
Review Article
Austin J Musculoskelet Disord. 2019; 6(1): 1053.
Muscle Stretching Techniques for Congenital Muscular Torticollis: Review of the Literature and Practical Applications
Pommerol P1, Jeandel C2 and Captier G*2,3
¹Centre PAPL Formation, 24 Rue Sully 69006 Lyon, France
²Service de Chirurgie Orthopédique et Plastique Pédiatrique, Hôpital Lapeyronie, CHU de Montpellier, Université de Montpellier, Montpellier, France
³EA2415, Aide À La Décision Médicale Personnalisée, Université Montpellier, Montpellier, France
*Corresponding author: Guillaume Captier, Hôpital Lapeyronie, 371 Av. du Doyen Gaston Giraud, 34090 Montpellier, France
Received: July 31, 2019; Accepted: September 09, 2019 Published: September 16, 2019
Abstract
Background: Congenital muscular torticollis is a risk factor for positional skull deformities. Sternocleidomastoid muscle stretching is at the basis of the treatment by physiotherapy for the myogenic forms.
Objective: To describe the techniques, frequency, and optimal duration of this conservative treatment as well as its efficacy.
Methods: Systematic review of clinical studies on infants younger than 18 months of age with congenital muscular torticollis published from 1990 to 2018. Comparative and cohort studies with follow-up and description of the used stretching technique were selected. Studies on the treatment of postural torticollis were excluded.
Results: Among the 508 studies identified by bibliographic search, ten met the inclusion criteria. They showed a large variation in stretching frequency, duration, and intensity. In 50% of cases, stretching was performed by two operators. The frequency of three times per week for infants younger than 6 weeks of age was the most common. The addition of stretching exercises at home by the parents was recommended. Treatment was more effective when started before 3 months of age, and the efficacy was assessed on the basis of the recovery of the head passive range of motion during lateral flexion and rotation.
Conclusions: Muscle stretching is the reference treatment for non-postural congenital muscular torticollis and allows its complete resolution, if started early. The parameters that influence the treatment success are the parents’ adhesion and the addition of a programme of home exercises/postural education.
Keywords: Infant; Congenital Muscular Torticollis; Stretching
Abbreviations
CMT: Congenital Muscular Torticollis; PT: Postural Torticollis; MT: Myogenic Torticollis; SCM: Sterno Cleidomastoid Muscle
Introduction
Congenital Muscular Torticollis (CMT) is characterized by a lateral flexion of the neck with rotation of the chin in the opposite direction. This musculoskeletal condition appears in the infant’s first weeks of life. It is a risk factor of postural skull deformities the incidence of which has increased after the recommendation of putting babies to sleep on their back to prevent sudden infant death [1,2]. Three clinical forms have been described: Postural Torticollis (PT) and two forms of Myogenic Torticollis (MT) caused by tightness of the Sternocleidomastoid (SCM) muscle or the presence of a fibrotic mass in the SCM muscle [3-5]. MT is characterized by a permanent limitation of the head passive range of motion, differently from PT. Manual muscle-stretching exercise is the reference treatment for MT. Different studies [4,6,7] have shown that muscle stretching allows limiting endomysial collagen fibril deposition and fibroblast migration around individual muscle fibers [8]. The treatment intensity is determined in function of the infant’s age, the type of muscle lesion, and the initial deficit of passive rotation [4]. The MT type is one of the significant predictive factors of the final result of conservative treatment [4,9,10]. Compared with MT with a lump or olive-like mass, MT due to muscle shortening are identified much later when the problems in lateral flexion and rotation become evident [11]. The main objective of this study was to review retrospective and prospective, comparative or not, clinical studies on muscle stretching for MT to determine the best modality (technique, frequency, and total number of sessions). The secondary objectives were to assess the efficacy of the physical treatment and to determine when to start, duration, and when/how to stop.
Methods
Literature search
Studies on CMT were identified by searching the following databases in 2018: Banque de Données en Santé Publique (BDSP; French Public Health Database) from 2005 to March 2018, CISMeF from 1998 to March 2018, Cochrane Library from 2002 to July 2018, EM Consulte from 1980 to July 2018, PEDro without limits and up to September 2018, MEDLINE via PubMed from 1994 to September 2018, and Google Scholar without limits and up to September 2018. This search was completed by a manual search using ResearchGate.
The key words used to interrogate these databases were: Torticollis in Infants, Torticollis Muscular Congenital with Inversion of the Words’ Order, Muscular Torticollis, Congenital Torticollis in Infants Stretching and Torticollis, Stretching and Torticollis Congenital Muscular Congenital Muscular Torticollis, and Physical Therapy and Torticollis Muscular Congenital. The word fibromatosis colli was not used because fibromatosis colli with CMT may regress spontaneously or show an almost inexistent torticollis [12].
Inclusion and exclusion criteria
Articles were selected on the basis of the following inclusion criteria: i) study on muscle stretching in infants with MT younger than 18 months at treatment initiation; ii) comparative or cohort study with follow-up; and iii) studies including a description of the muscle stretching technique.
Exclusion criteria were: i) incomplete description of the stretching protocol; ii) study that did not allow identifying the CMT types; iii) treatments concerning only PT; and iv) CMT associated with a neurological pathology.
Study selection
The literature and manual search returned 508 records that underwent four additional selection steps (Figure 1): i) selection based on the article title and key words (n=380 articles retained); ii) selection based on the inclusion criteria after reading the article summary (n= 48 articles retained); iii) these articles were fully read by two authors (PP and GC) (n=20 articles retained); and iv) ten articles were excluded based on the exclusion criteria, or due to lack of pertinence or contradictory data in the main text. The ten excluded articles included: Lee, 2015: study on two groups (treatment started before and after 6 weeks) of infants younger than 6 months using the conservative treatment protocol described by Emery [11] that included muscle stretching, massage and therapeutic ultrasound (important bias) and compared the effects of manual stretching and postural control intervention in infants with CMT (off topic); Haugen et al. 2011: study on a manual therapy without stretching; Ohman et al. 2011: off topic; Kwon and Park 2014, and Kim et al. 2009 [13]: studies on micro-current therapy; Giray et al. 2017, Ohman 2012: studies that included also kinesiology taping; Keklicek and Uygur 2018: study on soft tissue mobilization; Schertz et al. 2008 and 2012: follow-up of patients with torticollis, but poorly described treatment. The scientific pertinence of the selected articles (n=10) was assessed using the PEDro scale, a specific physiotherapy scale graded from 1 to 10 [14], and according to the levels of evidence proposed by French Higher health authority, where level I corresponds to the highest evidence level and level IV to the lowest.
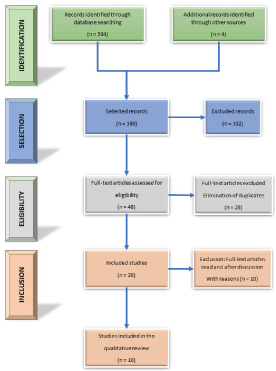
Figure 1:
Results and Discussion
After selection, ten studies were retained on MT treatment by passive muscle stretching in infants younger than 18 months of age. The different muscle stretching protocols are summarized in Table 1. The selected studies were not highly reliable [4,15] and of average quality. Specifically, the mean PEDro value was 5/10 (range: 2-7), and the HAS level was II for seven studies and IV for three studies.
Authors
Evidence level
Operators
Frequency
Repetitions (hold/ rest)
Treatment duration (mean)
Protocol
Outcome
Celayir, 2000 [28]
N=45 (<4 months) Prospective cohort studyHAS II
PEDro 5 /10Two with a medical doctor as instructor (no physical therapist)
8x/day at home
10 / session (10s hold) (total n=80 repetitions / day)
3.2 months
Therapeutic education with alternative positioning, handling and active range of motion by the parents in addition to passive stretching.
Surgery if failure.No surgery needed; 100% of success for all infants younger <4 months at treatment initiation
Asymmetry: 80% of infants recovered complete rotation without asymmetry; 20% showed complete rotation with mild asymmetry or mild rotation deficit without asymmetryChon et al. 2010 [26]
N=32:
1 group with olive-like mass and 1 group without.
Age <3 months Retrospective cohortHAS IV
PEDro 6/102 people, parent and physical therapist
5×/week in healthcare centre
4 sets of 15 stretches with 3min rest; 30 min / session
53.59 days
SCM stretching and finger pressure (5 to 10s); head positioning and therapeutic education programme of home exercises controlled daily
Muscle thickness: significant SMC reduction (P <0.05) in patients with MT with and without olive-like mass (no difference between groups).
Infants were younger than 3 months at treatment initiation.Ryu et al. 2016 [6]
N=61 infants with MT
Retrospective studyHAS II
PEDro 6/10Physical therapist or not (control group)
3x/week at the physical therapist
3 sets of 15 repetitions (1-2s hold)
Session duration: 30 min6.4 months
2 groups: with (N= 34) and without physical therapist (N=27; control).
Physical therapy was the only factor that promoted MT resolution: 27/34 infants with complete resolution in the treated group and 15/27 in the control group.
He et al. 2017 [32]
N=50 infants with CMT
Age <3months
Prospective randomized controlled trialHAS II
PEDro 6/10Physical therapist
Every day for 8 weeks
5 sets of 10, or 10 sets of 10 repetitions (10-15s hold)
Study for 8 weeks
Manual stretching of the affected SCM muscle.
10 stretches in rotation and 10 in flexionSignificant improvement in both groups (p <0.05). Head flexion and cervical passive motion range were better in the group with 100 repetitions than in the group with 50 repetitions at week 4 and 8 (p <0.05). Conclusion by the authors: Manual stretching therapy can improve efficiently head flexion, neck passive motion range and SCM muscle in infants with CMT. The modality with 100 repetitions per day is better.
Emery, 1994 [11]
N=101, Mean age: 4 months
Follow-up of a prospective cohort, not comparativeHAS II
PEDro 6/10Physical therapist and parents (stretching with two people)
2x/day
5 repetitions (10s hold)
4.7 months;
3.9 months without olive-like mass,
6.9 months with olive-like massSCM muscle handling with ipsilateral rotation and contralateral flexion. Alternative sleep positioning and righting reactions to strengthen the weak side
Complete resolution in 99% of patients (100/101); 1 surgery required. The pseudo-tumoral form was correlated with severity and longer duration of treatment. 36% received a cervical collar.
Cameron et al. 1994 [29]
N= 126
Retrospective cohortHAS IV
PEDro 2/102 parents
2x/day at home
10 repetitions (10s hold)
Up to 9-10 months of age for infants with MT detected <3 months of age.
Not described; but 4 failures excluded from the statistical analysis.
If treatment initiated <3 months of age, 100% of infants with complete resolution (no surgery).
If treatment initiated >3 months 45% of infants underwent surgery; 65% of infants had excellent results (complete range of motion and no asymmetry); 27% had good results (complete rotation and mild asymmetry or mild rotation deficit and no asymmetry); 8% had poor results (no improvement).Demirbilek et Atayurt 1999 [25]
N=57 aged <18 months
Retrospective cohortHAS IV
PEDro 2/102 people, parents
4-5x/day
40 repetition / session
Parents performed the passive stretching exercises and the active motion exercises.
Surgery if failure.If <3 months of age: no surgery
If between 3 and 6 months of age: 25% of surgery H10
If between 6 and 18 months of age: 71% of surgery
If between 6 and 18 months of age: 71% of surgery
If between 2 and 7 years of age: 100% of surgery.
Overall, 26% of patients (15/57) had surgery.Cheng et al. 2001 [30]
N=821
Prospective cohortHAS II
PEDro 5/101 physical therapist; parents had only instruction on posture
3x/week
3 repetitions of 15 stretches (1s hold and 10s rest)
Median:
1.4 months for PT
2.5 months for MT without mass
3.7 months for MT with olive-like massActive positioning to stretch the muscle, and righting to strengthen the weak muscle
Surgery: 7.5% of infants with MT with mass; 3.1% of infants with MT without mass; 0% for PT.
Ohman et al. 2010 [31]
N=20 with treatment onset <5 months of age
Randomized pilot studyHAS II PEDro 5 /10
1 group with physical therapist and 1 group treated by the parents
3x/week with a physical therapist, and home exercises by the parents every day (2x per 15min/day)
15min with unlimited repetitions (10-30s hold)
For both groups: Prone positioning, carrying with the affected side down to stretch the muscle, gentle passive stretching of the affected muscles
Treatment duration was two months shorter in the group with physical therapist than in the group with stretching done only by the parents
Lee et al. 2017 [44]
N= 102 infants
Torticollis of grade 1* (rotation >15°) and of grade 2 (15°<<30°) and age <6 months
Prospective cohortHAS II
PEDro 7/10Physical therapist
3x/week
physical therapy sessions10 stretches (10-30s hold)
Contralateral flexion and ipsi-lateral rotation6 months of treatment
1 group with treatment started before 6 weeks (N=55) and 1 group after 6 weeks (n=47) For both groups
manual stretching, therapeutic ultrasound (3 min), massage 5-7 minTreatment gave better results in the group that started before 6 weeks of age (ultrasound parameters and head range of motion and flexion)
Table 1:
Muscle stretching exercise modalities (Table 1)
Manual stretching is the most common type of treatment for MT. Its efficacy in resolving MT was demonstrated by Ryu et al. [6] by comparing two groups (with and without muscle stretching) of infants with MT that was detected before the age of 4 months. In the group with stretching, they found a significant correlation between physical therapy and resolution of the ultrasound parameters of MT at the SCM level. The authors concluded that physical therapy was the only factor that improved MT management with a programme of manual muscle stretching of 30 minutes (15 stretches of 1-2 seconds repeated three times, with a rest period of 10 seconds between stretches; 3 sessions per week) and home exercises carried out by the parents (for both groups). The stretching technique varied in the selected studies. In 50% of them, it needed two operators: one person to stabilize the infant’s shoulders and one to perform the stretch. Stretching was performed with the infant in supine position or on one side. In this case, the infant was placed on the opposite side relative to the affected side to take advantage of the body weight for muscle stretching. In function of the infant’s age, the patient was placed on the lap of the seated physical therapist or on the edge of a treatment table, while the therapist was mostly in front to hold the head. For a right torticollis, the skull was held with the right hand under the occiput, and the left hand on the chin. This hand position allows the rotation to the right and then the flexion to the left. A light traction was applied, and a rotation to the right was performed. This position was maintained for 5 to 10 seconds. The lateral flexion also was initiated with a light traction, followed by a light flexion to the front and a 10° rotation to the right. Then, the head was guided laterally in such a way that the left ear became close to the left shoulder [11]. The correct and stable hand placement is crucial to perform the stretching correctly. Kaplan et al. described several techniques and recommended that the technique should be chosen in function of the infant’s age and size [15]. They recommended increasing the passive motion range also through active positioning of the infant during feeding, playing, carrying. Demirbilek and Atayurt [16] described an “active stretching” modality in which passive stretching is associated with an active pressure constraint applied by the physical therapist. An alternative method consists in associating a light pressure, similar to a trigger [17]. Chon et al. described a variant for patients with MT with olive-like mass: the technique of myokinetic stretching [17], which is similar to the active stretching described by Demirbilek and Atayurt [16]. In myokinetic stretching, a sustained finger pressure is applied on the stretched SCM muscle to obtain a myofascial release. The authors think that it allows relaxing the muscle without side effects, such as local hypertonia, reflexive contraction, or pain. They also found that it decreased the treatment time to 53.59 ± 25.12 days, defined in this study as the time required for the disappearance of the olive-like mass, and not by the time needed to recover the maximum passive rotation range [18]. Finally, in a study not selected for this review, Lee compared (in two groups of 38 patients) manual stretching and postural education [19]. He did not find any significant difference between groups. We think that the two methods are complementary.
Timing and frequency of manual stretching
It is also important to find the best moment of the day for the treatment. Celayir proposed to the parents to do the exercises before each feed and up to eight times a day [20]. We propose systematically after the bath or after the nappy change. The stretching exercise frequency is a major element in MT management [18]. The treatment gives good results with a frequency of three times per week in infants younger than 6 weeks [19]. The different clinical trials recommend 5 to 7 sessions per week in total [6,16,17,20-22], with a treatment by a health professional three times per week [6,23,24]. This frequency led to 100% of resolution in most studies, if the treatment was initiated before the age of 3 months. The results were less good if the treatment was started after the age of 3 months [6,11,16,20,21]. As described by Ohman et al. [24], Emery [11], and Ryu et al. [6], we think that it is beneficial to entrust the treatment to a physical therapist. We conclude that manual stretching therapy for MT should be started in infants younger than 6 weeks of age with a frequency of three times per week. In infants older than 6 weeks of age, and particularly after 3 months, the frequency of five times per week seems to be unanimously accepted, especially if surgical treatment might be required, for instance for MT with a lump and a motion deficit higher than 30° [16].
Stretching can be repeated at home by the parents during the day. Comparison of the results obtained by Celayir [20] and Cameron et al. with very similar treatment protocols but different frequency (eight versus two sessions per day, respectively), suggests that it is better to repeat several times a large number of exercises to obtain better results [21]. This was confirmed by Demirbilek and Atayurt [16] (4-5 times per day). These authors suggest a more intensive protocol (15 repetitions, with three minutes of rest between sets, five times per day). It seems that at least thirty repetitions per day should be performed, and even more when the rotation deficit is higher than 30° and the treatment is initiated after the age of 3 months. He et al. recommended 100 repetitions [25]. These numbers highlight the importance of the parents’ participation.
Treatment duration
The total treatment duration is strongly correlated with the early diagnosis of MT [4,11,16,17]. According to the selected studies, it ranges from 3 to 7 months (Table 1). Overall, an early intervention (before 3 months of age) is more rapidly effective than a late intervention [4,6,9,11], and shortens the total duration of the treatment by ensuring a better result [4,11,16,17,19,26,27]. Two studies showed that a treatment started before 6 weeks of age gives significantly better results than interventions initiated later [19,28]. Petronic et al. also confirmed that if stretching is started within 1.5 months after birth (i.e., 6-7 weeks), the head and neck range of motion is recovered in 98% of patients [27]. Celayir reported a constant success rate (100%) associated with a shorter treatment (3.2 months) of daily sessions and a diagnosis before 4 months of age [20]. Manual stretching (by the physical therapist and the parents) should be stopped progressively. Upon MT resolution, defined by the recovery of the complete cervical range of motion, the infant should have at least one additional month of treatment to render the result stable in the long term [11,23].
MT monitoring
The effect of the stretching treatment should be monitored by evaluating the passive range of motion by flexing and rotating the head, and not on the basis of the infant’s spontaneous head posture, especially if assessed in supine position [13,19,24]. To complement the clinical examination, ultrasonography is the method of choice for the diagnosis/follow-up of CMT in infants [29], although its routine use is debatable [30]. The studies by Cheng et al. showed a good correlation between clinical examination and ultrasound images [9,31]. Ultrasonography allows an earlier and more precise diagnosis of torticollis [32], as well as an assessment of MT prognosis [33]. It allows determining the fibrosis coefficient and modulating the treatment intensity and repetitions accordingly. Therefore, the management can be adapted specifically to the MT severity, leading to an optimal programme.
Manual stretching complications
Intensive muscle stretching is not without complications. Indeed, SCM muscle rupture has been reported, as well as a case of clavicle fracture [34], although 90% of their patients obtained satisfactory results. Muscle “snapping” has been observed, particularly in studies where stretching was performed by the parents (12/126 in the study by Cameron et al.), with bruising or increased passive motion, suggesting muscle tear or rupture [21]. Some authors, for instance Flowers et al., described soft tissue micro-lesions that might reduce the motion range [35]. They suggested prolonged stretching at lower intensity to increase efficiently the motion range.
These complications do not seem to increase the need of surgery or affect the final outcome, and therefore they are a priori without danger [21,23]. However, Kaplan et al. recommended stopping the intervention if the infant resists or stops breathing [4]. Stretching must be pain-free and should not be continued if the infant feels pain because this could increase the muscle hypertonia [36].
Conclusion
In the presence of an infant with CMT, it is important to distinguish between PT, which does not need stretching, and MT, which greatly benefits from this conservative treatment. The outcome of manual stretching differs according to the torticollis type, the age of diagnosis/treatment initiation, and the parents’ adhesion to the treatment [15,37]. MT with olive-like mass are the most difficult to treat, although they are often detected earlier than the other MT. They also need generally a more intense and longer treatment. Starting the treatment before the age of 3 months with a frequency of three sessions per week with one or two operators seems to be the most effective option. We recommend associating stretching performed by a physical therapist with a programme of home exercises to be done by the parents, according to the protocol described by Emery [11]. Specifically, we suggest five stretching repetitions (10-second hold, and 10-second rest between repetitions) at least four times per day, with 3 to 7 sessions with a physical therapist per week, in function of the patient’s age, and the motion deficit severity.
Acknowledgement
The authors warmly thank Mrs. Elisabetta Andermarcher for the care she took in translating the text.
References
- Rogers GF, Oh AK, Mulliken JB. The Role of congenital muscular torticollis in the development of deformational plagiocephaly. Plast Reconstr Surg. 2009; 123: 643-652.
- Captier G, Dessauge D, Picot MC, Bigorre M, Gossard C, El Ammar J, et al. Classification and Pathogenic Models of Unintentional Postural Cranial Deformities in Infants: Plagiocephalies and Brachycephalies. Journal of Craniofacial Surgery. 2011; 22: 33-41.
- Cheng JC, Tang SP, Chen TM, Wong MW, Wong EM. The clinical presentation and outcome of treatment of congenital muscular torticollis in infants--a study of 1,086 cases. J Pediatr Surg. 2000; 35: 1091-1096.
- Kaplan SL, Coulter C, Fetters L. Physical therapy management of congenital muscular torticollis: an evidence-based clinical practice guideline: from the Section on Pediatrics of the American Physical Therapy Association. Pediatr Phys Ther. 2013; 25: 348-394.
- Boere-Boonekamp MM, Van der Linden-Kuiper LL. Positional preference: prevalence in infants and follow-up after two years. Pediatrics. 2001; 107: 339-343.
- Ryu JH, Kim DW, Kim SH, Jung HS, Choo HJ, Lee SJ, et al. Factors Correlating Outcome in Young Infants with Congenital Muscular Torticollis. Canadian Association of Radiologists journal = Journal association canadienne des radiologists. 2016; 67: 82-87.
- Laughlin J, Luerssen TG, Dias MS. Prevention and management of positional skull deformities in infants. Pediatrics. 2011; 128: 1236-1241.
- Lee YT, Yoon K, Kim YB, Chung PW, Hwang JH, Park YS, et al. Clinical features and outcome of physiotherapy in early presenting congenital muscular torticollis with severe fibrosis on ultrasonography: a prospective study. J Pediatr Surg. 2011; 46: 1526-1531.
- Cheng JC, Au AW. Infantile torticollis: a review of 624 cases. J Pediatr Orthop. 1994; 14: 802-808.
- Hwang JH, Lee HB, Kim JH, Park MC, Kwack KS, Han JD, et al. Magnetic resonance imaging as a determinant for surgical release of congenital muscular torticollis: correlation with the histopathologic findings. Ann Rehabil Med. 2012; 36: 320-327.
- Emery C. The determinants of treatment duration for congenital muscular torticollis. Phys Ther. 1994; 74: 921-929.
- Adamoli P, Pavone P, Falsaperla R, Longo R, Vitaliti G, Andaloro C, et al. Rapid spontaneous resolution of fibromatosis colli in a 3-week-old girl. Case reports in otolaryngology. 2014; 2014.
- Kim MY, Kwon DR, Lee HI. Therapeutic effect of micro current therapy in infants with congenital muscular torticollis. PM R. 2009; 1: 736-739.
- Brosseau L, Laroche C, Sutton A, Guitard P, King J, Poitras S, et al. Une version franco-canadienne de la Physiotherapy Evidence Database (PEDro) Scale : L’Échelle PEDro. Physiotherapie Canada. 2015; 67: 232-239.
- Kaplan SL, Coulter C, Sargent B. Physical Therapy Management of Congenital Muscular Torticollis: A 2018 Evidence-Based Clinical Practice Guideline From the APTA Academy of Pediatric Physical Therapy. Pediatr Phys Ther. 2018; 30: 240-290.
- Demirbilek S, Atayurt HF. Congenital muscular torticollis and sternomastoid tumor: results of nonoperative treatment. J Pediatr Surg. 1999; 34: 549-551.
- Chon SC, Yoon SI, You JH. Use of the novel myokinetic stretching technique to ameliorate fibrotic mass in congenital muscular torticollis: an experimenterblinded study with 1-year follow-up. Journal of back and musculoskeletal rehabilitation. 2010; 23: 63-68.
- La Flèche G, Labelle V, Rancourt C, Toulouse-Labrecque A-J, Trottier M-P. Recommandations portant sur la prise en charge optimale en physiothérapie de la clientèle pédiatrique atteinte de torticolis musculaire congénital. 2011.
- Lee I. The effect of postural control intervention for congenital muscular torticollis: a randomized controlled trial. Clinical rehabilitation. 2015; 29: 795- 802.
- Celayir AC. Congenital muscular torticollis: early and intensive treatment is critical. A prospective study. Pediatr Int. 2000; 42: 504-507.
- Cameron BH, Langer JC, Cameron GS. Success of nonoperative treatment for congenital muscular torticollis is dependent on early therapy. Pediatric surgery international. 1994; 9: 391-393.
- Schertz M, Zuk L, Zin S, Nadam L, Schwartz D, Bienkowski RS. Motor and cognitive development at one-year follow-up in infants with torticollis. Early Hum Dev. 2008; 84: 9-14.
- Cheng JC, Wong MW, Tang SP, Chen TM, Shum SL, Wong EM. Clinical determinants of the outcome of manual stretching in the treatment of congenital muscular torticollis in infants. A prospective study of eight hundred and twenty-one cases. J Bone Joint Surg Am. 2001; 83: 679-687.
- Ohman A, Nilsson S, Beckung E. Stretching treatment for infants with congenital muscular torticollis: physiotherapist or parents? A randomized pilot study. PM R. 2010; 2: 1073-1079.
- He L, Yan X, Li J, Guan B, Ma L, Chen Y, et al. Comparison of 2 Dosages of Stretching Treatment in Infants with Congenital Muscular Torticollis: A Randomized Trial. American journal of physical medicine & rehabilitation. 2017; 96: 333-340.
- Ohman A, Mardbrink EL, Stensby J, Beckung E. Evaluation of treatment strategies for muscle function in infants with congenital muscular torticollis. Physiother Theory Pract. 2011; 27: 463-470.
- Petronic I, Brdar R, Cirovic D, Nikolic D, Lukac M, Janic D, et al. Congenital muscular torticollis in children: distribution, treatment duration and outcome. European journal of physical and rehabilitation medicine. 2010; 46: 153-157.
- Tatli B, Aydinli N, Caliskan M, Ozmen M, Bilir F, Acar G. Congenital muscular torticollis: evaluation and classification. Pediatr Neurol. 2006; 34: 41-44.
- Haque S, Bilal Shafi BB, Kaleem M. Imaging of torticollis in children. Radiographics. 2012; 32: 557-571.
- Beasley SW. Routine ultrasonography is not indicated for sternomastoid tumours in infants. Journal of paediatrics and child health. 2015; 51: 233-234.
- Cheng JC, Metreweli C, Chen TM, Tang S. Correlation of ultrasonographic imaging of congenital muscular torticollis with clinical assessment in infants. Ultrasound Med Biol. 2000; 26: 1237-1241.
- Chen MM, Chang HC, Hsieh CF, Yen MF, Chen TH. Predictive model for congenital muscular torticollis: analysis of 1021 infants with sonography. Arch Phys Med Rehabil. 2005; 86: 2199-2203.
- Hu CF, Fu TC, Chen CY, Chen CP, Lin YJ, Hsu CC. Longitudinal follow-up of muscle echotexture in infants with congenital muscular torticollis. Medicine. 2017; 96: e6068.
- Leung YK, Leung PC. The efficacy of manipulative treatment for sternomastoid tumours. J Bone Joint Surg Br. 1987; 69: 473-478.
- Flowers KR, LaStayo PC. Effect of total end range time on improving passive range of motion. 1994. Journal of hand therapy: official journal of the American Society of Hand Therapists. 2012; 25: 48-54.
- Van Vlimmeren LA, Helders PJ, Van Adrichem LN, Engelbert RH. Torticollis and plagiocephaly in infancy: therapeutic strategies. Pediatric rehabilitation. 2006; 9: 40-46.
- Heidenreich E, Johnson R, Sargent B. Informing the Update to the Physical Therapy Management of Congenital Muscular Torticollis Evidence-Based Clinical Practice Guideline. Pediatr Phys Ther. 2018; 30: 164-175.