
Case Presentation
Ann Hematol Oncol. 2021; 8(9): 1363.
Adrenal Involvement in an SLE Patient with Antiphospholipid Syndrome
Mejía-Torres M, Carrión-Barberà I, Salman-Monte TC* and Monfort J
Department of Rheumatology, PasseigMaritim, Hospital del Mar de Barcelona, Spain
*Corresponding author: Tarek Carlos Salman Monte, Department of Rheumatology, PasseigMaritim 25-29, Hospital del Mar de Barcelona 08003, Spain
Received: June 06, 2021; Accepted: June 25, 2021; Published: July 02, 2021
Keywords
Systemic lupus erythematosus; Antiphospholipid syndrome; Adrenal insufficiency
Introduction
Addison disease related to SLE and mostly to Antiphospholipid Syndrome (APS) is a rare condition that should be suspected in patients presenting with abdominal complaints, fever, hypotension and hyponatremia [1-3]. Its prevalence remains unknown such as its time of onset once SLE or APS are diagnosed [3]. Nowadays, there is not enough evidence for recommending systematic screening regarding this involvement.
Its estimated mortality is 3.81% [1]. Nevertheless, under correct treatment, long-term survival is quite favourable [4]. Our main objective is to remind a very uncommon but life-threatening complication that might affect patients with Antiphospholipid Syndrome (APS) associated to SLE.
Case Presentation
In April 2018, a 44-year-old man was admitted to the Emergency Room with asthenia, nausea, weight loss (15 kg in one month), hypotension, renal impairment and hyperpigmentation. His medical history was positive for APS with two episodes of deep vein thrombosis when he was 14 and 17 years old. He was under treatment with acenocoumarol since then. Later, he met 2012 Systemic Lupus International Collaborating Clinics (SLICC) Classification Criteria for SLE (positive ANA test, lymphopenia, low C3 complement and APS antibodies) [5].
The week before, he had been admitted to the Nephrology hospitalization ward with the same symptoms and acute kidney injury AKI2 attributed to acute interstitial nephritis (due to history of treatment with NSAIDs and antibiotics for an otitis media) vs. acute tubular necrosis because the patient had already low blood pressure assumed to be caused by treatment with enalapril and low fluid intake. Methylprednisolone bolus and fluid therapy were prescribed. An echocardiogram revealed no pathological findings. His Quick PT at that time was 6,7%.
Considering all these previous events, the persistence of the symptoms and absence of response to fluid therapy, adrenal insufficiency was suspected. Therapy with hydrocortisone was started with the indication to increase dose under stress situations and the patient was referred to the Endocrinology Outpatient Facility.
An ACTH-cortisol test revealed low cortisol levels with stimulated ACTH. Addison disease was confirmed. 21-hydroxylase antibodies were negative, and an abdominal CT revealed adrenal bilateral nodules (Figure 1a). An adrenal MRI was compatible with bilateral haemorrhage (Figure 1b) and 17-OH progesterone levels were normal. Other causes, such as TB infection were excluded. Currently, the patient is totally recovered, under treatment with hydrocortisone, with high ACTH levels.
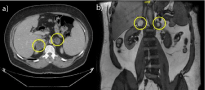
Figure 1: a) Bilateral adrenal nodules by CT. b) Bilateral adrenal haemorrhage
by MRI.
Discussion
Adrenal involvement in SLE patients with APS normally affects both glands in the form of venous thrombosis or adrenal haemorrhage. Autoimmune origin and microthrombi have been described [1-3]. Bilateral involvement might be due to anatomical and histological reasons (artery-vein ratio 3:1 [2-4,6] and similarities between the APS antibodies targets and adrenal cortical cells membranes [2,3,7]). Glandular damage is irreversible, and atrophy seems to be the outcome [2,3].
Most of its evidence is based on case reports [1]. No diagnostic algorithm has been stablished. Electrolyte, hormonal and autoimmune testing are necessary [1-3]. Infiltration, haematoma, malignancy or adrenal infection should be excluded through imaging studies [1-3]. Glucocorticoid supplementation is mandatory. Mineralocorticoid treatment depends on the plasma renin activity and the aldosterone levels [1,2]. Follow-up for evaluation of long-term adrenal function is very important [2].
Conclusion
We describe a case of primary adrenal insufficiency in a patient with SLE and APS with a short delay in the diagnosis and with a very good response to glucocorticoid treatment. Despite its low incidence, this complication should be considered in SLE/APS patients.
References
- Lee KH, Lee H, Lee CH, Kim JY, Kim JM, Kim SS, et al. Adrenal insufficiency in Systematic Lupus Erythematosus (SLE) and Antiphospholipid Syndrome (APS): A systematic review. Autoimmun Rev. 2019; 18: 1-8.
- Bansal R, Nath PV, Hoang TD, Shakir MKM. Adrenal insufficiency secondary to bilateral adrenal hemorrhage associated with antiphospholipid syndrome. AACE Clin Case Rep. 2019; 6: e65-e69.
- Mlekuš Kozamernik K, Jensterle M, Ambrožic A, Pfeifer M. Adrenal failure and antiphospholipid syndrome. J Int Med Res. 2020; 48: 300060520903659.
- Ramon I, Mathian A, Bachelot A, Hervier B, Haroche J, Boutin-Le Thi Huong D, et al. Primary adrenal insufficiency due to bilateral adrenal hemorrhageadrenal infarction in the antiphospholipid syndrome: long-term outcome of 16 patients. J Clin Endocrinol Metab. 2013; 98: 3179-3189.
- Petri M, Orbai AM, Alarcón GS, Gordon C, Merrill JT, Fortin PR, et al. Derivation and validation of the Systemic Lupus International Collaborating Clinics classification criteria for systemic lupus erythematosus. Arthritis Rheum. 2012; 64: 2677-2686.
- Presotto F, Fornasini F, Betterle C, Federspil G, Rossato M. Acute adrenal failure as the heralding symptom of primary antiphospholipid syndrome: report of a case and review of the literature. Eur J Endocrinol. 2005; 153: 507-514.
- Berneis K, Buitrago-Téllez C, Müller B, Keller U, Tsakiris DA. Antiphospholipid syndrome and endocrine damage: why bilateral adrenal thrombosis? Eur J Haematol. 2003; 71: 299-302.