
Research Article
Austin Med Sci. 2016; 1(2): 1009.
Quality of Life of Adults Participating in a Rehabilitation Program Following a Stroke
de Oliveira MR¹* and D’Oliveira A Jr²
¹Hospital SARAH Brasília, School of Medicine, Federal University of Bahia, Brazil
²Department of Medicine of Bahia - Federal University of Bahia, Brazil
*Corresponding author: Marcos Roberto de Oliveira, Neurological Rehabilitation Sector SARAH Network of Rehabilitation Hospitals - Hospital SARAH Brasília, DF, Brazil
Received: June 22, 2016; Accepted: August 29, 2016; Published: September 02, 2016
Abstract
Objective: To evaluate the self-perceived Health-Related Quality of Life (HRQoL) of adults participating in a rehabilitation program following Stroke.
Methods: Conducted quasi-experimental study, no control group, evaluated the quality of life of patients after CVA at admission and at the discharge of a rehabilitation program, using the following instruments: the Stroke Impact Scale (SIS), the Functional Independence Measure, the modified Rankin Scale, the Geriatric Depression Scale, the Hospital Anxiety and the Depression Scale (HADS), and a sociodemographic questionnaire.
Results: Twenty-five patients were evaluated, 11 men and 14 women. Their mean age was 48 years and the mean time of the lesion was 17.2 months. After the program, increases were found in physical performance, functional performance and in all the domains of the SIS except for the communication domain.
Conclusion: The patient participation in the rehabilitation program, suggests gains in physical and functional performance and in the individual’s perceptions of HRQoL following Stroke.
Keywords: Health-related quality of life; Stroke; Rehabilitation; Disability
Introduction
Stroke is defined by the World Health Organization (WHO) as “rapidly developing clinical signs of focal disturbance of cerebral function, with symptoms lasting 24 hours or longer”. It is the second cause of death worldwide and the leading cause of acquired disability in adults [1]. The overall incidence of Stroke in the
Latin American and Caribbean populations is 140 per 100,000 inhabitants [2]. Disabilities include impaired motor function, limitations in Activities of Daily Living (ADL), possible cognitive impairment and language disorders, depression and restrictions to social interaction, consequently affecting an individual perception of their quality of life [3].
Health-Related Quality of Life (HRQoL) is defined as the qualitative value attributed to the period of life that follows changes caused by lesions, according to functional states, perceptions, and social opportunities that are affected by disease, injury, treatment or public actions [4]. In addition to the physical, mental, and social aspects, there are new considerations relating to personal perceptions, personal beliefs, religiousness, and spirituality that need to be incorporated into the health-related concept [3,5]. This statement defines Health-Related Quality of Life (HRQoL) as a construct that focusses on the respondent’s subjective perception and consists of physical, mental, and social dimensions [6].
Studies have demonstrated improvements in physical and functional performance and in states of depression and anxiety following participation in rehabilitation programs. However, it is unsure whether these gains are maintained over time [7]. There is evidence that social support, realistic expectations, education, appropriate guidance to reduce the burden of patients’ caregivers in the months following Stroke increase the success of a rehabilitation program [8,9].
Therefore, the objective of the present study was to identify the factors that affect self-perceived HRQoL following a CVA in patients participating in a neurological rehabilitation program in a public rehabilitation hospital, and to evaluate possible sociodemographic, clinical and functional variables that could be predictive of the therapeutic responses.
Methods design
Quasi-experimental study, no control group, was conducted to evaluate self-perceived HRQoL in patients participating in a public neurological rehabilitation program following a CVA. The study was conducted at the SARAH Rehabilitation Hospital in the city of Salvador, Bahia, Brazil. A convenience sample was obtained of consecutive patients admitted to the rehabilitation program between March and October 2012 who met the study inclusion criteria. A total of 64 patients with sequelae following Stroke were admitted to the rehabilitation program and, of these, 25 fulfilled the inclusion criteria and agreed to participate in the study.
Participants
The inclusion criteria consisted of: a diagnosis of ischemic or hemorrhagic Stroke, confirmed by clinical evaluation and radiological findings on computed tomography and/or magnetic resonance imaging, and being at least 16 years of age.
Patients with any other associated neurological diseases or concomitant severe systemic diseases (uncontrolled hypertension, severe cardiomyopathies, coronary disease, heart arrhythmias and uncontrolled diabetes) were excluded, as well as patients with moderate to severe cognitive deficits as measured according to the Mini-Mental State Examination (MMSE) and those with moderate to severe aphasia or behavioral abnormalities.
The study was approved by the ethical review board of the SARAH network of rehabilitation hospitals, and all the participants provided written consent.
HRQoL was correlated with the patient’s clinical, functional and psychosocial status at two different time points: at admission to the rehabilitation program and at discharge from the hospital (after 4-6 weeks in hospital).
Outcome measures
HRQoL was measured using the Stroke Impact Scale (SIS), version 3.0 9. This scale consists of 8 domains (strength, hand function, mobility, activities of daily living -ADL and Instrumental Activities of Daily Living [IADL], memory and thinking, communication, emotion and participation/role function). The scores for each domain range from 0 to 100, with higher scores reflecting better HRQoL. The SIS also contains a question that independently measures the patient’s overall perception with respect to his/her recovery following the CVA, with scores ranging from 0 (no recovery) to 100 (full recovery). Each domain consists of 4-11 questions graded from 5 to 1 in accordance with the degree of difficulty, time spent and the amount of strength used. Functional data were obtained using the motor portion of the Functional Independence Measure (FIM) scale, version 4.0, consisting of items in which physical functions are evaluated. This instrument takes into consideration the individual status at that specific moment, with a maximum total score of 91 points [10,11]. For each item, the individual’s degree of independence in performing a certain task is graded, resulting in a score that ranges from 1 (completely dependent) to 7 (completely independent). Higher total scores reflect a greater degree of independence. The modified Rankin Scale (mRS), which measures patients’ overall functional independence, was also applied. This scale classifies results into 7 different graded categories: 0 (no symptoms at all), 1 (no significant disability despite symptoms), 2 (slight disability); 3 (moderate disability); 4 (moderately severe disability); 5 (severe disability) and 6 (dead). Higher scores reflect greater disability.
The presence of depression was investigated using the Hospital Anxiety and Depression Scale (HADS). In this study, only the 7-item depression section was used (HADS-D), with each item scoring from 0 to 3 according to the severity of symptoms. Scores ≥ 9 indicate the presence of depression. In elderl y patients (those over 65 years of age), the 15-item Geriatric Depression Scale (short form) (GDS-15) was used, with scores ≥ 6 being associated with depression.
The sociodemographic data collected consisted of sex, age, marital status, socioeconomic condition (mean monthly income and socioeconomic class), schooling and employment status.
The clinical data collected referred to the type of CVA (ischemic or hemorrhagic), the side of the brain affected and the time of lesion (acute/subacute ≤ 6 months or chronic > 6 months). All data were collected from electronic patient charts.
Statistical analyses
The data were treated descriptively and inferentially after having been stored in an Excel® 2003 database and analyzed using the R software program, version 2.15.2. A descriptive analysis was performed to identify the general and specific characteristics of the study sample, with results being expressed as absolute/relative frequencies, means, standard deviations, and medians. The Shapiro-Wilk test was used to test the normality of the data distribution. To compare means prior to and following the intervention, Student’s t-test or the Wilcoxon non-parametric test was used for paired samples. Significance level was defined at 5% throughout analysis.
Results
The sociodemographic characteristics of the participants and their comorbidities are shown in (Table 1). The study sample consisted of 14 women (56%) and 11 men (44%), with ages that ranged from 18 to 73 years (48.0 ± 15.2 years, mean ± standard deviation). Time since Stroke ranged from 2 to 60 months (mean 17.2 months), with 7 patients in the acute/subacute phase (28%) and 18 in the chronic phase (72%). Nineteen patients had hemiparesis on the left side (76%) and 6 on the right side (24%). All were able to walk, either alone or with support.
Variable
Value
Mean age: years ± standard deviation (Min-Max)
48.0 ± 5.2 (18-73)
Time since CVA; frequency (%)
Acute/sub-acute
7 (28)
Chronic
18 (72)
Sex; frequency (%)
Female
14 (56)
Male
11 (44)
laterality; frequency (%)
Right hemiparesis
6 (24)
Left hemiparesis
19 (76)
Ischemic CVA; frequency (%)
Atherosckrosis of large arteries
3 (12)
Cardioembolic
2 (8)
Lacunar
8 (32)
Other determined etiologies
0
Other undetermined etiologies
0
Hemorrhagic CVA; frequency (%)
Intraccerebral
10(40)
Subarachnoid
2(8)
Comorbidities: frequency (%)
Hypertension
17 (68)
Diabetes
5 (20)
Dyslipidemia
15 (60)
Other causes
17 (68)
Education; mean number of years of schooling (range)
7.6 (1-13)
Socioeconomic condition; frequency (%)
Employed
1 (4)
Sickness benefit
10 (40)
Retirement pension
12 (48)
No benefit
2 (8)
Socioeconomic class; frequency (%)
A1
0
A2
2 (8)
B1
0
B2
2 (8)
C1
12 (48)
C2
6 (24)
D
3 (12)
E
0
Marital status; frequency (%)
Married
16 (64)
Unmarried*
9 (36)
*Unmarried: This group consists of single, widowed or divorced individuals
Table 1: Sociodemographic data and comorbidities (n=25).
The mean number of years of schooling was 7.6 years (range 1-13 years). Most of the patients were married (64%) and the predominant socioeconomic class was C1 (48%). Mean gross family income was $715,20. With respect to socioeconomic conditions, only one patient (4%) was still employed, while 48% were retired and 40% were receiving sickness benefit from the federal government.
Thirteen patients had ischemic stroke (52%), while twelve (48%) had hemorrhagic stroke. The most common type of ischemic stroke was a lacunar stroke (n=8; 32%). The risk factors most associated with the cases of Stroke were hypertension (68%) and dyslipidemia (60%), either concomitantly or individually. Of the other risk factors found (68%), the most common were those associated with cardiovascular alterations.
Regarding the mood and cognitive status, 9 patients (36%) had depression. The mean MMSE score was 27.6 ± 1.81.
The mean duration of hospitalization was 36.7 ± 9.5 days (range 17-50 days). The admission and discharge data were statistically different compared to the gain measurement of the functional status measured using the modified Rankin Scale and the FIM scale (Z = -4.38; P<0.001; Z = -4.28; P<0.001, respectively) (Table 2).
Admission
Discharge
P-value
Modified Rankin scale;
mean (range )3 (1-4)
1 (0-4)
P < 0.001
FIM scale*;
mean / median (± standard deviation)72.8 / 77.0
(±14.1)83.3 / 88.0
(±11.9)P < 0.001
*Functional Independence Measure- motor portion only, with maximum total score of 91.
Table 2: Functional data (n=25).
The data of HRQOL were also statistically significant and different for the gain in the perception of HRQOL in the hospital for all the domains of SIS, except for the communication domain (P = 0.08) (Table 3). The HRQoL domains found to be most affected at admission, with mean scores ≤ 50, were: strength (47.7 ± 20.56), hand function (31.6 ± 28.12) and participation (46.0 ± 22.3) (Figure 1).
Domains
Number of Items
Admission
Discharge
Significance
Mean* SD (95%CI)
Mean * SD (95°AC1)
Strength
4
47.7 ± 20.5 (39.2-56.2)
63.4± 19.1 (55.5-71.3)
P<0.001
Memory and thinking
8
80.9 ± 17.8 (73.5-88.2)
86.6 ± 9.6 (82.7-90.6)
P<0.05
Emotion
9
68.7 ± 14.1 (62.9-74.6)
78.8 ± 11.2 (74.243.4)
P<0.05
Communication*
7
87.4 ± 11.1 (82.7-92.0)
90.1 ± 9.5 (86.2-94.1)
P<0.081*
ADL/IADL**
12
67.3 ± 15.5 (60.9-73.7)
79.9 ± 11.7 (75.144.8)
P<0.001
Mobility
10
72.6 ± 15.2 (66.3-78.9)
82.4 ± 9.9 (78.346.6)
P<0.05
Hand function
5
31.6 ± 28.1 (19.943.2)
49.8 ± 29.8 (37.4-62.1)
P<0.001
Participation
9
46.0 ± 22.3 (36.8-55.3)
63.0 ± 20.1(54.7-71.3)
P<0.001
Recovery Index (RI)
55.2 ± 22.3 (45.9-64.4)
73.2 ± 14.9 (67.0-79.3)
P<0.05
*Domain for which the difference was not statistically significant
**ADL (activities of daily living) and IADL (instrumental activities of daily living)
SD: standard deviation; 95%CI: 95% Confidence Interval; SIS: Stroke Impact Scale
Table 3: SIS evaluation scores at admission to and at discharge from the rehabilitation program.
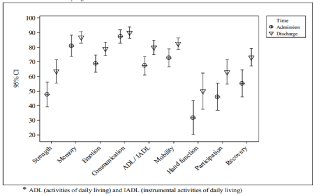
Figure 1: and 95% CI scores for each domain of stroke impact scale at
admission and discharge from the rehabilitation program.
No statistically significant differences were found between marital status (married or unmarried), the type of Stroke (ischemic or hemorrhagic) or the side of the brain affected by the lesion (left or right hemisphere) and any of the HRQoL domains.
Discussion
Stroke is a disease that is known to result in severe consequences for patients, their families and caregivers, since it is the most disabling of all chronic diseases, with major repercussions on the self-perceived HRQoL of its survivors. The sequelae resulting from Stroke lead to sensory and motor alterations, as well as cognitive and behavioral changes, altering patients’ physical, mental and social capacity.
Several studies conducted to investigate the repercussions of Stroke from a HRQoL perspective concluded that the psychosocial and physical well being of patients was strongly affected. Studies have evaluated Stroke patients with respect to their functional performance and presence of depression, and psychosocial issues such as social support, the patient’s social relationships, participation in leisure activities and return to work [3,16]. Better social support and family conditions have been associated with better results [9,17].
The most affected HRQoL domains, with means ≤ 50 in the SIS, were the following strength, hand function and participation. These findings are in agreement with those reported in the literature. Significant improvements were also found in all the domains evaluated at the time of discharge from the rehabilitation program, with the exception of the communication domain, which was found to be only slightly affected even at the time of admission to the program. It is estimated that approximately 20% of the patients who have had a Stroke are excluded from studies on HRQoL precisely because of aphasia or vascular dementia [18].
In the present study, 36% of patients were found to have depression, as measured using the HADS-D. This finding are little differs from reports in the international literature in which a frequency of 40% has been reported for cases of depression associated with a decline in HRQoL following CVA [20]. Depression is associated with increased disability and poorer function, in addition to affecting cognition, thus exerting a strongly negative effect on the rehabilitation process, on functional recovery and on HRQoL [18].
The time since Stroke (acute/subacute or chronic) was not found to have any effect on the majority of the domains evaluated in HRQoL in this study. A study conducted with patients evaluated during the acute phase 20 compared to the chronic phase [19,22], reported a similar improvement in perception of HRQoL in the functional domains. In a cross-sectional study conducted in Brazil by Froés et al. [16], an association was found between being female and having poorer physical functioning and perception of HRQoL. Similar findings have been reported in other studies [23,24]. In the present study, no statistically significant differences were found between sexes with respect to HRQoL, although men were slightly more likely to have higher mean scores in certain domains compared to the women.
Various studies have failed to find any association between HRQoL and education level, marital status, the hemisphere of the brain affected or comorbidities [16,24]. Studies of HRQoL have investigated socioeconomic, demographic and clinical aspects; however, few have succeeded in establishing any relationship with these variables [16].
Aprile et al. [23] found that physical components of HRQoL were more affected in patients with poor education levels, whereas mental components were affected to a greater extent in patients with higher education levels. In the present study, social class and mean family income were also found to increase as a function of the number of years of schooling.
Most of the patients in this study belonged to low social classes C or D, reflecting limited socioeconomic conditions in Brazil. A total of 88% of all the patients in the study received some kind of government benefit, either sickness benefit or a pension, with only one patient returned to work. The effect of Stroke in relation to the socioeconomic and productive conditions of individuals has been demonstrated, with the patient often being prevented from returning to work.
Improvements in functional performance, as measured by the modified Rankin Scale and the FIM, were found to have occurred between admission to the rehabilitation program and the end of the program, reflecting the real effect of these programs on these domains. Consequently, the improvements in functional performance led to improvements in the individuals’ perceptions of HRQoL in the physical domain, as well as to greater gains in patients’ participation and social interaction. These findings are in agreement with previous studies that also showed that improvements in functional performance exert an effect on an individual’s perception of HRQoL [7,19,21,25].
Paolucci et al. [26] reported that the level of functioning deteriorated with the severity of the Stroke, being considered one of the principal prognostic factors of consequences in functional performance.
It is important to identify the impact on each individual domain, since rehabilitation strategies and health promotion should be directed at specific problems. Such strategies include support in psychological and physical functioning, as well as social and family support, which will result in an increase in the patient’s sense of independence and participation. The rehabilitation program conducted within the SARAH network aims to achieving these objectives through an interdisciplinary approach, focusing on viable goals generated by the patients themselves and their families at each particular moment, as previously reported in other studies [27-29].
The present study found a connexion between HRQoL and an individual’s functionality level following Stroke, with a probable positive effect from participating in a neurological rehabilitation program. Although HRQoL and functional status are potentially related concepts, they represent different components of the individual’s health condition.
This study, provided comparative analyzes of patients before and after participating in a rehabilitation program, something that in Brazil most studies are cross-sectional.
Another fact was to have been held in a rehabilitation hospital specializing in this type of approach. Limitations to this study that should be mentioned include the fact that this was a convenience sample and that the number of patients was small, thus making it impossible to evaluate whether any correlations existed between the variables, the study design, absence of control group, only one examiner and patients in different stages of the disease (acute/subacute and chronic). Another important aspect that was not evaluated in this study is patient monitoring following discharge from hospital, including measurement of HRQoL, as has been performed in some international studies. This type of follow-up would enable data to be acquired on the extent to which improvements are maintained and to identify which domains are more affected following Stroke in this population.
Longitudinal and multicenter studies need to be conducted to increase knowledge on the affected constructs that are actually significant in the various regions and cultures, and the functional limitations that are modifiable through participation in rehabilitation programs.
In conclusion, in patients who have had a Stroke and whose HRQoL was more severely affected, the most affected domains were strength, hand function and participation. In relation to data on functioning, significant gains were found at discharge from the rehabilitation program compared to the data registered at admission.
Acknowledgement
We would like to thank Mr. Antonio Cunha Porto Maia important contribution in the statistical analysis performed by the discussions and data.
References
- O'Donnell MJ, Xavier D, Liu L, Zhang H, Chin SL, Rao-Melacini P, et al. Risk factors for ischaemic and intracerebral haemorrhagic stroke in 22 countries (the INTERSTROKE study): a case-control study. Inter stroke investigators. Lancet. 2010; 376: 112-123.
- Lavados PM, Hennis AJ, Fernandes JG, Medina MT, Legetic B, Hoppe A, et al. Stroke epidemiology, prevention, and management strategies at a regional level: Latin America and the Caribbean. Lancet Neurol. 2007; 6: 362-372.
- Carod-Artal FJ, Egidio JA. Quality of Life after Stroke: The Importance of a Good Recovery. Cerebrovasc Dis. 2009; 27: 204–214.
- Patrick DL, Erikson P. Health status and health policy. Oxford: Oxford University Press. 1993.
- Kranciukaite D, Rastenyte D. Measurement of quality of life in stroke patients. Medicina (Kaunas). 2006; 42: 709-716.
- Katona M, Schmidt R, Schupp W, Graessel E. Predictors of health-related quality of life in stroke patients after neurological inpatient rehabilitation: a prospective study. Health and Quality of Life Outcomes. 2015; 14; 13-58.
- Hopman WM, Verner J. Quality of life during and after inpatient stroke rehabilitation. Stroke. 2003; 34: 801-805.
- Kelley RE, Borazanci AP. Stroke rehabilitation. Neurological Research. 2009; 31: 832-840.
- Angeleri F, Angeleri VA, Foschi N, Gianquinto S, Nolfe G. The influence of depression, social activity, and family stress on functional outcome after stroke. Stroke. 1993; 24: 1478-1483.
- Carod-Artal FJ, Coral LF, Trizotto DS, Moreira CM. The Stroke Impact Scale 3.0 - Evalution of Acceptability, Reliability, and Validity of the Brazilian Version. Stroke. 2008; 39: 2477-2484.
- Riberto M, Miyasaki HM, Jucá SHH, Sakamoto H, Pinto PPN, Battistella LR. Validacao da versao brasileira da Medida de Independência Funcional. Acta Fisiátrica. 2004; 11: 72-76.
- Cincura C, Pontes-Neto OM, Neville IS, Mendes HF, Menezes DF, Mariano DC, et al. Validation of the National Institutes of Health Stroke Scale, modified Rankin Scale and Barthel Index in Brazil: the role of cultural adaptation and structured interviewing. Cerebrovasc Dis. 2009; 27: 119-122.
- Botega NJ, Bio MR, Zomignani MA, Junior CG, Pereira WAB. Transtornos de humor em enfermaria de clínica médica e validação da escala de medida (HAD) de ansiedade e depressão. Rev Saúde Pública. 1995; 29: 355-363.
- Almeida OP, Almeida SA. Confiabilidade da versão brasileira da escala de depressão em geriatria (GDS) versão reduzida. Arq Neuropsiquiatr. 1999; 57: 421-426.
- Béthoux F, Calmens P, Gautheron V. Changes in the quality of life of hemiplegic stroke patients with time: a preliminary report. Am J Phys Med Rehabil. 1999; 78: 19-23.
- Froés KSSO, Valdés MTM, Lopes DPLO, da Silva CEP. Factors associated with health-related quality of life for adults with stroke sequelae. Arquivos de Neuropsiquiatria. 2011; 69: 371-376.
- Kwok T, Lo RS, Wong E, Wai-Kwong T, Mok V, Kai-Sing W. Quality of life of stroke survivors: a 1-year follow-up study. Arch Phys Med Rehabil. 2006; 87: 1177-1182.
- Carod-Artal FJ. Determining quality of life in stroke survivors. Expert Rev Pharmacoecon Outcomes Res. 2012; 12: 199-211.
- Kong KH, Yang SY. Health-related quality of life among chronic stroke survivors attending a rehabilitation clinic. Singapore Med J. 2006; 47: 213-218.
- Barker-Collo SL. Depression and anxiety 3 months poster stroke: prevalence e correlates. Arch Clin Neurpsychol. 2007; 22: 519-531.
- Madden S, Hopman WM, Bagg S, Verner J, O’Callaghan CJ. Function status and health-related quality of life during inpatient stroke rehabilitation. Am J Phys Med Rehabil. 2006; 85: 831-838.
- Teixeira-Salmela LF, Faria CDC, Guimarães CQ, Goulart F, Parreira VF, Inacio EP, et al. Treinamento físico e destreinamento em hemiplégicos crônicos: impacto na qualidade de vida. Rev bras fisioter. 2005; 9: 347-353.
- Aprille I, Piazzini DB, Bertolini C, Bertolini C, Caliandro P, Pazzaglia C, et al. Predictive variables on disability and quality of life in stroke outpatients undergoing rehabilitation. Nerol Sci. 2006; 27: 40-46.
- Carod-Artal J, Egido JA, González JL, Varela de Seijas E. Quality of life among stroke survivors evaluated 1 year after stroke: experience of a stroke unit. Stroke. 2000; 31: 2995-3000.
- Muren MA, Hütler M, and Hooper Julie. Functional capacity and health-related quality of life in individuals post stroke. Top Stroke Rehabil. 2008; 15: 51-58.
- Paolucci S, Antonucci G, Grasso MG, Bragoni M, Coiro P, De Angelis D, et al. Funtional outcome of ischemic and hemorrhagic stroke patients after inpatient rehabilitation: A matched comparison. Stroke. 2003; 34: 2861-2865.
- Kalra L. The influence of stroke unit rehabilitation on functional recovery from stroke. Stroke. 1994; 25: 821-825.
- Musicco M, Emberti L, Nappi G, Caltagirone C, for the Italian Multicenter Study on Outcomes of Rehabilitation of Neurological Patients. Early and long-term outcome of rehabilitation in stroke patients: the role of patient characteristics, time of initiation, and duration of interventions. Arch Phys Med Rehabil. 2003; 84: 551-558.
- Barnes MP. Principles of neurological rehabilitation. J Neurol Neurosurg Psychiatry. 2003; 74: 3–7.