
Research Article
Austin J Musculoskelet Disord. 2023; 10(1): 1063.
The Butterfly Method for Cervical Movement Sense: Construct Validity and Clinical Applicability
Kristjansson E¹* and Gíslason MK²
¹Landspitali, University Hospital, Reykjavik, Iceland
²Institute for Biomedical and Neural Engineering,Reykjavik University, Iceland
*Corresponding author: Eythor KristjanssonLandspitali, University Hospital, Reykjavik, Vækeröveien 23, 0282 Oslo, Norway, Iceland
Received: December 17, 2022; Accepted: January 25, 2023; Published: January 31, 2023
Abstract
Introduction: The Butterfly Method was developed as there was no objective kinematic assessment and treatment method available at the time to address deficient movement sense in the cervical spine in clinical practice.Recently, two different methods have been introduced using a laser pointer mounted on the head and Virtual Reality (VR) glasses.
Purpose: To describe how incrementally more difficult closed-loop movement patterns were designed and created, based on features in motor control and learning. This is necessary to demonstrate that the outcome measures are logically, as well as theoretically, connected to the construct (content validity). To outline the assessment of the adequacy of the measures, which requires that three essential components to be established: unidimensionality, reliability and validity (construct validity).
Implications: Two studies, using the Butterfly Test, examined two different trajectories of Whiplash-Associated Disorders (WAD) grades I-II, one with mild pain and disability, and the other with moderate pain and disability. The results showed that there was a greater overlap between WAD and an asymptomatic group in the mild pain and disability trajectory, compared with the moderate pain and disability trajectory. The unidimensionality, reliability and discriminant validity of Butterfly Test has been established. The Butterfly Method is fast and easy to use and fits well into busy clinical practices. The outcome report is generated immediately after the test is finished. Patients can train in the Butterfly Exercise Program, while clinicians attend other tasks or train at home or at the office, as the exercise program is available through the Internet.
Keywords: Movement sense; Cervical spine; Neck; Assessment & treatment; Motor control
Introduction
Patients with chronic Neck Pain (NP), especially those with Whiplash-Associated Disorders (WADs), are difficult cases in which the functional joint stability may be compromised by direct damage to the mechanoreceptors and their axons because they have lower tensile strength than the surrounding collagen fibres [43,51]. This may lead to effects similar to those of “deafferentation.” [12] Chemical changes, brought about by ischemic or inflammatory events, may affect the sensitivity of the receptors [29,75] as well as reflex joint inhibition of the muscle spindles [42,81]. Pain [26], maladaptive neural plasticity [9,36] and brain alternations [15,26] have been identified as an important source for deficient motor control of the neck. Altered joint biomechanics, irrespective of the reasons, also causes different mechanoreceptors to fire too late or too early, too little or too much [13,71]. Patients who are affected by these conditions are unlikely to respond to conventional physical therapy approaches alone [35]. The consequent faulty recruitment muscle patterns result in the underestimation or overestimation of the movement situation, making the soft tissue liable to repeated microtrauma [7,24,25]. This may cause uncertainty for the person and increased muscular guarding [7,8]. This is thought to be an important factor in the maintenance, recurrence or progression of local and referred symptoms [17,25,38,39,71]. Identifying and resolving deficient cervical proprioception is therefore thought to be an important key in preventing ongoing symptoms [33,60].
Movement Sense
Deficient cervical movement sense has been researched to a much lesser extent than cervical position sense. A few systematic reviews have been conducted on Joint Position Sense Error (JPSE) with no uniform conclusions [18,19,41]. Higher (worse) score on JPSE test has been found in NP compared to controls and WAD versus controls [18,41]. Whether patients with WAD score higher than non-traumatic remain inconclusive [18]. Recently, two different methods have been introduced to test and treat deficient cervical movement sense in clinical practice, using a laser pointer mounted on the head and Virtual Reality (VR) glasses. In the laser beam method, the patient is required to trace a Zig-Zag (ZZ) pattern and a figure of eight (F8) pattern on the wall [21,61,80]. The task was to follow the target line (1mm,) as accurate as possible at a self-chosen speed with controlled head movements. The examiner determines visually the number of errors and time taken to perform the task or the performance was video-recorded for later automated image analysis for the extraction of outcome measures of the performance [21,61,74,80]. The VR method has three test modules. In the accuracy module, a moving yellow target is presented on a vertical or horizontal line, at a constant velocity of 10°/sec [62]. The participant is required to maintain the pilot’s head (the curser) on the moving target as closely as possible by tracing vertical/horizontal lines [63]. Research comparing the laser beam method (low tech) and the accuracy module in the VR system (high tech) concluded that both tools differentiated individuals with NP from controls with similar sensitivity and specificity, with some advantage to the VR [64].
The Butterfly Method
An important function of the proprioceptive system in neuromuscular control is to correct movement on a moment-to-moment basis [23]. This is especially so when non-learned complex movements are performed [6,50]. Therefore, “the Fly” was developed tracing slow, unpredictable movement patterns of short duration according to different theories about motor control, such as reflex, hierarchical, and system theories [5,14,40,46,48]. The test results indicated that the test was valid and capable of discriminating the accuracy of neck movements in women with WAD from asymptomatic women [32,49]. The main drawback of the original Fly Test was that no attempt was made to generate incrementally difficult sets of movement patterns to precisely grade the level of impairment for each individual. In order to increase the diagnostic utility of the test, further development was necessary, as were further studies on reliability and validity of the test. This was accomplished through a PhD project [54] and publications of articles [34,52,53,55]. A systematic review focusing on measuring methods and their clinimetric characteristics concluded that only thedynamic method The Fly appears to be morereliable than the JPSE test and is able to discriminate between different patient populations i.e., post-traumatic and non-traumatic neck pain [47]. Later, the name was changed to Butterfly Method as some found the Fly moving on the screen to be disgusting.
The Butterfly Method is essentially a computerized clinical assessment and treatment method for deficits of movement control in the cervical spine. The method consists of a softwaresuite in conjunction with an Inertial Measurement Unit (IMU) sensor. The sensor is placed on the subject’s head with a headgear to capture the 3D angles of the head and neck movements. A cursor appears on the screen, which indicates the position of the subject’s head, then the target (red dot) appears on the screen and starts to move. The subject is required to trace the target with the cursor (UMI sensor) upon the head as accurately as possible. The patterns of the cursor and target were represented in a 2D coordinate system. The patterns are defined in a standardized 100 x 100 coordinate system which is then normalized so it is independent of the resolution of the computer monitor used to display them.
The Butterfly Test
The target on the screen traces easy, medium and difficult unpredictable movement patterns, each of which are repeated three times in random order. The instruction to the patient is “do your best”. To familiarize the patient with the test procedure, one pre-test movement pattern is traced once. The Butterfly Test, measures the patient´s ability to correct cervical spine movements in real–time. The software program processes the data for 2D analysis of cervical spine movements. The results are downloaded into a report. The following three outcome measures are calculated, each of which represent three different percepts of proprioception. Amplitude Accuracy (AA) is indicated by mean deviations of movements in millimetres ±2 SD and represents how far in total the subject was away from the target. Directional Accuracy (DA), or time on target (ToT), undershoots (U) versus overshoots (O) are each indicated as a percentage (%) ±2 SD of the total time used to perform the trial. Jerk Index (JI) calculates the smoothness of movement by a unit less index from 0-5.
The Butterfly Exercise Program
The treatment part of the Butterfly Method isessentially a new computer-generated exercise program, designed to improve coordination of cervical spine movements. The patient is asked to trace incremental difficult movement patterns. For that purpose, the exercise program contains three classes of movement patterns: easy, medium, and difficult.
One or more of the following variables can be chosen as an extra option to make an exercise trial easier or more difficult within each class: The size of the pattern (5 sizes); The velocity (5 velocities); Target size (3); quadrant (4) i.e., the pattern can be moved on the screen to the one quarter of movement in which the patient has most deficient movement sense. For those who are most severely affected, the patterns can be made predictable, in the start of a treatment. When the patient clicks the "Get Patterns" button, 9 exercise patterns within the same class are displayed in random order on the screen, which make up one treatment session.
Feedback during and after an exercise trial is an essential part of the Butterfly Exercise Program. The following feedback is given:
Results of performance: The patient is given constant feedback while performing the exercise trial. The cursor changes colour according to how close or far the cursor is in relation to the tracing dot: when the dot and the cursor are in close approximation the cursor is green; when the cursor is behind or ahead of the dot, the cursor is yellow or red respectively. This feedback indicates the directional accuracy of the cervical spine movements.
Results of outcome: The results of outcome on completion of the test are shown in two ways for the patient: Firstly, by displaying a column, which indicates in percentages a) the time on target, b) the time behind target or undershoots, and c) the time ahead of target or overshoots (Figure 5). Secondly, the trajectory of the dot pattern and the pattern traced by the patient is displayed graphically after the exercise trial is finished to visually express the patient’s amplitude accuracy (Figure 3).
After one or two weeks with daily or every other day, 5-15 minutes of training, re-assessment is performed, which will decide whether the patient can start on a more difficult stage in the exercise program.Clinicians have to rely on their own reasoning skills when to decide to use the Butterfly Method. It is not recommended for patients complaining about severe dizziness or vertigo and severe visual disturbances as well as nausea. In more severe cases, it is recommended to adjust the exercise program by using small amplitude, low velocity, bigger target, and predictable movement pattern, preferably in the easy class. The set-up is shown in (Figure 2).
How was the Butterfly Method Designed?
Almost infinite patterns can be generated at each class: easy – medium – difficult in the Pattern Generation Software Program according to theories and principles in motor control and learning (Patent N0:US 9,757,055B2: Method for accurate assessment and graded training of sensorimotor functions). How the patterns were generated will be presented here. The boundaries between each of the three classes of patterns were composed of different relationships between number and acuity of the bends, the shape and length of the patterns, velocity and relationship between acceleration-deceleration [54]. Allnormal human movements are performed rhythmically with certain number of beats [67]. For the freely moving cervical spine the number of movement segments resembles the grammar of conducting an orchestra with certain number of beats [59]. Therefore, 3 – 4 – 6 beats for the easy, medium and difficult patterns, were implemented, respectively. The length of the patterns is therefore progressively increased (Figure 1). The velocity of the Butterfly is slow but subject to changes throughout each pattern. On the straighter parts, acceleration-deceleration is induced in a random order. The velocity in the bends obeys the 2/3 Power Law [16,30,37,77,78]. Basically the robust 2/3 Power Law states that the instantaneous velocity is lower in the more curved parts than in less curved parts of the bends. Most importantly, subjects cannot track a target motion accurately when it deviates from the 2/3 Power Law [22].
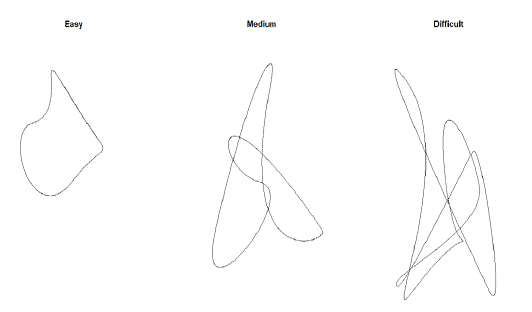
Figure 1: Test patterns (hidden) in the Butterfly Test. From left to right, Easy – Medium – Difficult. The duration is 25, 40, 50 seconds, respectively.

Figure 2: Set-Up. The centre of the monitor was placed at eye level and the subject sat 100 cm away from the monitor.
What is the Main Motor Control Features?
Aiming movements are composed of an initial impulse phase (feed-forward) and a current (feedback) control phase [20]. The initial impulse is hypothesized to be under central control and designed to bring the head into the vicinity of the target [20]. Once in the region of the target, the head-neck comes under feedback-based control. In this second “homing” phase, visual information about the relative positions of the head and target is used to make any adjustments to the movement pattern, necessary to bring the head to rest on the target [20,65,66,79]. These adjustments can take the form of corrections (submovements) such as discrete antagonist activity during deceleration or graded modulation of the muscular forces used to propel and/or brake the movement assisted by inertia in slow movements [10]. After the initial impulse phase, asymptomatic subjects tend to stop short of target i.e., undershoot [20]. Therefore a cone-shaped "free zone" was created in the Butterfly software around the target with the tail directed towards undershoots. The subject is deemed to be on target once within the "free zone".
An irregular and unfamiliar movement pattern is less predictable (pre-programmed and hidden in the software) and increases the difficulty of following the pattern accurately [20]. One strategy researchers have used to dissociate prior planning processes from on-line (feedback) control has been to unexpectedly change the movement requirements (acceleration-deceleration – different acuity in the bends), forcing the system to adjust to new requirements [82]. By introducing unexpected changes, any positive feedforward contribution to head-neck control can be eliminated in an attempt to examine the limits of the corrective (feedback) process [20,82].
The excursion of the pattern must not be too large to properly stimulate the mechanoreceptors that give rise to proprioception [58]. According to the ensemble coding theory, which holds that the sensory information created by all the mechanoreceptors that are active during a specific motor control performance is transmitted to the CNS in population codes [69]. This implies that ascribing a specific mechanoreceptor function to a particular motor control function is not relevant [69]. Research indicates that the muscle spindle afferents play the first violin in this ensemble but that other mechanoreceptors act to fine tune the afferent muscle spindle information by their reflex effects on the γ-motoneurones [4,69]. It seems that attenuation of muscular sense is most evident during large, rapid movements but in tasks requiring fine manipulation involving small, slow movements, muscular sense probably remains closer to static control levels [14].
When the shape of the pattern has bends of various degree it demands more precision in the tracking movement. Depending on the level of the curvature (acuity), undershoots or overshoots tend to take place when the direction of movement is reversed [20]. The strategy to undershoot the target with the initial impulse makes sense because it is more economical, in the terms of energy and time, to correct a movement that falls short of the target than to correct an overshoot [20]. From a processing point of view, the reversal in direction required by a target overshoot entails a change in the role of the muscles driving the movement; that is, the agonist muscles for the initial impulse become the antagonist muscles for the reversal and vice versa [20]. In this context, reversal movements have been shown to be more attention and energy demanding than extensions to an ongoing movement made in the same direction (undershoots) [79].
When accuracy in following a moving target is demanded it has been shown that more time is used in the deceleration phase [1]. Similarly, when more precision is demanded, the resulting movements are characterized by disproportionally larger deceleration than acceleration phases and by slower movement [2,3]. It has been suggested that this strategy may allow feedback information concerning endpoint accuracy to be monitored and used for adjustments of movements in order to optimize their accuracy [1]. In accordance, adding variable speed into the pattern, that would require deceleration – slowing down phase, can be used to increase the difficulty of the task. In the software the patterns are “closed” and time limited, therefore a less time is available for the deceleration phase, thus increasing the difficulty [28].
Features of the Three Outcome Measures
Amplitude Accuracy (AA)
(Figure 3) shows an example of individual AA performances.
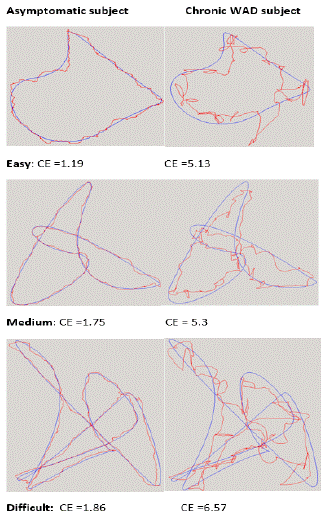
Figure 3: Example of the Amplitude Accuracy performances in the Butterfly Test for two single subjects. CE = constant error. A blue colour represents the path traced by the patient and a red colour represents the pattern traced by the dot.
(Figure 4) shows that the patients with WAD, grade I-II, performed consistently worse for AA than the asymptomatic group in certain regions of the test patterns. Regions of interest (RoI) were identified.
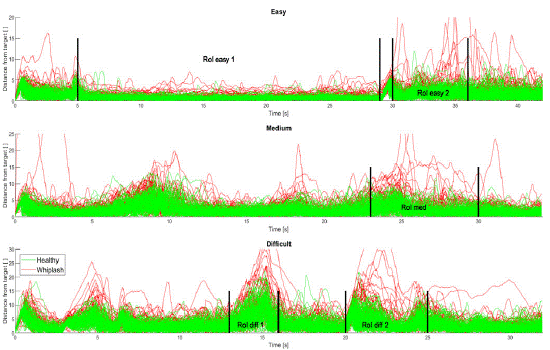
Figure 4: Distance between the cursor and the target in Amplitude Accuracy, as a function of time for all subjects and all patterns. Regions of Interest (RoI) have been defined for each pattern.
Directional Accuracy (DA) (Time on Target – Undershoots – Overshoots)
The best performance in the DA parameter is to spend as much time as possible on the target i.e., the Time-on Target (ToT) variable. Figure 5 shows the proportion of time spend on the target, behind the target or undershoots and ahead of target or overshoots. The ToT variable is most often used as an indicator when to change the difficulty level in the Butterfly Exercise Program. When ToT reaches 50% or more of the total time used to perform a trial, the exercise program can be made more difficult by using the variables within each level of difficulty. Overshoots are the worst outcome in DA as explained earlier.
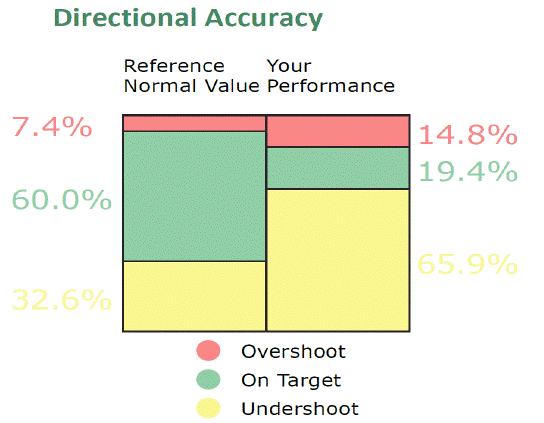
Figure 5: The column shows in percentage (%) the total time used to perform the trial for each measure within directional accuracy: time on target (green colour); undershoots (yellow colour); overshoots (red colour).
(Figure 6) shows that the velocity distribution is in line with the motor control features about deceleration – acceleration, as the velocity is higher, but variable, in the straighter parts and slower, but variable, in the bends. The easy pattern (3 beats) shows the most uniform velocity, as the bends are wider, whereas the difficult pattern has a wide range of velocities. For the difficult pattern (6 beats) it can be seen how the target moves faster on the straighter segments and decelerates when reaching the bends. Mean angular velocity of the head as a function of time is 1.8°/s for the easy pattern, 2.32°/sec for the medium pattern and 3.67°/sec for the difficult pattern. Research indicates that when participants move their heads faster than 2.1°/s, cervical input decreases and vestibular input increases [31]. Thus, the faster the head moves, the more vestibular afferention rather than cervical afferention is induced [45].
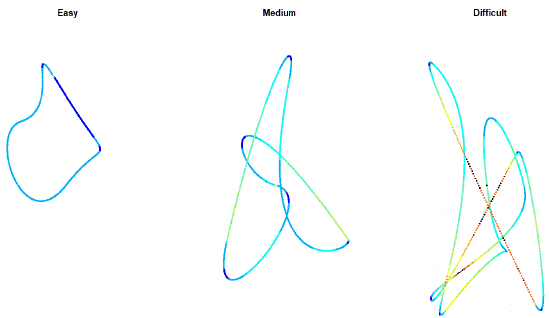
Figure 6: Velocity distribution on the patterns. Blue colours indicate slow velocities, yellow coloursindicate intermediate velocity, and red colours indicate high velocities.
Jerk Index
Jerk, i.e. smoothness of movement, was calculated and represented by an index (JI) normalized by the smoothness of the path of the dot itself. This was done by calculating the third derivative of the two-dimensional position data x(t) and y(t) and integrating the quadratic sum over time, using the equation based on the works of [73] Teulings et al., The baseline measure for the unitless Jerk Index, is 2.0, which was decided by measuring a group of asymptomatic soccer players.
Three Different Pain and Disability Trajectories in Wad
The Neck Disability Index (NDI) has been found to have different trajectories: 0-8% is no pain and disability. 10-28% is mild pain and disability (45%) – 30-48% is moderate pain and disability (39%) – 50-68% is severe pain and disability (16%) – > 70% is complete disability.70,76The numbers in parentheses are suggested percentage of the whole WAD population [70].
Mild Pain and Disability Trajectory
The Butterfly Test has been used to measure cervical movement sense in a group of WAD, grades I-II, (n=22) compared with asymptomatic subjects (n=42) (unpublished data). (Figure 7) shows the distribution of the measurements for AA for both groups and the three patterns. The WAD group shows a skewed distribution towards the higher values of the AA, whereas there exists a region in which the results overlap between the groups. By looking at the patient group, it was seen that some patients with mild WAD, grades I-II, manage to score in the Butterfly Test that is partial within the asymptomatic range. The AA results for the asymptomatic group are in the range with the findings of Oddsdottir et al [53].
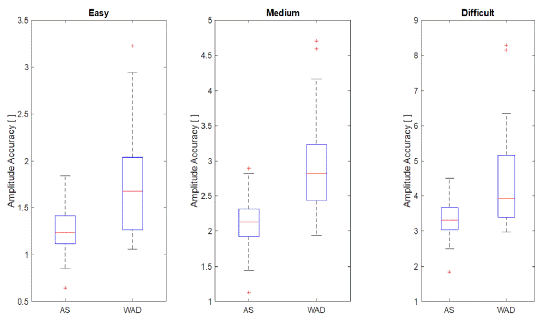
Figure 7: Boxplot distributions for Amplitude Accuracy between groups and patterns. AS: Asymptomatic. WAD: Whiplash Associated Disorders.
Moderate Pain and Disability Trajectory
The Butterfly Test (Fly Test) has been found to be reliable and valid method for a group of chronic WAD grade I-II, with moderate pain and disability. The study compared an asymptomatic group (n=18) with a group of chronic non-traumatic neck pain (n=18) and chronic WAD, grade I-II (n=18) [34]. Comparing the asymptomatic group and the chronic WAD group, grades I-II, could distinguish between the two groups by Receiver Operating Characteristic (ROC) curve (Figure 8). The Area Under the Curve (AUC) for easy, medium, and difficult patterns was 0.81, 0.85, and 0.85, respectively, for AA and 0.79, 0.84, and 0.85, respectively, for ToT. Table 1 shows the sensitivity and specificity with 95% confidence interval (CI) [54].
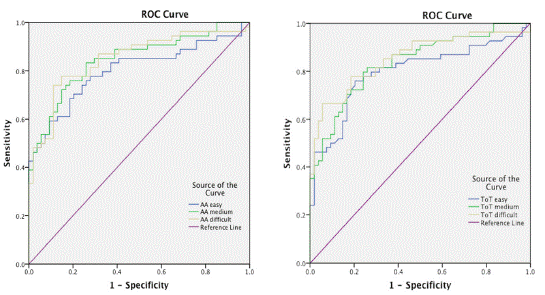
Figure 8: Receiver operating characteristic (ROC) curve for amplitude accuracy (AA) on the left and time-on-target (ToT) on the right, revealing how well the parameters can distinguish between the two groups, WAD and asymptomatic control.
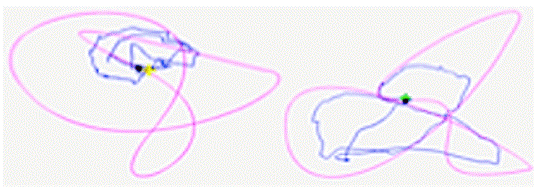
Figure 9: Performances of a patient with WAD, grade II, and severe pain and disability. Two movement patterns in pink (performances in blue). On the left the patient’s shoulders are held still. On the right, the patient is allowed to support her head with the hands. Her performance in AA was recorded as following on the right: easy pattern = 5.77 mm (4.74); medium = 5.85 mm (4.75); difficult =7.73 mm (6.84).
AA
AS vs. WAD
Sensitivity
89.7% (76.4–95.9)
Specificity
72.4% (61–81.6)
Positive Predictive Value
0.648 (0.51–0.76)
Negative Predictive Value
0,926 (0.82–0.97)
Likelihood Ratio +
3.259 (2.19–4.85)
Likelihood Ratio -
0.142 (0.01–0.36)
DA ToT
AS vs WAD
Sensitivity
74% (61–83.4)
Specificity
76.4% (63.2–86)
Positive Predictive Value
0.778 (0.65–0.87)
Negative Predictive Value
0.722 (0.59–0.82)
Likelihood Ratio +
3.132 (1.86–5.26)
Likelihood Ratio -
0.344 (0.22–0.54)
Table 1: Sensitivity-specificity (95% CI) – ROC-Curves.
Severe Pain and Disability Trajectory
No group comparison exists for thistrajectory, but a bunch of individual performances.
Discussion
Construct validity is about how well a test measures the concept it was designed to evaluate (e.g., cervical movement sense). It’s crucial to establishing the overall validity of a method [56]. The laser beam method [80] and the VR method [62] introduced to be used in a clinical setting may not just use perceptual feedbackrelying on proprioception but vestibular afferention and pre-programmed movements.Well learned simple movements and commonly performed tasks have less need for sensory input to correct the path [50,66]. When establishing construct validity, unidimensionality is of concern [56]. Unidimensionality involves establishing that a set of outcome measures relates to one and only one construct [56]. When a measure of one variable improperly includes empirical indicators that are related to another variable, we are in a sense combining two variables A and B to form a new variable C [56]. Treatment of multidimensional measures as if they were unidimensional can lead to false conclusions [56]. Serious problems arise regarding the interpretation of association between C and other variables, in that it is impossible to determine whether the association is a function of the underlying variable A and/or B [56]. This obviously has the potential to create false associations between two variables and therefore taint the findings of a study [56].
In the VR method, it can be argued that: 1). the target moves too fast; 2). the velocity is not variable, not challenging directional accuracy; 3). movements along straight lines are predictable. Therefore, the VR accuracy assessment doesn’t challenge neck proprioception but relays more on vestibular afferention [46,72]. However, the VR system is highly relevant in assessment and treatment of quick responses to external stimuli [62] and should be implemented after proper proprioceptive training. Dynamic variables in VR, such as velocity, smoothness, symmetry and accuracy reflect functional cervical motions [63]. In the laser beam method,it can be argued that tracing predictable ZZ and F8 patterns does not challenge neck proprioception in ways as the Butterfly Method does. The F8 and ZZ patterns do not follow the laws and principles about motor control theories. Firstly, the patterns are not rythmatic and have no beat. Secondly, because of the plasticity in the CNS, a simple and predictable pattern is learned quickly and the tracking task can be performed without relying on the proprioceptive information [28]. Thirdly, the velocity is not variable, not allowing deceleration-acceleration to occur in a controlled manner to measure directional accuracy. Fourthly, smoothness of movement is not accounted for, which is an important measure, especially in more severe cases. The authors admit that the video processing used with the custom-made software was rather time-consuming and needs skills in Matlab. [61] In a busy clinical setting, it is essential to generate the report, right at the fingertips, as in the Butterfly Test.
The F8 and ZZ patterns are not suited for treatment due to the aforementioned flaws and learning effects [28,45,50,68,72]. It is important when learning new skills that the task difficulty is adjustable to the individual's skill level, to ensure that the task is neither too difficult nor too easy. Motor learning is a complex process, and some of its complexities have been conceptualized in the challenge point framework theory [27]. The optimal challenge point represents the degree of task difficulty needed for an individual of specific skill level to optimize learning. By adjusting the task difficulty to the change in ability, the optimal challenge point is maintained [27]. The Butterfly Exercise Programfulfils these requirements, as the difficulty level can be adjusted (within and between classes) according to each patient’s capability. Evidence has shown that proprioceptive training is associated with reorganization within the sensorimotor cortex [2]. Previous studies indicate that sensorimotor exercises may reverse the pain induced cortical changes to a normal level based on the plasticity property of the nervous system [9,15,48]. The Butterfly Exercise Program is available over the Internet and can be used by patients at home or at the office, ensuring enough dosage to achieve neural changes.
Meisingset et al., tried to replicate the Butterfly Test by drawing the patterns on a paper, not taken into account the principles of motor control behind the generation of the patterns [44]. In addition, quite different set-up was used: standing 2.5 m from the patterns; two different pattern sizes; one repetition for healthy, two repetions for symptomatic; The same time duration (30 sec) to complete both the medium and difficult tasks; Researchers should use our original methodology when assessing and treating deficient movement control of the cervical spine.
It seems apparent that there is a need for specificity when prescribing therapeutic exercises in the management of sensorimotor disturbances in people with neck pain.In chronic cases, signs and symptoms of injury may abate, but the functional deficits persist and adaptive patterns develop secondary to the remaining functional deficits. This may be one important reason for recurrent neck pain, which is a major feature characterizing people with WAD [11].
Conflict of Interests
Dr. Kristjansson is the inventor of the Butterfly Method.
References
- Adam J. The effects of objectives and constraints on motor control strategy in reciprocal aiming movements. J Mot Behav. 1992; 24:173-185.
- Aman JE, Elangovan N, Yeh IL, Konczak J. The effectiveness of proprioceptive training for improving motor function: a systematic review. Front. Hum. Neurosci. 2014; 8:1075.
- Adamovich S, Berkinblit MB, Fookson O, Poizner H. Pointing in 3D space to remembered targets II. Effects of movement speed toward kinesthetically defined targets. Exp Brain Res. 1999; 125: 200-210.
- Bergenheim M, Ribot-Ciscar E, Roll JP. Proprioceptive population coding of two-dimensional limb movements in humans: I.Muscle spindle feedback during spatially oriented movements. Exp Brain Res. 2000; 134: 301-310.
- Bernstein N. The coordination and regulation of movement. London: Pergamon Press; 1967.
- Bizzi E, Hogan N, Mussa-Ivaldi FA, Giszter S. Does the nervous system use equilibrium-point control to guide single and multiple joints movements. Behav Brain Sci. 1992; 15:603-13.
- Bojsen-Møller F. Belastning af bevægeapparatet – om tolerans og præstation og deres tidsafhængighed. Månedsskr Prakt Lægegern. 1991; 69: 851–858.
- Bojsen-Møller F. Stræk og udspænding. In: Lund H ed, Muskel & Skelet Funktionen. Skodsborg Fysioterapiskole, Denmark 1998.
- Bonanni R, Cariati I, Tancredi V, Iundusi R, Gasbarra E, Tarantino U. Chronic pain in musculoskeletal diseases: do you know your enemy? J. Clin. Med. 2022; 11: 2609.
- Brebner J. Continuing and reversing the direction of responding movements: some exceptions to the so-called psychological refractory period. J Exp Psychol. 1968; 78: 120-127.
- Carroll L, Holm L, Hogg-Johnson S, et al., Course and Prognostic Factors for Neck Pain in Whiplash-Associated Disorders (WAD): Results of the Bone and Joint Decade 2000–2010 Task Force on Neck Pain and its Associated Disorders. Spine. 2008; 33: 583–592.
- Caulfield B. Functional Instability of the Ankle Joint: Features and underlying causes. Physiother. 2000; 86: 401-411.
- Cole KJ, Daley BJ, Brand RA. The sensitivity of joint afferents to knee translation. Sportverl Sportschad. 1996; 10: 27–31.
- Collins D, Cameron T, Gillard DM, Prochazka. Muscular sense is attenuated when humans move. J Physiol. 1998; 508: 635-643.
- DePauw R, Coppieters I, Meeus M, Caeyenberghs K, Danneels L, Cagnie B. Is traumatic and non-traumatic neck pain associated with brain alterations? - a systematic review. Pain Phys. 2017; 20: 245–260.
- de’Sperati C, Viviani P. The Relationship between Curvature and Velocity in Two-Dimensional Smooth Pursuit Eye Movements. J Neurosci. 1997; 17: 3932-3945.
- Deusinger RH. Biomechanics in clinical practice. Phys Ther 1984; 64: 1860–1868.
- de Vries J, Ischebeck BK, Voogt LP, van der Geest JN, Janssen M, Frens MA, et al. Joint position sense error in people with neck pain: a systematic review. Man Ther. 2015; 20; 736–744.
- de Zoete RMJ, Osmotherly PG, Rivett DA, Farrell SF, Snodgrass SJ. Sensorimotor control in individuals with idiopathic neck pain and healthy individuals: a systematic review and meta-analysis. Arch. Phys. Med. Rehabil. 2017; 98: 1257–1271.
- Elliott D, Helsen W, Chua R. A Century Later: Woodworth´s (1899) Two-Component Model of Goal-Directed Aiming. Psychol Bull. 2001; 127: 342-357.
- Ernst MJ, Williams L, Werner IM, Crawford RJ, Treleaven J. Clinical assessment of cervical movement sense in those with neck pain compared to asymptomatic individuals. Musculoskel Sci Pract. 2019; 43: 64-69.
- Flach R, Knoblich G, Prinz W. The two-thirds law in motion perception.Visual Cognition. 2004; 11: 461-481.
- Gandevia SC, Burke D. Does the nervous system depend on kinesthetic information to control natural limb movements? Behav Brain Sci. 1992; 15; 614-632.
- Gardner-Morse M, Stokes IAF, Lauble JP. Role of the muscles in lumbar spine stability in maximum extension efforts. J Orthop Res. 1995; 13: 802–808.
- Glencross D, Thornton E. Position sense following joint injury. J Sports Med. 1981; 21: 23–27.
- Giannoni-Luza S, Pacheco-Barrios K, Cardenas-Rojas A, Mejia-Pando PF, Luna-Cuadros MA, et al. Noninvasive motor cortex stimulation effects on quantitative sensory testing in healthy and chronic pain subjects: a systematic review and meta-analysis. Pain. 2020; 161: 1955–1975.
- Guadagnoli MA, Lee TD. Challenge Point: A Framework for Conceptualizing the Effects of Various Practice Conditions in Motor Learning. J Mot Behav. 2004; 36: 212-224.
- Jaric S, Corcos DM, Gottlieb GL, Ilic DB, Latash. The effects of practice on movement distance and final position reproduction: implications for the equilibrium-point control of movements.Exp Brain Res. 1994; 100: 353-359.
- Johansson H, Djupsjöbacka M, Sjölander P. Influences on γ muscle spindle system from muscle afferents stimulated by KCI and lactic acid. Neurosci Res 1993; 16: 49–57.
- Karklinsky M, Flash T. Timing of continuous motor imagery: the two-thirds power law originates in trajectory planning. J Neurophysiol. 2015; 113: 2490-2499.
- Kelders WPA, Kleinrensink GJ, van der Geest JN, Feenstra CI, Zeeuw I de, et al. Compensatory increase of the cervico-ocular reflex with age in healthy humans. J Physiol. 2003; 553: 311-317.
- Kristjansson E, Hardardottir L, Asmundardottir M, Guðmundsson K. A new clinical test for cervicocephalic kinesthetic sensibility: “The Fly”. Arch Phys Med Rehab. 2004; 85: 490-495.
- Kristjansson E, Treleaven J. Sensorimotor Function and Dizziness in Neck Pain: Implications for Assessment and Management. J Orthop Sports Phys Ther. 2009; 39: 364-77.
- Kristjansson E, Oddsdottir GL. The Fly: A new clinical assessment and treatment method for deficits of movement control in the cervical spine: reliability and validity. Spine. 2010; 35: E1298-1305.
- Kristjansson E, Björnsdottir SV, Oddsdottir GL. The long-term course of deficient cervical kinaesthesia following a whiplash injury has a tendency to seek a physiological homeostasis. a prospective study. Man Ther. 2016; 22: 196–201.
- Kuner R, Flor H. Structural plasticity and reorganisation in chronic pain. Nat Rev Neurosci. 2017; 18:113.
- Lacquaniti F, Terzuolo C, Viviani P. The law relating the kinematic and figural aspects of drawing movements. Acta Pcychol (Amst). 1983; 54:115-30.
- Laskowski ER, Newcomer-Aney K, Smith J. Refining rehabilitation with proprioception training. Phys Sportsmed. 1997; 25: 89–102.
- Lephart SM, Pincivero DM, Giraldo JL, Fu FH. The role of proprioception in the management and rehabilitation of athletic injuries. Am J Sports Med. 1997; 25: 130–137.
- Loeb GE, Brown IE, Cheng EJ. A hierarchical foundation for models of sensorimotor control. Exp Brain Res. 1999; 126: 1-18.
- Mazaheri M, Abichandani D, Kingma I, Treleaven J, Falla D. A meta-analysis and systematic review of changes in joint position sense and static standing balance in patients with whiplash-associated disorder. PLoS One. 2021; 16: e0249659.
- McGrea DA. Spinal cord circuitry and motor reflexes. Exerc Sport Sci Rev. 1986; 14: 105–141.
- McLain RF. Mechanoreceptor endings in cervical facet joints. Spine. 1994; 19: 495–501.
- Meisingset I, Woodhouse A, Stensdotter A-K, Stavdotter K, Stavdahl O, et al. Evidence for a general stiffening motor controlpattern in neck pain: a cross sectional study. BMC Musculoskel Disord. 2015; 16: 56.
- Mergner T, Nardi G, Becker W, Deecke L. The role of the canal-neck interaction for perception of horizontal trunk and head rotation. Exp Brain Res. 1983; 49: 198-298.
- Mergner T, Rosemeier T. Interaction of vestibular, somatosensory and visual signals for postural control and motion perception under terrestrial and microgravity conditions—a conceptual model. Brain Res Rev. 1998; 28: 118-35.
- Michiels S, De Hertogh W, Truijen S. et al., The assessment of cervical sensory motor control: a systematic review focusing on measuring methods and their clinimetric characteristics. Gait & Posture. 2013; 38: 1-7.
- Moseley GL, Flor H. Targeting cortical representations in the treatment of chronic pain: a review. Neurorehabil Neural Repair. 2012; 26: 646–652.
- Nordin M, Carragee EJ, Hogg-Johnson S, Weiner SS, Hurwitz EL, Peloso PM, et al. Assessment of neck pain and its Associated Disorders: Results of the Bone and Joint Decade 2000-2010 Task Force on Neck Pain and Its Associated Disorders. Spine (Phila Pa 1976). 2008; 33: S101-122.
- Nougier V, Bard C, Fleury M. et al. Control of single-joint movements in deafferented patients: evidence for amplitude coding rather than position control. Exp Brain Res. 1996. 109: 473-482.
- O’Conner BL, Densie VM, Brandt KD, Myres SL, Kalasinski LA. Neurogenic acceleration of osteoarthrosis. The effects of previous neurectomy of the articular nerves on the development of osteoarthrosis after transection of the anterior cruciate ligament in dogs. J Bone Joint Surg. 1992; 74-A: 367–376.
- Oddsdottir GL, Kristjansson E. Two different courses of impaired cervical kinaesthesia following a whiplash injury. A one-year prospective study. Man Ther. 2012; 17: 60-65.
- Oddsdottir GL, Kristjansson E, Gislason MK. Database of movement control in the cervical spine. Reference normal of 182 asymptomatic persons. Man Ther. 2013; 18: 206-210.
- Oddsdottir GL. Motor Control of the Cervical Spine: The Fly as a new objective assessment and treatment method for whiplash-associated disorders[PhD thesis]. Reykjavik, Iceland: University of Iceland; 2014.
- Oddsdottir GL, Kristjansson E, Gislason MK. Sincerity of effort versus feigned movement control of the cervical spine in patients with whiplash-associated disorder and asymptomatic persons: A case-control study. Physiother Theory Pract. 2015; 31: 403–409.
- O’Leary-Kelly SW, Vokurka RJ. The empirical assessment of construct validity. JOM. 1998; 16; 1998 387–405.
- Riemann BL, Lephart SM. The sensorimotor system, part I: the physiologic basis of functional joint stability. J Athl Train. 2002; 37: 71–79.
- Rowinski MJ. Afferent neurobiology of the joint. In: Gould JE (ed) Orthopaedic and Sports Physical Therapy. Mosby, St. Louis, 1990.
- Rudolf M. The Grammar of Conducting: A Practical Guide to Baton Technique and Orchestral Interpretation. 2nd ed. Schirmer Books, New York; 1980.
- Röijezon U, Clark NC, Treleaven J. Proprioception in musculoskeletal rehabilitation. Part 1: basic science and principles of assessment and clinical interventions. Man Ther. 2015; 20: 368–377.
- Röijezon U, Jull G, Blandford C, Daniels A, Michaelson P, Karvelis P, et al. Proprioceptive Disturbance in Chronic Neck Pain: Discriminate Validity and Reliability of Performance of the Clinical Cervical MovementSense Test. Front Pain Res. 2022; 3: 908414.
- Sarig Bahat H, Chen X, Reznik D, Kodesh E, Treleaven J. Interactive cervical motion kinematics: Sensitivity, specificity and clinically significant values for identifying kinematic impairments in patients with chronic neck pain. Man Ther. 2015; 20: 295-302.
- Sarig Bahat H, Kate Croft K, Carter C, Hoddinott A, Sprecher E, et al. Remote kinematic training for patients with chronic neck pain: a randomised controlled trial. Eur Spine J. 2018; 27: 1309-1323.
- Sarig Bahat H, Watt P, Rhodes M, Hadar D, Treleaven J, et al. High-vs. low-tech cervical movement sense measurement in individuals with neck pain. Musculoskelet Sci Pract. 2020; 45: 102097.
- Schmidt R, Lee T. Motor learning concepts and research methods. In: Motor control and learning. A behavioral emphasis. 4th ed. Champaign, IL.: Human Kinetics Publishers Inc. 2005: 301-320.
- Selen L, van Dieén J, Beek P. Impedance Modulation and Feedback Corrections in Tracking Targets of Variable Size and Frequency. J Neurophysiol. 2006; 96: 2750-2759.
- Shumway-Cook A. Motor Control. Theory and Practical Applications. Lippincott Williams & Wilkins. 2001.
- Shumway-Cook A, Woollacott MH, Rachwani J, Santamaria V. Motor Control: Translating Research into Clinical Practice. 6th North American ed. Lippincott Williams & Wilkins. 2022.
- Sjölander P, Johansson H, Djupsjöbacka M. Spinal and supraspinal effects of activity in ligament afferents. J Electromyogr Kinesiol. 2002; 12:167-176.
- Sterling M, Hendrikz J, Kenardy J. Compensation claim lodgement and health outcome developmental trajectories following whiplash injury: A prospective study. Pain. 2010; 150: 22-28.
- Suter E, Hertzog W. Does muscle inhibition after knee injury increase the risk of osteoarthrítis? Exerc Sport Sci Rev. 2000; 28: 15–28.
- Taylor JL, McCloskey DI. Proprioception in the neck. Exp Brain Res. 1988; 70: 351-360.
- Teulings HL, Contreras-Vidal JL, Stelmach GE, Adler CH. Parkinsonism reduces coordination of fingers, wrist, and arm in fine motor control. Exp Neurol. 1997; 146: 159-170.
- Treleaven J, Dillon M, Fitzgerald C, Smith C, Wright B, et al. Change in a clinical measure of cervical movement sense following four weeks of kinematic training. Musculoskel Sci Pract. 2021; 51: 102312.
- Thunberg J, Hellstrom F, Sjölander P, Bergenheim M, Wenngren B-I, Johansson H. Influences on the fusimotor-muscle spindle system from chemosensitive nerve endings in cervical facet joints in the cat: possible implications for whiplash induced disorders. Pain. 2001; 91: 15–22.
- Vernon H, Mior S. The Neck Disability Index: a study of reliability and validity. J Manipulative Physiol Ther. 1991; 14: 409-4015.
- Vieilledent S, Kerlirzin Y, Dalbera S, Berthoz A. Relationship between velocity and curvature of a human locomotor trajectory. Neurosci Lett. 2001; 305: 65-69.
- Viviani P, Terzuolo C. Trajectory determines movement dynamics. Neuroscience. 1982; 7: 431-7.
- Viviani P, Mounoud P. Perceptuomotor Compatibility in Pursuit Tracking of Two-Dimensional Movements. J Mot Behav. 1990; 22: 407-443.
- Werner IM, Ernst MJ, Treleaven J, Crawford RJ. Intra and interrater reliability and clinical feasibility of a simple measure of cervical movement sense in patients with neck pain. BMC Musculoskelet Disord. 2018; 19: 358.
- Windhorst U, Kokkoroyiannis T. Dynamic behaviour of alpha-motoneurons subjected to recurrent inhibition and reflex feedback via muscle spindles. Neurosci. 1992; 47: 897–907.
- Woodworth RS. The accuracy of voluntary movement. Psychol Rev. 1899; 3: 1-119.