
Case Series
Austin Med Sci. 2022; 7(2): 1066.
Double Transcrestal Sinus Lift Procedure with Collagen as Bone Void Filler Alone in Atrophic Maxilla: 5 Years Retrospective Radiological Study
Crespi R¹, Toti P², Covani U², Crespi G², Brevi BC³ and Menchini-Fabris GB¹*
¹School of Dentistry, Saint Camillus International University of Health and Medical Sciences, Italy
²Tuscan Dental Institute, Versilia Hospital, Italy
³Department of Maxillo-Facial Surgery, Hospital and University of Pisa, Italy
*Corresponding author: Menchini-Fabris GB, San Rossore Dental Unit, San Rossore Hospital, Vialedelle Cascine 152 San Rossore, 56122 Pisa, Italy
Received: June 30, 2022; Accepted: July 21, 2022; Published: July 28, 2022
Abstract
Objectives: The present study aimed to investigate the effectiveness of transcrestal double-elevation of the maxillary sinus (TSFE) with an implant placement during the second-stage surgery in the maxillary areas with a residual alveolar bone less than 3mm.
Materials and Methods: Patients with long-standing edentulous areas underwent double TSFE surgery involving a first transcrestal maxillary sinus floor augmentation with a collagen sponge to fill the intrabony cavity and a second osteotome-mediated sinus floor elevation by using an electromagnetic device and immediate implant placement. The radiographic changes in bone heightwere measured and compared during the different time intervals by nonparametric statistics with p < 0.01.
Results: Twenty-eight patients were retrospectively selected for the study. A total of 42 implants were positioned in 28 augmented sinuses. After the first TSFE surgery, no minor swelling of gingival mucosa, no mucositis, or flap dehiscence with suppuration was found. After three months a second TSFE with simultaneous implant placement was performed; four patients experienced minor nasal bleeding. Significant increases in the bone height had been respectively reported for the first (from 2.3±0.2 to 9.5 ± 0.3 mm) and second surgeries with p-values less than 0.0001 and an overall bone height measured 5 years after the first surgery of 12.2±0.3 mm.
Conclusion: The present study suggested to clinicians the possibility of osteotome double sinus lifting and grafting with highly absorbable collagen material, generally used as a haemostatic agent alone in case of residual bone height less than 3 mm.
Keywords: Double transalveolar sinus floor elevations; Collagen sponge; Highlyresorbable substitute material; Dental implants
Abbreviations
RBH: Residual Bone Height; CBCT:Cone Beam Computerized Tomography; CT:Computerized Tomography; AH:Alveolar Height; ΔAH:Alveolar Height Change; TSFE:Transalveolar Sinus Floor Elevation.
Introduction
Maxillary sinus pneumatization was a physiologic process that most commonly could occur in older adults after long-standing edentulism after the removal of more distal teeth [1]. It was highly likely that the cause of the “fourth expansion” of the maxillary sinus, as it’s usually called by the anatomists, could be explained as resulting from a disuse/atrophy phenomenon after tooth loss. Reduction of functional could create an imbalance between apposition and resorption of alveolar bone beneath the sinus so causing a shift in the remodeling process towards a combination of volume enlargement of the sinus as well as loss of the alveolar bone [2]. A very particular case was when the maxillary sinus was fully hyperpneumatized at the expense of the edentulous alveolar ridge [3]. To rehabilitate an edentulous patient with an implant-supported prosthesis in the posterior dentition, maxillary sinus surgery was often recommended if the Residual Bone Height (RBH) ranged from 1 mm to 6 mm in thickness [4].
It was recently supposed by some researchers that the substantial increase in the volume of bone beneath the sinus floor could be achieved without any use of bone-substituting materials [5,6].
Moreover, it seemed that simple elevation of the Schneiderian membrane could stimulate new bone formation, which was found to be very close to the limit of surgical margins [7]. Some studies describing results of simple elevation of the sinus membrane without any grafting material suggested that the membrane had good osteoinductive properties [8,9].
The present study aimed to investigate the effectiveness of transcrestal double-elevation technique of the maxillary sinus with an implant placement during the second-stage surgery in the maxillary areas with a residual alveolar bone less than 3 mm. The radiographic changes in height had to be measured and compared during the different time intervals.
Materials and Methods
Patient Selection
Subjects were arbitrarily selected from a single cohort of patients who underwent dental implant-supported prosthetic rehabilitation for the present study with a retrospective design with no control subjects or randomization. All patients were treated by a single experienced surgeon (UC) and rehabilitated by a single prosthodontist (CR) from October 2010 to November 2018 at the Tuscan Stomatologic Institute and followed up at the Complex Operating Unit of Maxillo-Facial Surgery of the University of Pisa.
Retrospective analyses of routinely collected data resulted from a revision process based on patients’ case sheets that were performed after all the subjects selected for this case-cohort study signed an explicit consent for the retrospective analysis.
All procedures performed in studies involving human participants followed the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Inclusion Criteria
Patients were included in the selection if they met the following criteria:
• adulthood (greater than or equal to 18 years); • mono or bilateral large edentulous area before rehabilitation in the posterior maxilla; • presence of residual bone height between 1 mm and 2 mm measured from the alveolar crest to floor of maxillary sinus; • treatment with double transcrestal sinus floor elevations technique; • delayed dental implant placement and prosthetic rehabilitation; • full set of preoperative (before first surgery) and postoperative 3D imaging at 3 months (before implant placement) and 5 years survey.
Exclusion Criteria
Patients were excluded if any of the following criteria were present:
• metal corruption of the CBCT scans;• treatment with irradiation and/or bone resection as part of a cancer treatment plan;• administration of bisphosphonates (intravenous and/or oral);• report of smoking habit (more than 10 cigarettes/days);• report of alcohol or drug abuse.
Surgical Procedure
The need for vertical bone augmentation was established by Computerized Tomographic (CT) scanning. All patients were administered local anesthesia (Lidocaine 2% with epinephrine 1:80,000, Xylocaine®, AstraZeneca SpA, Milan, Italy). Surgical guidelines recommended premedication with non-steroidal antiinflammatory drugs (mainly naproxen, 1.5g, Naprosyn, RecordatiSpA, Milan, Italy) and antimicrobial agents (mainly ciprofloxacin§§) 1 hour before surgery. Antibacterial and anti-inflammatory drugs administration was continued at most for one week after surgery. A partial-thickness flap was made by a crestal incision and elevated in the alveolar crestal area needing vertical expansion [10].
Occlusal and rectangular-shaped access to the maxillary sinus was created with bone tips mounted on a piezoelectric device (SONICflex™, Kavo, Germany). Then the edges of the trapdoor were gently fractured from the rest of the bone of the alveolar process with osteotomes mounted on an electromagnetic device (Magnetic Mallet®, Osseotouch, Turbigo, Italy www.osseotouch.com). The sinus membrane was carefully detached using a manual curette (De Marco N° 2, Hu-Friedy, Chicago, IL, USA), mobilized, and pushed inside the sinus with the autogenous bone fragment pushed [11]. When the amount of new space was deemed sufficient to meet the need of the clinician a collagen sheet (Condress®, Abiogen Pharma, Pisa, Italy) was placed to fill the gap and to maintain an apically displaced trapdoor. A primary wound closure by sutures was performed and removed after 7 days (Figure 1). The second same technique-the same surgeon approach was repeated after 3 months combined with an immediate implant placement procedure (Figure 2). The sinus floor was newly pushed up, and, after placement, the dental implant itself provided a tenting effect. After implant (Perfect, Avenir, Santarcangelo di Romagna, Italy) placement the flaps were positioned to their original level and secured with sutures. A scheme of the surgical steps was depicted in (Figure 3).
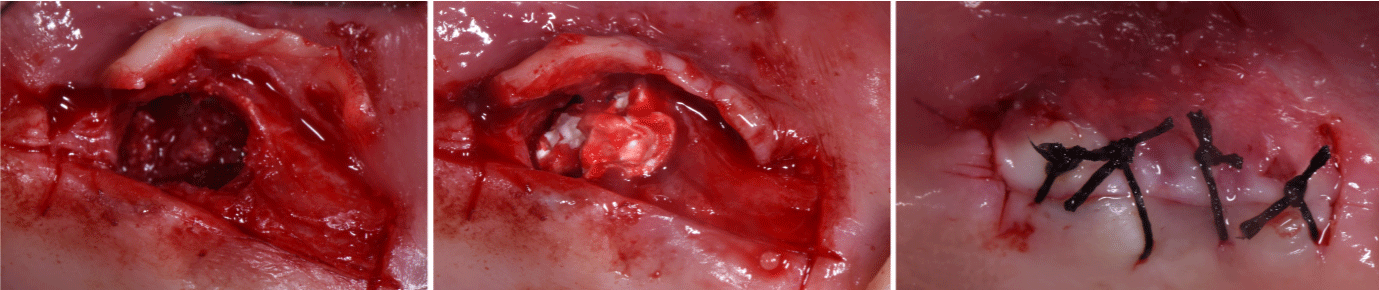
Figure 1: a) Image showing the edentulous ridge of the maxilla before surgery. When all the occlusal portion of the edentulous crest was marked the tip of the
corresponding bone expander was used. b) Clinical photograph showing totally mobile bone crest internally to the sinus cavity. (c) Collagen sheets placed in the
created cavity to maintain in its position the bone crest apically displaced.
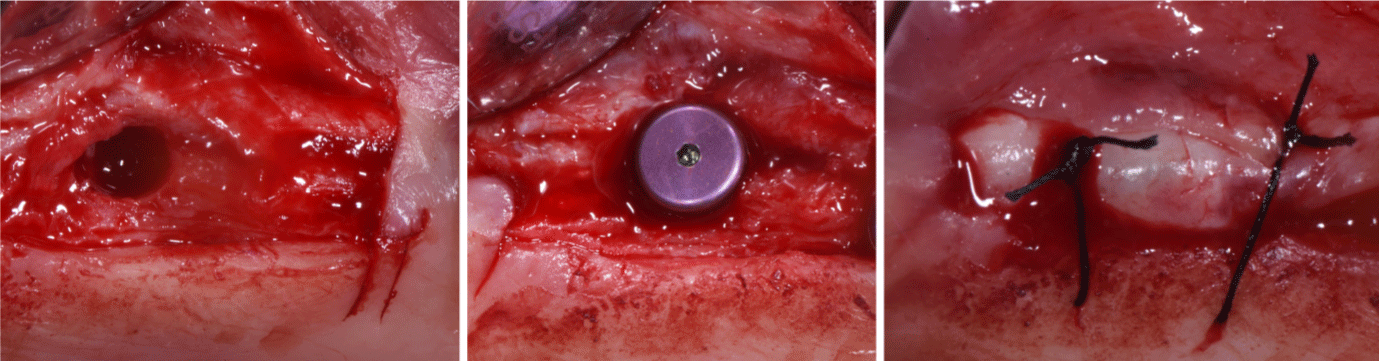
Figure 2: a) The implant site was created, expanding the tissue that filled the cavity created with the stage 1 in all directions; b) implant in place; c) buccal flap
was repositioned and stabilized with sutures tied to the margin of the lingual/palatal flap and anchored buccally with a loose loop to the periosteum at the level of
the alveolar mucosa.
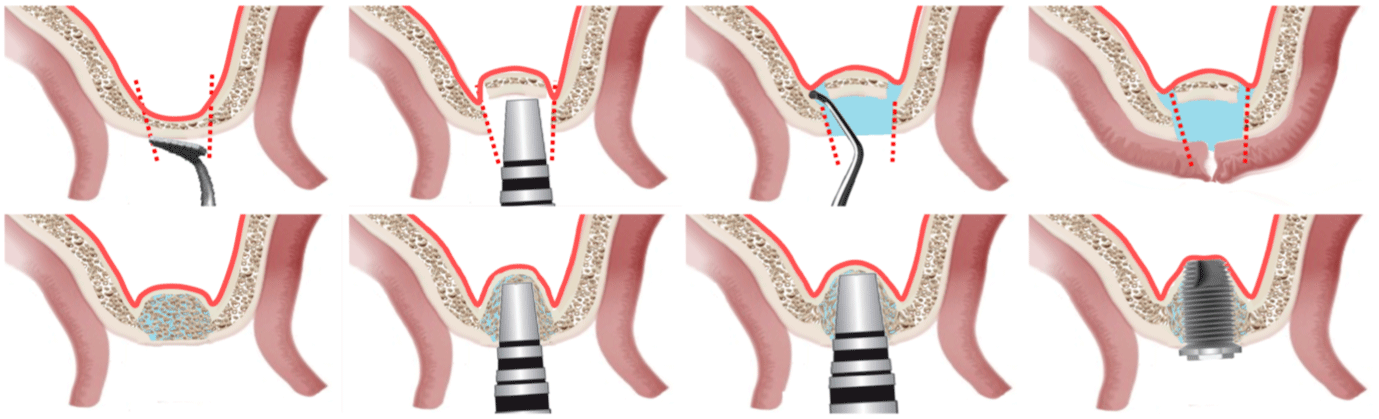
Figure 3: Scheme showing double-stage transalveolar sinus lift technique: A) bone crest incision; B) totally mobile bone crest internally to the sinus cavity; C)
membrane lifting; D) collagen sheets placed in the created cavity; E) healed site; FG) intermediate and lifting osteotome mounted on the Magnetic Mallet®; H)
implant placed.
The Final prosthetic restoration was cemented 5 months after implant placement.
Follow-up and Radiographic Assessments
The cone-beam computerized tomography scans (Gendex GXCB-500; Gendex Dental Systems 1910 North Penn Road Hatfield, PA 19440) allowed the clinician to view the amount of bone height beneath the maxillary sinus and enabled the surgeon to plan the surgeries. Preoperative and postoperative scans were modified appearing superimposable according to Crespi and co-workers and were saved as dicom files [12]. CBCT cross-sectional images were extrapolated from each set of the three scans superimposable in the space and measurements of Alveolar Height (AH), that is, the distance from the most coronal point of the alveolar crest to the floor of the maxillary sinus along the implant direction (Figure 4). The AlveolarHeight Change (ΔAH) was calculated following equation 1:
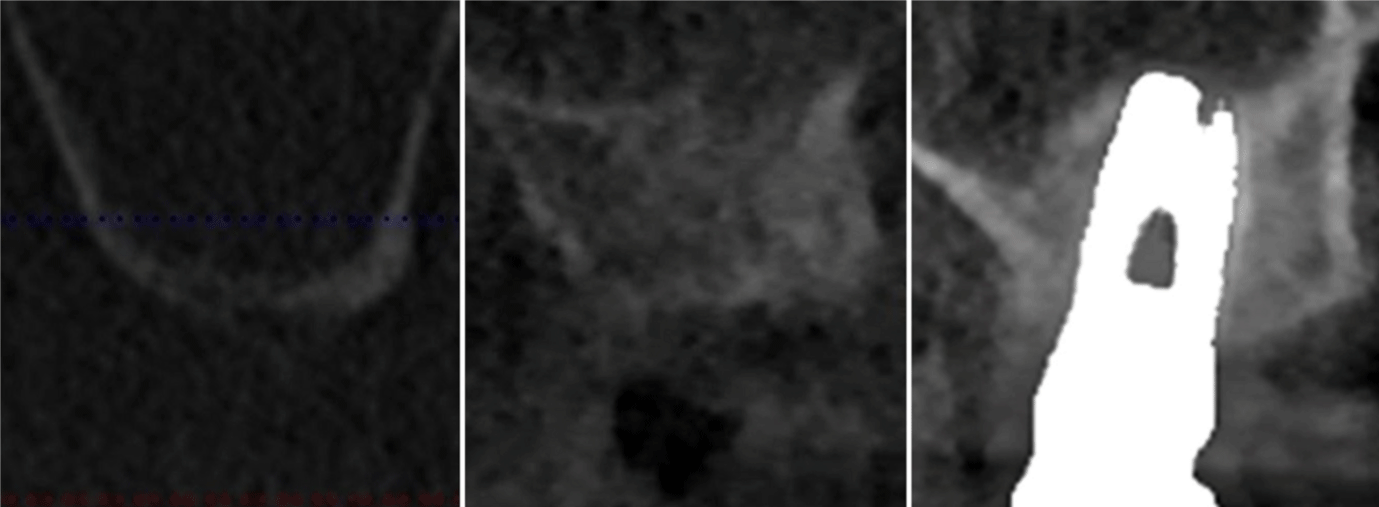
Figure 4: a) The distance between the ridge crest and the floor of the sinus is measured on a preoperative periapical cone beam; b) 3 months later, cone beam
cross sectional image revealed a modified profile or the cortical bone lining the floor of the maxillary sinus. The bone volume increase is evident; c) cone beam cross
section at 5 years follow-up. The modified profile or the cortical bone lining the floor of the maxillary sinus can be identified above the implant.
ΔAHpreop→postop=AHpostop-AHpreop (Equation 1)
A positive value of ΔAH represented the net bone gain expressed by the difference between the gain in bone height within the sinus and the crestal bone. All measurements of the bone height over time were taken twice (repeated 1 week apart) by two independent measurers (PT, GC), who were not involved in the performance of the surgical treatment with free standalone software (Osiris 4.19 the University of Genève. Switzerland).
Statistical Analysis
Statistical analyses were performed using a statistical tools package (Statistics Toolbox, MatLab 7.11; The MathWorks, Natick, MA, USA).
In the case of both bilateral procedures (alternating, never simultaneous) being selected, only one surgical site per patient was randomly chosen by a binary random number generator. Brown- Forsythe test of homogeneity was used to test if variance among all the subgroups was not the same; normality of data was tested by the Shapiro-Wilk test for all subgroups investigated. A Bland–Altman analysis measured the inter- and intraobserver agreements. The effects on alveolar height levels and bone level changes were evaluated with a non-parametric two-way repeated-measures test (Friedman). The data passed all the following four assumptions: the group was measured on three different occasions, and all the treated patients were selected from a single cohort (it could be assumed that subjects represented a random sample from the population of patients suffering from severe maxillary sinus hyperpneumatization); the outcome variables were measured at a continuous level, and the sample was not normally distributed. Friedman’s posthoc multiple comparisons test with Tukey’s honestly significant difference criterion was used for comparisons among time points. The related p-values were registered. Effects of the sample and results of a power analysis were respectively determined with a power of 0.99, the reported sample size, and the measures of central tendency and dispersion). Data were described as mean ± standard deviation and given to one decimal place. The methodology was reviewed by an independent statistician who set the level of significance at 0.01.
Results
Twenty-eight patients were selected for the present retrospective analysis. Subjects were 15 females and 13 males; the mean age was 51.7 years, varying from 31.8 to 71.2 years. A total of 42 implants were positioned in 28 sinuses lifted and grafted areas.
The preoperative value of the alveolar height was 2.3±0.2 mm as reported in Table 1. After the first TransalveolarSinus Floor Elevation (TSFE) surgery, no minor swelling of gingival mucosa was present in the first days after the surgical procedure; neither mucositis nor flap dehiscence with suppuration was found in the following days. After about three months a second TSFE procedure with a simultaneous implant placement was performed; four patients experienced minor nasal bleeding, which disappeared within the first 24 to 48 hours.
alveolar height (AH)
Friedman (time effect): df=2, MS=87808, c2 = 295.20, p-value <0.0001
Brown-Forsythe (homogeneity of variance): F=4.4649, df1= 2, df2=81, p-value = 0.0145
baseline
3 months
5 years
mean
size = 28
2.3±0.2
9.5±0.3
12.2±0.3
Shapiro-Wilk test p-value
0.0099
0.3872
0.1433
baseline versus 3 months
intragroup analysis p-value
< 0.0001°
post-hoc estimated effect size
ND
(post-hoc power analysis)
ND
3 months versus 5 years
intragroup analysis p-value
< 0.0001°
post-hoc estimated effect size
any size
(post-hoc power analysis)
1
baseline vesus 5 years
intragroup analysis p-value
< 0.0001°
post-hoc estimated effect size
ND
(post-hoc power analysis)
ND
Friedman (aspect effect, mesial/distal): df=1, MS=1.33, c2 = 0.0050, p-value = 0.9434
Brown-Forsythe (homogeneity of variance): F=4.6799, df1= 5, df2=162, p-value = 0.0005
baseline
3 months
5 years
mesial
size = 28
2.2±0.3
9.2±0.6
11.8±0.6
Shapiro-Wilk test p-value
0.009
0.1965
0.0432
distal
size = 28
2.3±0.4
9.7±0.7
12.5±0.6
Shapiro-Wilk test p-value
0.7943
0.1557
0.0934
mesial vs distal
intergroup analysis p-value
0.2455°
0.0372°
0.0111°
post-hoc estimated effect size
ND
82
36
(post-hoc power analysis)
ND
0.62
0.96
Friedman (aspect effect, buccal/palatal): df=1, MS=372.02, c2 = 1.39, p-value = 0.2369
Brown-Forsythe (homogeneity of variance): F=3.1976, df1= 5, df2=162, p-value = 0.0088
baseline
3 months
5 years
buccal
size = 28
2.2±0.3
8.7±0.6
12.4±0.5
Shapiro-Wilk test p-value
0.1331
0.9666
0.8318
palatal
size = 28
2.3±0.3
10.3±0.5
12.0±0.3
Shapiro-Wilk test p-value
0.0049
0.1452
0.5719
buccal vs palatal
intergroup analysis p-value
0.4873°
< 0.0001°
0.0395°
post-hoc estimated effect size
ND
6
49
(post-hoc power analysis)
ND
1
0.88
Table 1: Mean and standard deviation of the alveolar bone height at baseline (pre-extraction), at 3 months and after 5 years for sites underwent sinus lifting with collagen sponges and malleting implant insertion. Measurements were taken along the implant direction after three-dimensional scans fusion. Statistical comparisons: multiple comparison test with Friedman test and Tukey’s honestly significant difference criterion. Post-hoc paired comparison test: °Wilcoxon signed rank test with significant results in bold. Power analysis and effect of the sample size with a significance level of 0.01, and a power of 0.99 (ND when not applicable).
There was a suitable wound healing around temporary abutments, with a fine adaptation to the temporary crown. The final prosthetic restorations were cemented 3 months after implant placement. After fixed-prosthetic rehabilitation, no pain or prosthesis mobility was recorded.
Regarding the reproducibility of the intra- and inter-observer measurements, the intraobserver differences between the two measurements expressed in standard deviation units ranged from -1.4 to 1.7 with percentages of the sample within the range of the two standard deviations changed in the interval from 93.8% to 96.4%. The interobserver differences between the two measurements expressed in standard deviation units ranged from -1.2 to 1.8 with percentages of the sample within the range of the two standard deviations changed in the interval from 92.0% to 97.3%.
All radiographic outcomes were reported in Table 1 with statistics and power analyses calculated for each test based on the reported sample size. Non-parametric analysis of variance and posthoc tests applying the correction for multiple comparisons (Table 1) attested that, after surgical procedures, significant increases in the bone height had been respectively reported for first (from 2.3±0.2 to 9.5±0.3 mm) and second surgery with p-values less than 0.0001 and an overall bone height measured 5 years after the first surgery of 12.2±0.3mm. When aspects around dental implant have been investigated, linear measurements of alveolar height suggested that a significant difference with a p-value < 0.0001 had been registered at 3 months between the buccal (8.7±0.6) and the palatal side (10.3±0.5). These tendencies have been registered when also changes at the alveolar height have been calculated. Significant differences had been registered between the buccal (increases of 6.5±0.5 mm and 3.6±0.8 mm, respectively for first and second surgery) and the palatal sites (increases of 8.0±0.5 mm and 1.7±0.6mm, respectively for first and second surgery) as reported in (Figure 5).
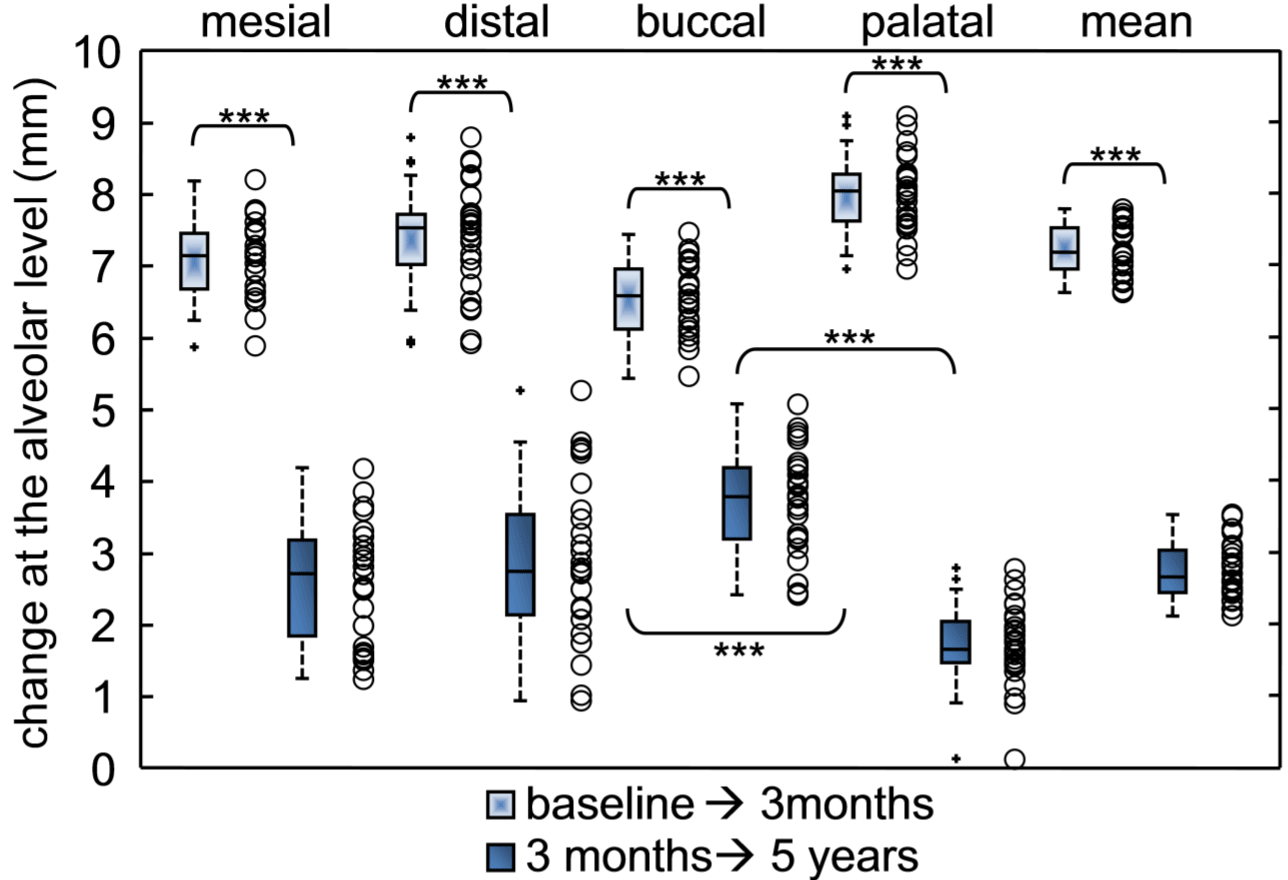
Figure 5: Scatter (empty points) and box plots for all-aspects (mesial, distal, buccal, palatal and their mean) regarding to changes at the alveolar height level (ΔAH)
at different time points: from baseline to 3 months in light-box; from 3 months to 5 years in full-box. In box-and-whiskers plot, the box line represents the lower,
median, and upper quartile values; the whisker lines include the rest of the data. Outliers (solid X) were data with values beyond the ends of the whiskers. Wilcoxon
signed rank test: * significant (p-value < 0.01), ** very significant (p-value < 0.001), *** extremely significant (p-value < 0.0001).
None of the selected patients experienced implant failure.
Discussion
The present study suggested the likelihood of an extension of the application of the osteotome sinus floor elevation procedure without grafting material to the severely reabsorbed atrophic maxillae in patients with hyper-pneumatized sinuses with a residual bone height of less than 3 mm.
The Lundgren and co-workers’ past experiences where they verified on radiographs the presence of new bone formation also for ungrafted sinus floor elevation highlighted the need to test the use of collagen as a filling material in transcrestal double-elevation technique to better understand its limits [13]. In addition to the lack of bone support, another problem to be solved when vertically augmenting the sinus floor in an atrophic maxilla was represented by the presence of type 4 bone in which, very frequently, the bony trabeculae disappeared or were simply covered with a thin cortical layer of compact bone [14].
Even though some authors reported that the Schneiderian membrane detachment because of exposure of the bone surface to osteoprogenitors binding sites had the feature of positively favored vascularization, cell colonization, and new bone formation [15], in separate experiments, the researchers found that both exposed walls of the maxillary sinus, as well as the Schneiderian membrane, contained a great number of vital osteocytes within hard and soft tissues [16] showing also potent osteogenic activities [17].
So bone expanders could be used for the creation of a suitable bone defect where a blood clot was formed and replaced by vascularized granulation tissue in a protected bony environment. Moreover, cells much more actively contributed to promoting osseous healing with their regenerative features such as neoangiogenesis and migration of mesenchymal osteoprogenitors[18], especially in the case where defects were surrounded by vital bone on many sides. Previous studies suggested that its particular characteristics made collagen ideal biomaterials for tissue engineering applications not only because of its perfect adaptation to the size of the defect, but also because of haemostatic properties that favored early stages of wound healing, fibroblasts attraction, and semi-permeability allowing nutrients to pass through [19], and initial adhesion and aggregation of platelets leading to a thrombus formation [20]. As previously mentioned, fast and effective achievement of bone regeneration required very close contact between the collagen and walls of bone defect during the onset of the healing process [21].
Some authors had suggested that mineralization of a grafted area within the maxillary sinus after surgery should start very close both to the floor and lateral/medial walls, proceeding from the outside towards the inside (centripetal healing) [22].
In the present study, significant bone gains had been reported for both the first (7.2±0.4 mm) and second surgeries (2.7±0.4 mm) with an overall increase in bone height from the baseline to 5-year of followup of 10.0±0.6 mm. So far, no data were available in the international scientific literature about the employment of double transcrestal sinus lifting particularly in conjunction with the use of collagen as a grafting material. Despite double sinus lift being a modified method of floor augmentation data of the present study seemed to be consistent with previous research describing osteotome sinus floor elevation technique without bone substitutes and immediate implant placement in the atrophic posterior maxilla. Within a few-year period of control after the implant being placed in a residual bone height of 2.4 to 4.6 mm and with an endosinus bone gain from 2.5 mm to 3.9 mm, the clinicians observed substantial shrinkage of the endosinus bone through the presence of implant protrusion into the maxillary sinus [23,24].
That suggested that a double lifting procedure employing collagen as the scaffold material could be efficient when the residual bone height was 3 mm or less. Rosen and co-workers making their final recommendations proposed to optimize the osteotome sinus floor elevation procedure by grafting bone substitutes, especially in areas with at least 5 mm of bone height [25]. The purpose of the first surgery was both to use highly absorbable bone substitute material based on collagen sheet for achieving stable bone recovery over time, and to prevent the implant from bulging into the maxillary sinus; in fact, at 5 years of follow-up a total bone height higher than 10 mm was observed all around the aspect of dental implants. Moreover, a significant difference in length was obtained at the coronal level between the buccal and palatal aspects. This was in large part probably due to the surgical procedure even though, for the moment, the authors did not know why this was.
The use of a space maintainer, as well as a highly resorbable scaffold, resulted in successful tissue regeneration [22,26]; these functions carried out by collagen sponges seemed to be essential because enhanced bone regeneration did not occur with the elevation of the sinus membrane alone and without the tenting effect of the dental implant.
The clinical conditions to achieve long-term success of the “periosteal tunneling” or “pocket” technique with bone substitutes was to create a properly prepared bone base, and maybe even better if bony walls protected it.
Moreover, the cells of regenerated bone were likely to migrate along the direction of the collagen fibers, oriented parallel to the periosteal tent-like surface, and proliferate and mineralize the scaffold [27].
Magnetoelectric devices could transfer energy directly to the bone with pulse pressures just along proper directions and leave intact the other surrounding tissues. It was highly likely that the minimal impacts could promote a faster recovery and reduce the volume of tissue losses during healing. When magnetoelectric surgery was compared with other conventional techniques (such as sonosurgery, piezosurgery, and piezoelectric devices) it should also be noted that the present device produced less heat and required less irrigation of the surgical site [28,29].
Since the present two-stage approach proposed a minimal volume increase at the first step, it could reduce the possibility of sinus membrane perforation (one of the most common postoperative complications of sinus surgery); and, in any case, with a residual bone height from 2 to 4 mm immediate implantation should be used just by short-length implants but not conventional implants had to be placed.
The image processing method could determine an inaccuracy in terms of outcome variables that was difficult to assess, such as the use of software that automatically performed superimposition. However, an estimate of inter- and intra-observer errors in the calculation of bone height, which depended on the level of knowledge of the clinician, was provided. Finally, the specificity of the surgical procedure, a double transcrestal sinus lifting, greatly limited the sample sizes, which led to the use of non-parametric statistical analysis.
Conclusion
Despite these considerations, the present study suggested to clinicians the possibility of osteotome double sinus lifting and grafting with highly absorbable collagen material, generally used as a haemostatic agent alone, in case of residual bone height less than 3 mm, and with delayed tapered implants placed during a secondary sinus lift. In any effort double transcrestal sinus floor elevation could be a very good choice for a less demanding surgery to simplify the rehabilitation process, especially in private practice.
References
- Ohba T, Langlais RP, Morimoto Y, Tanaka T, Hashimoto K. Maxillary sinus floor in edentulous and dentate patients. Indian journal of dental research: official publication of Indian Society for Dental Research. 2001; 12: 121-5.
- Price AM, Nunn M, Oppenheim FG, Dyke TEV. De novo bone formation after the sinus lift procedure. Journal of periodontology. 2011; 82: 1245-1255.
- Tallgren A. The continuing reduction of the residual alveolar ridges in complete denture wearers: A mixed longitudinal study covering 25 years. J Prosthet Dent. 2003; 89: 427-435.
- Tsai C, Pan W, Pan Y, Chan C, Ju Y, Wang Y, et al. Comparison of 4 sinus augmentation techniques for implant placement with residual alveolar bone height ≤3 mm. Medicine. 2020; 99: e23180.
- Nedir R, Bischof M, Vazquez L, Szmukler-Moncler S, Bernard J. Osteotome sinus floor elevation without grafting material: a 1-year prospective pilot study with ITI implants. Clinical oral implants research. 2006; 17: 679-686.
- Winter AA, Pollack AS, Odrich RB. Sinus/alveolar crest tenting (SACT): a new technique for implant placement in atrophic maxillary ridges without bone grafts or membranes. The International journal of periodontics & restorative dentistry. 2003; 23: 557-65.
- Pinchasov G, Juodzbalys G. Graft-Free Sinus Augmentation Procedure: a Literature Review. Journal of Oral & Maxillofacial Research. 2014; 5.
- Szabó G, Suba Z, Hrabák K, Barabás J, Németh Z. Autogenous bone versus beta-tricalcium phosphate graft alone for bilateral sinus elevations (2- and 3-dimensional computed tomographic, histologic, and histomorphometric evaluations): preliminary results. The International journal of oral & maxillofacial implants. 2001; 16: 681-92.
- Palma VC, Magro-Filho O, Oliveria JAD, Lundgren S, Salata LA, Sennerby L. Bone reformation and implant integration following maxillary sinus membrane elevation: an experimental study in primates. Clinical implant dentistry and related research. 2006; 8: 11-24.
- Langer B, Langer L. The superimposed flap: modification of the surgical technique for implant insertion. Int J Periodontics Restorative Dent. 1990; 10: 208-215.
- Crespi R, Capparè P, Gherlone E. Electrical mallet provides essential advantages in maxillary bone condensing. A prospective clinical study. Clinical implant dentistry and related research. 2013; 15: 874-882.
- Crespi R, Fabris GBM, Crespi G, Toti P, Marconcini S, Covani U. Effects of different loading protocols on the bone remodeling volume of immediate maxillary single implants: A 2- to 3-year follow-up. The International journal of oral & maxillofacial implants. 2019; 34: 953-962.
- Lundgren S, Andersson S, Gualini F, Sennerby L. Bone reformation with sinus membrane elevation: a new surgical technique for maxillary sinus floor augmentation. Clinical implant dentistry and related research. 2004; 6: 165- 173.
- Davies JE. Understanding peri-implant endosseous healing. Journal of dental education. 2003; 67: 932-949.
- Falah M, Srouji S. Raised Schneiderian membrane compared with peeled bony walls in the formation of bone. The British journal of oral & maxillofacial surgery. 2016; 54: 115-116.
- Zaffe D, D’Avenia F. A novel bone scraper for intraoral harvesting: a device for filling small bone defects. Clinical oral implants research. 2007; 18: 525- 533.
- Johansson L, Isaksson S, Lindh C, Becktor JP, Sennerby L. Maxillary sinus floor augmentation and simultaneous implant placement using locally harvested autogenous bone chips and bone debris: a prospective clinical study. Journal of oral and maxillofacial surgery: official journal of the American Association of Oral and Maxillofacial Surgeons. 2010; 68: 837-844.
- Carano RAD, Filvaroff EH. Angiogenesis and bone repair. Drug discovery today. 2003; 8: 980-989.
- Schwarz F, Rothamel D, Herten M, Sager M, Becker J. Angiogenesis pattern of native and cross-linked collagen membranes: An immunehistochemical study in the rat. Clin Oral Implants Res. 2006; 17: 403-409.
- Lie N, Merten H, Meyns J, Lethaus B, Wiltfang J, Kessler P. Elevation of the maxillary sinus membrane for de-novo bone formation: First results of a prospective study in humans. Journal of cranio-maxillo-facial surgery : official publication of the European Association for Cranio-Maxillo-Facial Surgery. 2015; 43: 1670-1677.
- Ceccarelli G, Presta R, Benedetti L, Angelis MGCD, Lupi SM, Baena RRY. Emerging Perspectives in Scaffold for Tissue Engineering in Oral Surgery. Stem Cells International. 2017; 2017: 1-11.
- Scala A, Lang NP, Velez JU, Favero R, Bengazi F, Botticelli D. Effects of a collagen membrane positioned between augmentation material and the sinus mucosa in the elevation of the maxillary sinus floor. An experimental study in sheep. Clinical oral implants research. 2016; 27: 1454-1461.
- Nedir R, Nurdin N, Vazquez L, Szmukler-Moncler S, Bischof M, Bernard J. Osteotome sinus floor elevation technique without grafting: a 5-year prospective study. Journal of clinical periodontology. 2010; 37: 1023-1028.
- Si M, Zhuang L, Gu Y, Mo J, Qiao S, Lai H. Osteotome sinus floor elevation with or without grafting: a 3-year randomized controlled clinical trial. Journal of clinical periodontology. 2013; 40: 396-403.
- Rosen PS, Summers R, Mellado JR, Salkin LM, Shanaman RH, Marks MH, et al. The bone-added osteotome sinus floor elevation technique: multicenter retrospective report of consecutively treated patients. The International journal of oral & maxillofacial implants. 1999; 14: 853-8.
- Rong Q, Li X, Chen SL, Zhu SX, Huang DY. Effect of the Schneiderian membrane on the formation of bone after lifting the floor of the maxillary sinus: an experimental study in dogs. The British journal of oral & maxillofacial surgery. 2015; 53: 607-612.
- Chen Y, Zhou S, Li Q. Microstructure design of biodegradable scaffold and its effect on tissue regeneration. Biomaterials. 2011; 32: 5003-5014.
- Heinemann F, Hasan I, Kunert-Keil C, Götz W, Gedrange T, Spassov A, et al. Experimental and histological investigations of the bone using two different oscillating osteotomy techniques compared with conventional rotary osteotomy. Annals of anatomy = Anatomischer Anzeiger : official organ of the Anatomische Gesellschaft. 2012; 194: 165-170.
- Papadimitriou DEV, Geminiani A, Zahavi T, Ercoli C. Sonosurgery for atraumatic tooth extraction: a clinical report. The Journal of prosthetic dentistry. 2012; 108: 339-343.