
Research Article
Austin J Musculoskelet Disord. 2021; 8(1): 1056.
The Role of Sonoelastography in the Diagnosis of Supraspinatus Tendinosis
Cavalieri S¹, Negroni D¹, Vinco A¹, Zagaria D¹*, Guglielmi R² and Carriero A¹
¹Department of Diagnosis and Treatment Services, Radiodiagnostics, Azienda Ospedaliero Universitaria Maggiore della Carità, Novara, Italy
²Istitute of Radiology, Spital Thurgau, AG Cantonel Hospital, Munsterlingen, Switzerland
*Corresponding author: Domenico Zagaria, Department of Diagnosis and Treatment Services, Radiodiagnostics, Azienda Ospedaliero Universitaria Maggiore della Carità, Novara, Italy
Received: March 15, 2021; Accepted: April 20, 2021; Published: April 27, 2021
Abstract
Purpose: The aim of the study was to evaluate the sensitivity and specificity of compressive elastosonography (“Strain Elastography”), integrated with the B-mode ultrasound examination, in supraspinatus tendinosis, using magnetic resonance imaging as the gold standard for diagnosis.
We also verified the intra-observer reproducibility of this elastosonographic method.
Materials and Methods: The supraspinatus tendons of 30 patients with shoulder pain and positive magnetic resonance imaging for tendinosis were examined with B-Mode ultrasound and compressive elastosonography in the absence of full-thickness tendon ruptures. At the same time, 30 control individuals, asymptomatic for shoulder pain and with a negative history of previous diseases affecting the rotator cuff, were examined with B-Mode ultrasound and compressive elastosonography.
The MRI exam was used as a gold standard reference exam for the diagnosis of tendinosis. At the “Strain” elastosonography the images were evaluated qualitatively with the color elastogram and quantitatively with the percentages of deformation of the supraspinatus tendon (Strain T), of the deltoid muscle used as reference tissue (Strain R) and of the SR/ST ratio (Ratio).
Results and Conclusions: The comparison between the group of individuals with tendinosis and the control group shows a statistically significant difference (p<0.05) for the Ratio values (SR/ST), respectively: 4.7 ± 0.14 vs 5.3 ± 0.19.
The different Ratio values indicate that the supraspinatus tendon, when compared with the deltoid muscle, is softer in patients with tendinosis than in the control group. As indicated by the statistical analysis of the ROC curve, the Ratio value of 4.8 represents the best sensitivity and specificity data (70% and 61% respectively). Elastosonography can therefore provide added value, compared to the conventional ultrasound examination only, to confirm the diagnosis of supraspinatus tendinosis. The analysis showed a low variance of results, due to its excellent intra-observer reproducibility (intraclass correlation coefficient = 0.86).
Future studies could aim to describe any changes in Stain T, Strain R and Ratio values in a cohort of individuals stratified by gender, age and BMI.
Keywords: Diagnostic imaging; Ultrasonography; Elastography; Share wave; Tendons; Muscle
Introduction
Rotator cuff tendinopathy is the leading cause of shoulder pain and the supraspinatus tendon is the most frequently involved [1,2]. Studies have shown that the prevalence of rotator cuff pathology fluctuates between 5% and 40% and that the prevalence increase is directly related to the age of the patients [3].
Shoulder ultrasound is a diagnostic imaging method widely used in clinical practice, which has the advantages of non-invasiveness, low cost and high tolerability.
In the literature there is a variability regarding the diagnostic accuracy of ultrasound in diagnosing tendinopathy of the rotator cuff tendons, this variability is influenced by the intrinsic limits of it and the experience of the clinician/sonographer [4].
Elastosonography is an ultrasound imaging technique capable of obtaining qualitative and quantitative information on tissues’ stiffness. It studies the physical properties of elasticity, based on the principle that an external force (e.g. manual compression with the probe) applied to a tissue induces a deformation of the tissue itself; the deformation induced is greater in softer tissues and lesser in harder tissues. This method was initially used in the diagnostic imaging of diseases of the liver, thyroid, breast, prostate, cervix and lymph nodes [5-9] and subsequently also in the study of the musculoskeletal system [10-13].
Currently two different techniques can be used in clinical practice: the “Strain” (compression) elastosonography and the “Shear Wave”. The “Strain” technique uses manual compression, while the “Shear Wave” technique requires the mechanical impulse to be generated by the ultrasound probe itself.
Both forms of elastosonography evaluate tissue stiffness, which is measured by Young’s modulus.
Young’s modulus can be calculated with the following equation:
E=σ/ε
where E is Young’s modulus measured in Pascals (Pa), σ is the externally applied force (“stress” measured in Pa), and ε is the strain, which is a unitless measure of the relative elongation of the tissue [14,15].
The “Strain Elastography” method was the first form of elastosonography to be developed with Ophir et al. in the early 1990s [16].
The operator exerts an external force through repeated compressions using the ultrasound probe.
The compressed tissue analysis can be visualized as a deformation map (elastogram) which allows a qualitative assessment of the tissue stiffness.
Most elastograms allow you to highlight different levels of stiffness (hard, intermediate and soft tissue) by means of a colour scale. It is also possible to carry out a quantitative analysis by placing ROIs that detect the percentage of deformation of the sampled tissue [17,18].
Few scientific research used compressive elastosonography for the evaluation of the supraspinatus tendon, highlighting how this method can provide additional data about the presence of tendinosis compared to the conventional ultrasound examination alone. Our study aims to confirm the possible added value of “Strain Elastography” in the diagnosis of supraspinatus tendinosis and to evaluate its intra-observer reproducibility by comparing it with shoulder MR, which we use as reference.
Materials and Methods
The cases were selected from symptomatic patients for shoulder pain with a diagnostic MRI study positive for degenerative changes of the supraspinatus tendon, in the absence of complete or focal full-thickness tendon ruptures. On the same day that the magnetic resonance was performed, the ultrasound evaluation in B-mode and the investigation with the compressive elastosonographic technique were carried out.
The controls were chosen from individuals asymptomatic for shoulder pain with a negative history of previous or current joint diseases, selected from the general population. This last group underwent B-mode ultrasound and elastosonographic examination but not magnetic resonance investigation.
Since our study protocol does not involve drugs or invasive procedures and we carried out diagnostic tests in compliance with the standards, there was no risk expected for the study subjects.
Nonetheless, each participant to the study received a face to face explanation about the study protocol and goals, was offered the chance to ask questions and then filled in and signed a consent form. Throughout the study period, each subject was treated according to the standards of Good Clinical Practice [19].
We used the following:
• Philips “Achieva” and “Ingenia” 1.5 Tesla high-field magnetic resonance devices;
• Toshiba “APLIO 500” ultrasound device with linear probe - type: PLT-1204BX 18LX7 - broadband and high frequency (from 7 to 18 Mhz) and module for the elastosonographic investigation in “Strain Elastography” mode;
• Microsoft “Excel” software for data archiving and analysis.
Study population
From February 2020 to August 2020, we enrolled patients who met the following inclusion criteria: 1) age eighteen or older; 2) for the case group: patients with shoulder pain; 3) for the case group: patients who were already due to perform an MR investigation of the shoulder and whose MR study showed tendon changes of the supraspinatus; 4) for the control group: asymptomatic subjects for shoulder pain and with no history of previous shoulder pathologies.
Subjects with the following criteria were excluded or not enrolled in the study: 1) previous surgery on the affected shoulder; 2) performing an MRI examination of the shoulder with intra-articular administration of paramagnetic contrast (arthro-MRI); 3) a diagnosis of neuromuscular and / or connective tissue diseases; 4) pregnancy or breastfeeding in progress; 5) for the case group: the presence of complete or focal full-thickness tear of the supraspinatus tendon, documented in a previous MRI study.
Patients included in the study underwent B-Mode ultrasound and “Strain” (compression) Elastosonography in order to confirm the pathological changes of the supraspinatus tendon found on magnetic resonance imaging and to collect the quantitative elastosonographic values of Strain T, Strain R and Ratio.
A basic patient’s history was also collected: gender, age, duration of shoulder pain expressed in months (if belonging to cases), shoulder affected by painful symptoms and dominance (right-handed or lefthanded).
The MR study was read by a senior radiologist with 15 years of experience in MSK radiology and acted as our gold standard for the diagnosis of supraspinatus tendinosis.
The MR study was performed in baseline conditions, following the standard protocols for the evaluation of the shoulder, by means of weighted sequences in DP, DP SPAIR and STIR, oriented on the three orthogonal planes of the space according to the shoulder’s anatomy. The following were considered as tendinosis findings: a hyperintensity of focal or diffuse intra-tendon signal in long TR sequences, such as from mucoid degeneration, associated with tendon thickening. Conversely, a focal full thickness tear or a complete tear of the tendon were considered as rupture findings [20].
For the ultrasound examination the patient was placed in a sitting position, with the arm behind the back and the elbow flexed 90 degrees, in order to better expose the supraspinatus moving it away from the acromion of the scapula, thus allowing a complete visualization of the tendon [21].
The ultrasound evaluation in B-Mode considered as signs of tendinosis: a thickening (increase in thickness versus healthy controls) with hypoechogenicity, sometimes inhomogeneous and a loss of the tendon’s fibrillar structure [22] (Figure 1).
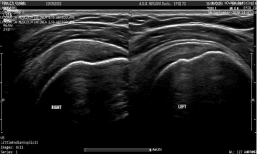
Figure 1:
During the B-Mode examination, the elastosonographic study was performed, according to the “Strain” (compression) technique, creating images along the long axis of the tendon.
The elastosonographic technique involves a qualitative analysis (“color elastogram”, which shows the more rigid tissues in blue and green, while the softer tissues in yellow and red) and a quantitative analysis, with the positioning of two ROIs (Region of Interest) with a diameter of 2 mm, one placed at the middle portion of the supraspinatus tendon (Strain T) and the other placed on the overlying deltoid muscle (Strain R), the latter used as reference tissue [23-24]. In this way we detected the following quantitative parameters:
• Strain T (ST), which corresponds to the percentage of deformation of the supraspinatus tendon.
• Strain R (SR), which corresponds to the percentage of deformation of the deltoid muscle.
• Ratio (Ratio), which corresponds to the numerical ratio between SR and ST (SR/ST).
For each individual we carried out the elastosonographic survey several times, including in the database the data of the values of Strain T, Strain R and Ratio of the five measurements that best met the accuracy criteria. The accuracy criteria of the measurements refer to the need to perform compressions with the probe at precise rhythms and intensities, the correctness of which is highlighted on the monitor when a pink frame is filled with a green rectangle. The numerical values (ST, SR and Ratio) are thus collected when the image is in the descending part of the sinusoidal curve, the latter indicating the compressions performed (Figure 2).
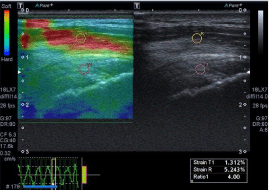
Figure 2:
Statistical analysis
A descriptive analysis of the variables under consideration was carried out. Using Student’s t-test, comparisons were made between independent groups. If the validity conditions of the test were not met, the corresponding non-parametic Mann-Withney-Wilcoxon test was used. Furthermore, the ROC curve of the elastosonographic test was calculated in order to provide data about the AUC, sensitivity and specificity of the test (in relation to the magnetic resonance used as gold standard).
To assess intra-observer reproducibility, a statistical analysis of the confidence intervals was performed with calculation of the Intraclass Correlation Coefficient (ICC). The test results were interpreted as <0.40 = poor; from 0.40 to 0.59 = fair; from 0.60 to 0.74 = good; ≥0.75 = excellent intra-observer reliability.
Results
From February 2020 to August 2020, 60 patients (30 cases and 30 controls) were enrolled, based on the inclusion and exclusion criteria.
The sample data was summarized in Table 1. The mean age of the total sample enrolled was 45.1 ± 15.7, median 42 (range 26-75) for men it was 45.7 ± 17.1 (median 45.4 with range 26-75) while for women it was 44 ± 13.8 (median 42 with range 27-66).
Tendinosis
Healthy
Patients
30
30
Men
18 (60%)
18 (60%)
Women
12 (40%)
12 (40%)
Mean age
Pain timing (months)57.8±9.9
14,7±23,632.2±8.1
-Tendinosis RM
30 (100%)
0 (0%)
Tendinosis US
30 (100%)
0 (0%)
Right side/Left side
16 (53.3%)/14 (46.7%)
15 (50%)/15 (50%)
Right-handed
30 (100%)
30 (100%)
Mean Strain T
l.l±0.04 (IC 95% 0.97; 1.12)
1.1±0.03 (IC 95% 1.02; 1.14)
Mean Strain R
4.6±0.14 (IC 95% 4.3;4.9)
5.5±0.14 (IC 95% 5.2; 5.8)
Mean Ratio
4.7±0.14 (IC 95% 4.4;5.0)
5.3±0.19 (IC 95% 4.8; 5.6)
Table 1:
The mean duration of shoulder pain in the case group was 14.7 ± 23.6 months. In detail, women underwent MRI after an average pain duration of 9.9 ± 10.8 months, while for men 17.8 ± 29.1 months.
None of the controls had shoulder pain, as a pre-requisite for inclusion in the group. In regard to the numerical values obtained from the elastosonographic investigation, in healthy controls, the variables Strain T, Strain R and Ratio respectively presented average values of 1.1 ± 0.03 (CI 95% 1.02; 1.14), 5.5 ± 0.14 (CI 95% 5.2; 5.8), and 5.3 ± 0.19 (95% CI 4.8; 5.6). In the cases, however, the mean values of Strain T, Strain R and Ratio were 1.1 ± 0.04 (95% CI 0.97; 1.12), 4.6 ± 0.14 (95% CI 4.3; 4.9) and 4.7 ± 0.14 (95% CI 4.4; 5.0). The case-control comparison between the variables using the t-Student test reported values of p<0.05 for Strain R and Ratio. Further details are available in Figure 3-5.
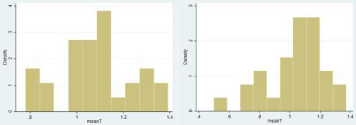
Figure 3:
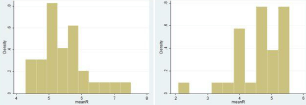
Figure 4:
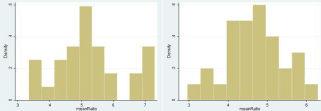
Figure 5:
The ROC curve of the diagnostic test ratio was obtained by elastosonography with MR imaging (Figure 6). This test showed an AUC of 0.67 (higher than the reference line of 0.5 with p<0.05, accuracy 67%). The best sensitivity and specificity values identified were respectively 0.70 and 0.61 with a cut-off ratio of 0.48. Although the statistical sample is of good potency (1-beta = 0.78), future studies may involve more subjects to perform an inference analysis on the population with greater accuracy.
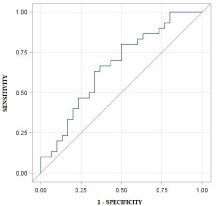
Figure 6:
Discussion
The aim of the study was to evaluate the added value of elastosonography in the diagnosis of supraspinatus tendinosis. All 60 individuals enrolled (30 cases and 30 controls) underwent ultrasound and elastosonographic examination: the data obtained with the “strain elastography” technique were analyzed by means of descriptive and inference statistics.
In all subjects, the tendon was sampled in correspondence with its middle portion, in order to make the data more homogeneous and to facilitate its reproducibility.
The deltoid muscle was chosen as the reference tissue (Strain R). Some authors use subcutaneous adipose tissue for the detection of Strain R, which often is the reference tissue for the elastosonography of glandular structures, for example for the breast [7,25-28]. Other authors prefer to use neighboring muscles (deltoid muscle) as a reference when evaluating the supraspinatus tendon, which are easy to sample even in lean subjects.
A study by Brage et al. “Ultrasonic strain elastography for detecting abnormalities in the supraspinatus tendon: an intra- and inter-rater reliability study” showed the reproducibility of the test applied to the deltoid muscle. In particular, the intra-observer and inter-observer reliability was excellent both for the raw values and for the ratios used in calculations.
Therefore, in agreement with Brage et al. In our study we preferred to use the deltoid muscle as reference tissue, which always has a sufficient thickness for correct sampling [23,24].
From a demographic point of view, the male/female ratio is comparable to the data reported in other studies [23,27].
The average age of the cases was on average higher than the average obtained in the study by Brage et al. However the standard deviation has a sufficient degree of overlap to consider this superimposable data [23].
The statistical analysis did not show correlations between the Strain R, Strain T and Ratio values in relation to gender or the duration of shoulder pain.
This study reported a statistically significant difference in the Ratio: the ratio between Young’s modulus of the reference tissue (deltoid muscle) and that of the supraspinatus tendon was lower in the group of cases (individuals with tendinosis diagnosed on MRI), compared to the control group consisting of healthy subjects.
The data of a lower rigidity of the supraspinatus tendon in subjects with tendinosis can be interpreted from a histopathological point of view: within the tendon there are phenomena of loss of collagen, infiltration of adipose tissue and an increase in water concentration [29].
The current data obtained using the deltoid muscle as Strain R are in line with other available studies that used the same protocol [30]. However, other published articles on the subject used equipment from different manufacturers compared to our study, obtaining numerical values that are not directly comparable.
The analysis of the variability of the confidence intervals has shown that there are no significant differences between the different samplings performed: there is therefore an excellent degree of intra-observer reproducibility of the method (intraclass correlation coefficient = 0.86).
The ROC curve (Figure 6) showed a statistically significant difference between the reference line with AUC of 0.5 and the AUC obtained by the “Strain Elastography” technique of 0.67 (p<0.05). Elastosonography is therefore able to identify tissue alterations in tendinosis. The test results on the borderline between the categories of low and moderate accuracy (0.5 = test not accurate, 0.5 to 0.7 poor accuracy, 0.7 to 0.8 low accuracy, 0.8 to 0.9 high accuracy test,> 0.9 excellent accuracy test), i.e. a diagnostic accuracy of 67%.
The elastosonographic investigation can therefore, if associated with the conventional ultrasound examination (B-mode), determine an increase in the sensitivity and specificity of the latter [24,31,32].
Statistical analysis recommended the Ratio value of 4.8 as the optimal cut-off, characterized by a sensitivity of 70% and specificity of 61%. In detail: a Ratio> 4.8 represents a rigid tendon, therefore indicative of a healthy tendon; conversely, a Ratio <4.8 would indicate a soft, tendinous tendon.
As reported by Mohtasib et al. conventional ultrasound examination compared with MRI shows sensitivity and specificity of 62% and 61% respectively for the identification of tendon changes in the supraspinatus, with a diagnostic accuracy of 62% [33].
According to the data collected in our study, elastosonography achieved a specificity value equal to the conventional ultrasound examination and a fairly higher sensitivity value. The use of this technique integrated with the B-mode exam can therefore increase the ability to identify tendinopathy. Future studies could investigate this aspect and investigate the diagnostic accuracy of the two tests performed together.
Study Limitations
The study has some limitations. In our study an ultrasound device was used: Toshiba “APLIO 500” with high frequency broadband linear probe (from 7 to 18 Mhz) and module for the elastosonographic investigation in the “Strain Elastography” mode. Further studies could compare different instruments (both in terms of different machines and probes) to report on any differences.
Of the various elastosonographic techniques, only the “Strain Elastography” was analyzed. The results therefore represent only a partial aspect of the elastosonography.
It was not possible to stratify the patients studied by demographic variables (e.g. age range, BMI, physical activity performed) or by the degree of tendon changes observed. Future studies should take these factors into account.
Conclusion
“Strain” (compression) elastosonography can be a useful complementary tool to confirm the diagnosis of tendinopathy of the supraspinatus, observed during a conventional ultrasound examination. A Ratio value of 4.8 represents an interesting cut-off in terms of sensitivity and specificity, respectively 70% and 61% when compared with the MRI study (gold standard) and makes the elastosonographic survey able to provide useful additional data for better diagnostic accuracy than the B-mode ultrasound examination alone.
Furthermore, the statistical analysis of the data shows a low variance of results, due to its excellent intra-observer reproducibility. Ideally, further studies could describe any changes in Stain T, Strain R and Ratio values in a cohort of patients stratified by gender, age, BMI and levels of physical activities.
Ethics Permissions
The study was conducted in compliance with the principles of the Declaration of Helsinki.
Abstract
References
- Vecchio P, Kavanagh R, Hazleman BL, King RH. Shoulder pain in a community-based rheumatology clinic. Br J Rheumatol. 1995; 34: 440-442.
- Lewis JS. Rotator cuff tendinopathy. Br J Sports Med. 2009; 43: 236-241.
- Wani Z, Abdulla M, Habeebullah A, Kalogriantis S. Rotator Cuff Tears: Review of Epidemiology, Clinical Assessment and Operative Treatment. Trauma. 2016; 18: 190-204.
- Chauhan NS, Ahluwalia A, Sharma YP, Thakur L. A Prospective Comparative Study of High Resolution Ultrasound and MRI in the Diagnosis of Rotator Cuff Tears in a Tertiary Hospital of North India. Pol J Radiol. 2016; 81: 491-497.
- Ferraioli G, Tinelli C, Zicchetti M, Above E, Poma G, Di Gregorio M, et al. Reproducibility of real-time shear wave elastography in the evaluation of liver elasticity. Eur J Radiol. 2012; 81: 3102-3106.
- Sebag F, Vaillant-Lombard J, Berbis J, Griset V, Henry JF, Petit P, et al. Shear wave elastography: a new ultrasound imaging mode for the differential diagnosis of benign and malignant thyroid nodules. J Clin Endocrinol Metab. 2010; 95: 5281-5288.
- Evans A, Whelehan P, Thomson K, McLean D, Brauer K, Purdie C, et al. Quantitative shear wave ultrasound elastography: initial experience in solid breast masses. Breast Cancer Res. 2010; 12: R104.
- Miyanaga N, Akaza H, Yamakawa M, Oikawa T, Sekido N, Hinotsu S, et al. Tissue elasticity imaging for diagnosis of prostate cancer: a preliminary report. Int J Urol. 2006; 13: 1514-1518.
- Palle L, Reddy MB, Reddy KJ, Kumari MV. Technical note: Real-time sonoelastography evaluation of Achilles tendon. Indian J Radiol Imaging. 2011; 21: 267-269.
- Brandenburg JE, Eby SF, Song P, Zhao H, Brault JS, Chen S, et al. Ultrasound elastography: the new frontier in direct measurement of muscle stiffness. Arch Phys Med Rehabil. 2014; 95: 2207-2219.
- Drakonaki EE, Allen GM, Wilson DJ. Ultrasound elastography for musculoskeletal applications. Br J Radiol. 2012; 85: 1435-1445.
- Hou SW, Merkle AN, Babb JS, McCabe R, Gyftopoulos S, Adler RS. Shear Wave Ultrasound Elastographic Evaluation of the Rotator Cuff Tendon. J Ultrasound Med. 2017; 36: 95-106.
- Baumer TG, Davis L, Dischler J, Siegal DS, van Holsbeeck M, Moutzouros V, et al. Shear wave elastography of the supraspinatus muscle and tendon: Repeatability and preliminary findings. J Biomech. 2017; 53: 201-204.
- Gennisson JL, Deffieux T, Fink M, Tanter M. Ultrasound elastography: principles and techniques. Diagn Interv Imaging. 2013; 94: 487-495.
- Domenichini R, Pialat JB, Podda A, Aubry S. Ultrasound Elastography in Tendon Pathology: State of the Art. Skeletal Radiol. 2017; 46: 1643-1655.
- Ophir J, Céspedes I, Ponnekanti H, Yazdi Y, Li X. Elastography: A Quantitative Method For Imaging The Elasticity of Biological Tissues. Ultrason Imaging. 1991; 13: 111-134.
- Klauser AS, Miyamoto H, Bellmann-Weiler R, Feuchtner GM, Wick MC, Jaschke WR. Sonoelastography: Musculoskeletal Applications. Radiology. 2014; 272: 622-633.
- Bercoff J, Tanter M, Fink M. Supersonic Shear Imaging: A New Technique For Soft Tissue Elasticity Mapping. Ieee Trans Ultrason Ferroelectr Freq Control. 2004; 51: 396-409.
- World Medical Association Declaration of Helsinki. Jama. 2013; 310: 2191- 2194.
- Risonanza Magnetica Dell’apparato Locomotore. Kaplan, Helms Et Al. Verduci Editore. 2006.
- Crdc F, Schiefer M, Mannarino P, Lacerda Ib, Machado Fjt, Farias Rgds, et al. Elastographic Analysis Of The Supraspinatus Tendon In Different Age Groups. Acta Ortop Bras. 2020; 28: 190-194.
- Échographie Musculoquelettique. Nicolas Sans Et Franck La Pégue - Elsevier Masson. 2009.
- Brage K, Hjarbaek J, Kjaer P, Ingwersen KG, Juul-Kristensen B. Ultrasonic strain elastography for detecting abnormalities in the supraspinatus tendon: an intra- and inter-rater reliability study. BMJ Open. 2019; 9: e027725.
- Brage K, Hjarbaek J, Boyle E, Ingwersen Kg, Kjaer P, Juul-Kristensen B. Discriminative and convergent validity of strain elastography for detecting tendinopathy within the supraspinatus tendon: a cross-sectional Study. Jses Int. 2020; 4: 310-317.
- Khodair SAZ, Ghieda U. Rotator Cuff Tendinopathy; Comparison between Conventional Sonography, Sonoelastography, and Mri In Healthy Volunteers And Patients With Shoulder Pain. In Ecr. 2016.
- Seo JB, Yoo JS, Ryu JW. The accuracy of sonoelastography in fatty degeneration of the supraspinatus: a comparison of magnetic resonance imaging and conventional ultrasonography. J Ultrasound. 2014; 17: 279-285.
- Seo J, Yoo J, Ryu J. Sonoelastography findings of supraspinatus tendon in rotator cuff tendinopathy without tear: comparison with magnetic resonance images and conventional ultrasonography. J Ultrasound 2015; 143-149.
- Prado-Costa R, Rebelo J, Monteiro-Barroso J. Ultrasound Elastography: compression elastography and shear-wave elastography in the assessment of tendon injury. Insights imaging. 2018; 9: 791-814.
- Lauser AS, Miyamoto H, Tamegger M, Faschingbauer R, Moriggl B, Klima G, et al. Achilles Tendon Assessed with Sonoelastography: Histologic Agreement. Radiology. 2013; 267: 837-842.
- Kocyigit F, Kuyucu E, Kocyigit A, Herek DT, Savkin R, Aslan UB. Investigation of biomechanical characteristics of intact supraspinatus tendons in subacromialimpingement syndrome: A Cross-Sectional Study with Real-Time Sonoelastog-Raphy. Am J Phys Med Rehabil 2016; 95: 588-596.
- Hajian-Tilaki K. Receiver Operating Characteristic (ROC) Curve Analysis for Medical Diagnostic Test Evaluation. Caspian J Intern Med. 2013; 4: 627-635.
- Yazigi Junior JA, Nicolao FA, Matsunaga FT, Archetti Netto N, Matsumoto MH, Tamaoki MJS. Sensitivity and specificity of ultrasonography in diagnosing supraspinatus lesions: a prospective accuracy diagnostic study. Sao Paulo Med J. 2018; 136: 292-297.
- Mohtasib RS, Alzahrani AM, Asiri YN, Rayes ZF, Alshaalan MA. Accuracy of shoulder ultrasound examination for diagnosis of rotator cuff pathologies: a single-center retrospective study. Ann Saudi Med. 2019; 39: 162-171.