
Case Report
Austin J Med Oncol. 2019; 6(1): 1044.
Skin Metastases from Ovarian Carcinoma
Hélène C1, Dorothée C1, Benjamin L1, Edouard G2, Claude EK1 and Alain L1*
¹Centre Catherine de Sienne, Hopital Privé du Confluent, 2 rue E Tabarly, 44202 NANTES, France
²Clinique Jules Verne, Route de Paris, 44000 NANTES, France
*Corresponding author: Alain Lortholary, Centre Catherine de Sienne, Hopital Privé du Confluent, 2 rue E Tabarly, 44202 NANTES, France
Received: June 12, 2019; Accepted: July 10, 2019; Published: July 17, 2019
Abstract
Skin metastases from malignant ovarian carcinoma are very uncommon. These ovarian cutaneous metastases must be classified as umbilical metastases (Sister Joseph nodule) and nonumbilical metastases. Skin lesions at abdominal incision scars or at paracentesis site are to be considered as a propagation malignant tumor cells and not as metastases.
We reported a 62-year-old woman with large skin metastases from highgrade serous papillary adenocarcinoma of the ovary, initially diagnosed as a low-grade carcinoma.
This case is uncommon with large skin metastases and transformation of a low grade to a high-grade ovarian carcinoma.
Keywords: Skin metastases; Ovarian cancer; Non umbilical nodule
Introduction
Skin metastases from ovarian carcinoma is a rare entity. About 3% of patients with malignant ovarian carcinoma are reported to have cutaneous metastases. Moreover, most of these cases reported have a sister Joseph’s syndrome (periumbilical nodules).
We report a case of a 62 years old woman with large cutaneous metastases from ovarian cancer that occur one year after the first line chemotherapy.
Case Presentation
A 61 years old woman presented with large inguinal node which was present one year before. She finally decide to consult a gynecologist in February 2017. This inguinal node was measured at 6 cm.
The scanner showed the voluminous inguinal node and voluminous ovarian tumors. Serum Ca 12.5 was 170 U/ml
A coelioscopy was done in March 2017 with salpingooophorectomy, peritoneal cytology, ablation of the umbilical nodule and biopsy of the inguinal node. Histology was reported as a serous papillary low-grade adenocarcinoma of the ovary stage IVB. She received 6 cycles of chemotherapy: paclitaxel and carboplatin with a partial response. Then she had optimal cytoreductive surgery in October 2017: hysterectomy, appendicectomy, omentectomy, inguinal and lombo-aortic lymph node dissection. It remains on histology the same low-grade ovary adenocarcinoma on all the lymph nodes resected.
In December 2018 the right inguinal lymph node reappeared with also large abdominal cutaneous lesions (Figure 1). These inflammatory skin lesions appeared rapidly. Histology was reported at this time as a high-grade sero papillary adenocarcinoma on the lymph node and the skin lesions. The computed tomography showed no other lesions than inguinal lymph nodes and cutaneous lesions. A new chemotherapy and a testing BRCA mutation are programmed.
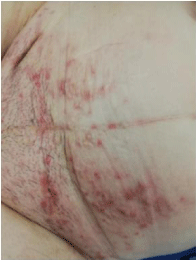
Figure 1: Diffuse skin metastases: high grade sero papillary adenocarcinoma.
Discussion
Skin metastases is a rare event in ovarian cancer ranged from 0.9% to 4% [1-3]. Mostly cutaneous metastases happened in breast cancer, lung cancer and kidney cancer [1-4]. In ovarian cancer, Otsukrand et al. [1] proposed a classification as umbilical metastases (Sister Joseph nodule) and nonumbilical metastases. They excluded skin metastases at abdominal incision scars or at paracentesis site. These last patients have a better prognosis [1]. The median survival of the others has been shown is poor: 4 months [5]. This median survival could be today much better with platin taxane chemotherapy and bevacizumab [1-6]. Sometimes when the skin lesions are small and isolated radiotherapy has been described as an option [7]. Our patient has developed non umbilical diffuse skin metastases. Nevertheless one year before she had umbilical nodule without umbilical symptoms. Skin ovarian metastases generally indicated a poor prognosis. In our patient, the long interval between the last chemotherapy and the cutaneous involvement seems to be a better prognostic factor. Some patients responded well to the palliative treatment [6]. This case is uncommon with large skin metastases and transformation of a low grade to a high grade ovarian carcinoma.
References
- Otsuka I, Matsuura T. Skin metastases in epithelial ovarian and fallopian tube carcinoma. Medecine. 2017; 96: 1-8.
- Dauplat J, Hacker N, Nieberg R, Berek J, Rose T, Sagae S. Distant metastases in epithelial ovarian carcinoma. Cancer. 1987; 60: 1561-1566.
- McDonald H, Moore M, Meffert J. Cutaneous metastases from adenocarcinoma of the ovary. JAAD case report. 2016; 2: 406-407.
- Brownstein M, Helwig E. Metastatic tumors of the skin. Cancer. 1972; 29: 1298-1307.
- Cormio G, Capotorto M, Di Vagno G, Cazolla A, et al. Skin metastases in ovarian carcinoma: a report of nine cases and a review of the literature. Gynecol Oncol. 2003; 90: 682-685.
- Karpate S, Samal S, Jain S. Recurrent ovarian malignancy presenting as cutaneous metastasis. Indian J Dermatol. 2009; 54: 3880-3381.
- Wiechert A,Garett l, Lin G, Goodman A. Management of a skin metastasis in a patient with advanced ovarian cancer. Gynecol Oncol Rep. 2012; 2: 124- 126.