Research Article
Austin J HIV/AIDS Res. 2014;1(2): 6.
Assessment of Anesthesiology and General Surgery Residents’ Knowledge of HIV/AIDS & Implications for Residency Education
Antonio Hernandez Conte*1, Robert Wong1, Jason Park2, Jillian Gottlieb2, Jun Tang1, Troy LaBounty3
1Department of Anesthesiology, Cedars-Sinai Medical Center, USA
2Department of Internal Medicine, Cedars-Sinai Medical Center, USA
3Department of Medicine, University of Michigan Medical Center, USA
*Corresponding author: Antonio Hernandez Conte, Cedars-Sinai Medical Center, 8700 Beverly Blvd, Suite 8211, Los Angeles, CA, 90048, USA
Received: October 17, 2014; Accepted: November 27, 2014; Published: November 29, 2014
Abstract
Study Objective: The authors were interested in ascertaining if educational modules pertaining to HIV/AIDS were offered to anesthesiology and general surgery residents and to assess the fund of knowledge related to HIV/AIDS.
Design: An email with an electronically-linked survey was mailed to the program directors of all anesthesiology and general surgery programs in the U.S. approved by the ACGME. In addition, the respective residency directors were asked to complete a survey regarding HIV/AIDS education.
Setting: The study was conducted in anesthesiology and general surgery residency programs in the U.S.
Subjects: The subjects were anesthesiology and general surgery residents, as well as residency program directors of both specialties.
Interventions: Interventions consisted of survey questions and associated responses to the 16-question (residents) and 6-question (program directors) surveys.
Measurements: Correctness of responses was recorded on all questions of the surveys; descriptive statistics and chi-square analysis were performed.
Main Results: The majority of anesthesiology (86%) and general surgery (87%) residents responded that they had not received any formal education pertaining to HIV/AIDS. Although both groups demonstrated a basic fund of knowledge of HIV/AIDS, more detailed questions led to higher incorrect responses between the two groups. Both groups of residents (anesthesiology – 89%; general surgery – 87%) believed that they would benefit from additional HIV/AIDS education during their training. The majority of anesthesiology and general surgery programs do not provide formal didactic or clinical training modules related to HIV/AIDS, but they personally believe this to be an important issue that warrants education during training.
Conclusions: This nationwide survey demonstrated that anesthesiology and general surgery residents in the U.S. lack formalized education in HIV/ AIDS, and they admit that this education is desired during their training. The authors of this study recommend that formal educational modules pertaining to HIV/AIDS be implemented during residency.
Keywords: Anesthesiology residency education; General surgery residency education; HIV/AIDS knowledge; HIV/AIDS perioperative education
Introduction
Since the initial reporting of the first clinical cases of the Human Immunodeficiency Virus-1 (HIV) and subsequent delineation of Acquired Immune Deficiency Syndrome (AIDS) thirty years ago, scientists and physicians have achieved a remarkable understanding of the pathogenesis of HIV, identified the clinical markers of progression from acute HIV infection to AIDS, defined the HIV/ AIDS clinical continuum and developed highly active antiretroviral treatment (HAART) [1-5].
In the 21st century, primary care physicians and infectious disease specialists are now effectively managing the long-term care of HIV seropositive (+) patients with great success. As a result of the aforementioned advances, persons with HIV and/or AIDS are living longer and more productive lives [6]. Due to the natural aging process, HIV/AIDS-associated pathology, and/or HAART-induced co-morbidities, patients with HIV/AIDS are presenting for surgical procedures at an increasing rate and for procedures similar to non- HIV infected individuals [7,8].
The majority of care in the perioperative setting in the United States is delivered by surgeons and anesthesiologists. Since the early days of the epidemic, these two medical specialties have been on the frontlines attending to the care patients with HIV/AIDS; however, their roles have dramatically changed from a supportive or palliative one to a more active role over the last fifteen years. The objective of this study was to ascertain if anesthesiology and general surgery residents receive formal exposure to HIV/AIDS didactic education and clinical training, as well as to evaluate basic fund of knowledge and responses to clinical situations pertaining to HIV/ AIDS. In addition, the authors also sought to objectively corroborate the presence or absence of formal HIV/AIDS-related educational programs in anesthesiology and general surgery residency programs by directly surveying program directors of both specialties.
Materials and Methods
Institutional Review Board (IRB) approval at Cedars-Sinai Medical Center was obtained prior to conducting this study, and the study is in full accordance with the principles set forth in the Helsinki agreement governing human medical studies. The primary tool utilized was a multiple-choice, voluntary survey posted on a web-based interface (www.surveymonkey.com, Portland, Oregon). A letter explaining the study and associated survey was sent by electronic-mail (e-mail) to all Accreditation Council of Graduate Medical Education (ACGME)-approved anesthesiology and general surgical residency program directors in the United States. A total of 132 anesthesiology and 247 general surgery ACGME-approved were listed in the online directory, however, only 93 anesthesiology programs and 169 programs provided e-mail contact information in the ACGME directory. Program directors were asked to forward the letter to their respective residents for review and voluntary participation; the email letter contained a direct link to the online survey posting which allowed anonymous completion and also contained online data collection, retrieval, and analysis tools. Residents were not able to view other respondent’s answers and were not informed as to the correctness of their responses.
The resident survey consisted of 16 questions with multiple-choice answers (“Yes/No”&“Best answer”). The survey questions ranged from general demographic details about level of training, size-of-city in which residency was located, presence of educational curriculum pertaining to HIV/AIDS, number of patients managed per year with HIV/AIDS, basic and advanced fund of knowledge questions for HIV/AIDS, hypothetical clinical situations, and self-assessment regarding need for further HIV/AIDS education (See Appendix A). Two questions were modified between the surgical and anesthesiology groups in order to more accurately assess specialty-specific issues of clinical care, however, the two questions were similar in nature and intent of discovery of knowledge base for that respective specialty so that comparison between the two specialties could be achieved.
Anesthesiology and general surgery program directors with listed email contacts were sent a letter requesting that they participate in a survey (see Table A) as well. The letter included an electronic link to an online survey composed of six multiple-choice questions. The survey’s purpose was to directly determine if educational modules pertaining to HIV/AIDS education were provided at their respective programs and to corroborate residents’ responses to the presence or absence of HIV/AIDS educational modules.
QUESTION #1��������������������������������������������������������������������������������������� ����������������ANESTHESIOLOGY� �SURGERY�� ��P-value
��������� ������������������������������������������������������������������������������������������������������������������������������������(N=71)��������������� �����(N=139 )
Is your program approved by the American Council in Graduate Medical Education?
q YES� �����100%��������� ��������100%������ ���P= 1.0
q NO�������������
QUESTION #2
Does your program offer formal didactic lecture(s) focused on “Universal Precautions”?
qYES� �������68.2%�������������� �76.2%���� ���P= 0.18
qNO��� �������32.8%�� �������������23.8%
QUESTION #3
Does your residency program offer didactic lecture(s) focused on prevention of infectious disease transmission?
qYES� �������55.6% ���������������65.9%� ������P= 0.11
qNO�� ��������44.4%���� �����������34.1%
�
QUESTION #4
Does your residency program offer didactic lecture(s) on perioperative management of the patient with HIV/AIDS undergoing surgery and/or anesthesia?
qYES�� ������27.3%���� �����������19%������ ����P= 0.18
qNO���� ������72.7%��� ������������81%
QUESTION #5
Does your residency program offer clinically-related training modules (i.e. problem-based learning discussion) on perioperative management of the patient with HIV/AIDS undergoing surgery and/or anesthesia?
qYES ��������22.7%���������� �����19%����� �����P= 0.51
qNO���� ������77.3%� ��������������81%
QUESTION #6
Do you believe your residents would benefit from didactic lectures and clinical training modules pertaining to the perioperative management of patients with HIV/AIDS?
qYES�� ������72.1%����� ����������82.8%� ������P= 0.066
qNO����� �����27.9% ���������������27.2%
Table A: Hiv education survey for acgme anesthesiology & general surgery program director s.
Data are presented as numbers of respondents (n), and percentages (%) of responses for each question. Categorical data between the two groups of residents and program directors were analyzed using the χ2 test or Fisher’s exact test where appropriate. A P value of <0.05 was considered statistically significant.
Results
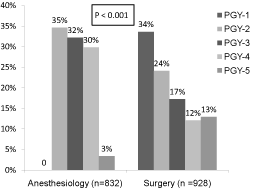
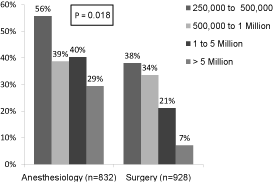
A total of 928 general surgery and 832 anesthesiology resident responses were collected; surveys were all fully completed. Figure 1 displays the distribution of the respondents in each year of residency training for each group; the distribution was significantly different (p=0.000) between the two groups. Figure 2 displays the distribution of the resident respondents based upon the size of the city where the residency program was located, and the distribution was significantly different (p=0.018) between the two groups.
Figure 1: Distribution of residents who responded to survey. PGY = Post-Graduate Year.
Figure 2: Size of city in which residency program is located.
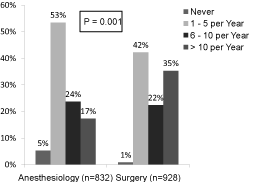
86% of anesthesiology and 87% of general surgery residents indicated that they had never received any formal education, didactic or clinical training in the perioperative management of patients with HIV/AIDS; there was no statistical difference between the two groups (p=0.739). Figure 3 illustrates the number of encounters with patients possessing HIV/AIDS by the two resident populations; there was a significant difference (p=0.001) between the two groups in their encounter rate.
Figure 3: How often do you manage the anesthetic/surgical care for patients with HIV/AIDS in one year?
From a basic knowledge perspective, 100% of both resident groups were able to accurately identify that being HIV positive does not imply a diagnosis of AIDS. In addition, both surgery (99.1%) and anesthesiology (97.1) residents correctly defined that a CD4+ count of < 200 cells/milliliter met AIDS-defining criteria. Both groups (surgery 78.5%, anesthesiology 83.2%) correctly answered that HAART usually consisting of three or more medications (no statistical difference). In addition, both surgery (92%) and anesthesiology (96%) had a majority of respondents that correctly identified a medication that was not a class of drugs utilized in HAART (p=0.27).
Two different questions assessed both resident populations in a similar manner but were unique to the nuances of the two different specialties. When asked about whether specific surgical contraindications existed in HIV/AIDS patients, a response of “yes” (40.7%) and “no” (59.3%) was noted by surgical residents. Anesthesiology residents were asked about potential HAART-general drug interactions with a response of “yes” (78.8%) and “no” (21.2%); there was statistical difference between the two groups (p=0.000) for the two questions. When asked about specific contraindications regarding insertion of foreign materials such as mesh or implants in HIV/AIDS patients, general surgery residents responded “yes”(22.2%) and “no”(77.8%), whereas when questioned about specific HAART drug-anesthetic drug interactions, anesthesiology residents responded “yes” (41.5%) and “no” (58.5%). The discordance was statistically significant between the two groups (p=0.003).
The two groups of residents answered divergently (Surgery – “yes” 49.6%, “no” 50.4%; Anesthesia – “yes” 26.9%, “no” 73.1%) when asked about whether obtaining detailed preoperative CD4+ count, viral load measurement and infectious disease consultation was necessary prior to undergoing surgery; this difference was statistically significant (p=0.001). In the first hypothetical clinical situation, 94.7% of anesthesiology residents and 88.9% of general surgery indicated they would proceed and not cancel surgery in a patient with HIV/AIDS not currently on HAART who did not show any clinical evidence of immune compromise. In the second clinical situation, 97.1% of anesthesiology residents and 91.5% of general surgery residents responded that they would not cancel or postpone an elective surgical case on the day of surgery in patients with AIDS on HAART but who did not exhibit any ongoing opportunistic infections. There was no statistical difference in the response rate between the two groups for both questions (p=0.148, p=0.186, respectively).When both groups of residents were asked if they were aware of any hospital or operating room procedures that minimized the risk of HIV transmission to health care workers (HCWs), 75.4% of general surgery residents and 80.8% of anesthesiology residents answered “yes” (p=0.240).
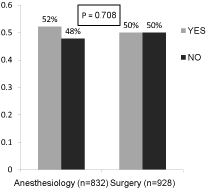
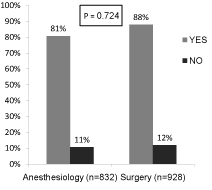
Figure 4 displays the response to whether or not residents believed they could adequately manage patients with HIV/AIDS (p=0.708). Figure 5 displays the responses from residents regarding if they believed they would benefit from more education regarding the pathogenesis of HIV, anti-viral treatment modalities and the surgical/ anesthetic management of the patient with HIV/AIDS (p=0.724).
Figure 4: Do you believe you have adequate training to manage the anesthetic/surgical care of a patient with HIV/AIDS?
Figure 5: Do you believe you would benefit from more education regarding the pathogenesis of HIV, anti-viral treatment modalities and anesthetic/surgical management of patients with HIV/AIDS?
71 surveys were completed by anesthesiology directors and 139 surveys by general surgery residency directors. Table A summarizes the responses by the residency program directors. There was no statistical difference between the responses by the two different groups of program directors.
Discussion
Although the apparent “visibility” of patients with HIV/AIDS in medical wards has almost vanished over the past fifteen years due to the effectiveness of HAART, HIV/AIDS is still a major public health concern. Approximately 1.3 million persons in the United States and over 34 million people worldwide are infected with HIV, and there is no sign of any decline in new rates of infection [9-11]. Improvements in HAART over the past fifteen years have greatly enhanced life expectancy in patients with HIV/AIDS, and the effectiveness of future HAART therapy is expected to continue to improve [6]. As a result of the continued advances in the therapeutic armamentarium against HIV and care by highly qualified medical specialists, surgeons and anesthesiologists in the perioperative arena are witnessing a surge of HIV+ patients presenting for surgical care similar to the general population. Since thirty years have passed since the initial onset of the HIV/AIDS epidemic, the authors believed it was important to assess if educational initiatives pertaining to HIV/AIDS during anesthesiology and general surgery residency training had kept pace with the continued evolution of treatment and management for HIV+ patients.
The survey that was conducted revealed a number of interesting demographic facets for the two study groups that were queried. From a level of training standpoint, the respondents did not possess a similar distribution in their level of training. Of note, the length of surgical training is longer (5 years) compared to the anesthesiology training period (3 years) and the authors did not survey post-graduate year-1 interns who would be entering anesthesiology residencies. The survey revealed that anesthesiology respondents tended to be located in larger cities (greater than 1 million) compared to their surgical counterparts; surgical resident respondents were from smaller cities (less than 1 million). One explanation for this phenomenon is that there are fewer anesthesiology residencies compared to general surgery residencies, and anesthesiology programs tend to be concentrated in larger cities. However, the inability to control the voluntary aspect of the survey may have led to differences in the demographic profile, and sampling bias may have inadvertently occurred.
With regard to the number of encounters with patients with HIV/AIDS, this study demonstrated that surgical residents manage a higher number of patients per year with HIV/AIDS compared to anesthesiologists. This may possibly occur because some patients with HIV/AIDS are treated for surgically-related issues (i.e. attended to by a surgeon) but may not necessarily require a procedure in the operating room. In addition, it is possible that conservative surgical non-operative management of patients with HIV/AIDS diminishes and/or eliminates the need for surgery. Therefore, anesthesiology residents encounter fewer patients with HIV/AIDS than their surgical counterparts.
With regard to whether or not HIV/AIDS educational modules were offered during anesthesiology and general surgery residencies, this study clearly revealed that the vast majority of anesthesiology and general surgery residents in the United States donot receive any formal didactic lectures or clinical training modules during their training. This result was equivalent between both specialties and persistent throughout all levels of training. To our knowledge, this finding has not been reported in the anesthesiology or general surgery educational literature. In addition, this was highly unexpected especially given that patients with HIV/AIDS now routinely undergo surgical care with few apparent barriers.
With regards to knowledge pertaining to policies and procedures utilized to minimize transmission of HIV (i.e. “universal precautions”), not all anesthesiology and general surgery residents were aware of this policy, however, there was no major difference between classes of residents. While a majority of residents did report exposure to this subject matter, one would presume that this issue would have been taught to all residents. Through the years, this policy has become standard practice for minimizing/preventing transmission of HIV from patient-to-patient, patient to health-care-worker and also from health-care-worker to patient [12]. Education and adherence to universal-precautions (UP) and blood-borne pathogen control policies are mandated by regulatory agencies and are considered a very basic tenet of infection control in the 21st century [13]. The deficiency in UP education may possibly be due to unstructured or informal learning modules when residents are introduced to the operative setting or possible oversight in assuming that this concept was taught at an earlier period during medical school surgical rotations. This knowledge gap has large public health implications since failure to adhere to UP may result in unnecessary workplace exposure to HIV, transmission of HIV, or exposure/transmission of other blood borne pathogens and infectious agents.
Although there was a lack of dedicated education in HIV/AIDS, this study demonstrates that both groups of residents were able to accurately define basic HIV/AIDS definitions and composition of HAART. While both groups of residents were able to fairly accurately identify classes of agents in HAART, surgical residents had a higher error rate. In straightforward clinical scenarios, both groups of residents answered questions correctly with a very small percentage in each group answering incorrectly. However, as clinical scenarios became more complex, the error rate increased in both groups, and difference in answers was noted between the two groups. Anesthesiology and general surgery residents were extremely divergent as to whether various preoperative laboratory studies and infectious disease pre-operative consultation was necessary. The lack of agreement may reflect the absence of prevailing guidelines or evidenced-based algorithms for the perioperative care of the HIV+ patient, however, it may also denote fundamental differences in the systematic process that patients with HIV/AIDS undergo when pre-surgical evaluations are conducted compared to pre-anesthetic assessments. Overall, both groups displayed knowledge deficits regarding complex questions regarding HIV/AIDS.
This study also demonstrated that while both anesthesiology and general surgery residents were almost evenly divided in whether or not they believe they have adequate training to manage the perioperative management HIV/AIDS, the majority of both groups of residents believed they would benefit from more training in the pathogenesis of HIV, HAART modalities and overall perioperative management of this patient population. This serves to emphasize that although residents are almost evenly split over whether they can adequately manage patients with HIV/AIDS, they admitted that education in this topic warrants further education. The survey completed by program directors corroborates that anesthesiology and general surgery resident do not complete formal educational training pertaining to HIV/AIDS. In addition, the directors acknowledge that they believe that further education related to HIV/AIDS is warranted during anesthesiology and surgical training.
The authors acknowledge that this study had several limitations. First, the study was not completed by all of the program directors or anesthesiology/general surgery residents in the United States. In addition, its distribution was dependent on the goodwill of program directors in forwarding it to their respective residents and their subsequent voluntary participation. Second, the survey questions were relatively straightforward and did not allow for subjective commentary. Third, limited assessment was made regarding complex clinical situations requiring detailed in-depth knowledge of HIV/ AIDS and was beyond the scope of this survey.
Despite the survey’s limitations, we believe this study dramatically demonstrates that educational modules during anesthesiology and general surgery residencies are not only warranted but absolutely necessary given the changing demographics and complex clinical continuum of patients with HIV/AIDS. The results of this survey have never before been demonstrated in the educational literature. The omission of educational modules relating to perioperative management of patients with HIV/AIDS may be related to the non-specific clinical goals outlined in the ACGME anesthesiology and surgical residency training educational curricula [14, 15]. Anesthesiology programs must have a wide spectrum of disease processes and surgical procedures available within the program so that each resident is provided with a broad exposure to different types of anesthetic management within the anesthesiology sector [14]. In both anesthesiology and surgical programs, residents must demonstrate knowledge of established and evolving biomedical, clinical, epidemiological and social behavioral sciences, as well as the application of this knowledge to patient care [14,15]. However, the broad curricular requirements make no specific mention of HIV/AIDS education as a distinct topic, and the specific coverage of HIV/AIDS as subject matter during anesthesiology and residency training is not explicitly mandated. Because educational principles are organized along patient care requirements in which residents will be exposed to a wide array of clinical cases with a variety of illnesses, the lack of educational modules or clinical training in HIV/AIDS may be more of a de facto oversight.
Regardless, of the mechanism for omission of HIV/AIDS training, this is a major deficiency in the educational curricula for perioperative physicians since surgeons and anesthesiologists routinely encounter this patient population regardless of location of training (smaller city versus larger metropolitan area).While extensive evidenced-based clinical algorithms surrounding the perioperative care of patients with HIV/AIDS are scarce, residents can nonetheless receive extensive didactic and clinical training in this area so that rational consideration to complex issues pertaining to HIV/AIDS can be addressed.
The utilization of multi-disciplinary modalities may prove effective in simultaneously addressing education of both anesthesiology and general surgery residents [16, 17]. Collaboration between surgical and anesthesiology programs is paramount as these two sectors repeatedly interact and non-aligned approaches may lead to management disputes or collisions between the two specialties when the patient with HIV/AIDS finally becomes a candidate for surgery. The authors acknowledge that this task may prove difficult in light of the time constraints imposed by current resident “work-hour” restrictions superimposed on the ever burgeoning expansion of the pharmacologic armamentarium coupled with technological advances in the perioperative arena. As the HIV/AIDS pandemic now enters its fourth decade and shows no signs of abating, the authors believe the worldwide impact of this disease warrants increased educational efforts targeting physicians in the perioperative sector.
Author Contributions
AHC, RW, JP, JT contributed towards study design, conduct of study, data collection and manuscript preparation. AHC, TL, JT, JG and JP contributed towards reference review, data analysis and manuscript preparation.
References
- Gottlieb MS, Schtoff R, Schanker HM, Weisman JD, Fan PT, Saxon A, et al. Pneumocystis carinii pneumonia and mucosal candidiasis in previously healthy homosexual men: evidence of a new acquired cellular immunodeficiency NEJM. 1981; 305: 1425-1431.
- Centers for Disease Control and Prevention. Pneumocystis pneumonia - Los Angeles. MMWR Morb Mort Wkly Report. 1981; 30: 250-252.
- Fauci AS. The Human Immunodeficiency Virus: infectivity and mechanisms of pathogenesis. Science. 1988; 239: 617-622.
- Fauci AS. The AIDS epidemic, considerations for the 21st century. NEJM. 1999; 341: 1046-1050.
- Carpenter CCJ, Cooper DA, Fischl MA, Gatell JM, Gazzard BG, Hammer SM, et al. Antiretroviral therapy in adults, updated recommendations of the International AIDS Society. JAMA. 2000; 283: 381-390.
- Pallella FJ, Delaney KM, Morrman AC, Loveless MO, Fuhrer J, Satten GA, et. al. Declining morbidity and mortality among patients with advanced human immunodeficiency virus infection. NEJM. 1998; 338: 853-860.
- Farizo KM, Buehler JW, Chamberland ME, White BM, Froelicher ES, Hopkins SG, et al. Spectrum of disease in persons with Human Immunodeficiency Virus infection in the United States. JAMA. 1992; 267: 1798-1805.
- Horberg MA, Hurley LB, Klein DB, Follansbee SE, Queensberry C, Flamm JA, et al. Surgical outcomes in Human Immunodeficiency Virus-infected patients in the era of highly active antiretroviral therapy. Arch Surg. 2006; 141: 1238-1245.
- HIV Surveillance Report: Diagnoses of HIV infection and AIDS in the United States and dependent areas. In. Edited by Control CfD; 2009.
- Implementation of the Declaration of Commitment on HIV/AIDS and the Political Declaration on HIV/AIDS. In. United Nations Sixty-fifth session, Agenda item 10. Presented at 2011 High Level Meeting on AIDS.
- Hall HI, Song R, Rhodes P, Prejean J, An Q, Lee LM, et al. Estimation of HIV incidence in the United States. JAMA. 2008; 300: 520-529.
- Siegel JD, Rhinehart E, Jackson M, Chiarello L, Committee HICPA. 2007 Guideline for Isolation Precautions: Preventing Transmission of Infectious Agents in Healthcare Settings. 2007.
- Joint Commission Resources. Comprehensive Accreditation Manual for Hospitals: The Official Handbook (CAMH). In; 2011.
- Accreditation Council for Graduate Medical Education. Program Requirements for Graduate Medical Education in Anesthesiology. In. https://www.acgme.org/acWebsite/downloads/RRC_progReq/040_anesthesiology_07012008_u03102008.pdf; 2011.
- Accreditation Council for Graduate Medical Education. Program Requirements for Graduate Medical Education in Surgery. In. https://www.acgme.org/acWebsite/downloads/RRC_progReq/440_general_surgery_01012008_u08102008.pdf.
- Bowen JL. Adapting residency training. Training adaptable residents. West J Med. 1998; 168: 371-377
- Riviello R, Ozgediz D, Hsia RY, Azzie G, Newton M, Tarpley J. Role of collaborative academic partnerships in surgical training, education, and provision. World J Surg. 2010; 34: 459-465.