading to NPC, which might be related to carcinogenic nitrosamine detected in fish.
Epstein-Barr Virus (EBV) infection also plays a role in the etiology of type II and III NPC [6].
The incidence of such tumors peaks between 20 and 30 years of age, and after 60 years of age.
NPC is typically unresectable at diagnosis, but is more responsive to chemotherapy and radiotherapy than other head and neck cancers [7]. Cervical lymph node metastases are present at diagnosis in 75- 90% of cases and are bilateral in more than 50% cases [8].
Distant metastases are present at diagnosis in 5-11% of patients, and the most common sites are bone, lung and liver tissue [9].
Metastases to the ovary commonly arise from the gastrointestinal tract, breast, lungs and controlateral ovaries.
Other rare primaries include endometrium, melanoma, pancreas and carcinoid [10].
To our knowledge, the current study describes the only case of a patient with an ovarian metastasis from nasopharyngeal carcinoma.
Case Presentation
In October 2012, a 57-year-old 0 from Algiers was admitted to the department of Head and Neck Surgery at Jules Bordet Institute in Brussels. She was suffering from nasal obstruction, sinusitis and intermittent epistaxis since a few weeks. The patient did not smoke or consume alcohol. She didn’t notice any weight loss over the past months. Physical investigation was totally normal. Endoscopic inspection showed a large nasopharyngeal mass localized in the posterolateral wall of the cavum. The histological examination of the biopsy resulted in the diagnosis of undifferentiated NPC (UCNT, WHO III) (Figure 1). Serological tests for EBV were positive.

Figure 1: Undifferentiated nasopharyngeal carcinoma. Neoplasic cell nests
with syncytial growth pattern and interspersed non-neoplastic lymhoid
component. Tumor cells have round to oval nuclei, prominent eosinophilic
nucleoli.
Additionally, a PET-CT and a CT scan of the neck, chest, abdomen and pelvis were performed. No arguments for metastatic disease were retained. The CT scan and MRI did show an expansive growing process in the superior and posterolateral left wall of the cavum. The tumor mass extended to the choanae and the left parapharyngeal space with homolateral pathological lymph nodes (Figure 2).
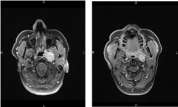
Figure 2: MRI show an expansive growing process in the superior and
posterolateral left wall of the cavum. The tumor extended to the choanae and
the left parapharyngeal space. There is a retrophayngeal node (N1).
Based on these findings, the patient was diagnosed with UCNT cT2bcN1M0. According to the American Joint committee on Cancer Staging [11], the patient was diagnosed with stage III nasopharyngeal carcinoma. During the Multidisciplinary Oncologic Consultation (MOC), cisplatinum based CRT was proposed as the best treatment option for this patient.
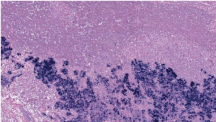
Figure 3: In-situ-hybridization for EBV-DNA (EBER). EBV chromogenic insitu-
hybridization reveals the presence of EBV DNA in the tumor cells (blue
staining) of the liver metastasis.
Seventy Gy were delivered over the course of 33 weeks on the tumor and on bilateral lymph nodes. Concomitant triweekly cisplatinum was administrated in a curative setting. The patient received only two cycles of cisplatinum iv 100 mg/m² during radiotherapy, instead of the initially planned three cycles due to severe side-effects (grade II asthenia , grade III nausea and vomiting, grade IV dysphagia, grade IV erythema in the radiation field and grade II renal insufficiency). Due to severe mucositis, the persisting dysphagia required a Total Parenteral Nutrition (TPN) instead of a feeding tube.
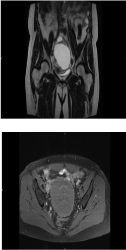
Figure 4: MRI show a voluminous, irregular cystic mass of 10cm invading
the left ovary.
Full clinical and radiological remission was achieved after radiotherapy completion.
Fourteen months after the last adjuvant treatment was administrated, during a routine follow up examination, CT and Positron Emission Tomography-Computed Tomography (PETCT) scans revealed a hypermetabolic lesion in the left liver. The lesion was focal, unique and micronodular (13mm) in segment III. A partial left hepatectomy of segments II and IV was performed by coelioscopy. The pathology report confirmed a single metastasis from undifferentiated carcinoma of nasopharyngeal type. Immunolabelling was thus performed.
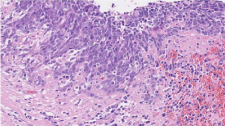
Figure 5: Ovarian metastasis from a Schmincke’s tumor.
In-situ-hybridization for EBV-DNA (EBER) and EBV were both positive and the keratin AE1/AE3 and keratin 5/6 showed a immunohistochemistry pattern compatible with the diagnosis (Figure 3).

Figure 6: EBER positive in the ovarian metastasis from a Schmincke’s tumor.
Five months later the patient discovered a swollen left preauricular mass. The cervical MRI confirmed multiple augmented lymph nodes on the left side and one suspicious node of 2cm in diameter localized in the left pre-auricular zone. A left neck dissection at the levels I, II and Va and an excision of the left pre-auricular lesion was performed. Histological evaluation revealed the presence of two lymph nodes metastases (one pre-auricular node and one cervical node at level Va) massively invaded by an undifferentiated carcinoma of nasopharyngeal type. EBER and EBV were strongly positive. A multidisciplinary evaluation concluded that there was no reason to administer any systemic adjuvant treatment after the surgery. The patient was monitored every six months by clinical examination and imaging (PET-CT and CT scan).
The patient’s condition remained stable over a period of almost two years.
In June 2016, forty one months after primary diagnosis, a voluminous hypermetabolic lesion in the left ovary was detected by positron emission tomography-computed tomography (PET-CT). Additionally a CT scan and a MRI were carried out. Both showed a voluminous, irregular cystic mass of 10cm invading the left ovary and a para-aortic lymph node near L2 (Figure 4).
The radiological characteristics were highly suspect for a primary ovarian tumor. The previous sites of NPC metastasis were unchanged from prior examinations.
The patient was therefore referred to the Department of Mammo Pelvic Surgery and underwent a debulking with a total hysterectomy, annexectomy, appendicectomy and a para-aortic and aorta-cava dissection.
Histopathological analysis confirmed the evidence of an ovarian metastasis from a Schmincke’s tumor (Figure 5). The nodes dissection was exempt of malignancy. Immunolabelling with keratin 19 was highly present but EBV and EBER detection were positive (Figure 6). The tumor type was consistent with the original nasopharyngeal biopsy taken in October 2012.
Unfortunately, five months later a new unique lesion appeared in the left iliac wing.
The PET-CT scan did not display any further metastatic diseases. An external radiotherapy with 30Gy was delivered on the left iliac wing over three cycles during 6 days.
Complete clinical remission was achieved. Faced with this atypical clinical presentation, the MOC concluded that there was no place for a systemic adjuvant treatment with the argument that the recurrences were localized and had always been treated with a curative intente. The last follow-up in March 2017 didn’t showed any signs or symptom of local recurrence. At the time of this report, the patient was disease free, doing well and went back to Algiers until her next follow-up in September 2017. Neoplasic cell nests with syncytial growth pattern and interspersed non-neoplastic lymhoid component. Tumor cells have round to oval nuclei, prominent eosinophilic nuleoli. EBV chromogenic in-situ-hybridization reveals the presence of EBV DNA in the tumor cells (blue staining) of the liver metastasis
Discussion
Lymphoepithelial tumors are the most common carcinoma of the nasopharynx. From the 3 types of nasopharynx carcinoma belonging to the World Health Organization classification, only the non-differentiated type is considered to be a Schmincke’s tumor. Incidence is higher in South Asia and North Africa. The tumor is three times more common in males than in females [12]. The incidence of the tumor according to age, peaks between 20 and 30 years of age, and after 60 years of age.
The detection of the Epstein-Barr virus is not necessary to establish a diagnosis of NPC, however, it may be useful for cases where the diagnosis is unclear. In our case EBV infection might only partially explain the development of this rare type of cancer. Therefore it is assumed that underlying genetic mechanisms play an important role in the pathophysiology of NPC [13]. First line therapy consists of primary radiation of the tumor’s primary region and its lymphatic drainage channels. Concomitant chemotherapy can be applied for advanced NPC (AJCC stage III-IV) to decrease distant metastasis and improve locoregional control, as well as improve overall survival [14].
In case of cervical tumor spreading, a salvage neck dissection reduces the risk of local recurrence if residual disease remains after treatment. Unlike other head and neck tumors, prognosis remains poor; more than one-third of cases will present local and/or metastatic recurrence [1]. Although significant advances have been made in the integration of radiotherapy and chemotherapy for the treatment of patients with NPC, distant metastasis remains a major cause of mortality and treatment failure for these patients. There is a 5-year survival rate of 60% in stage I and II (according to UICC classification) [15]. Furthermore, there is a 5-year survival rate of 25% in stage III and IV [16].
Metastasis to the ovary from a NPC has never been reported. To the best of our knowledge, this is the first report of a nasopharyngeal carcinoma that metastasized to the ovary. The potential for misdiagnosis and confusion is high, as primary ovarian cancer is far more common than NPC and the radiographic appearance of these lesions can be similar. The clinical context of concurrent or remote NPC may guide the pathologist to consider this rare diagnosis.
The anatomic extent of the metastasis is closely associated with the prognosis of the patient with metastatic NPC [17]. As is the case in this report, a single metastatic lesion in an isolated location is typically reported to be associated with prolonged survival compared to multiple metastatic lesions in a single or multiple locations [18,19]. The reported overall survival of NPC patients after the detection of distant metastases ranges from 22 to 120 months [20]. In conclusion, we presented the only case of a 57-year old woman with an ovarian metastasis from UCNT (stage III), an extremely rare event but worth considering in patients displaying an ovarian lesion at imaging and presenting a history of primary or recurrent nasopharyngeal carcinoma.
More than 4 year after primary diagnosis and following four recurrences, the patient is currently disease free. The four recurrences were detected using imaging since the patient was asymptomatic. To date there are no real recommendations regarding head and neck follow-up, we suggest the use of routine imaging at long term. We would like to emphasize the fact that in such uncommon evolution, follow-up should be tailored to the specific situation. Although unsupported by guidelines, routine PETCT could be performed in these type of cases.
References
- Chan DK, Lee AW, Poon YF, Foo W, Law SC, Cheung FK, et al. Retrospective analysis of 5037 patients with nasopharyngeal carcinoma treated during 1976-1985: overall survival and patterns of failure. Radiat Oncol Biol Phys. 1992; 23: 261-270.
- Regaud C. Lympho-épitheliome de l'hypopharynx traité par la roentgenthérapie. Bull Soc Franc Otorhinolaryngol.1921; 34: 209-214.
- Schmincke A. Über lymphoepitheliale Geschwülste. Beitr Pathol Anat.1921; 68: 161-170.
- Paul W, Bruce H, Thomas Robbins K, Regan Thomas J, Mark A, Richardson et al. Cummings Otolaryngology. 5th 2010.
- Dickens P, Srivastava G, Loke SL, Chan CW, Liu YT. Epstein-Barr virus DNA in nasopharyngeal carcinomas from Chinese patients in Hong Kong. J Clin Pathol. 1992; 45: 396-397.
- Lo KW, Chung GT, To KF. Deciphering the molecular genetic basis of NPC through molecular, cytogenetic, and epigenetic approaches. Semin Cancer Biol. 2012; 22: 79-86.
- Guigay J, Temam S, Bourhis J, Pignon JP, Armand JP. Nasopharyngeal carcinoma and therapeutic management: the place of chemotherapy. Ann Oncol. 2006; 17: 304-307.
- Altun M, Fandi A, Dupuis O, Cvitkovic E, Krajina Z, Eschwege F, et al. Undifferentiated nasopharyngeal cancer (UCNT): current diagnostic and therapeutic aspects. Int J Radiat Oncol Biol Phys. 1995; 32: 859-877.
- Vokes EE, Liebowitz DN, Weichselbaum RR. Nasopharyngeal carcinoma.Lancet. 1997; 350: 1087-1091.
- Khunamornpong S, Suprasert P, Chiangmai WN. Metastatic tumors to the ovaries: a study of 170 cases in northern Thailand. Int. J. Gynecol. Cancer. 2006; 16: 132-138.
- Edge S, Byrd D, Compton C. AJCC Cancer Staging Manual.7th Springer; New York, NY: 2010.
- Chua ML, Wee JT, Hui EP, Chan AT. Nasopharyngeal carcinoma. Lancet. 2015.
- Chang ET, Adami HO. The enigmatic epidemiology of nasopharyngeal carcinoma. Cancer epidemiology, biomarkers & prevention: a publication of the American Association for Cancer Research, cosponsored by the American Society of Preventive Oncology. 2006; 15: 1765-1777.
- Lu H, Peng L, Yuan X, Hao Y, Lu Z, Chen J, et al. Concurrent chemoradiotherapy in locally advanced nasopharyngeal carcinoma: a treatment paradigm also applicable to patients in Southeast Asia. Cancer Treat Rev. 2009; 35: 345-353.
- Strutz J, Mann W.2. Auflage: Thieme Verlag; Praxis der HNO-Heilkunde, Kopf- und Halschirurgie; pp. 2010; 478-480.
- Brennan B. Nasopharyngeal carcinoma. Orphanet J Rare Dis. 2006; 1: 2
- Shen LJ, Wang SY, Xie GF, Zeng Q, Chen C, Dong AN, et al. Subdivision of M category for nasopharyngeal carcinoma with synchronous metastasis: time to expand the M categorization system. Chin J Cancer. 2015; 34: 40.
- Lin S, Tham IW, Pan J, Han L, Chen Q, Lu JJ, et al. Combined high-dose radiation therapy and systemic chemotherapy improves survival in patients with newly diagnosed metastatic nasopharyngeal cancer. Am J Clin Oncol. 2012; 35: 474-479.
- Pan CC, Lu J, Yu JR, Chen P, Li W, Huang ZL, et al. Challenges in the modification of the M1 stage of the TNM staging system for nasopharyngeal carcinoma: A study of 1027 cases and review of the literature. Exp Ther Med. 2012; 4: 334-338.
- Li JX, Huang SM, Wen BX, Lu TX. Prognostic factors on overall survival of newly diagnosed metastatic nasopharyngeal carcinoma. Asian Pac J Cancer Prev. 2014; 15: 3169-3173.