
Case Report
Austin Head Neck Oncol. 2021; 4(1): 1010.
A Diagnostic Challenge: Gingival Lesions in a Postirradiated Nasopharyngeal Carcinoma Patient
Sng JHT*, Lum JL, Loy CHR and Yeo JF
Discipline of Oral and Maxillofacial Surgery, National University Centre for Oral Health, Singapore
*Corresponding author: Timothy SJH, Discipline of Oral and Maxillofacial surgery, National University Centre for Oral Health, National University of Singapore, 9 Lower Kent Ridge Road, 119085, Singapore
Received: January 04, 2021; Accepted: February 24, 2021; Published: March 03, 2021
Abstract
This paper shares a diagnostically challenging case of radiation-induced sarcoma that first presented as gingival ulcerations and pain in a postradiated nasopharyngeal carcinoma patient. Insufficient information from the clinical presentation and non-specific findings from initial imaging results hindered early diagnosis. Nonetheless, correlation with medical history, prompt histopathological analysis and PET-CT imaging eventually led to a definitive diagnosis. This case report aims to increase the awareness of this uncommonly known but deadly long-term complication of head and neck radiotherapy. Clinicians ought to include radiation-induced sarcoma in their list of differential diagnosis when a patient, with a history of head and neck radiotherapy, presents with persistent gingival or oral mucosa lesions, alveolar bony exposure or other suspicious dental-related symptoms.
Keywords: Radiation-induced sarcoma; Post-irradiation; Nasopharyngeal carcinoma; Gingiva; Oral cavity
Abbreviations
NPC: Nasopharyngeal Carcinoma; ANUP: Acute Necrotizing Ulcerative Periodontitis; ORN: Osteoradionecrosis of the Jaw; OSCC: Oral Squamous Cell Carcinoma; RIS: Radiation-induced Sarcoma; MRI: Magnetic Resonance Imaging; PET-CT: Positron Emission Tomography-computed tomography; FDG: Fluorodeoxyglucose
Case Presentation
A 65 year old Chinese man presented to an oral & maxillofacial surgeon for management of persistent & severe pain over his upper and lower left posterior gingiva. The pain started 2 weeks ago. Previously diagnosed with Nasopharyngeal Carcinoma (NPC), he underwent radiotherapy 30 years ago. He has been in clinical remission since then. An ex-smoker for 44 years, the patient quit smoking 2 years ago. No abnormalities were detected on extraoral examination. Intraoral examination revealed poor oral hygiene, heavily restored dentition and rampant caries. Multiple sinus tracts, likely associated with necrotic teeth, were also seen. Regions of white punched-out ulcers were present along the gingival margins of his upper and lower left posterior teeth (Figure 1). The ulcers were extremely tender to palpation. Periapical radiographs of the involved region revealed severe bone loss and periapical radiolucencies associated with root resorption (Figure 2).
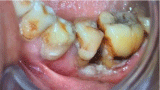
Figure 1: White punched-out ulcers along the gingival margins of lower left
posterior teeth.
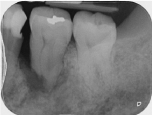
Figure 2: Periapical radiograph depicting marked bone loss, periapical
radiolucency and root resorption on #36 (lower left first molar).
Differential Diagnosis
• Acute Ulcerative Necrotizing Periodontitis (ANUP)
• Osteoradionecrosis of the jaw (ORN)
• Recurrence of Nasopharyngeal Carcinoma (NPC) with distant metastasis
• Primary Oral Squamous Cell Carcinoma (OSCC)
• Radiation-Induced Sarcoma (RIS)
From the clinical presentations alone, ANUP was initially suspected. Nonetheless, the gingiva lesions & pain did not subside despite mechanical periodontal debridement and a course of metronidazole. Human immunodeficiency virus and Herpes Simplex virus screening were negative too. Having undergone radiotherapy for NPC, osteoradionecrosis of the jaw (ORN) was our next reasonable working diagnosis. However, non-specific findings from periapical radiographs, panoramic radiographs and MRI preclude differentiation amongst lesions associated with ORN, infection and neoplastic processes. This diagnostic challenge from the abovementioned imaging modalities is consistent with that of a case report [1].
In fact, the MRI findings were suggestive of ORN and more obvious pathologic progression was found on the asymptomatic contralateral (right) side of the patient’s mandible (Figure 3). While it reinforced what was seen on the panoramic radiograph (Figure 4), it further complicates the clinical situation: which is persistent pain and ulceration of the upper and lower left gingiva. Other differential diagnosis considered were the recurrence of NPC with distant metastasis and primary oral squamous cell carcinoma.
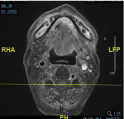
Figure 3: MRI: Fairly extensive patchy marrow changes with enhancement in the mandible. Focal cortical defect at the anterior cortex of the right hemimandible body.
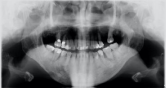
Figure 4: Incidental finding from the panoramic radiograph showing more
prominent patchy mixed radiolucency on the right body of the mandible.
Angular bone loss and periapical radiolucency of tooth #36 & #46 (lower left
and right first molars) are evident.
Definitive Diagnosis
Incisional biopsies of the affected left upper and lower gingiva were performed. Histological reports revealed high-grade malignancy with sarcomatoid appearance suggestive of pleomorphic spindle cell sarcoma (Figure 5). This was suggestive of a post-radiation sarcoma of the oral cavity (cT2N0M0). In addition, PET-CT scans (Figure 6) revealed intensely FDG-avid lesions of both the left maxilla and hemimandible with associated cortical erosions that are compatible with suspected high-grade neoplasms on recent histological examination.
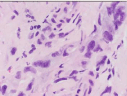
Figure 5: Spindle cells with abundant cytoplasm showing marked nuclear atypia.
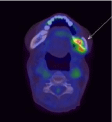
Figure 6: Intensely FDG-avid lesions involving left maxilla and the hemimandible
with associated cortical erosions. There is moderate FDG uptake in
the right hemi-mandible, which is indeterminate.
Management
Patient was referred to his primary otorhinolaryngology team for further management of oral cavity radiation induced sarcoma (cT2N0M0). A left mandibulectomy and resection of left maxilla together with reconstruction via a left free fibular flap and dental prosthesis respectively were proposed. However, the patient passed away shortly after due to complications related to his recovery from a recent stroke.
Discussion
Radiation-Induced Sarcoma (RIS) of the oral cavity is a less commonly known complication of radiation therapy. With its prolonged latency and usually delayed diagnosis, RIS has a worse prognosis than primary sarcoma. Due to the aggressive pattern of local growth and recurrence, RIS of the skull region has the least favorable prognosis [2].
It is not uncommon for head and neck cancer patients to present at a dental clinic, complaining of a myriad of dental problems. However, a lack of correlation between patient’s medical history and clinical findings may obviate the appropriate management in cases of radiation-induced sarcoma, distant metastasis or even new primary oral squamous cell carcinoma. With an increasingly ageing population and improving survival outcomes for NPC-afflicted patients treated by radiotherapy, the risk of acquiring lifetime mutations and incidence of radiation-induced sarcoma may be increasing [3,4].
As such, one should always have a high index of suspicion when attending to such patients, especially when faced with unusual clinical presentations such as atypical dental pain, gingival lesions, spontaneous alveolar bone exposure, rapidly progressive periodontitis, etc. Without any biopsy or further imaging performed, treating such patients with ANUP or ORN targeted modalities alone or adopting a “wait-and-see” approach would certainly cause delays in appropriate intervention against RIS. Suspicious clinical findings together with relevant medical history should prompt for histopathological analysis via biopsy.
A general criterion of radiation-induced sarcoma [5] are:
• Treatment with therapeutic irradiation at least 3 years prior to development of sarcoma
• A sarcoma arising within the field of previous therapeutic irradiation
• Differing histology between the sarcoma and the primary tumor that required radiotherapy
Early detection and timely intervention may help mitigate the complications related to radiation-induced sarcoma of the head and neck. As such regular comprehensive dental reviews and timely referral to the appropriate specialists offer such patients the best chance for cure and survival. To our knowledge, this is the first case report of oral cavity radiation-induced sarcoma with initial presentation of gingival pain and ulcerative lesions.
References
- Wood J, Ver Halen J, Samant S, Florendo N. Radiation-induced sarcoma masquerading as osteoradionecrosis: case report and literature review. J Laryngol Otol. 2015; 129: 279-282.
- Maghami EG, St-John M, Bhuta S, Abemayor E. Postirradiation sarcoma: a case report and current review. Am J Otolaryngol. 2005; 26: 71-74.
- Robinson E, Neugut AI, Wylie P. Clinical aspects of postirradiation sarcomas. Journal of the National Cancer Institute. 1988; 80: 233-240.
- Wei Z, Xie Y, Xu J, Luo Y, Chen F, Yang Y, et al. Radiation-induced sarcoma of head and neck: 50 years of experience at a single institution in an endemic area of nasopharyngeal carcinoma in China. Med Oncol. 2012; 29: 670-676.
- Arlen M, Higinbotham NL, Huvos AG, Marcove RC, Miller T, Shah IC. Radiation-induced sarcoma of bone. Cancer. 1971; 28: 1087-1099.