
Case Series
Austin J HIV/AIDS Res. 2016; 3(1): 1018.
Non-Aids Associated Kaposi Sarcoma amongst 4 Patients in Cameroon (Central Africa)
Enow Orock GE¹*, Weledji EP², Meli J³, Fewou A4, Ndom P5 and Doh AS5
¹Faculty of Health Science, University of Buea, Regional Hospital Buea, Buea, Cameroon
²Faculty of Health Science, University of Buea, Buea, Cameroon
³Infectious disease Unit, General Hospital Yaounde, Yaounde, Cameroon
4Faculty of Medicine and Biomedical Science, University of Yaounde I, Yaounde, Cameroon
5National Cancer Control Committee, Yaounde, Cameroon
*Corresponding author: Enow Orock GE, Faculty of Health Science, University of Buea, Regional Hospital Buea, Buea, Cameroon
Received: December 24, 2015; Accepted: January 07, 2016; Published: January 11, 2016
Abstract
Background: Kaposi sarcoma is very strongly associated with HIV infection. The disease is rare in HIV negative patients and has distinct clinical and prognostic attributes from AIDS associated counterpart. The group at risk to develop non-AIDS related KS in our community are elderly men, although both sexes and children are not immune to the disease.
Patients and Methods: In order to define risk-groups and major clinical features we retrospectively evaluated clinical data of all patients with non-AIDS associated KS in the Yaounde population in Cameroon, Central Africa, between 2004 and 2014, a period of 10 years. Data were extracted from the Yaounde Cancer Registry and from patient records for the period under study.
Results: 4 patients were identified with non-AIDS Kaposi sarcoma in a ten years study period giving an incidence of 2.5 in this community. The average age at onset of the disease was 42 years. The patients ranged in age from 6-64 years and included 3 (75%) males and 1 (25%) female with a male-to-femaleratio of 3:1. The tumour was located in the skin (50%), cervical lymph nodes (25%) and viscera (25%). 3 patients had a localized disease at time of diagnosis against 1 with a metastatic disease. This later died of his disease 2 years after diagnosis, while 2 others were doing well after treatment and 1 was lost to follow up. 2(50%) of the KS clinical subtypes were classified to be of the African endemic type, while1 (25%) was classic and the other (25%) was unclassified.
Conclusion: Kaposi sarcoma does occur in HIV negative patients. Unlike KS in AIDS patients, non-AIDS associated Kaposi sarcoma is a localized disease which mostly involves the skin of the lower limb, common in elderly otherwise healthy men but also in women and children and responds well to treatment. Kaposi sarcoma should be actively ruled out in clinical, biological and pathologic investigations of all patients including HIV sero negative patients.
Keywords: Non-AIDS; Kaposi sarcoma; Cameroon
Introduction
Kaposi Sarcoma (KS) is prevalent worldwide [1,2]. It is caused by the human herpes virus 8 (HHV-8) or Kaposi’s Sarcoma-Associated Herpes Virus (KSHV). Since Moritz Kaposi [3] first described this malignant neoplasm, the disease has been reported in five separate clinical settings, with different presentations, epidemiology, and prognosis [4]. It occurs in various forms which include AIDSassociated KS, classic KS, African endemic KS, Mediterranean KS, iatrogenic KS, and KS in homosexual men without HIV infection [5]. The debate has always been to identify the etiopathological involvement of this herpes virus in the pathogenesis of Kaposi’s sarcoma, rather than as a contamination of yet another opportunistic virus in immune suppressed AIDS patients [6]. In spite of its strong association with the HIV/AIDS, KS does occur in HIV negative patients.
Case Series
Case 1
A 42 years old heterosexual male technician, secondary school graduate, presented with a lesion in the skin of the lower right limp below the knee of 6 months duration. Hard lymph nodes were found in the ipsilateral groin. He had not been on any medication for prolonged treatment of any disease. Biopsy and histology of the lesions reported a Kaposi sarcoma. He was seronegative to HIV tests. A diagnosis of Kaposi sarcoma with regional lymph node metastasis was made. The patient was referred for further management in the oncology department. He died two years after.
Case 2
A 64 years old heterosexual male was seen with cervical lymphadenopathy of unknown duration. A biopsy and histology of the lymph nodes revealed a KS. There was no history of prolonged treatment for any disease. The patient tested negative to HIV.
Case 3
A biopsy was done on a 6 years old female patient from an unspecified thoracic soft tissue tumor. The parents were both seronegative to HIV and had no lesion diagnosed as KS. The child had not been in close contact with a KS patient. The antenatal and obstetric history was uneventful. Clinically the child presented with cough and weight loss. A CT scan found an anterior mediastinal mass that was biopsied. Histology of the tumor biopsied reported a KS in this patient who was seronegative to HIV.
Case 4
A 55 years old heterosexual university graduate and businessman consulted for a skin “patch” on the left second toe that had increased in size and bleed twice in recent months. No other associated symptoms were found. Numerous tests for HIV serology were negative. He received several sessions of chemotherapy for KS that was diagnosed histologically on a biopsy of the specimen. He is alive and well 5 years after treatment without recurrence.
Results and Discussions
Cancer has been found to be a public health problem in Cameroon [7] with KS representing about 6.9% of the national cancer burden [8]. In an earlier study, KS was reported to be the commonest AIDSassociated malignancy in the country, and occurred among 30.6% of HIV/AIDS patients [8].
The disease is a previously rare, tumour-like lesion of controversial biological nature. It has since the early 1980s become frequent in patients with AIDS, particularly in homosexuals. It is endemic in Central Africa predominantly in otherwise healthy men but also in women and children [6,9]. The tumour which is strongly associated with the Human Immunodeficiency Virus infection is the predominant AIDS-defining tumour in our community (50.4% of ADCs) [10] and elsewhere [11]. In spite of this strong etiological association of KS with AIDS, many cases of non-AIDS KS have been reported [12].
Endemic KS, which has two types, African cutaneous Kaposi sarcoma and African lymphadenopathic Kaposi sarcoma was described in young African people, mainly from sub-Saharan Africa. It is a more aggressive disease that infiltrates the skin extensively, especially on the lower limbs. This type is not related to HIV infection. Like KS in AIDS, the skin is the commonest site for non- AIDS associated KS.
Kaposi sarcoma is rare and associated with HHV-8 infection, but not exclusive to HIV/AIDS patients [13]. The first non-AIDS associated cases in were reported as far back as 1872 as a form of the cancer in older people of eastern Mediterranean origin [14].
Of a total of 463 patients diagnosed with KS in a ten years period (2004-2014) in this study, 4 patients were seronegative to HIV. This gave a non- AIDS: AIDS- associated Kaposi sarcoma ratio of 1:116. The mean age at diagnosis of the group was 42 years. The youngest patient was 6 years old, while the oldest developed his disease by the age of 64. These findings are similar to those reported by Lena-Jacobs [12]. The tumour we found was histologically similar to what has been reported on literature (Figure 5).
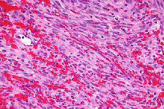
Figure 5: Micrograph of a Kaposi sarcoma showing the characteristic.
Spindle cells, high vascularity and intracellular hyaline globs. H&E stain.
KS occurs in this community in near equal proportions between males (49.6%) and females (50.4%) [14]. On the other hand, a male predominance has always been reported in non-AIDS associated KS [12]. Similarly, we found 75% male patients (n = 3) versus 25% female patients (n = 1) with a male/female ratio of 3:1 in our study (Figure 2). Our findings are also similar to [12] reporting on a study of 20 non-AIDS KS. But also differ from Lena who found a predominance of classic (15/20) and iatrogenic (5/20) subtypes of KS in his study on a population. All our patients (100%) were local ethnic indigenes of this black sub Saharan Central African community. Nkegoum [9] had found 60 cases of children with Kaposi sarcoma in Cameroon in a 23 years retrospective study.
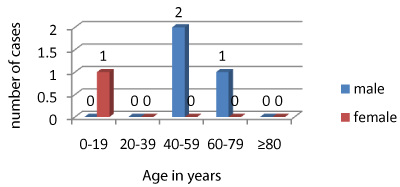
Figure 2: Distribution of patients by age and by sex. The mean age is 42
years, while female patients are teenagers and males are elderly.
Previous reports [12] have shown that unlike KS in AIDS patients, non-AIDS associated KS is a rather localized process which rarely involves lymph nodes or organs. In our study we found a 25% lymph node location and 25% metastasis at diagnosis (Figure 1).
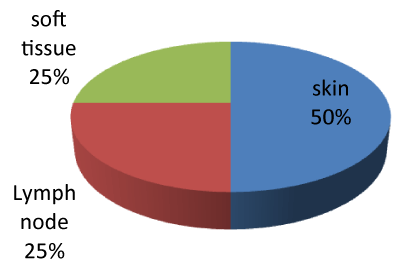
Figure 1: Site of non-AIDS KS amongst patients. The skin is predominant site
for non-AIDS associated KS.
Regarding the clinical Subtype 50% of our cases were African endemic subtype while 25% were classic and 25% unclassified (Figure 4), unlike Lena [12] who found 15/20 cases of classic KS and 5/20 cases of iatrogenic KS in his study.
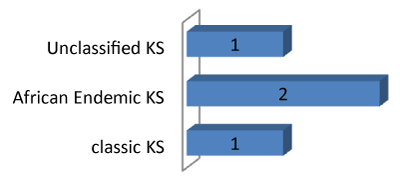
Figure 4: Bar chart showing clinical subtypes of non-AIDS associated KS.
African endemic type (50%) is commonest NAA-KS in this community.
Be it AIDS associated or non-AIDS associated, KS has been reported by previous works to be of good prognosis [12]. In this study only 1 patient (25%) was confirmed dead after treatment. This patient was diagnosed at advanced stage of disease with regional lymph node metastasis (Figure 3).
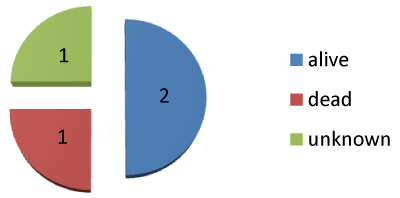
Figure 3: Disease outcome in patients with non-AIDS KS. 50% 5 years
survival rate for NAA-KS after treatment.
Conclusion
KS does occur in HIV negative patients. Unlike KS in AIDS patients, non-AIDS associated KS is a localized disease which mostly involves the skin of the lower limb, common in elderly otherwise healthy men but also in women and children, and responds well to treatment. KS should be actively ruled out in clinical, biological and pathologic investigations of all patients including HIV seronegative patients.
References
- Cook-Mozaffari P, Newton R, Beral V, Burkitt DP. The geographical distribution of Kaposi sarcoma and of lymphomas in Africa before the AIDS epidemic. Br. J. Cancer 1998; 78: 1521–1528.
- Olsen SJ, Chang Y, Moore PS, Biggar RJ, Melbye M. Increasing Kaposi sarcoma-associated herpesvirus seroprevalence with age in a highly Kaposi sarcoma endemic region, Zambia in 1985. AIDS; 1998 12(14): 1921–1925.
- Kaposi M. Idiopathisches multiples Pigmentsarkom der Haut. Arch. Dermatol. Syph. 2007; 4: 181-187.
- Memar OM, Rady PL, Tyring SK. Human herpesvirus-8: detection of novel herpesvirus-like DNA sequences in Kaposi's sarcoma and other lesions.JMol Med (Berl). 1995; 73: 603-609.
- Schalling M, Ekman M, Kaaya EE, Linde A, Biberfeld P. A role for a new herpes virus (KSHV) in different forms of Kaposi's sarcoma.Nat Med 1995; 1: 707-708.
- Doh AS, Ndom P, EnowOrock GE, et al. Cancer in Cameroon. A practical guide. Nat. Can. Cont. Comm. 2007; 1: 12-18.
- EnowOrock GE. Cancer Incidence and Trends in Yaounde, Cameroon edsDoh AS, Ndom P. Lam. Acad. Pub.2012; 66-69.
- Nkegoum B. Kaposi's sarcoma in children in Cameroon before and during the HIV epidemic 2014 NCRI Cancer Conference, The BT Convention Centre Liverpool UK 2 - 5 November 2014 .
- EnowOrock G, Agyingi L, Nnap L, Ewane TP, Ngai J, Fewou A, et al., From Hiv/Aids to Hiv Cancer: An Analysis of Transition from Hiv Infection to Cancer amongst Patients in Cameroon.Int JHIV/AIDS Prev, Educ and Beh Sc. 2015; 1: 14-20.
- Akarolo-Anthony SN, Dal Maso L, Igbinoba F, Mbulaiteye SM, Adebamowo CA. Cancer burden among HIV-positive persons in Nigeria: preliminary findings from the Nigerian AIDS-cancer match study. Infect Agents and Cancer 2014; 9:1.
- Lena J, Gisela M, Ko-Ming C, Claus G. Non-AIDS Associated Kaposi's Sarcoma: Clinical Features and Treatment Outcome .PLoS One. 2011; 6: 183-197.
- Iman S, Abdalla A, Alaa M, Rehab S, Ola B, Emad Eid. Isolated Kaposi Sarcoma in two HIV negative patients. J. Dermatol. CaseRep. 2011; 5: 24–26.
- Gönen M, Cenker A, Kiyici H, Kalkan M. Penile Kaposi's sarcomas in a circumcised and HIV-seronegative patient. Int. J.Urol 2006; 13: 318–320.
- EnowOrock GE, Verla VS, Ashuntantang GE, Ndom P, and Doh AS. Kaposi Sarcoma: A review of 387 cases seen in Yaounde, Cameroon. Glob Adv Res J of Med and Med sc. 2013; 2: 193-198.