
Case Report
Austin Neurol & Neurosci. 2016;1(1): 1002.
An Interesting Case of Neurofibromatosis Type 1 with Dysplastic Perineal Artery Vascular Lesion
Bajawi MA1#, Mzimbiri JM1,2#, Khamis IH³, Rashid KS1,2, Bajawi MA¹ and Fang LJ¹*
¹Department of Neurology, Xiangya Hospital of Central South University, China
²Department of Neurosurgery, Muhimbili Orthopedic and Neurosurgical Institute, Tanzania
³Department of Radiology, Ocean Road Cancer Institute, Tanzania
#Equally contributed
*Corresponding author: Fang Liang Juan, Department of Neurology, Xiangya Hospital of Central South University, 410008, Changsha, Hunan, China
Received: January 01, 2016; Accepted: January 28, 2016; Published: January 29, 2016
Abstract
Background: Neurofibromatosis type-1 is characterized by café au lait macules, cutaneous neurofibromas, and gliomas; development of plexiform neurofibromas; a high incidence of orthopedic complications; and relatively high incidence learning disabilities. Few studies have documented on the systemic vasculopathy complication(s) associated with this condition.
In this report, we present an interesting case-based review of a 48-year-old man who had perineal artery bleeding secondary to dysplastic vasculopathy which was managed by interventional artery embolism surgery. We discuss the clinical findings and management plan.
Case Description: A 48-year-old man known patient of NF-1 presented to us with a history of progressive increase in number of café au lait spot lesions, and tenesmus/pain in the perineum for two weeks prior to admission at our emergency department. The buttocks and scrotum were found to be tender and ecchymosed with bulla. His abdominal-pelvic Computerized Tomography (CT) scan findings revealed left perineum hematoma and effusions, and bilateral scrotum and penis sheath cavity hematocele or hydrops. His CT angiography done at another center reported perineal artery injury.
Conclusion: Our presented case demonstrated obvious dermatological lesions with dysplastic vascular complication but remarkably fewer ocular and neurological sequelae. We advise more studies to be done to focus on the cause(s) of arterial bleeding in patients with NF-1.
Keywords: Café au lait macules; Ecchymosis; Neufibromatosis type 1; Perineum hematoma; Vasculopathy
Abbreviations
CALM: Café au lait macules; CT: Computerized Tomography; CNS: Central Nervous System; INR: International Normalized Ratio; MRI: Magnetic Resonance Imaging; NF: Neurofibromatosis; OPG: Optic pathway glioma; PT: Prothrombin Time; WHO: World Health Organization
Introduction
Neurofibromatosis (NF) refers to a group of genetic disorder that primarily affects the growth of neural tissues. Occurring in two forms namely NF type 1 and NF type 2; the former which is also known as Von Recklinghausen’s disease, is the most common type and accounts for about 90% of all NF cases with a prevalence of 1 case per 3,000 births [1]. Only 50% of NF-1 patients have positive family history of the disease; the rest of the patients represent spontaneous mutation [2].
The neurofibromas represent the major cause of morbidity and mortality; they affect long portions of nerves, infiltrate the nerve and surrounding tissue, resulting in widespread disfiguration and mechanical complications. We report a case of a 48-year old patient with NF-1 and briefly discuss the clinical manifestations and management plan.
Case Report
Presentation and examination
A 48-year-old man, construction worker and a known patient of NF-1 presented to our emergency department with a history of itchy, sudden progressing increase in number of skin lesions, and pain in the perineum for two weeks prior to admission. The dull aching moderate pain was associated with tenesmus and numbness of the buttocks more on the left side. The patient reported that he had never experienced such symptoms before since he was newly diagnosed at the age of 6-year-old. He denied the history of hearing loss and poor vision. He also reported to enjoy the full psychosocial support from his family members including his father who has similar condition like him.
On physical examination the patient showed an acutely ill appearance, but oriented and a febrile. His Rosenbaum V/A was found to be 6/24. Evaluation of his mathematical calculation was normal.
On local examination, the patient had multiple café au lait macules located at his back. His buttocks were tender, ecchymosed and with bulla (Figure 1). Digital Rectal Examination (DRE) revealed no palpable mass in the rectum.
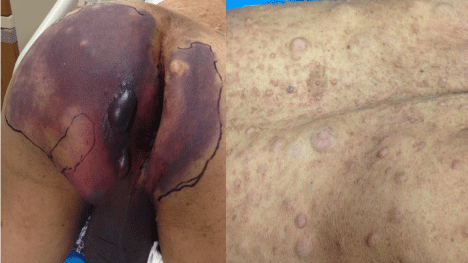
Figure 1: Left: Note the ecchymosis of the scrotum and buttocks with bulla.
Right: The most common neurocutaneous lesions associated with NF-1, that
is, café au lait macules.
Radiological and laboratory findings
His full blood picture was essentially normal. Patient was also investigated for his bleeding profile including PT, APTT and INR which were found to fall within normal range with slightly increased D-dimer. Results of urinalysis revealed positive hematuria (+++), and negative proteinuria, however his renal and liver function test were normal. Serology for HIV/AIDS, hepatitis B and C and syphilis were negative.
His chest X-ray film was normal. Abdominal and pelvic Computerized Tomography (CT) scan imaging revealed multiple irregular soft tissues with strip signs around it. The findings were suggestive of the left perineum hematoma and effusions, and bilateral scrotum and penis sheath cavity hematocele or hydrops (Figure 2). Prior to admission in our emergency department, the patient also reported that he underwent a diagnostic pelvic CT angiography at another hospital which revealed blood vessel injury.
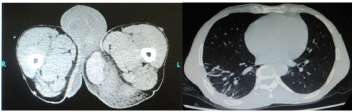
Figure 2: Left: showing significant swelling of the soft tissue of the left hip
and perineum with an underlying round shaped, slightly high signal focus
region which was measured at about 113 × 61 mm in coronal position and
without significant changes after the enhancement. Features are suggestive
of perineum hematoma. Right: Normal chest and pelvic x-ray.
The patient was treated with I.V vancomycin, vitamin K1 and hemocoagulase, and Ibuprofen. He also underwent an interventional arterial embolism surgery for arresting the bleeding.
The patient was discharged from our emergency department in good condition. His follow up was unremarkable.
Discussion
Clinical characteristics
NF-1 is characterized by café au lait macules, cutaneous neurofibromas, and gliomas; development of plexiform neurofibromas; a high incidence of orthopedic complications; and relatively high incidence learning disabilities.
Patients are born with the disorder however clinical manifestations are age-dependent. One study demonstrated that NF1 can be diagnosed by six (6) years of age in most cases by routine physical examination with special attention to the disease –associated skin stigmata [2]. This correlates to the findings of the aforementioned case.
Dermatologic disorders
Our presented case demonstrated two (2) of the most common skin manifestations of NF-1, Café Au Lait Macules (CALM) and peripheral cutaneous neurofibromas (also known as fibroma molluscum), yet possessed neither ocular nor learning disabilities. CALM are well circumscribed, light to dark brown macules of varied size. Peripheral cutaneous neurofibromas present as soft, flattened, or pedunculated skin lesions of varying size and number, most commonly occurring on the trunk. These lesions also tend to be progressive in nature, similar to CALM.
CNS features
One of the most common and characteristic brain abnormalities in NF-1 is Optic Pathway Glioma (OPG), occurring in about 20% of patients of NF-1[3]; in fact, presence of bilateral OPG is considered pathognomonic. Its manifestations include decreased visual acuity or loss of color vision and visual field defects. The patient highlighted in this case report demonstrated none of the aforementioned symptoms as documented on his CT scan report that was done six years ago.
Vasculopathy
Renal and gastrointestinal systems are frequently involved. Secondary hypertension is seen in up to 30% of patients with NF1 [4], and can lead to significant morbidity if not recognized early. On study reported the common locations of arterial abnormalities; aorta (22%), renal arteries (16%), mesenteric (16%), extracranial carotidvertebral arteries (13.5%), intracranial (5%), subclavian-axillary (4%), ileofemoral (4%) and secondary vascular compression caused by peripheral nerve sheath tumors [5]. We think that the aforementioned case had dysplastic vascular lesions of perineal artery which resulted into perineal hematoma. We ruled out prolonged constipation as a cause of his perineal bleeding.
Diagnosis
Thorough patient history, complete physical examination, including full neurological and/or ophthalmological examinations, and radiological imaging is important in the diagnosis and appropriate treatment of any patient diagnosed with NF-1. Criteria for diagnosis of NF-1 have been established by NIH Consensus Development Committee. A firm diagnosis of NF-1 may be made when a patient exhibit 2 or more of the following: (1) 6 or more café au lait macules, >5mm before puberty, >15mm after puberty; (2) 2 or more neurofibromas; (3) 1 or more plexiform neurofibromas; (4) axillary or inguinal freckling; (5) optic glioma; (6) 2 or more iris hamartomas; (7) 1 or more distinctive bone lesions (eg, sphenoid dysplasia, pseudo arthrosis); and (8) a first-degree relative who also meets these diagnostic criteria for NF-1.
MRI precedes CT in diagnosing NF-1 associated tumors because of its superior soft tissue contrast resolution. However, if the tumor is located on the bone or causing bone complications, then the CT scan becomes the best modality for diagnosis. Vascular evaluation with MRA is preferred as the screening modality for vascular anomalies. CTA should be considered only if MRA is vague. An interventional CTA can be useful as both a diagnostic and therapeutic after an initial screening with non-invasive imaging.
Complications
Several complications associated with NF-1 have been reported as a result of clinical variability of the manifestation of the disease. They range from ocular and neurological complications secondary to neoplasia, dysplasia and structural deformity. These include visual impairment, raised Intracranial Pressure (ICP), hypopituitarism, and strabismus due to OPG. Those due to mass effect may include headache, hydrocephalus and seizures for intracranial tumors; while pain, myelopathy or radiculopathy, and scoliosis are such complications due to spine/spinal cord involvement.
Treatment
Surgery is indicated in special situations like large disfiguring tumors and pressure on adjacent structures. Other neural tumors in patients with NF-1 should be managed in the same manner as in the general population; focal, resectable, and symptomatic lesions.
If tumors are unresectable chemotherapy and/or radiotherapy may be appropriate. When malignant degeneration is suspected, biopsy with or without internal decompression may be indicated and followed up with serial imaging (MRI/CT). Laser surgery has been shown to successfully remove those lesions that are painful, enlarging rapidly, or arising in an area prone to irritation, such as the belt line.
Other management modalities include psychological support, pain management and family education.
Conclusion
In summary, we have presented a case of NF-1 and discussed his clinical findings in relation to the relevant literature. Our presented case had obvious dermatological lesions with dysplastic vascular lesion complication. We advise more studies to be done to focus on the cause(s) of arterial bleeding in patients with NF-1.
Acknowledgement
Our sincere gratitude goes to Dr. Xiao Fang, PhD, and Vice Director of Neurology department at Xiangya hospital of CSU for his constructive criticism, valuable comments and tireless efforts on discussing the case.
References
- Gajeski BL, Kettner NW, Awwad EE, Boesch RJ. Neurofibromatosis type I: clinical and imaging features of Von Recklinghausen’s disease. J Manipulative Physiol Ther. 2003; 26: 116-127.
- Nandigam K, Mechtler LL, Smirniotopoulos JG. Neuroimaging of neurocutaneous diseases. Neurol Clin. 2014; 32: 159-192.
- Blazo MA, Lewis RA, Chintagumpala MM, Frazier M, McCluggage C, Plon SE. Outcomes of systematic screening for optic pathway tumors in children with Neurofibromatosis Type 1. Am J Med Genet A. 2004; 127A: 224-229.
- Zinnamosca L, Petramala L, Cotesta D, Marinelli C, Schina M, Cianci R, et al. Neurofibromatosis type 1 (NF1) and pheochromocytoma: prevalence, clinical and cardiovascular aspects. Arch Dermatol Res. 2011; 303: 317-325.
- Oderich GS, Sullivan TM, Bower TC, Gloviczki P, Miller DV, Babovic- Vuksanovic D, et al. Vascular abnormalities in patients with neurofibromatosis syndrome type I: clinical spectrum, management, and results. J Vasc Surg. 2007; 46: 475-484.