
Case Report
Austin J Musculoskelet Disord. 2016; 3(2): 1037.
Cure of a Giant Cell Reparative Granuloma of the Maxilla
Elansari R*, Elababsi R, Elbaghdadi T, Abada R, Rouadi S, Roubal M and Mahtar M
Ent Department 20 August Hospital, University Hospital Ibn Rochd Casablanca, Morocco
*Corresponding author: Rachid Elansari, Ent Department 20 August Hospital, University Hospital Ibn Rochd Casablanca, Morocco
Received: November 08, 2016; Accepted: December 28, 2016; Published: December 30, 2016
Abstract
Giant cell granuloma or Central Giant Cell Granuloma (CGCG) is a benign maxillary lesion of unknown etiology. This tumor, infrequent, non-painful evolution, sometimes exhibiting aggressive behavior. Only histological study allows the diagnosis of certainty.
The reported case is a 13 year old who consult a dentist for a vestibular-palatal swelling left looks of 26, who underwent tooth extraction with antibiotics without improvement .the axial CT scan of the face objectified a hétérodensetissular mass of 46*42mm seat at the rear and middle part of the two nasal cavities, with lysis of the nasal septum and the posterior portion of the vomer.
Routine laboratory investigations including serum calcium, phosphorous and alkaline phosphatase were within normal limits. A biopsy of the lesion was in favor of a CGCG. The treatment consisted of combined surgical excision by para-latero-nasal route and endonasal approach. With a follow up of 3 years, we have noted no tumor recurrence.
Though defined histologically as benign lesions, giant cell granuloma have the capacity for local destruction. Thus, a treatment modality that would arrest the growth is mandatory
Keywords: Reparative granuloma; CGCG; Giant cells; Maxilla; Tumor; Exeresis
Introduction
Giant cell reparative granuloma or central giant cell granuloma (CGCG, classified by the World Health Organization) is an uncommon benign lesion of the jaws although some may demonstrate an aggressive behavior. More common in the mandible than in the maxilla.
Case Presentation
13 years old, came for a consultation with her dentist for a painful swelling on the left posterior maxilla involving buccal and palatal tissue. An extraction under local anesthesia of tooth 26, suspected as causal, was performed and an immediate postoperative bleeding was noted. An ant biotherapy was prescribed for 7 days.
Three weeks after the removal of tooth 26, the swellings till persisted. The patient was referred to our ENT DEPARTEMENT 20 August hospital. During the clinical examination, a Swelling was found involving the left hemi-palate and alveolar bone crest corresponding to teeth 25, 26, 27 and 28. The covering mucosa seemed normal and firm to palpation.
An axial CT scan of the face revealed soft tissue window without contrast agent demonstrating the expansileheterodense mass of 46*42mm with well-defined borders centered on the nasal cavity, with lysis of the nasal septum, the horizontal part of the palatine bone with extension to the alveolar process of the right maxillary bone (Figure 1).
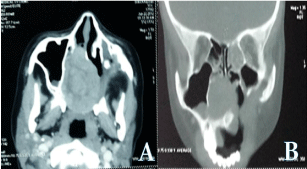
Figure 1: A: axial CT scan of the face revealed expansible hetero dense
mass of 46*42mm with well-defined borders centered on the nasal cavity,
with lysis of the nasal septum and the palatine bone, B: coronal CT scan of
the face revealed extension to the alveolar process of the right maxillary bone
and medial wall of right maxillary sinus.
Routine laboratory investigations including serum calcium, phosphorous and alkaline phosphatase were within normal limits. A surgical biopsy under local anesthesia was performed showing a voluminous bone cavity filled with a highly hemorrhagic.
Histopathological examination showed proliferating fibroblastic stroma intermingled with osteoclastic giant cells. Areas of hemorrhage were seen and the giant cells were clustered around the areas of hemorrhage (Figure 2). A diagnosis of CGCG was made.
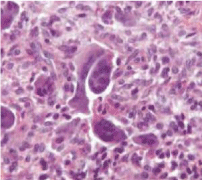
Figure 2: Microscopic view: Many multi-nucleated giant cells can be seen
amidst fibroblasts presenting an irregular, non-mitotic nucleus.
Considering results of the CT scan images, the biological assessment and the biopsy, a surgical excision was decided and paralatero- nasal route combined to endoscopic approach.
Once the flap elevated, the tumor was immediately exposed. During monobloc excision, the tumor was highly hemorrhagic and crisp. A complete curettage of all colonized bone trabeculae was performed until bone tissue of healthy appearance was obtained.
The complete excision is controlled by a maxillary sinusoscopy using an optic instrument under 30 degrees. A coverage antibiotherapy for 7 days, a level 2 analgesics and a mouthwash with 0.12% chlorhexidine were prescribed.
At 1 month postoperatively, healing of the mucosa was firstly obtained on the buccal and no residual pain was indicated.
At 6 months, one year and three years postoperatively, the patient described no more discomfort and the clinical examination did not reveal any residual swelling or dental pain (Figure 3).

Figure 3: Without any residual swelling in clinical examination after three
years follow up.
Discussion
Central giant cell granuloma is a non-neoplastic proliferation of unknown etiology. CGCG accounts for less than 7% of all benign lesions of mandible and maxilla. These lesions occur 2-3 times more frequently in mandible than in maxilla [1]. They generally occur in patients in 2nd and 3rd decades of life. But can occur from infants to 7th decade of life. 74% of the patients are under 30 years at the time of presentation [2]. It is 2-3 times common in female than in males but, there is no apparent explanation for female preponderance. They have been reported in other in parts of a body including small bones, skull, spine, clavicle, tibia, humerus, and ribs [3]. Peripheral type was four times more common than central type and is seen in middle aged and elderly patients [4]. Non specific pain and swelling are the most common clinical manifestations [4]. Multiple lesions are rare but have been reported. But, when multiple lesions occur investigations should be done to rule out hyperparathyroidism.
Trauma has been considered as important etiological factor for the initiation of lesion. Radiologically CGCG appears as non specific, multiloculated lesions which due to slow growth cause thinning and scalloping of cortex, which however is rarely breached [5]. Sometimes aggressive lesions may be present with bone destruction [3,5]. CT scan is excellent for demonstration of bone thinning or destruction. MRI is the best modality of evaluating the extent of the lesion. It has low to intermediate intensity signals on both T1 W and T2 W images similar to GCT. Mild post enhancement is evident both on CT and MRI. Histologically multinucleated giant cells in a cellular vascular stoma with new bone formation are detected. The osteoclast like giant cells has irregular distribution and is associated with areas of hemorrhage [6]. Ultra structurally the proliferating cells include spindle shaped fibroblasts, myofibroblasts and inflammatory mono nuclear cells [1,6]. Surgery is the traditional and most accepted form of treatment for CGCG. However, the extent of tissue removal ranges from simple curettage to unblock resection [6]. The incidence of recurrence after surgery is 4-20 %. The eradication of lesion does not require more than two excisions.
Conclusion
CGCG is a less frequent tumor found in daily ENT surgeon practice. Its rareness leads to diagnostic difficulties.
A rigorous diagnostic approach is needed including meticulous history taking, attentive clinical examination, complete radiological examination, targeted biological assessment and anatomopathological analysis.
Conventional treatment by surgery with curettage associated or not to an extensive excision engenders the least recurrence.
References
- Walstad WR, Fields T, Schow RS, Mckenna SJ. Expansible lesion of anterior maxilla. J Oral Maxillofacial Surg. 1999; 57: 595-599.
- Sholapurkar AA, Pai KM, Ahsan A. Central giant cell granuloma of the anterior maxilla. Indian J Dent Res. 2008; 19: 78-82.
- Shah UA, Shah AK, Kumar S. Giant cell reparative granuloma of the jaw: a case report. Indian J Radiol Imag. 2006; 16: 677-678.
- Curtis NJ, Walker DM. A case of aggressive multiple metachronous central giant cell granulomas of the jaws: differential diagnosis and management options. Int J Oralmaxillofac Surg. 2005; 34: 806-808.
- Murphy MD, Nomikos GC, Flemming DF, Gannon FH, et al. Imaging of giant cell tumor and giant cell reparative granuloma of bone: radiologic–pathologic correlation. Radiographics. 2001; 21: 1283-1309.
- Ciorba A, Altissimi G, Giansanti M. Giant cell granuloma of maxilla: case report. Acta Otorhinolaryngol Ital. 2004; 24: 26-29.