
Case Report
Ann Hematol Oncol. 2020; 7(8): 1315.
Immune Thrombocytopenia (ITP): Enigma of an Old Disease
Caplan A1, Ahlstrom S2, Sharma A3* and Mollick J4
1Internal Medicine Resident, St. Mary’s Medical Center, San Francisco, USA
2Physician Assistant, Tucson, USA
3Assistant Clinical Professor of Medicine, University of California, San Francisco, USA
4Associate Clinical Professor of Medicine, University of California, San Francisco, USA
*Corresponding author: Atul Sharma, Assistant Clinical Professor of Medicine, University of California, San Francisco, USA. E-mail: atul.sharma@ucsf.edu
Received: September 14, 2020; Accepted: October 12, 2020; Published: October 19, 2020
Abstract
“Immune thrombocytopenia,” formerly Idiopathic Thrombocytopenic Purpura (ITP), an autoimmune disorder, is characterized by isolated thrombocytopenia, with platelet count less than 10 x 10 to the 9th /L [1,2]. Estimated ITP incidence is 100 cases, per million persons per year. Approximately 50% of cases occur in children [3]. In adults, it tends to follow a chronic course, with mucocutaneous bleeding being the most common manifestation [4]. A rare, though major cause of fatal bleeding in patients with ITP, is intracerebral hemorrhage; less than 1% of all cases [5]. Here we discuss a case of a 26-year-old Asian female patient, with refractory ITP and intracerebral hemorrhage, leading to brain death. We explore current treatment recommendations and suggested approaches to therapy as well as challenges.
Keywords: ITP; Immune thrombocytopenia; Idiopathic thrombocytopenic purpura; Intracerebral hemorrhage
Case Presentation
A 26 y/o Asian female, with a three year history of ITP, who had been previously treated with steroids (prednisone and dexamethasone), IVIG, and Eltrombopag (oral TPO analog) for intractable mucocutaneous bleeding with poor response to steroids and IVIG. She had also recently been started on rituximab approximately two weeks prior to presentation. Of note, despite multiple attempts, we were unable to obtain records from the patient’s outpatient hematologist to confirm her diagnostic and treatment history. We were, however able, to confirm that the patient had never been previously hospitalized for ITP symptoms, and thus we postulate that she likely did achieve remission previously.
On this occasion, the patient was sent to the ED, by her hematologist, for progressive LLE pain and worsening oral mucosal bleeding. Her LLE pain was described by the patient as a “tingling sensation moving from the calf to hip, with worsening pain at the hip and knee joints”. She denied recent falls or trauma. She additionally reported the presence of oral hemorrhagic bullae, causing “discomfort with eating and persistent taste of blood.”
She had been hospitalized two weeks prior to this admission with multiple petechiae of the hard and soft palate, spontaneous epistaxis, and ecchymosis of lateral left thigh. She was noted to have a platelet count <1 and received 50 grams IVIG and platelet transfusion, with subsequent improvement of platelets to 41k/ul. Spontaneous bleeding symptoms successively resolved and she was discharged home in stable condition with close outpatient follow up.
When she represented, her vital signs were normal with physical exam notable for bullae of buccal mucosa, and tip and R lateral tongue. Petechiae of bilateral LEs, and ecchymosis of the R lateral thigh and L lateral calf was also found on exam. No joint edema or effusions were noted. The neurological exam was benign. Labs were notable for platelet count of 5K/ul.
The patient was given 50mg IVIG without steroids, however, unlike during previous admission, she did not exhibit decrease in bleeding symptoms. She developed epistaxis shortly after admission. After consult with hematology/oncology, she was given additional IVIG and steroids; methylprednisolone 60 mg twice daily for 4 days. She was not transfused with platelets. The epistaxis ceased.
Approximately 24 hours into her hospital stay a rapid response was called when patient was noted to have an episode of emesis followed by new onset right sided facial droop, with right upper and lower extremity weakness. A Stroke Alert was called. A noncontrast head CT demonstrated a large left basal ganglia bleed, hemorrhage into the adjacent ventricle, and early trapping of the left temporal horn (Figure A). She was immediately transferred to ICU and intubated, due to worsening neurologic deficits and mentation. Immediately after intubation, the patient began to seize, and was given lorazepam IV and a loading dose of Levatiracetem. She was subsequently transferred to a tertiary care center with neurosurgery services.
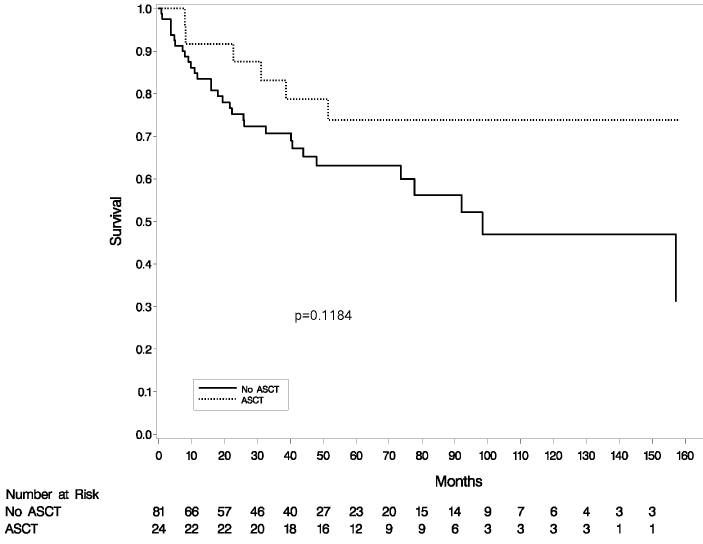
Figure A: Stroke Alert.
On arrival to the tertiary care center, initial non-contrast head CT showed expanding hematoma (Figure B). The patient rapidly lost brainstem reflexes despite maximal medical therapy, including mannitol and strict blood pressure control, with continuous transfusion of platelets. A hematology consultant agreed transfusion of platelets was an appropriate intervention. Her thrombocytopenia contra-indicated surgical intervention. More than 48 hours after admission to the tertiary care center, the patient continued to be comatose, had absent brain stem reflexes, a positive apnea test. She was ultimately pronounced brain dead.

Figure B: Arrival to tertiary care center.
Discussion
The 2019 American Society of Hematology Guidelines for ITP (Figure C) recommends that providers treat ITP primarily with a short course of corticosteroids (<6 weeks) and IVIG for uncontrolled bleeding in patients, with platelet counts <30 x 109/L [6]. In some patients, observation may be sufficient, especially those with platelet count >30 x 109/L with minimal or no bleeding and no other comorbid conditions that merits intervention [7]. Potential side effects of corticosteroids administration include hypertension, hyperglycemia, alteration in sleep and mood, gastric ulcer, glaucoma, myopathy and osteoporosis [8].

Figure C: Flowchart for the identification and treatment of patients with refractory ITP [12]. Ag: Antigen; ANA: Anti-Nuclear Antibodies; CMP: Comprehensive
Metabolic Panel; CRP: C-Reactive Protein; CMV: Cytomegalovirus; ESR: Erythrocyte Sedimentation Rate; Eval: Evaluation; HCV: Hepatitis C Virus; H pylori:
Helicobacter pylori; plt/Plt: Platelets; PT: Prothrombin Time; PTT: Partial Thromboplastin Time; TIBC: Total Iron Binding Capacity; Tx: Treatment.
Combination therapy with rituximab and corticosteroids (recommendation 5) at time of diagnosis is not favored unless remission is highly likely and benefit outweighs potential adverse reactions of rituximab. Additionally, rituximab is desired in adults with corticosteroid dependent or refractory ITP. Thrombopoietic Receptor Agonist (TPO-RA) and splenectomy is an appropriate next step in management in those patients with ITP > 3months who are steroid dependent or non- responsive. Hematology Society Guidelines further suggest second-line treatment with TPO-RA analogs & Rituximab, with cautious monitoring of potential toxicities [6]. When all first line agents have been exhausted and splenectomy is not being pursued, some of the older immunosuppressive agents such as 6-mercaptopurine, Azathioprine, Cyclosporin A, Danazol, Cyclophosphamide, and Mycophenolate can be tried. These older agents are usually used in combination with the more standard treatments discussed above. One treatment approach for refractory ITP is to combine drugs with different mechanisms of action, allowing for potential synergy between agents. For example, initiation of a TPO-RA to boost platelet production in combination with a drug that interferes with platelet clearance (eg, Danazol) or autoantibody production (eg, azathioprine or mycophenolate) can be tried [9].
In this case, the patient was treated prior to hospital admission with corticosteroids, per guidelines, without remission for severe mucocutaneous bleeding symptoms. She received IVIG during her first hospitalization with increase in platelet numbers. Unfortunately, bleeding symptoms resumed after brief remission. She subsequently received a recommended second-line medication, Eltrombopaq, a oral TPO-RA analog, with appropriate reductions in dosage, for Asian ethnicity; starting dosage of 25 mg v 50mg [10]. Eltrombopag is approved for chronic ITP (>12 months) refractory to steroids and IVIG. Some smaller trials have shown that initiation of Eltrombopag earlier in the disease process or at time of diagnosis yields good results [11]. The EXTEND trial demonstrated the improvement of platelet count (Figure D) in those patients treated with Eltrombopag [12]. Again, although Guideline recommended treatment was provided, thrombocytopenia and bleeding persisted. Finally, 4 days prior to her final admission, she received her first dose of Rituximab with 3 more doses planned for the week she was admitted.

Figure D: EXTEND Trial [11].
Refractory ITP carries a poor prognosis. Over time, disease progression and risk of medication induced toxicities increases, leading to poor quality of life and higher hemorrhagic and infections morbidity and mortality [13]. Refractory bleeding in patients with ITP results is associated with the risk of ICH in 1% of patients [5]. This patient was determined to be refractory to medical treatment, post confirmation of failure of primary and second-line treatments, per Society of Hematology Guidelines 2019.
Mainstay of therapy for life threatening hemorrhage includes high dose-corticosteroids, IVIG, and platelet transfusion [14]. Highdose corticosteroids (eg, high-dose dexamethasone or intravenous methylprednisolone) often results in a platelet count improvement by 2-5 days.
IVIG (1-2 g/kg) can produce a platelet count rise even faster, within 12-48 hours [15]. If an immediate rise in platelet count is needed (i.e. in a patient with life threatening intracranial hemorrhage like our patient described above) platelet transfusion is recommended. Our patient received platelet transfusion but her platelet count did not improve.
Although splenectomy can be considered in some medically refractory ITP patients, this patient was not a candidate for surgery, due to low platelet count (<5,000) after recommended medical treatment and transfusion. Tragically, she developed ICH, before additional stabilization could be provided.
Conclusion
ITP is a diagnosis of exclusion that is made in patients with isolated thrombocytopenia. The pathophysiology of ITP is highly complex and much remains poorly understood. The mechanism of ITP is characterized by autoreactive antibodies associated with impaired T and B cells, leading to the destruction of platelets and defects in thrombopoiesis and megakaryocyte maturation1. Current treatments for ITP are directed at different aspects of the cycle of antibody production and platelet sensitization, clearance, and production.
Here we discussed a case of a 26y/o F with medically refractory ITP and intracerebral hemorrhage leading to death. We briefly shed light on current treatment guidelines for ITP,
However, much uncertainty still exists regarding progression of treatment in refractory cases such as this. Randomized trials are lacking that directly compare the efficacy and safety of second- line treatments and significant ambiguity remains leaving treatment choice up to expert opinion. One thing that is clear is the need for individuation.
Until clear data exists, we recommend continuing to treat patients with an individualized, patient centered approach. Treatment choice should be based on patient factors, including duration of ITP, frequency of bleeding episodes requiring hospitalization or rescue medication, comorbidities, age of the patient, medication adherence, medical and social support networks, patient values and preferences, cost, and availability. In the future, biomarkers will hopefully exist to predict responses to specific treatments enabling precision in treatment choice.
References
- Cines DB, Blanchette VS. Immune Thrombocytopenic Purpura. N Engl J Med. 2002; 346: 995-1008.
- Siraj Mithoowani MD, Donald M. Arnold MD. Consultative Hemostasis and Thrombosis (Fourth Edition). 2019.
- Cines DB, Blanchette VS. Thrombocytopenic Purpura. N Engl J Med. 2002; 346: 995-1008.
- Cooper N, Ghanima W. Immune Thrombocytopenia. N Engl J Med. 2019; 381: 945-955.
- Psaila B, Petrovic A, Page LK, Menell J, Schonholz M, Bussel JB. Intracranial Hemorrhage (ICH) in children with Immune Thrombocytopenia (ITP): study of 40 cases. Blood. 2009; 114: 4777–4783.
- Neunert C, Terrell DR, Arnold DM. American Society of Hematology 2019 guidelines for immune thrombocytopenia published correction appears in Blood Adv. 2019; 3: 3829-3866.
- Provan, Drew. “Updated international consensus report on the investigation and management of primary immune thrombocytopenia.” Blood advances. 2019; 3: 3780-3817.
- Buchman AL. Side effects of corticosteroid therapy. J Clin Gastroenterol. 2001; 33: 289- 294.
- Cuker A, Neunert CE. How I treat refractory immune thrombocytopenia. Blood. 2016; 128: 1547-1554.
- Yang R, Li J, Jin J. Multicentre, randomised phase III study of the efficacy and safety of eltrombopag in Chinese patients with chronic immune thrombocytopenia. Br J Haematol. 2017; 176: 101-110.
- Gonzalez-Porras J, Bastida J. Eltrombopag in immune thrombocytopenia: efficacy review and update on drug safety. Therapeutic Advances in Drug Safety. 2018; 9: 263- 285.
- Wong, Raymond SM. “Safety and efficacy of long-term treatment of chronic/ persistent ITP with eltrombopag: final results of the EXTEND study.” Blood. 2017; 130: 2527- 2536.
- Miltiadous O, Hou M, Bussel JB. Identifying and treating refractory ITP: difficulty in diagnosis and role of combination treatment. Blood. 2020; 135: 472-490.
- Izak, Marina, James B Bussel. “Management of thrombocytopenia.” F1000 prime reports. 2014; 6: 45.
- Chugh S, Darvish-Kazem S, Lim W. Rituximab plus standard of care for treatment of primary immune thrombocytopenia: a systematic review and meta-analysis. Lancet Haematol. 2015; 2: 75-81.