
Editorial
Ann Hematol Oncol. 2022; 9(6): 1411.
How to Prevent and Control Sickle-Cell Anaemia and β-Thalassemia Major in the Tribal People of the Scheduled Area of Rajasthan (India)?
Choubisa SL*
Department of Advanced Science and Technology, National Institute of Medical Science and Research, NIMS University Rajasthan, Jaipur, Rajasthan 303121, India
*Corresponding author: Choubisa SL, Department of Advanced Science and Technology, National Institute of Medical Science and Research, NIMS University Rajasthan, Jaipur, Rajasthan 303121, India
Received: October 03, 2022; Accepted: October 28, 2022; Published: November 04, 2022
Abstract
In India, Rajasthan is the largest state and it has total number of 33 districts. Eight of these districts, namely Banswara, Chittourgarh, Dungarpur, Pali, Pratapgarh, Rajasamand, Sirohi, and Udaipur districts have been grouped together as the “scheduled area” of Rajasthan. This is the most backward and underdeveloped area where more than 70% of the tribal populations reside. In this area, most dominating endogamous tribes are Bhil, Damor, Meena, Garasiya, Kathudia, and Sahariya and several communicable, noncommunicable and water-borne diseases are endemic. Some inheritable life threatening red cell genetic diseases or disorders, such as sickle-cell anaemia (Hb-SS) and β-thalassaemia major are also endemic in this tribal region. The maximum prevalence of genes in trait form of these genetic diseases in tribals has been found 31.14% and 9.00%, respectively. However, sickle-cell and β-thalassaemic genes are important and highly significant as these are causing morbidity and mortality in the tribal people. In fact, sickle-cell anaemia and β-thalassaemia major are lethal and found in adults and children, respectively. The curative option of these genetic diseases is bone marrow transplant and their available remedy is lifelong blood transfusion and removal of iron by chelation therapy. Both the options not only cost more, but also cause constant torment to the child. The cost of bone marrow technology is also so high that it is not easy for tribals to afford it. Secondly, this technology is not so accessible that everyone can get its facility. But by adopting special measures, the occurrence of these dangerous genetic diseases in tribals can be prevented and controlled. In this communication, these measures have been focussed.
Keywords: β-thalassaemia; Erythrocyte; Genes; Prevention and control; Red cell genetic disorders or diseases; Rajasthan; Scheduled area; Sickle-cell anaemia (Hb-SS); Tribals; India
Introduction
In India, Rajasthan is the largest state and it has total number of 33 districts. Eight of these districts, namely Banswara, Chittourgarh, Dungarpur, Pali, Pratapgarh, Rajasamand, Sirohi, and Udaipur districts have been grouped together as the scheduled area which is located in south eastern part of Rajasthan (Figure 1). This area is the most backward and underdeveloped and characterised with preponderance of diverse tribal communities. As per Census of 2011, total population of scheduled area is 64, 63,353, out of which scheduled tribe population is 45, 57, 917 which is 70.43% of the total population of the scheduled area. Three districts of this tribal dominating area, namely Banswara, Dungarpur and Pratapgarh are known as full tribal districts and remaining are partial tribal districts. In this area, the most dominating endogamous and tribes are Bhil, Damor, Meena, Garasiya, Kathudia and Sahariya and several parasitic and non-parasitic and water-borne diseases are endemic [1-23]. However, few inheritable life threatening diseases, such as sickle-cell anaemia (Hb-SS), a and β-thalassaemia syndromes, and G-6-PD are also endemic in tribals of this area [24-38].
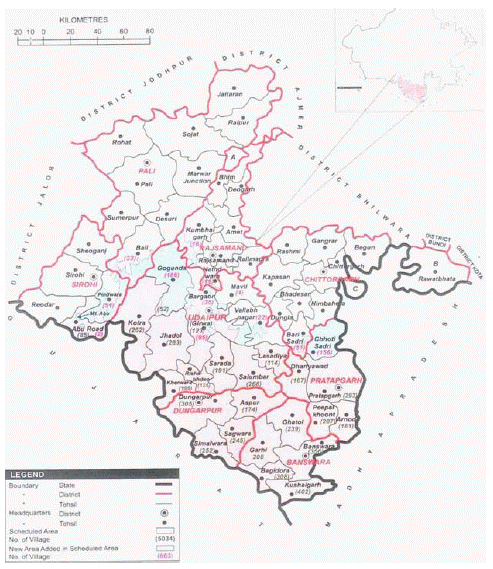
Figure 1: Map showing scheduled area of Rajasthan as per notification of Government of India, 2018.
The socio-economic and nutritional status, literacy rate, and health education in the tribal people of this area is very poor. These people are not even health conscious. In general, tribal people prefer to live in the forest and remote hilly areas in isolated form. Financially, tribals are depending on traditional agriculture, animal husbandry, and forest yields. However, for daily income, they prefer daily wages and farming work. These people have several health deteriorating bad habits, such as consuming of wine, smoking, and tobacco. In general, tribal people are shy, conservative, highly orthodox, and superstitious.
Status of Sickle-cell and β-thalassaemic Genes in Tribals
In India, erythrocyte genetic disorders (haemoglobinopathies and G6PD deficiency) have been extensively studied in diverse populations of different states and union territories [39-49]. In the state of Rajasthan, haemoglobinopathies (abnormal haemoglobins and a and β-thalassaemia) and G6PD deficiency have also been well studied in subjects belonging to different populations, such as Schedule Tribe (ST), Schedule Caste (SC), Other Backward Caste (OBC), General Caste (GC) populations, and minor communities as well [50-56].
It is well documented that abnormal or mutant haemoglobins (Hbs) are synthesised due to structural defects either in alpha or beta polypeptide chains of globins by the mechanism of substitution or deletion of amino acid residues. This is also known as ‘point mutation’ which is generally taking place under the control of genes that are responsible for synthesis of Hb molecule. In human population, more than 1100 abnormal or mutant Hbs have already been identified. However, medical and health and evolutionary point of view, sicklecell haemoglobin (Hb-S) is important and highly significant.
In India, Hb-S is the commonest genetic disorder and more prevalent in various populations as compared to other abnormal Hb variants. However, the maximum incidence of sickle-cell gene has been reported in tribal subjects of different geographical provinces [39,47]. In the country, the origin of sickle-cell gene is still controversial. However, this gene was detected for first time in India by Lehman and Cutbush [57]. These workers have reported relatively a high incidence (3.3% to 30.0%) of Hb-S genes in diverse tribes. In the north eastern, western, southern, and central India, the prevalence of Hb-S gene in diverse tribal communities found to be 0-18%, 0-33.5%, 1-40%, and 22.5-44.4%, respectively and its frequency varies between 0.31- 0.41 [58]. In the scheduled area of Rajasthan, the maximum prevalence of Hb-S gene was found to be 14.6% and 31.14 % in Gameti and Garasiya tribes, respectively [24]. From this area, 1.47% incidence of sickle-cell gene in homozygous state (Hb-SS or sickle-cell anaemia) in Bhil tribe has also been reported [31]. The co-inheritance of the Hb-S gene with abnormal Hb-C (Hb-SC) was also reported in tribals of scheduled area [34,59] which is the rarest combination being reported from India (Figure 2).
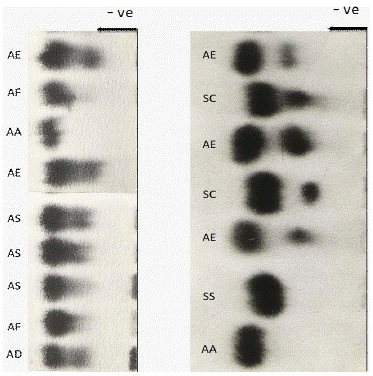
Figure 2: Paper-electrophorosis showing migration pattern of Hb variants
detected in various populations of scheduled areas of Rajasthan, India [50].
Thalassaemia is also one of the haemoglobinopathies and found more common in diverse Indian populations. Abnormal Hbs are the resultant of changes in structure of polypeptide a and β- globin chains while thalassaemia is due to delay or unbalanced production of these chains. During their production, both are structurally normal. Based on delay in synthesis of a and β- globin chains, two forms of thalassaemia, a and β-thalassaemia are recognised which are widely distributed globally. However, medical and health point of view, β-thalassaemia is more significant.
In almost all the Indian populations, genes for both β- thalassaemia minor (trait) and β- thalassaemia major (disease) are endemic and rampant with varying incidence. This indicates that India is a rich reservoir for β-thalassaemic genes [43,45,46,60]. Subjects having these genes are the carriers of β- thalassaemia major. Generally, these people (carriers) are normal in appearance and live life-long as healthy person. The frequency of β- thalassaemia carriers in India varies from 1% to 17% with an average of 3.2% [60]. However, β-thalassaemia major is lethal and found in children.
In the scheduled area, the incidence of β-thalassaemic genes varied greatly in various tribes. The maximum prevalence (9.0%) of β- thalassaemia trait was reported in the Bhil tribe. However, 0.35% prevalence of β- thalassaemia trait in GC, 3.96% in SC and 7.05% in OBC population has also been reported [50]. In few unrelated tribal children, genes β- thalassaemia major have also been detected. However, interaction β-thalassaemic genes with genes of abnormal Hb-S, D and E has also been detected in the scheduled area but the prevalence of such association of mutant genes are rare [50,61].
Prevention and Control
It is well known that Hb-S and β- thalassaemic genes appear in individuals in homozygous state then causes serious and lifethreatening diseases, sickle-cell anaemia (Hb-SS) and β- thalassaemia major, respectively, Both are responsible for morbidity and high rate of mortality in them. In fact, both the diseases are fatal. It is estimated that 35 to 45 million people are silent carriers of the β- thalassaemia in India [62]. Every year about 10,000 children are born with thalasseamia major in the country accounting for 10% of thalasseamia major worldwide. Around eight to ten thousand cases of thalasseamia being added every year in India. In fact, India has a huge burden with an estimated around 100,000 patients with a β-thalassemia syndrome and around 150,000 patients with sickle- cell disease [62]. Whatsoever, in the country, both the diseases are more prevalent in tribal population as compared to non-tribal populations.
Mostly, illiterate tribal people of scheduled area, generally, used their own traditional methods for the treatment of sickle-cell anaemia and β-thalassaemia. One of the methods, which is cruel, terrible and very painful method, they stained with hot iron rods on the patient’s forehead, hands, feet, abdomen, etc. for the treatment. Many times patients die by this non-scientific method.
The curative option of these red cell genetic diseases is stem cell therapy or bone marrow transplant and their available remedy is lifelong blood transfusion and removal of iron by chelation therapy. Both the options not only cost more, but also cause constant torment to the child. The cost of bone marrow technology is also so much that it is not a matter for everyone to afford it. And it is not possible at all for tribal people. Secondly, this technology is not so accessible that everyone can get its facility. Therefore, to save the tribal health and economy, the prevention and management are better options so that these diseases can be control in the coming generation of tribal people.
For the prevention and control of these diseases, it is necessary to identify their carriers prominently and create awareness among the tribal people about them. Both of these are such important factors by which the expected success in controlling these diseases is achieved. But for this there is a need for proper, timely, and effective management. In every district Government hospital of scheduled area, it is necessary to have a genetics consultant along with adequate screening or testing facilities for the identification of carriers. Those who are carriers of these diseases, as far as possible, they should neither be married nor have physical relations with them. It is necessary to take these steps so that children are not born with such red cell genetic diseases. This is possible through genetic counselling by genetic counsellor. A concentrated effort towards education and awareness generation will continue to be needed in the tribals of scheduled area. At least one community health centre at each block should have prenatal diagnosis and fetal sampling procedures. Abortion of such pregnant babies having red genetic defects also helps in the prevention of these diseases or can lead to a significant reduction in affected births. Stem cell transplantation in Government hospital at regional level should be encouraged for low risk patients and families who can afford the cost.
A joint effort by all, the Rajasthan State Government with help from NGOs and corporate houses and strongly backed by political support would be required for success of prevention and control programme for these genetic diseases in the scheduled tribal area of Rajasthan. Moreover, in the scheduled area, the implementation and following the guidelines for the prevention and control of sickle-cell disease and β-thalassaemia prepared by the National Health Mission, Ministry of Health and Family Welfare, New Delhi (2016) is also useful and highly suggestive.
Conclusions
In scheduled area of Rajasthan, genes of sickle-cell anaemia and β-thalassaemia major are endemic in the tribal people. The highest incidences of these genes in trait form are found to be 31.14% and 9.0%, respectively. When these genes occur in homozygous states then these are more serious to health and causing considerable morbidity and mortality among the tribal people. Both the red cell inheritable diseases are fatal, irreversible and untreatable. Therefore, it is more important to run a health project with the help from Rajasthan State Government and NGOs in the most backward and underdeveloped scheduled area of Rajasthan to prevent and control of these dreaded genetic diseases in the tribal individuals. It is also suggestive that “neonatal screening” is also better way for early diagnosis of these lethal diseases and their carriers.
Acknowledgements
The author thanks to Dr. Anurag Choubisa, Geetanjali Medical College and Hospital, Udaipur 313002, India for cooperation.
References
- Choubisa SL, Sharma PN, Parmar L. Haemoglobin-A2 and glucose-6- phosphate dehydrogenase deficiency in relation to malaria. Indian Journal of Parasitology.1984; 8: 247-249.
- Choubisa SL, Sharma PN. Incidence of larval trematodes infection and their seasonal variation in the fresh water molluscs of southern Rajasthan. Records of Zoological Survey of India. 1986; 83: 69-80.
- Choubisa SL, Choubisa L. Prevalence of vaginal Trichomoniasis in Dungarpur district, Rajasthan. Indian Journal of Parasitology. 1991; 15: 97-99.
- Choubisa SL, Choubisa L. Prevalence of intestinal and malaria parasitic infections in tribal students of Dungarpur (Rajasthan). Indian Journal of Parasitology. 1992; 16: 55-57.
- Choubisa SL. Guinea worm (Dracunculus medinensis) in Rajasthan, India: A case report. Journal of Parasitic Diseases. 2002; 26: 105-106.
- Choubisa SL, Choubisa DK, Choubisa L. Focus on red cell genetic defects and malaria. Journal of Parasitic Diseases. 2003; 27: 99-103.
- Choubisa SL, Choubisa DK, Choubisa L. The ABO blood groups and malaria. Journal of Parasitic Diseases. 2005; 29: 109-111.
- Choubisa SL, Choubisa L. Trichomonas veginalis parasitic infection (Trichomoniasis) in subjects inhabiting rural environment of tribal region of southern Rajasthan. Journal of Parasitic Diseases. 2005; 29: 77-80.
- Choubisa SL, Choubisa L. Intestinal helminthic infections in tribal population of southern Rajasthan, India. Journal of Parasitic Diseases. 2006; 30: 163- 167.
- Choubisa SL. Amoebiasis among tribals of Rajasthan (India). Journal of Communicable Diseases. 2009; 41: 53-55.
- Choubisa SL, Verma R, Choubisa L. Dracunculiasis in tribal region of Rajasthan (India): A case report. Journal of Parasitic Diseases. 2010; 34: 94-96.
- Choubisa SL, Jaroli VJ, Choubisa P, Mogra N. Intestinal parasitic infection in Bhil Tribe of Rajasthan, India. Journal of Parasitic Diseases. 2012; 36: 143-148.
- Choubisa SL, Jaroli VJ. Gastrointestinal parasitic infections in diverse species of domestic ruminants inhabiting tribal rural areas of southern Rajasthan, India. Journal of Parasitic Diseases. 2013; 37: 271-275.
- Choubisa SL, Choubisa DK, Joshi SC, Choubisa L. Fluorosis in some tribal villages of Dungarpur district of Rajasthan, India. Fluoride. 1997; 30: 223-228.
- Choubisa SL. Fluoride distribution and fluorosis in some villages of Banswara district of Rajasthan. Indian Journal of Environmental Health. 1997; 39: 281- 288.
- Choubisa SL. Fluorosis in some tribal villages of Udaipur district (Rajasthan). Journal of Environmental Biology. 1998; 19: 341-352.
- Choubisa SL. Chronic fluoride intoxication (fluorosis) in tribes and their domestic animals. International Journal of Environmental Studies. 1999; 56: 703-716.
- Choubisa SL. Endemic fluorosis in southern Rajasthan (India). Fluoride. 2001; 34: 61-70.
- Choubisa SL, Choubisa L, Choubisa DK. Endemic fluorosis in Rajasthan. Indian Journal of Environmental Health. 2001; 43: 177-189.
- Choubisa SL. Fluoride in drinking water and its toxcosis in tribals, Rajasthan, India. Proceedings of National Academy of Sciences, India Section B: Biological Science. 2012; 82: 325-330.
- Choubisa SL, Choubisa D. Neighbourhood fluorosis in people residing in the vicinity of superphosphate fertilizer plants near Udaipur city of Rajasthan (India). Environmental Monitoring and Assessment. 2015;187(8):497.doi: 10.1007/s10661-015-4723-z.
- Choubisa SL. A brief and critical review of hydrofluorosis in Rajasthan, India. Fluoride. 2018; 51: 13-33.
- Choubisa SL. Status of chronic fluoride exposure and its adverse health consequences in the tribal people of the scheduled area of Rajasthan, India. Fluoride. 2022; 55: 8-30.
- Negi RS. Sickle cell distribution in India. Ph. D. thesis, Calcutta University, Calcutta, India, 1967.
- Jain RC, Andrew AMR, Choubisa SL, Acharya A, Joshi KC. Sickle cell gene in the Mina tribal population of Kherwara tehsil of Udaipur district in Rajasthan. Indian Journal of Medical Research. 1983; 78: 522-555.
- Jain RC, Andrew AMR, Choubisa SL. Sickle cell and thalassaemic genes in tribal population of Rajasthan. Indian Journal of Medical Research. 1983; 78: 836-840.
- Jain RC, Choubisa SL, Acharya A, Andrew AMR, Chhaparwal JK, Joshi KC. Incidence of G-6-PD deficiency in the tribal population of southern Rajasthan. Journal of Association of Physicians of India. 1983; 32: 266-267.
- Choubisa SL, Choubisa L, Pande S, Srivastava YK. Incidence of abnormal haemoglobins and G-6-PD deficiency in school children of Udaipur (Rajasthan), India. Journal of Tropical Medicine and Hygiene. 1987; 90: 215- 216.
- Choubisa SL. Sickle cell traits in Damor tribe of Dungarpur district, southern Rajasthan. Man in India. 1990; 70: 454-458.
- Choubisa SL. Distribution of Hb-Bart’s (a-thalasseamia) in various population of Dungarpur district of Rajasthan (India). Indian Journal of Physical Anthropology and Human Genetics.1990; 6: 43-48.
- Choubisa SL. Abnormal haemoglobins, thalassaemia and G-6-PD enzyme deficiency in Rajasthan (Western-India). Haematologia. 1991; 24: 153-165.
- Choubisa SL, Choubisa DK, Khare S. a-thelasseamia (Hb-Bart’s) in Rajasthan (India). Haematologia. 2000; 30: 209-213.
- Choubisa SL, Choubisa L. Erythrocyte mutant genes in inhabitants of arid environment of Western-Rajasthan (India). Indian Journal of Physical Anthropology and Human Genetics. 2006; 25: 45-50.
- Choubisa SL, Choubisa DK, Choubisa, L. Erythrocyte genetic disorders in inhabitants of Aravali hilly environment. Indian Journal of Physical Anthropology and Human Genetics. 2004; 23: 145-159.
- Choubisa SL. Sickle cell haemoglobin, thelasseamia and G-6-PD enzyme deficiency genes in Garasiya tribe inhabited malaria endemic areas of Sirohi district, Rajasthan (India). Journal of Communicable Diseases. 2009; 41: 13- 18.
- Choubisa SL, Choubisa A. Status of erythrocyte genetic disorders in people of desert and humid environments, Rajasthan, India: focus on natural selection in tribals against malaria. Proceedings of Indian National Science Academy. 2021; 87: 433-445.
- Choubisa SL, Choubisa A. A brief review of sickle-cell haemoglobin, β-thalassaemia and G-6-PD deficiency genes among tribals of scheduled area of Rajasthan, India: focus on tribal health. Journal of Biomedical Research and Environmental Sciences. 2021; 2: 1187-1196.
- Mohanty SS, Parihar S, RK Huda, Toteja GS, Sharma AK. Prevalence of sickle cell anemia, β-thalassemia and glucose-6-phosphate dehydrogenase deficiency among the tribal population residing in the Aravali hills of Sirohi region of Rajasthan state. Clinical Epidemiology and Global Health. 2022; 13: 100916.
- Bhatia HM, Rao VR. Genetic Atlas of India. Institute of Immunohaematology, Indian Council of Medical Research, Seth GS Medical College, Bombay, India, 1987.
- Patel AB, Athavale AM. Sickle cell disease in Central India. Indian Journal Paediatrics. 2004; 71: 789-793.
- Balgir RS. The burden of haemoglobinopathies in India and the challenges ahead. Current Science. 2000; 79: 1536-1547.
- Balgir RS. Spectrum of haemoglobinopathies in the state of Orissa, India: A ten years cohort study. Journal of Association and Physicians of India. 2005; 53: 1021-1026.
- Sarnaik SA. Thalassaemia and related haemoglobinopathies. Indian Journal of Pediatrics. 2005; 72: 319-324.
- Munshi A, Anandraj MP, Joseph J, Shafi G, Anila AN, et al. Inherited hemoglobin disorders in Andhra Pradesh. India: a population study. Clinica Chimica Acta. 2009; 400: 117-119.
- Colah R, Gorakshakar A, Phanasgaonkar S, et al. Epidemiology of β-thalassemia in western India: mapping the frequencies and mutation in sub-regions of Maharashtra and Gujarat. British Journal of Haematology. 2010; 149: 739-747.
- Colah RB, Mukherjee MB, Martin S, Ghosh K. Sickle cell disease in tribal populations in India. Indian Journal of Medical Research. 2015; 141: 509-515.
- Patel A, Naik P, Shah M, Narmadeshwar S, Prakash P et al. Prevalence of common hemoglobinopathies in Gujarat: an analysis of a large population screening programme. National Journal of Community Medicine. 2012; 3: 112-116.
- Ghosh K, Colah RB, Mukherjee MB. Haemoglobinopathies in tribal populations of India. Indian Journal of Medical Research. 2015; 141: 505- 508.
- Serjeant GR, Ghosh K, Patel J. Sickle cell disease in India: a perspective. Indian Journal of Medical Research. 2016; 143: 21-24.
- Choubisa SL. Study of certain haematological genetic polymorphic systems in relation to malaria endemicity in tribes residing in arid and humid ecosystems of Rajasthan. A technical report. Indian Council of Medical Research, New Delhi. 1997; 1-24.
- Choubisa SL, Parmar L, Purohit VK. Abnormal haemoglobins in subjects belonging to scheduled castes of Udaipur district (Rajasthan). Indian Journal of Medical Research. 1984; 80: 463-468.
- Choubisa SL. Sickle cell haemoglobin, glucose-6-phosphate dehydrogenase deficiency and thalassaemic genes in relation to malaria endemicity. Indian Journal of Parasitology. 1985; 9: 131-133.
- Choubisa SL, Parmar L, Chouhan MB, Sharma SL. Sickle cell trait in scheduled castes of Rajasthan. Indian Journal of Pathology and Microbiology. 1986; 29: 386-390.
- Choubisa SL, Choubisa L, Pande S, Bhatt DK. Abnormal haemoglobins, thalassaemia and G-6-PD deficiency in Suthar community of southern Rajasthan. Indian Journal of Physical Anthropology and Human Genetics. 1987; 14: 9-16.
- Choubisa SL. Abnormal haemoglobins, thalassaemia and G-6-PD deficiency in school children belonging to scheduled castes and tribes of Rajasthan, India. Indian Journal of Anthropology and Human Genetics. 1988; 14: 31-40.
- Choubisa SL. Erythrocyte genetic disorders in subject belonging to general castes and other backward castes of Aravali hilly region of Rajasthan (India). Indian Journal of Physical Anthropology and Human Genetics. 2003; 22: 33- 43.
- Lehmann H, Sukumaran PK. Sickle cell trait in Southern India. British Medical Journal. 1952; 1: 404-405.
- Kaur M, Dangi CBS, Singh M, Singh H, Kapoor S. Burden of sickle cell diseases among tribes of India- a burning problem. International Research Journal of Pharmacology and Applied Sciences. 2013; 3: 60-80.
- Choubisa SL. Haemoglobin-C gene in India? Current Science. 2010; 99: 860.
- Agarwal MB. The burden of haemoglobinopathies in India - time to wake up? (Editorial). Journal of Association of Physicians of India. 2005; 53: 1017-1018.
- Bansal RK, Sharma UB, Singh M, Saxena JS. Haemoglobinopathies in anaemic children of eastern Rajasthan. Indian Pediatrics. 1988; 25: 10-12.
- Colah R, Italia K, Gorakshakar A. Burden of thalassemia in India: The road map for control. Pediatric Hematology Oncology Journal. 2017; 2: 79-84.