
Special Article – Arthritis and Rheumatic Diseases
Austin J Musculoskelet Disord. 2015;2(3): 1024.
Midfoot Osteoarticular Tuberculosis: Case Report
Oriundo MA¹ and Sampaio ML¹*
Department of Medical Imaging, University of Ottawa, Canada
*Corresponding author: Sampaio ML, Department of Medical Imaging, University of Ottawa, L2121 CPCR Building, 501 Smyth Road, Ottawa, Canada
Received: June 17, 2015; Accepted: July 07, 2015; Published: July 10, 2015
Abstract
Tuberculous osteomyelitis/arthritis in the foot is a rare manifestation of the osteoarticular tuberculosis, usually secondary to pulmonary tuberculosis with hematogenous spread. Its overlap with gout is even more unusual. We report the case of a patient that was diagnosed with tuberculous osteomyelitis of the midfoot overlapped with gouty arthritic changes. Mycobacterium tuberculosis was isolated in a bone biopsy culture and the patient received antibiotic treatment for 15 months due to the bone involvement.
Keywords: Tuberculosis; Gout; Tuberculous osteomyelitis; Tuberculous arthritis; Arthritis; Infection; Foot
Abbreviation
NSAIDs: Non-Steroid Anti-Inflammatory Drugs; Anti-CPP: Antibody Cyclic Citrullinated Peptide; CT: Computed Tomography; MTP: Metatarsophalangeal; TMT: Tarsometatarsal; PAS: Periodic Acid-Schiff
Case Presentation
A caucasian north-American 60 year-old-male with right midfoot pain and medical history of bilateral feet gouty arthritis on treatment, with previous working history at a correctional facility. No other relevant previous medical history. The patient started to develop severe right midfoot pain and tenderness with swelling on January 2013. He was treated as a new acute onset of gouty arthritis with acetaminophen and NSAIDs, but without relief of the symptoms. On follow-up, a screening of autoimmune serology tests was requested and it revealed mild-positive anti-CCP (late May 2013). He was then treated with methotrexate orally weekly and prednisone for 7 days for presumed rheumatoid arthritis. By mid-June 2013 the patient presented some chills, rigors and night sweats, but he denied any cough, chest pain, hemoptysis, rash, eye redness or abdominal pain. On July 2013 chest x-rays and a chest CT (Figures 1 and 2) were performed and they showed a spiculated nodule within the right upper lobe, together with diffuse parenchymal centrilobular nodules in a miliary pattern. This was diagnosed as highly concerning for post-primary respiratory tuberculosis and on the following week a diagnostic bronchoscopy with bronchial washing was performed. The microbiology examination demonstrated acid fast bacilli on the Ziehl- Neelsen stain (July 2013), confirming the diagnosis of pulmonary tuberculosis. At this point the patient was admitted to our institution. On admission the right foot physical examination demonstrated tenderness, swelling and warmth along the right lateral aspect of the midfoot. No other areas appear to be involved. Radiographs of the feet were done and demonstrated mild asymmetric joint space narrowing and small periarticular erosions bilaterally at the two firsts MTP joints, with adjacent soft tissue swelling and mildly mineralized soft tissue nodules, compatible with tophi (Figure 3A). Also, there was severe right midfoot arthropathy involving the navicularcuneiform, intercuneiform and the 1st to 5st TMT joints, particularly the latter (Lisfranc joint), with periarticular bone demineralization. There were also subchondral cyst/erosions at the talar body and minimal peripheral osteophytes and joint effusion at the ankle. These finding were most in keeping with severe polyarticulargouty arthritis. However, the possibility of superimposed infection was raised, including the possibility of tuberculous arthritis, and both a fluoroscopy-guided aspiration of the first TMT joint with a 22G needle and a fluoroscopy-guided bone biopsy of the base of the first metatarsal bone with a 18G bone biopsy needle (Figure 4) were performed during the first week of his admission. The histopathological results of the bone biopsy showed a benign bone with necrotizing granulomatous inflammation. No micro-organism were seen with the special stains (PAS, Grocott, Ziehl-Neelsen). No crystals were identified by polarized light. Microbiological studies to rule out aerobic or anaerobic micro-organism were negative in both the samples from the joint aspiration and bone biopsy. Also, non-acid fast bacilli were not found in the samples. The diagnosis at this point was then of respiratory tuberculosis and gouty arthritis of the foot. The patient was treated with quadruple therapy anti-tuberculosis (isoniazid, rifampin, pyrazinamide and ethambutol) and colchicine plus NSAIDs for the gouty arthritis. He was discharged 10 days after the start of the antituberculosis therapy, also presenting improvement of the general symptoms and no complications from treatment. However, 5 weeks later, Mycobacterium tuberculosis complexes were isolated in the culture of the samples from both the bronchoalveolar lavage and the bone biopsy. So, the suspected previous diagnosis of tuberculous osteomyelitis of the midfoot was confirmed. As a result, the duration of the anti-tuberculosis treatment was prolonged to 15 months. The culture also showed that the Mycobacterium tuberculosis were sensible to the first line anti-tuberculous drugs. Ethambutol was discontinued in the fourth week of treatment due to a paradoxical treatment reaction and pyrazinamide was given until the seventh week of treatment as planned. Two months after the beginning of the anti-tuberculous therapy the foot symptomatology presented a gradual improvement.
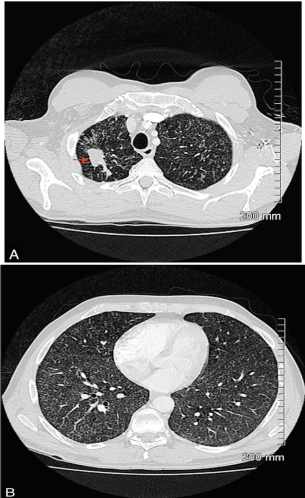
Figure 1: Chest CT without contrast.2mm axial images, lung reconstruction
and window. A) Lung apex. Right apical nodule (arrow). B) Middle third
pulmonary zones. Disseminated micro nodules with in both lobes (miliary
pattern).
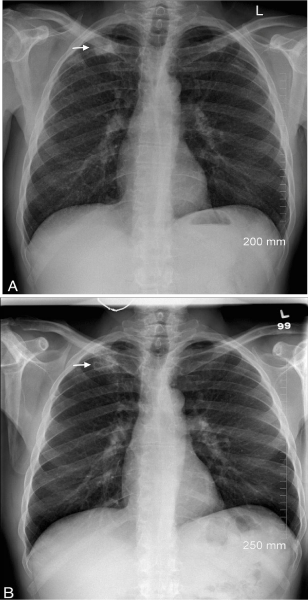
Figure 2: Chest x-ray, PA views. A) At presentation and B) 6 months post
antituberculosis treatment. Radiological response to treatment with reduction
of the micro nodular pattern. Right apical nodule (arrows).Note the interval
cavitation of the nodule in B.
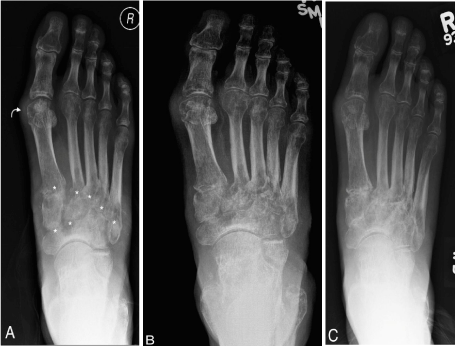
Figure 3: Right foot x-rays, frontal views. A) At the presentation. Severe
midfoot arthritic changes (asterisks), including peri-articular bone
demineralization. Mineralized soft tissue mass about the 1st MTP (curved
arrow).B)four months and C)fourteen months follow-ups.Relatively stable
appearance of the arthritic changes of the TMT, MTP and interphalangeal
joints, associated to mild improvement of soft tissues swelling adjacent to
the TMT joints. There was no progression of bone destruction. In C) there
was also improvement of the midfoot peri-articular demineralization and mild
sclerosis around the midfoot bone erosions.
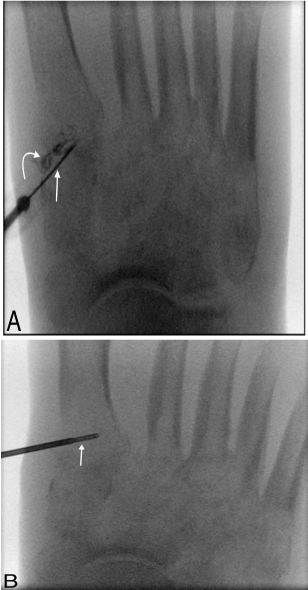
Figure 4: A) Right first TMT joint aspiration with a 22-gauge needle (arrow)
under fluoroscopic guidance. Contrast medium (curved arrow) was injected
at the end of the procedure to demonstrate the intra-articular positioning. B)
First metatarsal base bone biopsy with 18-gauge bone needle (arrow) under
fluoroscopic-guide.
The chest follow-up x-rays (Figure 2B) of January 2014 showed improvement of the miliary pattern and the right upper pulmonary nodule presented cavitation. The right foot follow-up x-rays dated November 2013 and September 2014 (Figure 3B and 3C) showed no progression of the chronic arthritic/gouty changes previously described. However, the latter follow-up showed some improvement of the peri-articular bone demineralization and some sclerosis of the midfoot erosions, suggestive of ongoing healing. In January 2014 the patient also presented spontaneously drained pasty pus from the lateral aspect of the midfoot. The culture of this discharge did not isolate any Mycobacterium tuberculosis. The patient was treated with isoniazid and rifampicin until October 2014, without any complication, being discharged and having completed 15 months of treatment, with overall improvement of the symptoms.
Discussion
Tuberculosis can potentially affect any organ or system of the body and it can be devastating if left untreated. Osteoarticular tuberculosis makes up less than 3% of the cases of extra-pulmonary tuberculosis and it can affect bones, joints, tendons and bursae [1- 4]. The most common musculoskeletal manifestation of tuberculosis is tuberculous spondylitis, corresponding to 50% of the cases. The different components of the appendicular skeleton are affected less frequently [1,2,5]. The specific involvement of foot is considered very rare and it represents less than 1% of the cases [4]. The involvement of the midfoot is even rarer and to our knowledge only a single case was previously reported in English language [6]. Osteoarticular tuberculosis is mostly secondary to hematogenous dissemination of pulmonary tuberculosis. In our case, the midfoot symptoms started five months before the onset of general and respiratory symptoms. Osteoarticular tuberculosis of the midfoot was not suspected at the beginning given the history of gouty arthritis and typical radiological findings. However, after the confirmation of pulmonary tuberculosis and the absence of improvement of the foot symptoms following the initial treatment for gout, the possibility of an extremely rare overlap between tuberculous osteomyelitis/arthritis and gout was hypothesized. This association was previously reported by Lorenzo et al in 1997 [7]. Periarticular bone demineralization and swelling of soft tissues have been reported as the first radiographic signs of osteoarticular tuberculosis, consisting of a non-specific set of signs that may be encountered in bones and joints infections, crystal and inflammatory arthritis. These finding were present in this case, however the mineralized soft tissue mass and the pattern of arthritic distribution were typical for gouty arthritis. Therefore, gout was a clinical and radiological distractor in the present case. Furthermore, appendicular osteoarticular tuberculosis has been reported mostly as a monoarthropathy and less frequently as an oligoarthropathy, more typically involving major weight-bearing joints such as the hip and knee, at times presenting as a pseudo-mass or “cold abscess” [3,5,6]. This form of tuberculosis is also a paucibacillary lesion, potentially difficult to by confirmed on stain or even on culture [3,4,8]. In our case, the presence of Koch’s bacilli was confirmed in the bone biopsy of the first metatarsal bone, but the bacilli were not identified in the acid fast staining. The fluoroscopy-guided biopsy of the bone turnedout to be adequate and the need of an open bone biopsy was not necessary in our case. Also, acid fast bacilli were not found in the joint aspiration sample. Note that the diagnosis of tuberculous arthritis is normally presumed taking into account the overall clinical and radiological findings. Bone involvement associated with tuberculosis arthritis is also more frequent when compared to isolated involvement of the bone [2]. The treatment of osteoarticular tuberculosis consists in a combination of multi anti-tuberculous drugs at least for 12 months [2,3,8]. Our patient showed a good clinical and radiological response to the treatment as seen in the thoracic radiological followups. The foot radiological evaluation demonstrated a relatively stable appearance of the chronic arthritic/gouty changes, with late follow-up improvement of the bone demineralization and mild sclerosis of erosions, favoring arthritic healing. These findings favor a good therapeutic response. Surgical treatment of osteoarticular tuberculosis includes joint debridement, lavage, synovectomny and drainage of abscesses. If osteoarticular tuberculosis is left untreated, it may lead to significant functional disability [2,3,8-11].
References
- Harisinghani MG, McLoud TC, Shepard JA, Ko JP, Shroff MM, Mueller PR. Tuberculosis from head to toe. Radiographics. 2000; 20: 449-470.
- Dhillon MS, Aggarwal S, Prabhakar S, Bachhal V. Tuberculosis of the foot: An osteolytic variety. Indian J Orthop. 2012; 46: 206-211.
- Berrady MA, Hmouri I, Benabdesslam A, Berrada MS, E Yaacoubi M. Tuberculosis arthritis of the metatarsal phalangeal: a rare location. Pan Afr Med J. 2014; 17: 323.
- Magnussen A, Dinneen A, Ramesh P. Osteoarticular tuberculosis: increasing incidence of a difficult clinical diagnosis. Br J Gen Pract. 2013; 63: 385-386.
- Dahuja A, Dahuja G, Kaur R, Bansal K. Isolated tuberculosis of talus: a case report. Malays Orthop J. 2014; 8: 61-62.
- Hachimi H, Tahiri L, Kadi N, Ibrahimi A, Elmrini A, Harzy T. [Tuberculosis of the midfoot, an unusual location: report of a case]. Pan Afr Med J. 2012; 11: 53.
- Lorenzo JP1, Csuka ME, Derfus BA, Gotoff RA, McCarthy GM. Concurrent gout and Mycobacterium tuberculosis arthritis. J Rheumatol. 1997; 24: 184-186.
- Agarwal A, Qureshi NA, Khan SA, Kumar P, Samaiya S. Tuberculosis of the foot and ankle in children. J Orthop Surg (Hong Kong). 2011; 19: 213-217.
- Mittal R, Gupta V, Rastogi S. Tuberculosis of the foot. J Bone Joint Surg Br. 1999; 81: 997-1000.
- Watts HG, Lifeso RM. Tuberculosis of bones and joints. J Bone Joint Surg Am. 1996; 78: 288-298.
- Davies PD, Humphries MJ, Byfield SP, Nunn AJ, Darbyshire JH, Citron KM, et al. Bone and joint tuberculosis. A survey of notifications in England and Wales. J Bone Joint Surg Br. 1984; 66: 326-330.