Case Report
Austin J Endocrinol Diabetes. 2014;1(3): 1001.
Endoscopic Repair of Delayed Cerebrospinal Fluid Leakage 10 Years after Gamma Knife Radiosurgery for Pituitary Adenoma: A Case Report
Masayuki Iwato1, Yasuhiko Hayashi1*, Daisuke Kita1, Issei Fukui1, Tadao Miyamori2 and Junichiro Hamada1
1Department of Neurosurgery, Graduate School of Medical Science, Kanazawa University, Kanazawa, Japan
2Division of Neurosurgery, Toyama Municipal Hospital, Toyama, Japan
*Corresponding author: Yasuhiko Hayashi, Department of Neurosurgery, Graduated School of Medical Science, Kanazawa University, 13-1 Takaramachi, Kanazawa, Ishikawa, 920-8640, Japan
Received: February 28, 2014; Accepted: April 06, 2014; Published: April 08, 2014
Abstract
Cerebrospinal fluid (CSF) leakage is a major complication during and after transsphenoidal surgery (TSS) for pituitary tumors. To prevent postoperative CSF leakage causing meningitis, sellar floor reconstruction with artificial or autologous materialsis recommended. Mucosa in the sphenoid sinus can cover the CSF fistula or materials used for the sellar floor reconstruction in the perioperative period, resulting in the disappearance of CSF leakage. In this case, a 60-year-old woman presented with CSF leakage. She had undergone TSS for a large pituitary macroadenoma 21 years prior and gamma knife radiosurgery was delivered for a residual tumor 11 years after the TSS. Endoscopic surgical repair of the CSF leakage was successfully performed. Although delayed CSF leakage is very rare in patients who did not experience CSF leakage in the perioperative period after TSS, it can occur if the residual pituitary adenoma was treated with irradiation. This mucosal atrophy due to irradiation was considered the possible cause for the delayed CSF leakage in our case. Thus, endoscopic surgery is useful for the detection and repair of the CSF fistulas.
Keywords: Transsphenoidal surgery, Cerebrospinal fluid leakage, Endoscope, Radiosurgery.
Abbreviations
CSF: Cerebrospinal Fluid; GKS; Gamma Knife Radiosurgery; MRI; Magnetic Resonance Imaging; TSS; Transsphenoidal Surgery.
Introduction
Advances in endoscopic procedures have increased the surgical indications for the various intracranial lesions, mainly because they provide a wide–angled view and decreased surgical trauma [1,2]. Endoscopic surgery is also increasingly used for transsphenoidal surgery (TSS) on pituitary tumors. However, a major complication of TSS is cerebrospinal fluid (CSF) leakage, which is reported to occur in 0.4–9.6% of cases regardless of the introduction of the endoscope [3–5]. It tends to occur within a week after TSS, and in most of the patients, it rarely occurs if CSF leakage has previously disappeared spontaneously or with the aid of surgical procedures [3,6]. Many materials available for sellar floor reconstruction have been reported, including autologous fat, muscle and fascia, vascularized mucosal flaps, or artificial buttress materials and titanium mesh [7–11].
Here, We present the case of a patient with extremely delayed CSF leakage, occurring 21 years after her initial TSS for a pituitary macroadenoma and 10 years after gamma knife radiosurgery (GKS) for its local recurrence. We discuss the mechanisms underlying the development of delayed CSF leakage and the endoscopic procedures applied for fistula repair.
Case Report
When the patient was 33 years old, she manifested amenorrhea and galactorrhea. Six years later, she noticed a disturbance in her visual acuity and bilateral temporal hemianopsia. Magnetic resonance imaging (MRI) showed a tumor measuring 30 mm in diameter in the sella turcica and extending into the bilateral cavernous sinus and the suprasellar region. TSS for the pituitary adenoma was performed in a local hospital, and it resulted in the partial removalof the tumor. Postoperatively, there was no CSF leakage, and her visual symptoms disappeared. When she was 44 years old, MRI showed regrowth of the residual tumor into the sphenoid sinus and clivus. She underwent GKS (20Gy; prescription isodose 50%) 11 years after the first operation (Figure 1A, B). Follow–up MRI revealed significant shrinkage of, and multiple cystic changes inside, the tumor at the base of the sellar floor (Figure 1C).
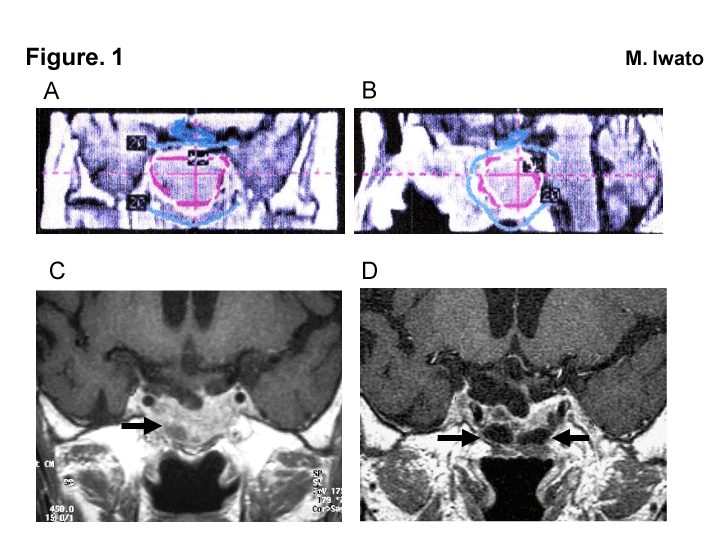
Figure 1: (A) Coronal and (B) sagittalMRI sections showing the dose planning for gamma knife radiosurgery to address tumor recurrence. Note that the 50% prescription isodose center (red circle) covered the sellar floor and the sphenoid sinus. (C) MRI performed 5 years after the gamma knife radiosurgery showing multiple small cystic changes (arrow) in the sphenoid sinus,and the descent of the diaphragmasellae into the sellar cavity. (D) MRI pergormed before the endoscopic repair of the CSF leakage. Note the large and small cystic changes in the sphenoid sinus (arrows). The diaphragmasellae has descended into the sellar cavity, and the adenoma has significantly shrunk.
At the age of 60, she felt the flow of liquid into her pharynx and frequent fluid discharge from her right nostril. She was referred to our hospital, and radioisotope cisternography clearly revealed CSF leakage into the sphenoid sinus. Despite her CSF leakage, she had no signs or symptoms of bacterial meningitis.
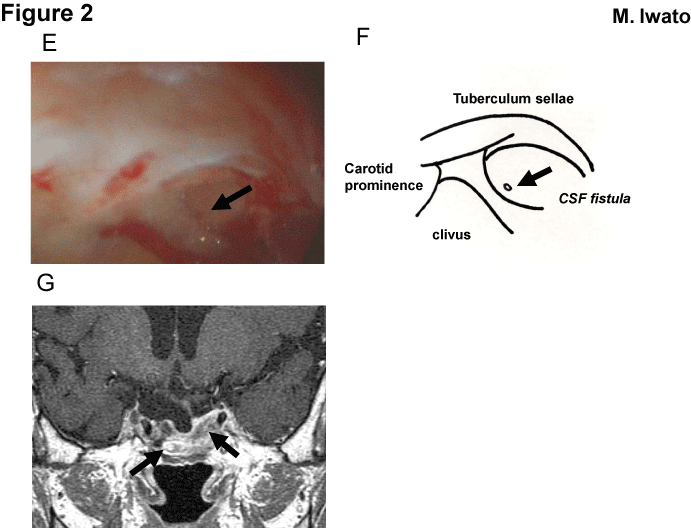
MRI revealed a remarkable empty sella without tumor recurrence. T1–weighted MRI showed hypointense area in the sphenoid sinus, representing fluid retention (Figure 1D). An endoscopic endonasal TSS was performed to repair the CSF fistula causing CSF leakage. The sphenoid sinus mucosa was thin and degenerated. There was a small fistula in the upper part of the sellar floor, with clearly recognizable CSF coming up from the fistula under an angled rigid–endoscope observation (Figure 2E, F). The defect was carefully covered with a polyglycolic acid sheet and fibrin glue. The sella turcica was packed with abdominal fat and fascia, and covered with a nasal pedicled mucosal flap. Valsalva maneuver was performed to confirm the CSF leakage repair. Lumbar spinal drainage was conducted for 5 days after the operation. Postoperatively, her symptoms of CSF rhinorrhea disappeared immediately. Follow–up MRI showed no signs of fluid collection in the sphenoid sinus (Figure 2G). Five years after the repair of the CSF fistula, she has still not experienced further episodes of CSF leakage.
Figure 2: (A) Intraoperative photograph showing thin and degenerated nasal mucosa and a small fistula at the upper part of the sellar floor (arrow). (B) Schematic findings of the intraoperative photograph in Figure 2A.(C) MRI performed 6 months after the endoscopic repair shows the disappearance of cystic changes in the sphenoid sinus (arrows). The sphenoid sinus was packed with an autologous fat graft.
Discussion
We define “delayed” CSF leakage after TSS as occurring more than 1 year after the operation. Two previous case reports described patients with delayed CSF leakages occurring 1.5 and 10 years after TSS [3,5] (Table 1). One patient had taken bromocriptine for 1 year [3]. The other underwent GKS 6 months after TSS; this patient manifested delayed CSF leakage and subsequent recurrent bacterial meningitis [5]. In both cases,the patients were treated by the repair of their CSF fistulas with microscopic TSS.
CaseNo.
Age (yrs), Sex
initial tumor size(mm)
Histology
Duration after TSS
Dopamine agonist administration
Post-operative irradiation /duration after irradiation
Treatment for CSF leakage
outcome /follow up periods
Case13)
ND
ND
PRL
1.5Y
yes
no
mTSS
GR/ND
Case25)
35, F
ND
PRL
10Y
no
yes (GKS)/9.5Y
mTSS
GR/1.5Y
present case
60, F
34
NF
21Y
no
yes (GKS)/10Y
eTSS
GR/6Y
Table 1: Delayed CSF leakage after TSS for pituitary adenoma reported previously.
Our patient had no history of bromocriptine administration or bacterial meningitis and her delayed CSF leakage occurred 21 years after her first TSS for a pituitary macroadenoma and 10 years after GKS for tumor recurrence.
The mechanisms underlying delayed CSF leakage have been reported by several authors. Ciric et al [3] suggested that the diaphragma sellae descends into the sella turcica after the removal or shrinkage of a large pituitary tumor, and that delayed CSF leakage is a result from continuous CSF pulsatile forces, disrupting theregeneration of the nasal mucosa covering the sellar floor, which is damaged by irradiation.
The side effects of irradiations of the nasal mucosa have been addressed by several authors. Langendijk et al described that acute inflammation and subsequent chronic mucosal atrophy are among the side effects of radiation therapy, which can persist many years after the radiation therapy itself [12]. In rabbits subjected to irradiation, the nasal mucosa manifested degenerative changes and epithelial metaplasia on electron microscopic images [13]. Lou et al reported these degenerative pathological findings in a patient with nasopharyngeal carcinoma who had undergone irradiation treatment 23 years earlier [14]. Pathological findings reflecting the extremely long–term effects of irradiation included epithelial metaplasia,collagen–fibers deposition, a reduction in cytoplasmic volume, and cellular vacuolation [14], suggesting that irradiation may be a risk factor for onducing CSF leakage. In our patient, MRI showed significant shrinkage of the tumor after GKS. We posit that mucosal degeneration in the sphenoid sinus arose as a direct long–term effect of the GKS she had received.
The most common methods for preventing postoperative CSF leakage are autologous bone placement in the epidural space, the packing of autologous fat tissue and fascia, and the application of fibrin glue in the sella turcica and sphenoid sinus [6–11]. In order to avoid CSF leakage, biological nasal mucosa regeneration is essential. In both previously reports of patients with delayed CSF leakage, the leakage points were located on the sellar floor; appropriate mucosal coverage over the sellar floor avoided further episodes of CSF leakage. To detect the leakage site exactly in our patient, endoscopic exploration was also very useful. Despite the use a microscope to detect the exact location of the CSF fistula in our case, we did not succeed because the fistula was hidden in a blind corner of the sellar floor. Intraoperative observation with an angled–rigid endoscope enabled us to inspect a large, well–illuminate area and may be to be superior to microscopic observation for the detection and repair of a leakage point. We believe an endoscopic procedure is the best choice for achieving complete repair of a CSF fistula.
Conflict of Interest Disclosure
All authors have no conflict of interest.
References
- Cappabianca P, Cavallo LM, Colao A, Del Basso De Caro M, Esposito F. Endoscopic endonasal transsphenoidal approach: outcome analysis of 100 consecutive procedures. Minim Invasive Neurosurg. 2002; 45: 193-200.
- Kitano M, Taneda M. Subdural patch graft technique for watertight closure of large dural defects in extended transsphenoidal surgery. Neurosurgery. 2004; 54: 653-660.
- Ciric I, Ragin A, Baumgartner C, Pierce D. Complications of transsphenoidal surgery: results of a national survey, review of the literature, and personal experience. Neurosurgery. 1997; 40: 225-236.
- Laws ER Jr, Thapar K. Surgical management of pituitary adenomas. Baillieres Clin Endocrinol Metab. 1995; 9: 391-405.
- Ogawa Y, Tominaga T. Delayed cerebrospinal fluid leakage 10 years after transsphenoidal surgery and gamma knife surgery - case report - . Neurol Med Chir (Tokyo). 2007; 47: 483-485.
- Esposito F, Dusick JR, Fatemi N, Kelly DF. Graded repair of cranial base defects and cerebrospinal fluid leaks in transsphenoidal surgery. Neurosurgery. 2007; 60: 295-303.
- Cappabianca P, Cavallo LM, Colao A, de Divitiis E. Surgical complications associated with the endoscopic endonasal transsphenoidal approach for pituitary adenomas. J Neurosurg. 2002; 97: 293-298.
- Cappabianca P, Cavallo LM, Mariniello G, de Divitiis O, Romero AD. Easy sellar reconstruction in endoscopic endonasal transsphenoidal surgery with polyester-silicone dural substitute and fibrin glue: technical note. Neurosurgery. 2001; 49: 473-475.
- Cappabianca P, Cavallo LM, Valente V, Romano I, D'Enza AI. Sellar repair with fibrin sealant and collagen fleece after endoscopic endonasal transsphenoidal surgery. Surg Neurol. 2004; 62: 227-233.
- Dusick JR, Esposito F, Kelly DF, Cohan P, DeSalles A. The extended direct endonasal transsphenoidal approach for nonadenomatous suprasellar tumors. J Neurosurg. 2005; 102: 832-841.
- Seiler RW, Mariani L. Sellar reconstruction with resorbable vicryl patches, gelatin foam, and fibrin glue in transsphenoidal surgery: a 10-year experience with 376 patients. J Neurosurg. 2000; 93: 762-765.
- Langendijk JA, Doornaert P, Verdonck-de Leeuw IM, Leemans CR, Aaronson NK . Impact of late treatment-related toxicity on quality of life among patients with head and neck cancer treated with radiotherapy. J Clin Oncol. 2008; 26: 3770-3776.
- Ohashi Y, Nakai Y, Ikeoka H, Koshimo H, Esaki Y. Functional and morphological pathology of the nasal mucosa after x-ray irradiation. Clin Otolaryngol Allied Sci. 1988; 13: 435-446.
- Lou PJ, Chen WP, Tai CC. Delayed irradiation effects on nasal epithelium in patients with nasopharyngeal carcinoma. An ultrastructural study. Ann Otol Rhinol Laryngol. 1999; 108: 474-480.