
Special Article – Rural Medicine
Austin Med Sci. 2020; 5(1): 1038.
Self-reported Barriers to Surgical Access in Rural Alabama: A Quality Controlled Assessment of Patient Perspectives
Smood B and Paxton R*
Department of Community Medicine and Population Health College of Community Health Sciences Institute for Rural Health Research, The University of Alabama, USA
*Corresponding author: Raheem J. Paxton, Department of Community Medicine and Population Health College of Community Health Sciences Institute for Rural Health Research, The University of Alabama, USA
Received: December 13, 2019; Accepted: January 11, 2020; Published: January 18, 2020
Abstract
Limited data exist on the barriers to surgical care in rural America. Prior studies have focused primarily on select procedures and not patient-reported barriers. As part of medical student’s capstone project during a rural medicine acting internship at a regional campus, we adapted and piloted a survey to examine barriers to surgery in the rural Deep South.
Methods: A participatory process was used to modify an existing survey. The final survey was piloted in a convenient sample of adults (N=10, Mean age = 61, 100% rural, 50% female). Descriptive statistics were used to characterize the study population.
Results: Among patients surveyed, 80% self-reported comorbid conditions. Commonly reported barriers to surgical care were lost wages due to surgery (75%), no one to care for family or belongings while out for surgery (75%), fear of surgery and/or complications (75%), and surgery not being an emergency (50%). The average distance travelled to receive surgery was 25 miles, or 31 minutes.
Discussion: Our data indicate that rural adults have several comorbid conditions and perceive that factors of affordability (e.g., lost wages) and acceptability (e.g., fear of surgery) are the most significant hurdles to surgery. Additional research and larger samples are needed to examine potential differences and disparities that may exist.
Keywords: Rural medicine; Healthcare barriers; Disparities; Surgery
Introduction
Rural populations experience significant challenges that contribute to poor health [1,2]. The challenges that are most concerning are those related to access to adequate healthcare. Studies have indicated that rural adults experience financial burdens, geographic isolation, lack of transportation, and high patient to provider ratios, which hinder adequate access to care [3-6]. The barriers to care experienced by rural Americans often translate to greater disease burden and higher mortality rates when compared to urban Americans [7].
The barriers observed in general access to care often translate to even greater deficits in access to surgical care [8,9]. Studies conducted in the United States correlate poor surgical outcomes in rural areas to lower socioeconomic status and inadequate access to surgical facilities and/or specialists [1,2,10-13]. In rural developing countries, common patient-reported barriers to surgical care include structural (i.e. distance to care, lacking nearby facilities/specialists), cultural (i.e. fears of surgery, or societal norms that discourage seeking care) and financial (i.e. lost wages during/after surgery, direct costs) factors [4]. To our knowledge, the patient-reported barriers experienced by rural Americans have not been adequately examined. Prior studies have focused exclusively on selected surgical procedures, and rarely address patient-perceived barriers to surgical care, particularly among populations with considerable disease burden [1-3,6,7,9-18]. Americans living in the rural Deep South are vulnerable especially to adverse health outcomes as a result of financial, geographic, contextual, and cultural barriers [1,2,6-8,10,14]. Thus, there is a need to elucidate the patient-reported perceived barriers that contribute to inadequate surgical care [15].
The purpose of this study was to address a significant gap in the literature by identifying patient-perceived barriers to surgical care through convenient sampling of adults living in the rural Deep South. This work reflects a capstone project of a third-year medical student’s community engagement as a requirement of an 8-week sub-internship in rural family medicine at the Tuscaloosa Regional Campus of the University of Alabama at Birmingham.
To do so, we applied a systematic approach to account for response bias. We used a participatory process to identify, adapt, and pilot our instrument in a rural patient population. To maximize participation and prevent misinterpretation, clear definitions and short surveys in plain language are requisite, particularly in rural communities where literacy is low [19-22]. Therefore, we sought to develop a survey that accurately assessed patients’ opinions regarding access to surgical care in order to provide important context when considering potential solutions. We provide a reliable, pilot-tested survey distributed to patients that can serve as a guiding framework for future investigations that may identify targeted solutions for addressing the perceived barriers to surgical care apparent to rural adults.
Methods
Sample and Survey design
Study participants were recruited from a Federally Qualified Healthcare Center (FQHC) in a rural city in the Deep South during two summer months of 2018. All survey participants were asked to participate in a self-reported survey and provide feedback based on their perception of surgical barriers in their respective communities. The instrument was pre-piloted for survey modification purposes. The final survey was established when 10 consecutive patients were able to complete the survey without assistance or suggestions for improvement. Only these 10 surveys were used in the analysis of this study, establishing a ‘true sample’ for this pilot study. The Flesch– Kincaid Grade score was 8.3, indicating statements were written in plain English and easily understood by 13 to 15 year old students. Eligibility criteria included living in rural Alabama (Pickens County) for more than 10 years, some high school education, and being an established patient at the local FQHC. Anonymized surveys were collected on paper and responses were manually transferred into a secure access database for analysis. The study protocol was approved by the University of Alabama Institutional Review Board as part of a larger community needs assessment study.
Procedures
To administer the survey, nursing staff provided patients with the questionnaire upon entering the exam room, which could be completed while waiting for the physician. Patients were educated on the purpose of the questionnaire, which included a written description of the study with consent to participate. Participation was voluntary. No incentive was provided. Patients were instructed that surgery is defined as any procedure requiring general anesthesia (“being put to sleep”). Distance travelled for surgery was calculated as the mileage from the home city to the hospital where participants reported receiving the procedure.
Survey modifications
Participant feedback was sought for general suggestions to improve the questionnaire, including readability, areas needing clarification, and length. Suggested modifications were incorporated at the end of one week intervals. In total, five versions of the questionnaire were distributed before establishing the final form of the survey. Primary concerns during survey development included that the survey was too long, which should be able to be completed before the physician entered the room.
Scaled responses for the primary endpoint were modified from a five-point Likert format and reduced to three-point responses including “Yes, No, or Maybe” [23]. Text size was increased, as many patients cited not having their reading glasses as a reason for not completing the survey. Open-ended responses we removed in the final product, but incorporated the commonest open-ended responses from pilot-surveys.
Measures
Barriers to Surgical Care: The instrument utilized for this study consisted of 19 of 38 barrier-specific items of a questionnaire that was developed and validated previously [24]. Items that were not relevant to rural Americans and those that were redundant were removed. The remaining 19-items pertained to the following domains: acceptability (e.g., fear of pain, anesthesia, complications), affordability (e.g., cost and lost wages), and accessibility (e.g., distance and time between referral and procedure). The original items was rated on a binary scale (yes or no). We revised the rating scale by adding a response category (i.e., maybe). Participants were asked to respond to the 19-items based on their perceptions of barriers in the community. Perceived barriers influencing access to surgical care were classified among three previously defined dimensions including: acceptability, accessibility, and affordability [24].
Those who had not received surgery that was previously recommended were asked to answer additional questions regarding their interest in the surgery, and check off the barriers that prevented the surgery. Additional questions, such as, “how hard is it for your community to get surgery if they needed it” and “types of surgeries previously had” were asked. The former was rated on a Likert-type response scale that included the following responses: “much harder, somewhat harder, not harder or easier, somewhat easier, much easier” [23]. The second question allowed participants to indicate whether or not they had a particular surgery.
Sociodemographic and medical characteristics
Study participants also self-reported their age, gender, education, insurance status, current employment, and chronic health conditions. A modified version of the Charleston Comorbidity index was utilized and total number of chronic health conditions were computed by summing the number of conditions indicated on the instrument.
Statistical Analysis
Descriptive statistics were computed to examine participant responses. Simple frequencies, percentages, means, standard deviations, and ranges were computed. Survey reliability was calculated using Chronbach’s alpha. As this is a pilot study with a small sample size, no significance tests were computed. All data were analyzed with SPSS version 24.0.
Results
Patient Characteristics
A total of 11 final surveys were distributed, and 10 were completed (90%). One patient declined to participate. We intentionally recruited 5-male and 5-female participants. All participants self-reported their race as Caucasian. Descriptive statistics of study participants were reported in Table 1. On average, participants were 61 years old (range 27-86) at survey completion, reported a previous diagnosis of high blood pressure (80%) or depression (40%), had Preferred Provider Organization insurance (40%), and completed at least some college (50%). Participants were either employed full-time (40%) or retired (40%). The average number of self-reported comorbid conditions was 3 (range 0 to 8; Table 2).
TABLECREATED
Table 1: Patient characteristics.
TABLECREATED
Table 2: Self-reported comorbidities among all patients.
Surgical Experience
In total, 7 (70%) participants reported receiving a prior surgery. Among these, 2 (29%) patients had 1 previous operation, 4 (57%) had 2 operations, and another had 4 operations. Average distance travelled to receive surgery was 25 miles (range 14 to 37 miles), or 31 minutes (range 17 to 43 minutes).
Most patients had prior orthopedic procedures (57%). Other common operations included cholecystectomy or hysterectomy (Table 3). The number of surgeries ranged from 0 to 4 with a mean of 1.8. A total of 3 participants indicated that they had not received a surgery recommended to them by a physician. One individual responded that this was because they could not “afford the surgery”. In addition to cost, a second participant cited that “they did not think they needed surgery” and “lacked sufficient information” to move forward with the surgery. Both patients had prior surgeries. A third participant (who never received surgery) responded that the potential “lost income from surgery” was a significant factor in their decision, in addition to a lack of desire to have surgery, and believing that their condition would not become an emergency.
TABLECREATED
Table 3: Self-reported patient surgical experience among individuals receiving surgery.
Perceived Barriers to Surgery
Most participants responded that it was difficult for their community to get surgery compared to others, with 6 (60%) stating it was “much harder” and 2 (20%) believing that it was “somewhat harder”. Frequencies of reported barriers to surgical care are shown in Figure 1. Among those answering that surgery is more difficult to get in their community, a majority 7/8 (88%) had undergone surgery in the past.
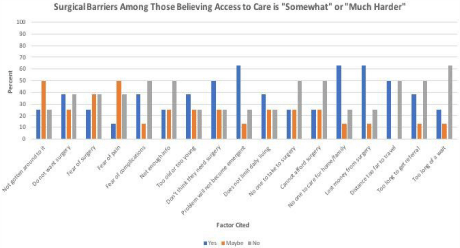
Figure 1: Percent of Patients citing factors making it difficult to obtain surgery.
Among 8 patients responding that it was “much more” or “somewhat more” difficult to obtain surgery where they live compared to other communities, they cited
the following factors scaled from, “yes”, to “maybe” to “no”. Non-emergent problems, lost wages from time off, and no one to care for their family, home, farm, etc.
were the most often cited factors.
Reliabilities of metrics defining barriers to surgical domains, including acceptability, accessibility, and affordability were 0.84, 0.89, and 0.86, reflecting high internal consistency reliability [24]. Among 8 (80%) patients reporting that surgery was more difficult to obtain in their community, environmental and resource reported barriers to care were predominate. Lost money from taking time off of work, no one to care for family or property, fear of surgery or complications, and the perception that the problem would not become emergent was cited by 6 (75%) patients. Five (63%) cited that the problem did not affect their daily living enough to warrant surgery. Excessive costs, or distance was cited by half of patients. Only 3 patients (38%) cited too long of wait times. Males appeared to be most concerned with no one being able to care for property or family.
Discussion
This study highlights the utility of regional medical campuses in exposing medical students to healthcare inequities that challenge rural populations, in order to cultivate and inspire a professional mindset focused on improving access to care in some of the nation’s most vulnerable populations. In this study, we demonstrate a simplified survey that can be implemented in rural family medicine clinics (and modified using several guiding principles) to elucidate other factors equally concerning to patients. Most patients indicated that it was harder to get surgery in their rural communities, and that there are several individually perceived barriers that prevent surgical care. The most commonly reported perceived barriers to surgical care were lost wages, no one to care for belongings while out on surgery, fear of surgery and/or complications, and the belief that their problem would not become an emergency. These data provide new insight into the challenges that prevent access to surgical care in the rural Deep South.
Others have demonstrated that more than half of patients who are referred for surgical care do not receive surgery; however, it is unclear why.16-18 Physicians often speculate that cost is the chief barrier [25]. While financial burdens for rural communities are real, this may overshadow other equally important challenges, such as the burden of lacking social support, as demonstrated in this study [1,4,6-9,12,13,24,26]. Prior studies have investigated communication barriers (particularly in non-English speaking populations), insurance status, and long wait times, yet rarely together.3,6,13 Because administering community health surveys can cost up to $25,000 for broad implementation, it is essential to establish a framework for community analysis that is both cost-effective and accurate [20]. We demonstrate a simplified survey that can be distributed in rural family medicine clinics (and modified using several guiding principles) to elucidate factors that concern patients. Additional research is needed to determine whether the barriers we observed are generalizable to others living in the rural Deep South. Furthermore, a larger, ethnically diverse sample is needed to clarify our observations.
Many studies identifying barriers to rural surgical care are inferential, extrapolating demographic or geographic data and outcomes without regard for patient perceptions [1,10,12,13,27]. Contrary to previous findings, our data suggests that only half of participants in this pilot-study believe travel distance and/ or transportation is a significant deterrent to surgical care [12]. Despite patients reporting long commutes between their hometown and surgical sites, we observed that every patient forgoing a recommended surgery alternatively cited financial concerns. This may reflect that while rural populations are accustomed to traveling extensive distances for routine activities (i.e. grocery shopping, gas refueling, work, etc.), coordinating tasks to optimize the efficiency of a long commute may weigh heavily in their cost-benefit analysis when deciding to obtain surgical care. Moreover, wait times do not appear to be as oppressive as has been previously reported in both surgical and primary care, suggesting that the inconveniences of accessibility may not weigh as heavily as those of affordability and psychosocial acceptability [8,13].
By surveying established patients at a FQHC (which are developed in part to improve access to primary care in low-income communities), it appears that barriers other than geographic isolation may continue to present unique challenges in improving access to surgical care. Communication barriers may well be synonymous with surgical barriers.
Patients often underestimate the severity of their medical conditions, and overestimate their ability to manage them [28]. However, self-reflection through surveys alone has been demonstrated to increase patient interest in healthcare management [28]. A striking number of participants in this study cited fear as a limitation to surgical care. As such, psychosocial perceptions (i.e. skepticism, distrust, antipathy) and/or communication barriers may deter patients from following through with care. It remains to be seen if this pilotsurvey could facilitate communication and patient consideration of indicated surgical interventions that might otherwise be dismissed. This underscores the importance of establishing trust and providing adequate education to rural community members while balancing patient autonomy, which could direct subsequent resource allotment for targeted interventions to improve surgical accessibility.
There were several strengths associated with this study. In particular, the survey established the framework and provides necessary principles for developing a concise and comprehendible survey for assessing the perceptions of community members. The development process illustrated the importance of participant feedback in developing a targeted survey that can be used for future investigation into patient perspectives. Despite the strengths, there were a number of weaknesses. The small sample of responses using the final survey is undoubtedly a limitation to this pilot and proofof concept study, which prevents drawing significant conclusions. In addition, self-report surveys are associated with recall and response bias. Lastly, these data do no imply causal inference.
In summary, we used a participatory process to adapt and pilot a survey assessing barriers to surgical care in the rural Deep South. The intensive and iterative process contributed to successfully launching our pilot survey in a small rural clinic. Results of this survey demonstrate several important principles that must be maintained in future investigations into barriers to surgery as a framework for future research [29]. This pilot study elucidates that barriers to surgery are complex and multifactorial, yet provides as a model for survey development and implementation for a more intricate and customized analysis to understanding key factors to improving access to surgical care in rural communities. In addition to improving the proximity of surgical services and reducing the financial strain of elective surgical procedures, implementing systemic solutions that reduce the burden of surgery and recovery times may ultimately prove paramount to improving access to rural surgical healthcare [30,31].
References
- Gruber K, Soliman AS, Schmid K, Rettig B, Ryan J, Watanabe-Gallowys S. Disparities in the Utilization of Laparoscopic Surgery for Colon Cancer in Rural Nebraska: A Call for Placement and Training of Rural General Surgeons. J Rural Health. 2015; 31: 392-400.
- Zahnd WE, Hyon KS, Diaz-sylvester P, Izadi SR, Colditz GA, Brard L. Ruralurban differences in surgical treatment, regional lymph node examination, and survival in endometrial cancer patients. Cancer Causes Control. 2018; 29: 221-232.
- Broman AT, Hafiz G, Muñoz B, Rodriguez J, Snyder R, Klein R, et al. Cataract and barriers to cataract surgery in a US Hispanic population: Proyecto VER. Arch Ophthalmol. 2005; 123: 1231-1236.
- Grimes CE, Bowman KG, Dodgion CM, Lavy CB. Systematic review of barriers to surgical care in low-income and middle-income countries. World J Surg. 2011; 35: 941-950.
- Gulack BC, Heydari S, Figueroa, Sherry S Ross, David Boyd, Henry E Rice, et al. Ranking and Rating Analyses of Barriers to Surgical Care for Children in Guatemala. Int J Surg Res Pract. 2015; 2: 1-5.
- Ojinnaka C, Vuong A, Helduser J, Nash P, Ory MG, McClellan DA, et al. Determinants of variations in self-reported barriers to colonoscopy among uninsured patients in a primary care setting. J Community Health. 2015; 40: 260-270.
- Fradgley EA, Paul CL, Bryant J. A systematic review of barriers to optimal outpatient specialist services for individuals with prevalent chronic diseases: what are the unique and common barriers experienced by patients in high income countries?. Int J Equity Health. 2015; 14: 52.
- Rust G, Ye J, Baltrus P, Daniels E, Adesunloye B, Fryer GE. Practical barriers to timely primary care access: impact on adult use of emergency department services. Arch Intern Med. 2008; 168: 1705-1710.
- Khubchandani JA, Shen C, Ayturk D, Kiefe CI, Santry HP. Disparities in access to emergency general surgery care in the United States. Surgery. 2018; 163: 243-250.
- Carr BG, Bowman AJ, Wolff CS, Mullen MT, Holena DN, Branas CC, et al. Disparities in access to trauma care in the United States: A population-based analysis. Injury. 2017; 48: 332-338.
- Mannschreck D, Matsuno RK, Moriarty JP, Levinson KL, Temkin SM, Fader AN, et al. Disparities in Surgical Care Among Women With Endometrial Cancer. Obstet Gynecol. 2016; 128: 526-534.
- Albornoz CR, Cohen WA, Razdan SN, Pusic AL, Cordeiro PG, Matros E, et al. The Impact of Travel Distance on Breast Reconstruction in the United States. Plast Reconstr Surg. 2016; 137:12-18.
- Bauder AR, Gross CP, Killelea BK, Butler PD, Kovach SJ, Fox JP, et al. The Relationship Between Geographic Access to Plastic Surgeons and Breast Reconstruction Rates Among Women Undergoing Mastectomy for Cancer. Ann Plast Surg. 2017; 78: 324-329.
- Markin A, Habermann EB, Chow CJ, Zhu Y, Vickers SM, Al-Refaie WB. Rurality and cancer surgery in the United States. Am J Surg. 2012; 204: 569- 573.
- Westerveld D, Yang D. Through Thick and Thin: Identifying Barriers to Bariatric Surgery, Weight Loss Maintenance, and Tailoring Obesity Treatment for the Future. Surg Res Pract. 2016: 8616581.
- Pitzul KB, Jackson T, Crawford S, Sockalingam S, Hawa R, Urbach D, Okrainec A, et al. Understanding disposition after referral for bariatric surgery: when and why patients referred do not undergo surgery. Obes Surg. 2014; 24: 134-140.
- Diamant A, Milner J, Cleghorn M, Okrainec A, Jackson TD, Quereshy FA, et al. Analysis of patient attrition in a publicly funded bariatric surgery program. J Am Coll Surg. 2014; 219: 1047-1055.
- Afonso BB, Rosenthal R, Li KM. Perceived barriers to bariatric surgery among morbidly obese patients. Surgery for Obesity and Related Diseases. 2010; 6: 16-21.
- Ostby PL, Armer JM, Smith K, Stewart BR. Patient Perceptions of Barriers to Self-Management of Breast Cancer-Related Lymphedema. West J Nurs Res. 2017; 193945917744351.
- Kwan K, Do-reynoso V, Zarate-gonzalez G. Development and implementation of a community health survey for public health accreditation: Case study from a rural county in California. Eval Program Plann. 2018; 67: 47-52.
- Willson ML, Vernooij RWM, Gagliardi AR. Questionnaires used to assess barriers of clinical guideline use among physicians are not comprehensive, reliable, or valid: a scoping review. J Clin Epidemiol. 2017; 86: 25-38.
- Gayet-ageron A, Agoritsas T, Schiesari L. Barriers to participation in a patient satisfaction survey: who are we missing?. PLoS ONE. 2011; 6: e26852.
- Derrick B and White P. Comparing Two Samples from an Individual Likert Question. International Journal of Mathematics and Statistics. 2017; 18: 1-13.
- Gyedu A, Abantanga F, Boakye G, Gupta S, Otupiri E, Agbeko AE, et al. Barriers to essential surgical care experienced by women in the two northernmost regions of Ghana: a cross-sectional survey. BMC Womens Health. 2016; 16: 27.
- Tork S, Meister KM, Uebele AL, Hussain LR, Kelley SR, Kerlakian GM, et al. Factors Influencing Primary Care Physicians’ Referral for Bariatric Surgery. JSLS. 2015; 19.
- Coburn N, Fulton J, Pearlman DN, Calvin Law, Brenda DiPaolo BS, Blake Cady, et al. Treatment variation by insurance status for breast cancer patients. Breast J. 2008; 14: 128-134.
- Kelly C, Hulme C, Farragher T. Are differences in travel time or distance to healthcare for adults in global north countries associated with an impact on health outcomes? A systematic review. BMJ Open. 2016; 6: e013059.
- Henchcliffe BE, Holihan JL, Flores-gonzalez JR, Mitchell TO, Ko TC, Kao LS, et al. Barriers to Participation in Preoperative Risk-Reduction Programs Prior to Ventral Hernia Repair: An Assessment of Underserved Patients at a Safety-Net Hospital. JAMA Surg. 2016; 151: 488-490.
- Meara JG, Leather AJ, Hagander L, Alonso N, Ameh EA, Bickler SW, et al. Global Surgery 2030: evidence and solutions for achieving health, welfare, and economic development. Lancet. 2015; 386: 569-624.
- Soffin EM, Gibbons MM, Ko CY, Wick EC, Cannesson M, Scott MJ, et al. Evidence Review Conducted for the Agency for Healthcare Research and Quality Safety Program for Improving Surgical Care and Recovery: Focus on Anesthesiology for Total Hip Arthroplasty. Anesth Analg. 2018.
- Kalogera E, Nelson G, Liu J, Ko CY, Wick E, Dowdy SC, et al. Surgical Technical Evidence Review for Gynecologic Surgery Conducted for the AHRQ Safety Program for Improving Surgical Care and Recovery. Am J Obstet Gynecol. 2018.