
Case Report
Ann Hematol Oncol. 2015;2(1): 1016.
A Case of Splenic Marginal Zone Lymphoma with Mismatched Morphology and Phenotype, Karyotype and Clinical Course
Sorigue M1*, Juncà J2, Gassiot S1, Navarro JT2, Mate JL3 and Millà F2
1Department of Hematology, Hospital Gerans Trias i Pujol, Spain
2IJC, Hospital Germans Trias i Pujol, Spain
3Department of Pathology, Hospital Germans Trias i Pujol, Spain
*Corresponding author: Sorigue M, Department of Hematology. Hospital Germans Trias i Pujol, Ctra. Canyet s/n 08916 Badalona, Spain
Received: November 06, 2014; Accepted: January 05, 2015; Published: January 07, 2015
Abstract
Background: Splenic marginal zone lymphoma is a rare chronic lymphoproliferative neoplasm with a very indolent clinical course and a noncharacteristic phenotype and karyotype. Peripheral blood morphology can be the first clue to the diagnosis.
Methods: Here, we report a case of a patient with splenic marginal zone lymphoma, alive 20 years after initial diagnosis, with very atypical and immature lymphocytes in peripheral blood smear since then.
Results: Peripheral blood phenotype and karyotype and pathological analysis of splenectomy sample, as well as the clinical evolution were compatible with splenic marginal zone lymphoma. Conversely, peripheral blood morphology was, from the start, atypical and suggestive of a high-grade lymphoproliferative disorder.
Conclusion: Integrating all clinical and laboratory data is essential to make an appropriate diagnosis and guide the therapeutic options offered to patients.
Keywords: Splenic marginal zone lymphoma; Atypical morphology; Indolent lymphoma
Abbreviations
MZL: Marginal Zone Lymphoma; MALT: Mucosa-Associated Lymphoid Tissue; SMZL: Splenic Marginal Zone Lymphoma
Case Presentation
A 65 year-old woman was sent for hematologic evaluation in 1994 because of the incidental finding of peripheral blood lymphocytosis. She was asymptomatic. On physical examination splenomegaly, without hepatomegaly or any enlarged lymph nodes, was palpable. The peripheral blood smear revealed large-sized cells, with a wide nucleus occupying most of the cell space, with immature and reticulated chromatin, and one or more conspicuous nucleoli. In some cells the nucleus adopted an irregular form. The cytoplasm was basophilic without any granularity (Figure 1). However, phenotypical exam of the lymphocytes was compatible with SMZL and peripheral blood cytogenetic analysis revealed a complex karyotype, including a trisomy of chromosome 3 and an imbalanced traslocation involving chromosome 7q36. Methacrylate-embedded bone marrow showed a nodular and paratrabecular pattern of infiltration by small, mature and monomorphic lymphocytes. The diagnosis of SMZL was made.
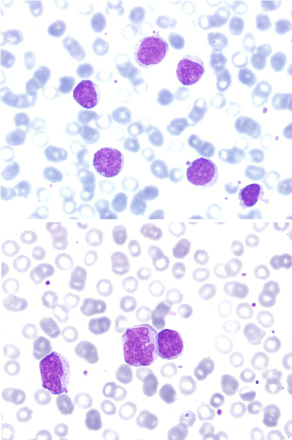
Figure 1: Peripheral blood smear at diagnosis in 1994. Atypical and large
lymphocytes showing convoluted nuclei and fine chromatin. (May-Grünwald
Giemsa x40 and x100, top and bottom).
Tests at diagnosis are shown on Table 1.
September 1994
May 25th, 1999
August 8th, 2001
March 5th, 2002
September 9th, 2005
October 29th, 2007
December 10th, 2013
Splenomegaly
4cm below costal border
15cm below costal border
6cm below costal border
Not applicable
Hepatomegaly
Not palpable
6cm below costal border
Not palpable
Lymph nodes
None palpable
CT scan
Splenomegaly.
Splenomegaly, hepatomegaly and enlarged nodes in splenic hilum (1-2cm)
Splenomegaly
No findings
Hemoglobin (g/L)
120
87
95
136
146
142
117
Lymphocyte count (x10e9/L)
28
13.5
24.3
38.1
139
43
16.6
LDH
Normal
β2M (mg/L)
2.5
4.4
4.3
3.1
2.6
7.8
IgM (mg/dL)
498
1590
450
2120
HCV, HIV
Negative
Phenotype
CD19+, CD20+, CD22+, DR+, CD5-, CD10-, CD23-
Cytogenetic findings
48, XX, +1, del(1)(p32), +3, del(3)(p21), der(7)t(1;7)(p32;q36)[20] (peripheral blood)
48, XX, +1, del(1)(p32), +3, del(3)(p21), der(7)t(1;7)(p32;q36)[2] (spleen)
Bone Marrow biopsy
Evidence of chronic lymphoproliferative disease
Evidence of chronic� lymphoproliferative disease
Not repeated
Treatment indication
B symptoms
B symptoms
B symptoms
Progressive lymphocytosis
B symptoms
Treatment
None
CNOPx6
Splenectomy
RCVPx6
RCVPx6
RCVPx6
HCV: Hepatitis C Virus; HIV: Human Immunodeficiency Virus; CNOP: Cyclophosphamide, Mitoxanthrone, Vincristine, Prednisone; RCVP: Rituximab, Cyclophosphamide, Vincristine, Prednisone; Normal laboratory values: Hemoglobine 120-160g/L; lymphocyte count: 1.5-3.5x10e9/L; β2M (mg/L) <2.4mg/L; IgM<230mg/dL.
Table 1: Physical findings, analytical findings and treatment during the course of the disease.
The clinical course has also been characteristic of indolent lymphoma. For 20 years she has been followed up in the outpatient setting. She has been admitted on 6 occasions, 3 of them because of B symptoms, which led to the administration of chemotherapy, and the other 3 because of pneumonia. She also received a therapeutic splenectomy in 2001. The pathological analysis revealed infiltration
by a chronic lymphoproliferative disease positive for CD20 and CD79a, compatible with SMZL. Overall, the patient has been treated for her lymphoproliferative disorder 5 times, 4 of them with polychemotherapy (3 of those including rituximab), and has achieved as many clinical complete responses, i.e., normalization of the blood counts and disappearance of splenomegaly and any enlarged lymph nodes. Tests performed before the start of each course of chemotherapy are also shown in Table 1.
In 2013 she was admitted because of delirium and worsening of her functional and cognitive impairment secondary to pneumonia, which resolved favorably with antibiotics. Lymphocytosis (16.6x10e9/L) and mild anemia (hemoglobin 117g/L) were noted, and there were no enlarged lymph nodes. Peripheral blood lymphocytes still showed the same morphology (Figure 2) and phenotype observed at diagnosis. The patient is currently alive and asymptomatic.
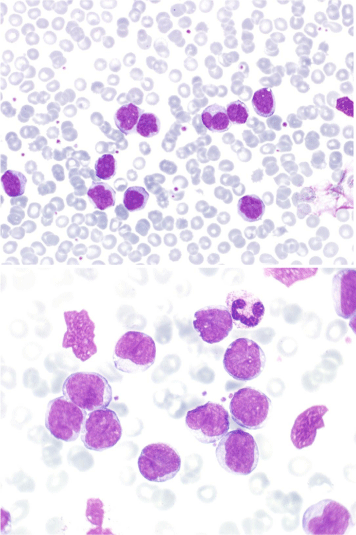
Figure 2: Peripheral blood smear in 2005 where the same lymphocytes could
be seen (May-Grünwald Giemsa, x40 and x100, top and bottom).
Discussion
MZL is a low grade chronic lymphoproliferative disorder arising from post-germinal center marginal zone B cells. It encompasses three entities, depending on the affected organ; MALT lymphoma, SMZL and nodal marginal zone lymphoma.
SMZL is often diagnosed incidentally, either because of cytopenias, splenomegaly or detection of clonal peripheral blood lymphocytosis with a compatible phenotype, which can be seen in more than half of cases (SMZL with villous lymphocytes) [1]. Enlarged lymph nodes are rarely seen. Although diagnosis is traditionally made by histological examination of the spleen, bone marrow histology along with a suggestive phenotype are considered enough to establish it [2- 4]. However, some groups have made the diagnosis with peripheral blood lymphocyte morphology and phenotype [5-7].
On peripheral blood smear, SMZL typically presents with
middle-sized, mature and villous lymphocytes. Unlike the villous cells of hairy-cell leukemia, lymphocytes in SMZL are smaller, their villi are shorter and polar, and their nuclei contain a more condensed chromatin [8].
The phenotypic exam of all subtypes of MZL is characterized by the expression of B-cell antigens and surface immunoglobulin, along with lack of expression of CD5, CD10, CD43 and CD103 although CD5 is occasionally positive [4,9]. It is currently unknown whether CD5 positivity confers a different clinical course [10].
Cytogenetic abnormalities are frequently found in SMZL. The most common are gain of 3q and deletion of 7q [9,11]. The characteristic translocation seen in MALT lymphoma, t (11;18) (q21;q21), is always negative in SMZL [9].
Diagnosis has classically been established by microscopic examination of splenic tissue, where small, mature lymphocytes are seen surrounding or invading the germinal centers in the white pulp and infiltrating the red pulp. Differential diagnosis includes other low-grade lymphoproliferative disorders in the rare cases in which they affect the spleen primarily. These include: follicular lymphoma, which typically presents with preserved or only slightly altered germinal centers in which centrocytes (i.e., small, mature and cleaved lymphocytes) often predominate; mantle cell lymphoma, which presents with mature lymphocytes with a particularly irregular nucleus and almost always cyclin D1 translocation; and small lymphocytic lymphoma, which presents with small lymphocytes with hyper condensed chromatin, a high nucleus-to-cytoplasm ratio and variably effaced germinal centers.
At the time of diagnosis SMZL may not require treatment, particularly if the patient is asymptomatic. When therapy is required, splenectomy or alkylating agents have historically been the agents of choice although rituximab seems to have improved Reponses and time to next treatment [12].
Like other indolent lymphomas, MZL is generally considered not curable, except when treated with allogeneic stem cell transplantation. Nevertheless, the time between relapses is often measured in years and patients' quality of life is usually preserved [5,13,14], even though a small percentage of cases do follow a more aggressive course [1,15,16] or undergo transformation to diffuse large B cell lymphoma [6,7,17].
In the case reported here there was a clear mismatch between, on the one hand, a very indolent clinical course and a phenotype and karyotype suggestive of marginal zone lymphoma and, on the other hand, a very atypical morphology. Both morphological and cytometric exams were repeated several times during the course of the disease.
The patient is still alive 20 years after initial diagnosis, having achieved complete clinical responses with every course of chemotherapy. Although, typically, relapses in indolent lymphomas are increasingly frequent with each successive therapeutic course, this has not been the case in our patient. In light of recent evidence [15,18,19] this might be partly explained because of the addition of rituximab in the last three courses of therapy.
In clinical practice it is not unusual to find a patient where not all clues point to the same diagnosis. This case underscores the need for a comprehensive hematological evaluation, taking into account cytology, cytometry and cytogenetics to reach the proper diagnosis and offer the most appropriate therapeutic options.
References
- Arcaini L, Lazzarino M, Colombo N, Burcheri S, Boveri E, Paulli M, et al. Splenic marginal zone lymphoma: a prognostic model for clinical use. Blood. 2006; 107: 4643-4649.
- Boveri E, Arcaini L, Merli M, Passamonti F, Rizzi S, Vanelli L, et al. Bone marrow histology in marginal zone B-cell lymphomas: correlation with clinical parameters and flow cytometry in 120 patients. Ann Oncol. 2009; 20: 129-136.
- Arcaini L, Paulli M. Splenic marginal zone lymphoma: hydra with many heads? Haematologica. 2010; 95: 534-537.
- Matutes E, Oscier D, Montalban C, Berger F, Callet-Bauchu E, Dogan A, et al. Splenic marginal zone lymphoma proposals for a revision of diagnostic, staging and therapeutic criteria. Leukemia. 2008; 22: 487-495.
- Troussard X, Valensi F, Duchayne E, Garand R, Felman P, Tulliez M, et al. Splenic lymphoma with villous lymphocytes: clinical presentation, biology and prognostic factors in a series of 100 patients. Groupe Français d'Hématologie Cellulaire (GFHC). Br J Haematol. 1996; 93: 731-736.
- Mulligan SP, Matutes E, Dearden C, Catovsky D. Splenic lymphoma with villous lymphocytes: natural history and response to therapy in 50 cases. Br J Haematol. 1991; 78: 206-209.
- Parry-Jones N, Matutes E, Gruszka-Westwood AM, Swansbury GJ, Wotherspoon AC, Catovsky D. Prognostic features of splenic lymphoma with villous lymphocytes: a report on 129 patients. Br J Haematol. 2003; 120: 759-764.
- Swerdlow S, Campo E, Harris NL, Jaffe ES, Pileri SA, Stein H, et al (editors). WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues. Lyon, France: IARC Press. 2008.
- Salido M, Baró C, Oscier D, Stamatopoulos K, Dierlamm J, Matutes E, et al. Cytogenetic aberrations and their prognostic value in a series of 330 splenic marginal zone B-cell lymphomas: a multicenter study of the Splenic B-Cell Lymphoma Group. Blood. 2010; 116: 1479-1488.
- Baseggio L, Traverse-Glehen A, Petinataud F, Callet-Bauchu E, Berger F, Ffrench M, et al. CD5 expression identifies a subset of splenic marginal zone lymphomas with higher lymphocytosis: a clinico-pathological, cytogenetic and molecular study of 24 cases. Haematologica. 2010; 95: 604-612.
- Solé F, Salido M, Espinet B, Garcia JL, Martinez Climent JA, Granada I, et al. Splenic marginal zone B-cell lymphomas: two cytogenetic subtypes, one with gain of 3q and the other with loss of 7q. Haematologica. 2001; 86: 71-77.
- Kalpadakis C, Pangalis GA, Angelopoulou MK, Sachanas S, Kontopidou FN, Yiakoumis X, et al. Treatment of splenic marginal zone lymphoma with rituximab monotherapy: progress report and comparison with splenectomy. Oncologist. 2013; 18: 190-197.
- Kahl B, Yang D. Marginal zone lymphomas: management of nodal, splenic, and MALT NHL. Hematology Am Soc Hematol Educ Program. 2008.
- Cervetti G, Galimberti S, Pelosini M, Ghio F, Cecconi N, Petrini M. Significant efficacy of 2-chlorodeoxyadenosine{+/-} rituximab in the treatment of splenic marginal zone lymphoma (SMZL): extended follow-up. Ann Oncol. 2013; 24: 2434-2438.
- Chacón JI, Mollejo M, Muñoz E, Algara P, Mateo M, Lopez L, et al. Splenic marginal zone lymphoma: clinical characteristics and prognostic factors in a series of 60 patients. Blood. 2002; 100: 1648-1654.
- Montalbán C, Abraira V, Arcaini L, Domingo-Domenech E, Guisado-Vasco P, Iannitto E, et al. Risk stratification for Splenic Marginal Zone Lymphoma based on haemoglobin concentration, platelet count, high lactate dehydrogenase level and extrahilar lymphadenopathy: development and validation on 593 cases. Br J Haematol. 2012; 159: 164-171.
- Camacho FI, Mollejo M, Mateo MS, Algara P, Navas C, Hernández JM, et al. Progression to large B-cell lymphoma in splenic marginal zone lymphoma: a description of a series of 12 cases. Am J Surg Pathol. 2001; 25: 1268-1276.
- Tsimberidou AM, Catovsky D, Schlette E, O'Brien S, Wierda WG, Kantarjian H, et al. Outcomes in patients with splenic marginal zone lymphoma and marginal zone lymphoma treated with rituximab with or without chemotherapy or chemotherapy alone. Cancer. 2006; 107: 125-135.
- Else M, Marín-Niebla A, de la Cruz F, Batty P, Ríos E, Dearden CE, et al. Rituximab, used alone or in combination, is superior to other treatment modalities in splenic marginal zone lymphoma. Br J Haematol. 2012; 159: 322-328.