
Case Report
Austin J Musculoskelet Disord. 2016; 3(1): 1027.
Parosteal Lipoma of the Proximal Radius
John SH1, Chad CBS1, Kathleen SB1*, Valerie AF2, Marcia FB3 and Joseph B1
1Division of Musculoskeletal Oncology, Department of Orthopedic Surgery Rutgers, The State University of New Jersey-New Jersey Medical School, USA
2Department of Pathology and Laboratory Medicine, Rutgers, The State University of New Jersey-New Jersey Medical School, USA
3Department of Radiology Rutgers, The State University of New Jersey-New Jersey Medical School, USA
*Corresponding author: Kathleen S Beebe, Department of Orthopedics, Division of Musculoskeletal Oncology New Jersey Medical School Rutgers, The State University of New Jersey 140 Bergen St. Suite D-1610 Newark, NJ 07103, USA
Received: November 30, 2015; Accepted: January 19, 2016; Published: January 22, 2016
Abstract
Parosteal lipomas and are described as surface osseous lipomas which are contiguous with the periosteum. They represent 15% of osseous lipomas and most occur in the fifth and sixth decades with a slight male predilection. To date, only 150 of these tumors have been reported in the literature. We present a rare case of Parosteal lipoma with cytogenetic correlation. The clinical implications of this lesion will also be discussed.
Keywords: Parosteal lipoma; Forearm; Tumor
Introduction
Lipomas are common benign soft-tissue tumors, which are usually asymptomatic [1]. Grossly, they are encapsulated, yellow soft tissue masses that may also have other tissue components incorporated within them. These lipomas are named according to the coexisting tissues; such as angiolipoma, fibrolipoma andosteolipoma [2].
Osseous lipomas have been classified according to their site of origin: either within bone (intraosseous) or on its surface (juxtacortical). Surface osseous lipomas are subdivided into Parosteal and subparosteal lipomas, depending on their relationship to the bone periosteum [3]. To the best of the author’s knowledge, about Parosteal lipomas have been reported to date, representing less than 0.3% of allipomas. These unusual masses most frequently arise in the femur, tibia, humerus and radius [4,5].
Case Report
A 62 year old woman presented with a palpable mass in the anterior left proximal forearm. She had noticed the mass enlarging over the preceding year, but denied any pain or loss of function associated with anterior intraosseous nerve compression, such as loss of pincer grip. Physical examination revealed a fixed, nonpulsatile mass over the volar radius. The patient had full range of motion at theel bow, wrist and fingers, but did show a mild decrease in grip strength compared to the contra lateral hand. She denied any tenderness upon diffuse palpation.
Conventional radiographs of the left forearm displayed an oval density in the soft tissues volar to the radial shaft (Figure 1). Magnetic Resonance Imaging (MRI) done the same day demonstrated a welldefined mass composed of mostly fatty tissue, with diffuse areas of hypo intensity, consistent with cortical bone, which was contiguous with the cortical bone on the volar radial shaft (Figure 2). A wholebody bone scan showed increased activity in the region of the proximal radius, consistent with erosion of the radial cortex by the adjacent lesion.
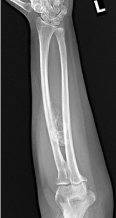
Figure 1: A and B-Radiographs forearm.1A). Frontal radiograph of the left
forearm: There is an ossify density adjacent to the ulnar cortex of the radial
shaft (arrowheads). Subtle thickening of the cortex is seen (open arrow). 1B).
Sagittal radiograph shows surrounding radiolucent lipomatous mass (open
arrow) and ossify density adjacent to volar cortex of radius (arrowhead).
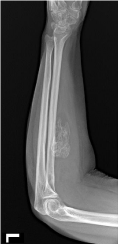
Figure 2: Axial CT image of left forearm demonstrate ossify excrescence
on the volar cortex of the radial shaft, without medullary continuity. It is
surrounded by a lipomatous soft tissue mass.
Computed Tomography (CT) of the left forearm revealed a focus of ossification in continuity with the volar radial shaft surrounded by fat, suggesting a Parosteal Lipoma (Figure 3). The mass began 5.9cm distal to the radial head and extended 6cm distally. Radiographically the lesion was compressing the flex or digit or umsuperficialis and profundus and the anterior intraosseous neurovascular bundle. Based on imaging, the mass was suspected to be benign and the patient was indicated for a marginal excision.
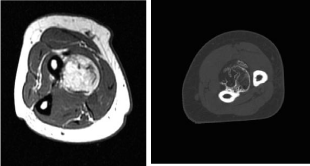
Figure 3: Short axis MR T1W image of left forearm shows ossify density filled
with fatty marrow on the volar cortex of the radius. There is no medullary
continuity. Thin lipomatous mass surrounding lesion with the underlying volar
radial shaft periosteum.
At the time of surgery, a 12cm incision was made over the mass to the level of the fascia, utilizing the interval between the brachioradialis and pronator teres.The fascia was then incised and retracted, at which point the radial artery was identified and feeding vessels branching from the artery were ligated to maintain hemostasis. The pronator teres and flexor Carpi radialis were retracted medially and the brachioradialis laterally to visualize the lesion (Figure 4).
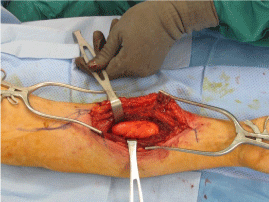
Figure 4: Intraoperative photo depicting the surgical approach and anatomic
location of the mass.
The lesion was resected from surrounding soft tissues and a firm attachment to the proximal radial shaft was noted. The mass and underlying periosteum were resected along with a small superficial portion of the radial cortex using anosteotome with care taken to avoid fracturing the radius. Following resection the radius was confirmed to be intact through fluoroscopic imaging.
The specimen was submitted for analysis by a musculoskeletal pathologist. Grossly the specimen was noted to be composed of an adipose tissue mass demonstrating an intimate association with the underlying bone. As per protocol, the specimen was submitted for cytogenetic analysis. Histologically, the lesion consisted of mature adipose tissue with relatively consistently sized adipocytes demonstrating a contiguous relationship with the periosteum (Figure 5). Additionally, the lesion demonstrated a female karyotype with a derivative chromosome 12. Cytogenetic studies demonstrating rearrangements of chromosome 12q13-15 are commonly identified in lipomas. This histologic and cytogenetic finding confirmed the diagnosis of Parosteal lipoma.
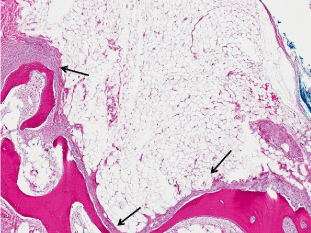
Figure 5: Mature adipose tissue mass demonstrating attachment to
theperiosteum (arrows) with underling bone (Hematoxylin and eosin, 100X).
Three months post-resection, of the Parosteal lipoma from the proximal radius, the patient had full range of motion of the digits, wrist and the elbow, including supination and pronation. She denied any neurovascular symptoms and the surgical site was well healed.
Discussion
Parosteal lipomas are rare lesions of ossified adipose tissue that occur on long bones [6]. The lesions are benign, but can cause neurovascular symptoms if allowed to enlarge to the point of compression of adjacent structures [1]. When located adjacent to the neck of the radius, these masses can cause nerve compression, leading to intraosseous nerve palsies [7].
Due to the possibility of complications involved with an untreated radial neck Parosteal lipoma, it is important to treat in a timely manner. The difficulties associated with a forearm lesion resection arise as a result of adjacent vulnerable structures. Injury to neurovascular structures, as well as the possibility of fracture or loss of motion may lead to long term sequelae and loss of function. For these reasons, care must be taken to maintain the integrity of these structures.
An anterior approach to proximal volar radial shaft lesions, utilizing the interval between the brachioradialis and pronator teres allows for full visualization of the lesion and underlying proximal radius. In addition, the adjacent neurovascular bundle can be mobilized and controlled, as needed, to maintain hemostatis and avoid iatrogenic neuropathies. Using the fascial separation between the muscles allows for minimal sequelae as a result of the surgical approach and post-operative heeling.
In summary, we report on a case of a proximal volar radial shaft Parosteal lipoma, with its interesting cytogenetic abnormalities and provide an overview of the literature with regards to Parosteal lipomas.
References
- Kline DG, Hudson AR. Nerve injuries: operative results for major nerve injuries, entrapments, and tumors (1st ed). Philadelphia: WB. Saunders.
- Demirkan F, Demirkan N. Ossifying Lipoma at the Wrist. Aegean Pathology Journal. 2004; 19-21.
- Kapukaya A, Subasi M, Dabak N, Ozkul E. Osseous lipoma: eleven new cases and review of the literature. Acta Orthop Belg. 2006; 72: 603-614.
- Ek ET, Slavin JL, Blackney MC, Powell GJ. Parosteal lipoma associated with an underlying osteochondroma arising from the hallux. Skeletal Radiol. 2007; 36: 689-692.
- Saksobhavivat N, Jaovisidha S, Sirikulchayanonta V, Nartthanarung A. Parosteal ossifying lipoma of the fibula: a case report with contrast-enhanced MR study and a review of the literature. Singapore Med J. 2012; 53: e172-175.
- Bispo Junior RZ, Guedes AV. Parosteal lipoma of the femur with hyperostosis: case report and literature review. Clinics (Sao Paulo). 2007; 62: 647-652.
- Ganapathy K, Winston T, Seshadri V. Posterior intraosseous nerve palsy due to intermuscular lipoma. Surg Neurol. 2006; 65: 495-496.