
Case Report
Ann Hematol Oncol. 2014;1(3): 1015.
Four Malignancies - One Patient
Kenyeres A1*, Kovács G1, Barna S2, Bedekovics J3, Méhes G3, Illés A1 and Miltényi Z1
1Department of Hematology, University of Debrecen, Hungary
2Scanomed LTD, University of Debrecen, Hungary
3Department of Pathology, University of Debrecen, Hungary
*Corresponding author: Kenyeres A, Department of Hematology, University of Debrecen, 4032 Debrecen, Nagyerdeikrt. 98, Hungary
Received: November 21, 2014; Accepted: December 05, 2014; Published: December 08, 2014
Abstract
Introduction: Cancer survivors have an increased risk of developing further malignancies. Their development is affected by many facilitating factors, and they can occur metachronously or synchronously with the other neoplasms.
Case Report: Our patient was an elderly man, who developed four primary malignancies. He had intraepithelial neoplasia of the prostate at the age of 70. Five years later, he presented with Kaposi sarcoma of skin. At 84 years of age he developed synchronous stadium IV peripheral T-cell lymphoma and adenocarcinoma of the colon.
Discussion: There are different studies and theories about correlation between occurrence of lymphoid malignancies and other tumors, and it is likely that malignancies of lymphoid cells are high risk factors for developing second neoplasms.
Keywords: Multiple primary neoplasms; T-cell lymphoma; Gastrointestinal adenocarcinoma; PET/CT
Abbreviations
CHOP: Cyclophosphamide Hydroxidaunorubicin Oncovin Prednisone; ECOG: Eastern Cooperative Oncology Group; HE: Hematoxylin-Eosin; MPMN: Multiple Primary Malignant Neoplasm; NHL: Non-Hodgkin's Lymphoma; PET/CT: Positron Emission Tomography - Computed Tomography
Introduction
The number of cancer survivors is increasing with progress of medical treatment, but these patients have higher risk for development of a second or higher order primary cancer [1]. Multiple Primary Malignant Neoplasms (MPMNs) are defined as distinct tumors, presenting a definite pattern of malignant disease, and the possibility that one of the tumors is a metastasis of another is excluded [1]. According to literature roughly 2-12% of all patients with two metachronous or synchronous tumors go on to develop a third or fourth neoplasm [2]. Another study estimated the incidence of secondary malignant tumors to be 3-5%, while occurrence of triple tumors is 0,5%, and that of quadruple tumors 0,3% [1]. Proposing factors include prior cancer treatment, environmental agents, immune abnormalities and genetic predisposition [1,3,4]. Majority of MPMNs are carcinomas, and they occur in the same, or in paired organs, and in embriologically related organs [1,5]. MPMNs can be divided according to interval between presentation of the tumors. Cancers are considered to be synchronous when they are diagnosed simultaneously or within six months of each other, while metachronous cancers are defined when the second is diagnosed more than six months after the first [6].
Case Presentation
The patient is a male born in 1928. He was treated twice because of deep venous thrombosis in 1997 and 1998. Searching for the background of thrombi, further investigation revealed stage II intraepithelial neoplasia of the prostate. The patient underwent total androgenic blockade monotherapy for four years. In 2003, a 4x3 mm brownish black nodule was completely excised from the skin of the right thigh, which histologically proved classic type Kaposi sarcoma. He was HIV negative; he received no additional therapy following surgery. Chronic renal failure developed in 2006 and Hemodialysis was started in 2010. In August of 2012 he presented with strong bleeding from a lesion of the left forearm 4-5 cm in diameter which first appeared 1,5 years earlier. Biopsy was performed and histology revealed cutaneous manifestation of T-cell Non-Hodgkin's Lymphoma (NHL) (Figure 1). At the same time he complained of itching and nocturnal sweats. Staging including flowcytometry from peripheral blood and bone marrow, cristal biopsy and PET/CT, revealed stadium IV/A disease, International Prognostic Index (IPI) 4, high risk, ECOG 1.
A: Massive, diffuse infiltration of medium sized atypical lymphoid cells within the dermis with intraepithelial infiltrative component (HE, original magnification: x200). B: Mitotic ratio is increased, arrows indicate mitotic figures (HE, original magnification: x400).Tumor cells show CD3 (C) and CD4 (D) positivity.
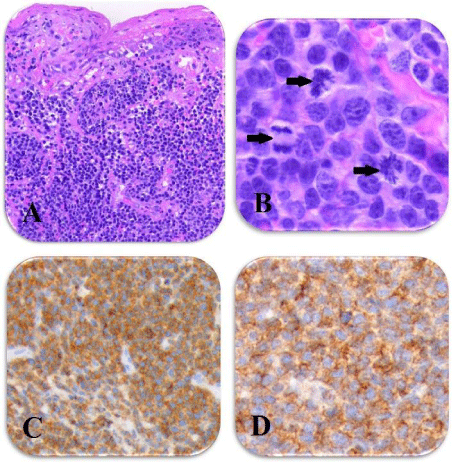
Figure 1: Peripheral T-cell NHL.
A: Massive, diffuse infiltration of medium sized atypical lymphoid cells
within the dermis with intraepithelial infiltrative component (HE, original
magnification: x200). B: Mitotic ratio is increased, arrows indicate mitotic
figures (HE, original magnification: x400).Tumor cells show CD3 (C) and CD4
(D) positivity.
There was a 3 cm long, intensely enhancing thickening of the bowel wall in the sigmoid region, which raised the possibility of a primary process (Figure 2). He received the first cycle of reduced CHOP treatment. We chose epirubicin instead of doxorubicin to minimize the risk of cardiotoxicity. Before the second cycle of chemotherapy, colonoscopy was performed, which showed polyps in the cecum and rectum, diverticulosis of colon, and a 5 cm long, rugged surfaced, hemorrhagic lesion, which did not narrow the lumen and involved one third of the colon's circumference. Biopsy was performed and histology showed infiltrating adenocarcinoma. The patient had no p53 gene mutation. Consultant oncologist did not recommend any active treatment of colonic tumor, since it did not cause ileus and the patient had no complaint. After three cycle of CHOP chemotherapy, PET-CT showed partial remission of the lymphoma (Figure 3), so he received a fourth cycle of chemotherapy. Less than two weeks later the patient presented with weakness, swollen lymph nodes and new skin lesions on chest and arms. After consulting the nephrologist, we continued the systemic chemotherapy with reduced, modified IGEV (ifosfamide, gemcitabine, vinorelbine) protocol adjusted to hemodialysis. On the eighth day of observation sensomotoric aphasia presented. Magnetic Resonance Imaging (MRI) was performed, which showed severe cerebral atrophy, but no brain lymphoma. His condition declined, hypostatic pneumonia developed, and he died a few days later.
Primer staging PET/CT revealed cutaneous manifestation of lymphoma in upper and lower extremities and involvement of axillary and inguinal lymph nodes. There was a 3 cm long, intensely enhancing thickening of the bowel wall in sigmoid region, which raised the possibility of a primary process.
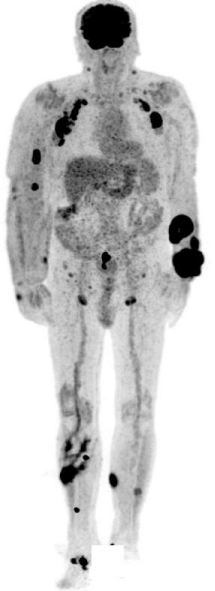
Figure 2: Primer staging PET/CT.
Primer staging PET/CT revealed cutaneous manifestation of lymphoma in
upper and lower extremities and involvement of axillary and inguinal lymph
nodes. There was a 3 cm long, intensely enhancing thickening of the bowel
wall in sigmoid region, which raised the possibility of a primary process.
The pathological enhancement disappeared in the lower limbs and in the right arm, but pronounced decrease in the size and activity of the lesions is seen in other regions. A new lesion is appeared on the left side of the chest, and the progression of the rectal carcinoma toward the bladder is suspected.

Figure 3: Interim PET/CT.
The pathological enhancement disappeared in the lower limbs and in the right
arm, but pronounced decrease in the size and activity of the lesions is seen in
other regions. A new lesion is appeared on the left side of the chest, and the
progression of the rectal carcinoma toward the bladder is suspected.
Discussion
The risk of developing a new malignancy is increasing with the number of previous tumors. Prior cancer treatment, immune abnormalities, environmental and genetic factors can stand in the background [1,3,4]. But in many cases we cannot uncover the cause of MPMNs. It suggests that tumors generally predispose to the appearance of another primary neoplasm. It is particularly true with malignancies of the lymphoid cells. However our patient's second tumor, Kaposi sarcoma, presented nine years before the diagnosis of lymphoma, it could have been the first manifestation of insufficient T-cell function, which is an important predisposing factor for developing Kaposi sarcoma.
There are only few cases in the literature, when NHL and gastrointestinal carcinoma present synchronously. Probability of synchronous colonic carcinoma and lymphoma in the same patient was estimated to be 0,0002% by Barron and Localio [7]. In 2011 Papajík et al. examined 209 patients with newly diagnosed NHL. Initial staging F-18fluorodeoxyglucose PET/CT revealed findings suspicious for second malignancy in six cases. With further investigations before lymphoma therapy two patients were diagnosed with colorectal carcinoma, one with esophageal adenocarcinoma, one with invasive ductal breast carcinoma, one with medullary thyroid carcinoma, and one with squamous cell lung carcinoma [8]. However, in 1957 Moertel and Hagedorn concluded that the presence of a malignant lymphoma did not seem to predispose tothe development of any other type of primary malignancy [9], Cornes in 1960 reported that coexisting adenocarcinomas either occur synchronously or follow, but never precede, lymphoma [5]. Barron and Localio in 1976 suggested that lymphomatous process may be the initial event, which compromises patient's immune defense against development of colon cancer [7]. These latter reports based their conclusions on the fact that in most cases, progression of lymphoma seemed to be more extended than the carcinoma, as it happened also in our case. In contrast Yap and Soh reported a case in 2012, when follicular NHL was diagnosed during further examinations of a patient with invasive rectal adenocarcinoma. They considered lymphoma to be the second primary malignancy, and prioritized the treatment of the symptomatic rectal cancer [10].
Although peripheral T-cell lymphomas frequently show extra nodal manifestation, it's very important to perform further investigations if first staging PET/CT reveals positive lesion suspicious for second malignancy.
References
- Demirci U, Coskun U, Gocun PU, Gurlek B, Saka B, Ozturk B, et al. Four different malignancies in one patient: a case report. Cases J. 2010; 3: 53.
- Angurana SL, Kapoor R, Kumar P, Khosla D, Kumar N, Sharma SC, et al. Quadruple malignancy in a single patient: a case report and comprehensive review of literature. J Cancer Res Ther. 2010; 6: 230-232.
- Quilon JM, Day S, Lasker JC. Synchronous tumors: Hodgkin disease presenting in mesenteric lymph nodes from a right hemicolectomy for colon carcinoma. South Med J. 2004; 97: 1133-1135.
- Noh SK, Yoon JY, Ryoo UN, Choi CH, Sung CO, Kim TJ, et al. A case report of quadruple cancer in a single patient including the breast, rectum, ovary, and endometrium. J Gynecol Oncol. 2008; 19: 265-269.
- Cornes JS. Multiple Primary Cancers: Primary Malignant Lymphomas and Carcinomas of the Intestinal Tract in the Same Patient. J Clin Pathol. 1960; 13: 483-489.
- Lee TK, Barringer M, Myers RT, Sterchi JM. Multiple primary carcinomas of the colon and associated extracolonic primary malignant tumors. Ann Surg. 1982; 195: 501-507.
- Lee DY, Hong SW, Chang YG, Lee WY, Lee B, Kang YK. Synchronous T-cell lymphoma in patient with colon cancer: a case report. J Korean Surg Soc. 2012; 83: 60-64.
- Papaji¬k T1, Myslivecek M, Sedova Z, Buriankova E, Prochazka V, Raida L, et al. Synchronous second primary neoplasms detected by initial staging F-18 FDG PET/CT examination in patients with non-Hodgkin lymphoma. Clin Nucl Med. 2011; 36: 509-512.
- Moertel CG, Hagedorn AB. Leukemia or lymphoma and coexistent primary malignant lesions: a review of the literature and a study of 120 cases. Blood. 1957; 12: 788-803.
- Yap J, Soh A. Adenocarcinoma of the proximal rectum and synchronous non-Hodgkin's lymphoma. J Gastrointest Oncol. 2013; 4: 101-102.