
Research Article
Ann Nurs Res Pract. 2017; 2(3): 1024.
Intrapartum Administration of Synthetic Oxytocin and Downstream Effects on Breastfeeding: Elucidating Physiologic Pathways
Cadwell K* and Brimdyr K
Healthy Children Project, Inc., The Center for Breastfeeding, USA
*Corresponding author: Karin Cadwell, The Center for Breastfeeding, Healthy Children Project, Inc. 327 Quaker Meeting House Road, East Sandwich, MA 02537, USA
Received: November 30, 2017; Accepted: December 18, 2017; Published: December 26, 2017
Abstract
The importance of breastfeeding as a public health priority has increased as new research reinforces the health benefits to both mother and nursling, even continuing years after weaning. However, many women do not nurse as long as they intend. Birth practices such as labor medications and the routine separation of mother and baby are two of the several intrapartum influences on breastfeeding outcomes. This paper seeks to elucidate the physiologic mechanisms affecting breastfeeding outcomes of the commonly administered intrapartum drug, synthetic oxytocin.
A modified ascending, link tracing methodology was used to identify studies about breastfeeding and human lactation which describe possible physiologic pathways related to the intrapartum use of synthetic oxytocin on breastfeeding outcomes. A cascade model was constructed with the findings of three physiologic pathways: dysregulation of the maternal OT system, crossing of the fetal blood brain barrier, and uterine hyper stimulation. Downstream negative effects related to breastfeeding include decreased maternal endogenous oxytocin, increased risk of negative neonatal outcomes, decreased neonatal rest during the first hour with the potential of decreasing the consolidation of memory, decreased neonatal pre-feeding cues, decreased neonatal reflexes associated with breastfeeding, maternal depression, somatic symptoms and anxiety disorders. No positive relationships between the administration of synthetic oxytocin and breastfeeding were found. Practices that could diminish the nearly ubiquitous practice of inducing and accelerating labor with the use synthetic oxytocin should be considered when evaluating interventions that affect breastfeeding outcomes.
Keywords: Breastfeeding; Oxytocin; Pitocin; Labor; Synthetic oxytocin
Introduction
The United States’ Healthy People Goals have included measurements of breastfeeding rates since their inception in the late 1970’s. However, only since a United States’ government funded research analysis of breastfeeding’s relationship to maternal and child health outcomes in 2007 [1] was published, have credible cost estimates of the contribution of suboptimal breastfeeding been published [2,3]. The most recent calculation [4] includes not only the money spent on nine pediatric and five maternal diseases, (billions of dollars), but also the calculation that for every 597 women who optimally breastfeed in the United States, one maternal or child death could be prevented.
The recently published document, Recommendations for Preventative Services for Women Final Report to the US. Department of Health and Human Services, Health Resources & Services Administration [5] includes, as one of the preventive measures for improving public health for women, their families and communities, improving access to breastfeeding services and supplies. The 2017 copyright holder is the American College of Obstetrics and Gynecologists (ACOG), although an interdisciplinary team, including government representatives, took part in the process of developing the document. Interventions both at the individual level (education, counseling and mother-to mother support, for example) and system level (such as the Baby-Friendly Hospital Initiative, training of health professionals, practices such as skin-to-skin care and rooming-in) are cited as having been shown to be effective in increasing breastfeeding initiation and intensity.
Of note is the absence from the report of intrapartum interventions (such as continuous labor support by doulas or birth attendants) that have been demonstrated to have a positive influence on breastfeeding outcomes [6]; the recommendations also do not address intrapartum medications that have been shown to have a negative influence on breastfeeding outcomes. This study seeks to identify the physiological pathways and clarify possible downstream effects on breastfeeding of one intrapartum drug, synthetic oxytocin.
Background synthetic oxytocin (synOT) is a manufactured product identical to endogenous oxytocin (OT). After being synthesized by Vincent du Vigneaud, who won the Nobel Prize in chemistry in 1955 in part for this work, Sandoz Pharmaceuticals made the commercial product available. Research studies using synOT were published in the following years and the drug became integrated into clinical practice as an induction and augmentation agent in labor (via continuous IV infusion), to reduce blood loss after birth (via IM injection), and to stimulate milk ejection (as a nasal spray).
Over time, synOT came to be understood not just as a drug to be administered in cases of obstetric crisis, but also as an elective management tool, useful in conforming women’s bodies to a predetermined timeline. The use of synOT in obstetrics integrated smoothly into the US. Post-World War II medicalized concept of birth and breastfeeding; it could make women’s non-compliant physiologic processes fit into an industrial model [7]. In this model, the clock and calendar are used to dictate the precise duration of pregnancy (the expected date the baby should be born, the due date”), the tolerable length of each stage of labor, the total number of allowable hours of labor, how long each breastfeeding should last, the number of breast feedings each day, how much time there should be in-between feedings and when weaning should occur.
The Institute for Safe Medication Practices (ISMP) has listed IV oxytocin (synOT) as one of the 12 medications most implicated in harmful errors in acute care hospitals [8]. According to a survey of liability cases, approximately 50% of paid liability claims affecting maternity services involve alleged misuse of oxytocin” [9]. In addition, synOT has received a Black Box” or Boxed” warning (the strongest caution the United States Food and Drug Administration (FDA) can give) which reads “Not for Elective Labor Induction: not indicated for elective labor induction since inadequate data to evaluate benefit vs. risk; elective induction defined as labor initiation without medical indications’ [10]. In spite of cautions, labor induction rates in the United States have been increasing since the early 1990s to 23.8% nationally [11], however in a study of 19 US. hospitals, the induction rate was reported to be 42.9% for first time mothers and 31.8% for multiparas [12]. The rate of synOT used for augmentation is estimated to be between 50 and 60% [13], with highest use in conjunction of an epidural for pain management. In addition, women in the United States are to be administered an IM injection of synOT after the baby is born if they do not have an IV in place, according to the Association of Women’s Health, Obstetric and Neonatal Nurses’ (AWHONN) guidelines [14], suggesting that there is a near universal exposure to synOT for birthing women in the United States.
The hormone oxytocin (from the Greek meaning swift birth”) has several functions beyond the obvious one: the mediation of uterine contractions. Oxytocin is predominantly produced in the hypothalamus, stored and secreted in a periodic bolus fashion [15] or pulses from the posterior pituitary. Oxytocin receptors (OTRs) are found on the smooth muscle cells in the uterus and the breast, where they work to contract the uterine muscles during labor and birth and the myoepithelial cells in the breast to eject milk. The central nervous system, including the spinal cord and the brain, also has OTRs; the hippocampal clusters of OTRs in the brain are thought to be integral in facilitating social learning, memory consolidation and bonding.
Method
A prior study [16] demonstrated that synOT administration during labor was related to a decreased probability that the newborn would self-attach to the breast and suckle while in skin to skin contact with the mother within the first 60 minutes after birth when compared to non-synOT exposed neonates. Videotape analysis showed that the exposed neonates had significantly fewer minutes of rest.
In order to further understand these prior findings and to seek the physiological pathways affected by synOT related to breastfeeding, a modified ascending link tracing methodology was utilized. The ascending, link tracing method (also called chain referral” or snowball” method) has been primarily used in sociology to find hidden or elusive populations and has proven to be effective [17]. The technique involves finding one member of the population and seeking referral to others. In this case, the process was modified to begin with one research study (instead of one human member of a population) and snowball” to additional research studies using relevant references until saturation is reached. This method was chosen in the hope of capturing the widest possible range of physiologic pathways.
Beginning with one citation used in a prior study [18], relevant studies were linked by locating any cited references that could refer to physiologic pathways which might be affected by synOT or the physiologic relationship of synOT to breastfeeding. The references cited in the new article were accessed to continue the link tracing. The PubMed feature similar articles” for each article was also used to access the maximum possible number of articles. This referral linking process was continued until reaching saturation, when no new physiologic pathways with downstream breastfeeding implications were identified. The collection and analysis was performed between May 15 and November 13, 2017.
Results
Three pathways related to physiologic effects on breastfeeding by synOT administration were identified: dysregulation of the maternal OT system, the crossing of the fetal blood brain barrier by synOT, and hyper stimulation of the uterus. Six downstream outcomes that could possibly affect breastfeeding include decreased maternal endogenous oxytocin, increased risk of negative neonatal outcomes, decreased neonatal rest during the first hour with the potential of decreasing the consolidation of memory, decreased neonatal pre-feeding cues, and decreased neonatal reflexes associated with breastfeeding, and in the long term, increased maternal OT levels possibly related to the observed increased risk of maternal depression, somatic symptoms and anxiety disorders. A cascade model was constructed in order to demonstrate the findings (Figure 1).
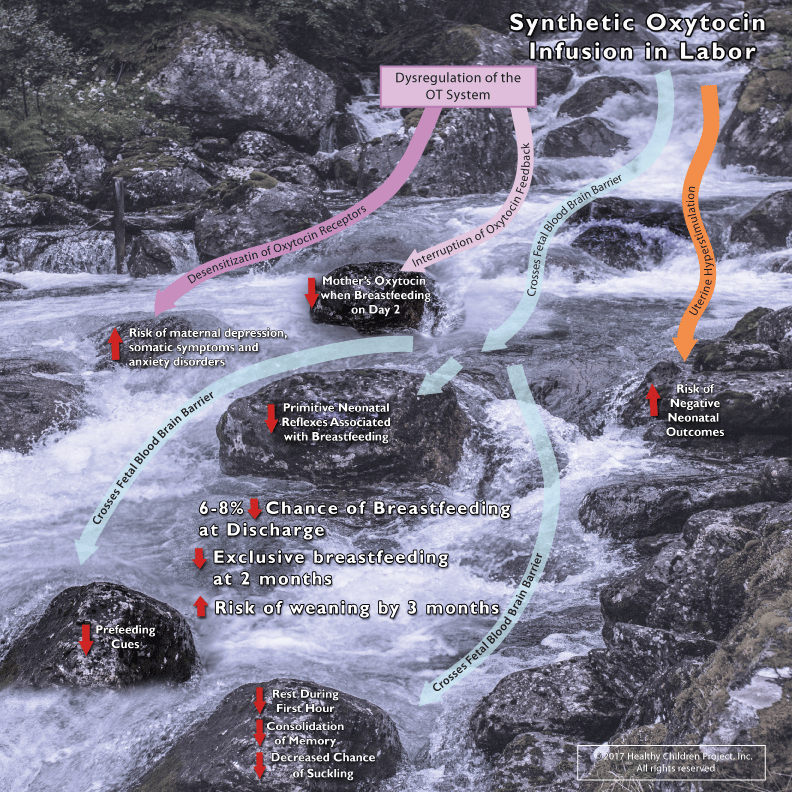
Figure 1: Synthetic Oxytocin Infusion in Labor.
Discussion
Pathway 1
Dysregulation of the Maternal OT System: The peripartum dysregulation of the maternal OT system can be understood to be similar to the physiologic process of insulin dysregulation. The administration of exogenous OT, synOT, may inhibit the action of the maternal endogenous OT in the immediate postpartum through desensitization of OT receptors, first via negative feedback mechanisms that at inhibits the release of the mother’s own OT [19] and subsequently a greater production of endogenous circulating OT [20], possibly due to receptor site damage or the resetting of the OT system upwards to a higher level.
During suckling, OT pulses are released in response to the stretching of the nipple. The secreted OT stimulates the contraction of the myoepithelial cells in the breast resulting in the milk ejection reflex (also called let-down). Jonas, Johansson and colleagues demonstrated that as soon as the second day postpartum, untoward effects of synOT infusion during labor could be measured in new mothers during a breastfeeding. The results were inversely dose dependent with the mothers who had received the highest doses of synOT releasing the lowest amount of their own, endogenous, OT. Mothers who had received only IM synOT (after the birth of the baby) were not studied [19]. It is suspected that a negative feedback mechanism had been activated that inhibited the release of mothers’ own OT.
The desensitization of OT receptors in labor by synOT may be responsible for longer term effects as well. When studied at two [44,45] and three months postpartum [18,46], the amount of synOT the mother had received in labor was positively correlated with her own plasma OT levels. This may be due to a physiologic phenomenon similar to insulin resistance in diabetes or that the “exposure to synOT resets” the natural oxytocin system to a higher basal level to better respond to the body’s needs’ [23]. Breastfeeding outcomes were negatively affected.
Very high or very low levels of peripheral OT have been shown to be associated with symptoms of post-traumatic stress syndrome, depression and anxiety [21]. The findings that women who had been administered intrapartum synOT compared to mothers who had not been exposed had a more than 30% increased relative risk of depressive and anxiety disorders in the first year postpartum are concerning [22]. Gu and colleagues [23] found similar results at 2 months postpartum. The mothers in the Gu study also had an increased risk of symptoms of somatization in the mothers who had been exposed to synOT.
Postpartum depression is related to breastfeeding outcomes. Although the cause and effect relationship is not clear between breastfeeding outcomes and postpartum depression [24], breastfeeding discontinuation by 12 weeks has been correlated with maternal depressive symptoms [24, 25].
Pathway 2
SynOT Crossing the Fetal Blood Brain Barrier: SynOT administered to the laboring woman is thought to cross the placenta and the not-completely-mature fetal blood-brain barrier during labor and desensitize the infant’s central nervous system OTRs [32,39,40] negatively affecting the function of the nervous system OTRs. Studies of the expression of newborn neurobehavioral pre-feeding cues and reflexes demonstrate the sensitivity to synOT of the exposure of the baby during labor. Bell and colleagues found that the babies who had been exposed to synOT were 11.5 times more likely to perform in the lowest to medium levels of pre-feeding organization compared to the babies of mothers who were not exposed. The babies of mothers who were not exposed were more likely to perform at the high level [41]. Other researchers studying newborn’s Primitive Neonatal Reflexes (PNRs) identified the inhibition of several of the reflexes including all of those associated with breastfeeding (the rhythmic reflexes - suck, jaw jerk and swallowing) as significantly lower in the exposed group. The results were not dose dependent [42]. We reported in a prior study that newborns that were skin-to-skin with their mothers in the first hour after birth had a different experience when compared to those whose mothers had been administered synOT [16]. The analysis of videotapes of the behavior of studied babies was in relation to Windstorm’s 9 Stages (Figure 2). Six of the nine stages focus on the activities of the newborn during the first hour -propelling towards the ultimate goal of survival, suckling. The birth cry (stage 1) inflates the babies’ lungs with the initial survival activity of breathing. Activity (stage 3), crawling (stage 4) and familiarization (stage 7) are the locomotive/location aspects of the behavior driving towards suckling (stage 8). What then is the purpose of the resting (stage 5) which occurs, not in order as the others, but interspersed throughout the first hour?

Figure 2: Windstorms’ 9 Stages during skin-to-skin immediately after birth.
At first, we postulated that this non-locomotive, seemingly nonactivity stage, allowed the baby to regroup, perhaps to collect energy for the more vigorous stages. Certainly, the continued contact of the newborn skin to skin with the mother during the periods of rest allows for the reactivation of stimulus-specific neural activity, as the baby continues to smell the mother and the odors of the areola, breast and Montgomery gland secretions, to feel the mother’s skin, and to listen to the mother’s heartbeat during the first hour. However, review of research conducted in the field of memory and consolidated learning expanded our thinking to consider the resting (Stage 5) as an opportunity for the baby to consolidate the important learning of the first hour, and the memories acquired through smelling, tasting and feeling the mother on the way to suckling, and continue this in memory consolidation stage 9, sleep, which has the already been established by considerable research.
Memory consolidation is thought to depend upon a temporally evolving process that involves interactions between the hippocampus and neocortex. While the hippocampus is critical for the initial creation of an episodic memory trace, it is hypothesized that long-term storage results from the restructuring of information across hippocampal-neocortical networks over time, resulting in a distributed memory representation” [43] and this consolidation is thought to be mediated by “replay’ ’’ [44].
Researchers have now described a significant correlation between the initial encoding and the subsequent period of awake rest. The more activity in the hippocampus and cortical regions of the brain at resting time, the stronger the memory when tested later [44]. With this recent addition of rest to sleep as a state where learning (through consolidating and strengthening memories) is solidified, we hypothesized that the function of rest in the first hour is to consolidate the memories of the mother’s face, her smell, touch, and sound. We wondered about the effect of synOT administration to the mother in labor on the infants rest while skin to skin in the first hour since there are clusters of OTRs in hippocampus, the site of memory consolidation.
After eliminating the confounder of epidural medications, the synOT exposed babies in our prior study had 10% fewer minutes of rest. Newborns exposed to neither synOT nor fentanyl epidural rested for a mean of 17:17.32 and a median (25th-75th quartile) of 15:53.90 during the first hour after birth. Newborns exposed to synOT (but not fentanyl epidural) rested for a shorter mean of 10:42.41 and a median of 11:22.85 during the first hour after birth. Analysis of the means with the Mann-Whitney Test give a Mean Rank of 15.18 to the first group, and a Mean Rank of 9.08 to the second, a significant difference (p=.031).
The decreased duration of rest is significant since the quantity of neural reactivation during post-learning rest positivity predicts performance” [45]. The hippocampus with its clusters of OTRs [46] is the part of the brain associated with solidifying memories [44] as well as social behavior and bonding [46]. It is not surprising then, that the babies who were exposed to synOT had a significantly diminished chance of suckling in the first hour compared to babies who were not exposed. (p=.027) It is estimated that 22% of neonatal deaths could be averted if breastfeeding is started within the first hour [47].
Pathway 3
Uterine Hyper stimulation: The uterine myometrium contains OTRs which increase as pregnancy advances. The uterus is responsive to oxytocin throughout pregnancy [19] (pages 177-200) and, because synOT is biochemically identical to endogenous OT, when OTRs are occupied by either synOT or OT, myometrial contractions result [20,21]. Receptor sensitivity to oxytocin rapidly increases when a woman is in spontaneous labor [30,31]. Because OT is normally released in a pulsatile fashion, the smooth cells of the myometrium in the uterus are allowed recover between pulses. However, receptor desensitization as well as a decrease in the percentage of receptor cells [32] can result when women are exposed to longer times of synOT infusions or higher amounts of synOT. “Clinical use of high dose oxytocin (synOT) infusion longer than 3 to 4 hours may be counterproductive to the augmentation of uterine contractions’ (p. 502) with the potential uterine effect of poor contractility, atony [33,34] and hemorrhage.
A recent US research trial questioned whether labor induced with synOT would progress without continuous synOT infusions. The researchers were able to demonstrate that discontinuing the synOT infusion after labor had been achieved did not result in a higher rate of cesarean births [28]. An accompanying editorial titled “Oxytocin use during active labor: too much of a good thing [9]?’ reminded the reader that synOT for labor induction and augmentation has been understudied. (p. 439) Researchers report that administration of synOT is often unstructured and without a correct diagnosis [30]. New standards, uniformity of care in the use of synOT [27], checklists, and more research [28] have been suggested.
When the uterus contracts during labor there is an intermittent decrease of the flow of blood to the space where oxygen exchange takes place between the mother and the fetus. These interruptions in blood flow, when contractions occur with normal frequency, are well tolerated by the healthy fetus [48].
Hyper stimulation, defined as more than 5 contractions in 10 minutes for 2 consecutive 10 minute periods, was documented in 30.2% of labors induced with synOT [49]. The more contractions experienced by the laboring mother and her fetus in 30 minutes, the greater the negative effect on the newborn infant [50]. The odds of neonatal morbidity were maintained even when augmentation and induction were assessed separately in a large population study [51].
The reduced intervillous exchange of oxygen and carbon dioxide associated with uterine hyper stimulation may result in fetal hypoxia or acidosis. It’s not clear, however, if the negative consequences seen in the infant are primarily due to acidosis or hypoxia [52], however fetal and neonatal academia has been associated with multiorgan dysfunction, hypotoxic ischamic encephalopathy, seizures, cerebral palsy, long-term neurological deficits and neonatal death” [53].
Uterine hyper stimulation and resulting acidosis may be measured as umbilical cord artery pH of 7.0 or less [54], although even a more neutral pH of =7.60 may place newborns at risk for adverse outcomes [55]. The risk for the severe neonatal outcomes listed above may be more likely with the lowest umbilical cord artery pH while newborns with an umbilical cord pH measured to be closer to the mean are more likely to experience an APGAR less than 7 at 5 minutes, the need for assisted ventilation and NICU admission [53,55,56] - each with the possibility that the newborn will be separated from his mother.
Elander and Lindberg’s [57] research paved the way for understanding the effects on the baby of the separation from mother shortly after birth for medical reasons and subsequent breastfeeding outcomes. Separated term newborns were compared with nonseparated newborns at three months of age with the finding that that the frequency of exclusive breastfeeding in the separated group was 37%. The frequency of exclusive breastfeeding in the non-separated group was 72%. Even brief separation of mother and baby for resuscitation, brief respiratory support or a low Apgar score may deprive the dyad of the experience of immediate, continuous and uninterrupted skin-to-skin in the first hour.
Recent research examined early separation of the mother and baby versus skin to skin contact for the first 1-3 hours after birth in relation to exclusive breastfeeding at hospital discharge [58]. With a sizable population of more than twenty-one thousand dyads, the robust findings indicate a dose-response relationship between early skin-to-skin contact and breastfeeding exclusivity at hospital discharge.
If the ejection of the mother’s milk [19], the baby’s pre-feeding cues [41], the baby’s primitive neonatal reflexes associated with feeding [42], the amount of rest (and memory consolidation), whether the baby is separated from the mother and whether or not the baby suckles in the first hour [16] are altered in babies exposed to synOT, it follows that breastfeeding outcomes should be affected as well. It shouldn’t be a surprise, then, that a large study of almost 50,000 women showed that the chance of breastfeeding at discharge from the hospital (day 2) was diminished by 6-8% if the mother had been administered intrapartum synOT [63]. At two months postpartum, the mothers who were most likely to be exclusively breastfeeding had received the lowest amounts of synOT or who had not been induced [23,64]. Another study found that the risk of stopping breastfeeding by 3 months was significantly higher (2.29, 95% CI 1.41-3.74) if the mother had received synOT, particularly if the mother was younger than 27 [18].
Labor induction or augmentation with synOT may have effects for the baby as well as the mother. synOT use may lead to uterine hyper-stimulation, fetal bradycardia and increase the level of lactate found in the amniotic fluid [59], a condition that risks acidemia of the newborn as evidenced by respiratory distress, lowered 5 minute Apgar Scores compared to the 1 minute score as well as other negative neonatal outcomes [60,61]. Reanalysis of data published previously [16] reveals that augmentation with synOT was significantly associated with a medical crisis for either the mother or infant (p=.012). The finding of increased neonatal morbidity with the use of synOT for both induction and augmentation is troubling [16,51].
Conclusion
Although not every study examined in a recent systematic review of literature linking the administration of synOT and breastfeeding outcomes described negative effects of this common obstetrical practice, no study found a favorable breastfeeding outcome [62]. Because OT is important for successful lactation, any negative impact of synOT on breastfeeding outcomes should be of concern, and a consideration in studies of sub-optimal breastfeeding.
There is still much to learn about the effects of intrapartum administration of synOT. Concerns continue to emerge. For example, it has been documented in other mammals that synOT infusions epigenetically alter the OTR gene. Does this phenomenon happen in humans as well [65]? Is there a higher amount of OT in the first feedings of colostrum after administration of synOT? Could that effect the immunological development of the infant gut and contribute to other epigenetic changes [20]? Is there a relationship between complications of labor, labor drugs, (including synOT) and the development of Autism Spectrum Disorder (ASD)? Smallwood and colleagues [66] found in their study that children with autism were 2.32 times more likely to have been exposed to synOT than children without ASD p=.004 while another study [67] found no relationship between labor induction and ASD diagnoses. A 2017 meta-analysis that collated data from 37,634 autistic children and 12,081,416 nonautistic children enrolled in 17 studies [68], concluded that induction of labor was one of the prenatal, perinatal, and postnatal factors related to autism. The authors remind us that the finding of autism may be a result of multiple rather than single factors. As with the question of possible epigenetic effects, the physiologic pathway is unclear. It’s also important to remember that not all exposed babies and mothers are affected by synOT; the hormone OT may play a part in directing other hormones, and other factors, (stress, smoking, gestational age) may predispose mothers and/or their babies to be more vulnerable.
Ragusa and colleagues espouse the pre-cautionary principle when considering the use of synOT which still lacks reasonable assurance that it is non-harmful for perinatal and immunological development.” (20, p.7) A large population Australian study found that the risk of adverse outcomes was increased even among low risk women [51].” In the light of these findings, moderating intrapartum interventions, particularly the use of synOT, should be included in the list of preventive measures that can lead to an improvement in breastfeeding outcomes, along with individual and system interventions.
References
- Ip S, Chung M, Raman G, Chew P, Magula N, DeVine D, et al. Breastfeeding and maternal and infant health outcomes in developed countries. Evid Report Technology Assess. 2007; 153: 1-186.
- Bartick M, Reinhold A. The burden of suboptimal breastfeeding in the United States: A pediatric cost analysis. Pediatrics. 2010; 125: 1048-1056.
- Bartick MC, Stuebe AM, Schwarz EB, Luongo C, Reinhold AG, et.al. Cost analysis of maternal disease associated with suboptimal breastfeeding. Obstet Gynecol. 2013; 122: 111-119.
- Bartick MC, Schwarz EB, Green BD, Jegier BJ, Reinhold AG, Colaizy TT, et al. Suboptimal breastfeeding in the United States: Maternal and pediatric health outcomes and costs: Suboptimal breastfeeding in the United States. Matern Child Nutr. 2017; 13: e12366.
- Women’s Preventive Services Initiative (US). Multidisciplinary Steering Committee, author, American College of Obstetricians and Gynecologists, issuing body, United States. Health Resources and Services Administration, sponsoring body. Recommendations for Preventive Services for Women Final Report to the US. Department of Health and Human Services, Health Resources & Services Administration. 2017.
- Langer A, Campero L, Garcia C, Reynoso S. Effects of psychosocial support during labour and childbirth on breastfeeding, medical interventions, and mothers’ wellbeing in a Mexican public hospital: A randomised clinical trial. Br J Obstet Gynaecol. 1998; 105: 1056-1063.
- Fiona Dykes. Breastfeeding in Hospital: Mothers, Midwives and the Production Line. Oxon, England. Routledge.
- Institute for Safe Medication Practices. ISMP List of High-Alert Medications in Acute Care Settings. Cited. 2017.
- Prasad MR, Funai E. Oxytocin use during active labor: Too much of a good thing? Am J Obstet Gynecol. 2012; 207: 439-440.
- Pitocin (Oxytocin Injection, USP) Synthetic label. Cited. 2017.
- Martin JA, Hamilton BE, Osterman MJK, Driscoll AK, Mathews TJ. Births: Final Data for 2015. Natl Vital Stat Rep Cent Dis Control Prev Natl Cent Health Stat Natl Vital Stat Syst. 2017; 66: 1.
- Laughon SK, Zhang J, Grewal J, Sundaram R, Beaver J, Reddy UM. Induction of labor in a contemporary obstetric cohort. Am J Obstet Gynecol. 2012; 206: 486-489.
- Declercq ER, Sakala C, Corry MP, Applebaum S. Listening to Mothers II: Report of the Second National U.S. Survey of Women’s Childbearing Experiences. J Perinat Educ. 2007; 16: 9-14.
- Guidelines for Oxytocin Administration after Birth: AWHONN Practice Brief Number 2. J Obstet Gynecol Neonatal Nurs. 2015; 44: 161-163.
- Armstrong WE, Hatton GI. The puzzle of pulsatile oxytocin secretion during lactation: Some new pieces. Am J Physiol Regul Integr Comp Physiol. 2006; 291: 26-28.
- Brimdyr K, Cadwell K, Widström A-M, Svensson K, Neumann M, Hart EA, et al. The Association Between Common Labor Drugs and Suckling When Skin-to-Skin During the First Hour After Birth. Birth Berkeley Calif. 2015; 42: 319-328.
- Salganik MJ, Heckathorn DD. Sampling and Estimation in Hidden Populations Using Respondent-Driven Sampling. Sociol Methodol. 2004; 34: 193-239.
- García-Fortea P, González-Mesa E, Blasco M, Cazorla O, Delgado-Ríos M, González-Valenzuela MJ. Oxytocin administered during labor and breast-feeding: A retrospective cohort study. J Matern Fetal Neonatal Med. 2014; 27: 1598-1603.
- Jonas K, Johansson LM, Nissen E, Ejdebäck M, Ransjö-Arvidson AB, Uvnäs-Moberg K. Effects of intrapartum oxytocin administration and epidural analgesia on the concentration of plasma oxytocin and prolactin, in response to suckling during the second day postpartum. Breastfeed Med Off J Acad Breastfeed Med. 2009; 4: 71-82.
- Ragusa A, Svelato A, Silberstein R, Rinaldo D. Does the use of oxytocin in the third stage of labour have an impact on breastfed babies’ health? Looking for a viable alternative. J Pharmacol Clin Toxicol. 2017; 5: 1090.
- Cyranowski JM, Hofkens TL, Frank E, Seltman H, Cai H-M, Amico JA. Evidence of dysregulated peripheral oxytocin release among depressed women. Psychosom Med. 2008; 70: 967-975.
- Kroll-Desrosiers AR, Nephew BC, Babb JA, Guilarte-Walker Y, Moore Simas TA, Deligiannidis KM. Association of peripartum synthetic oxytocin administration and depressive and anxiety disorders within the first postpartum year. Depress Anxiety. 2017; 34: 137-146.
- Gu V, Feeley N, Gold I, Hayton B, Robins S, Mackinnon A, et al. Intrapartum Synthetic Oxytocin and Its Effects on Maternal Well-Being at 2 Months Postpartum. Birth. 2016; 43: 28-35.
- Pope CJ, Mazmanian D. Breastfeeding and Postpartum Depression: An Overview and Methodological Recommendations for Future Research. Depress Res Treat. 2016: 4765310.
- Taveras EM, Capra AM, Braveman PA, Jensvold NG, Escobar GJ, Lieu TA. Clinician support and psychosocial risk factors associated with breastfeeding discontinuation. Pediatrics. 2003; 112: 108-115.
- Dennis C-L, McQueen K. The relationship between infant-feeding outcomes and postpartum depression: a qualitative systematic review. Pediatrics. 2009; 123: 736-751.
- Caldeyro-Barcia R, Heller H, editors. Oxytocin. London, UK: Pergamon Press. 1959.
- Diven LC, Rochon ML, Gogle J, Eid S, Smulian JC, Quiñones JN. Oxytocin discontinuation during active labor in women who undergo labor induction. Am J Obstet Gynecol. 2012; 207: 471-478.
- Blanks AM, Thornton S. The role of oxytocin in parturition. BJOG Int J Obstet Gynaecol. 2003; 110: 46-51.
- Selin L, Almström E, Wallin G, Berg M. Use and abuse of oxytocin for augmentation of labor. Acta Obstet Gynecol Scand. 2009; 88: 1352-1357.
- Caldeyro-Barcia R, Sereno JA. The response of the human uterus to oxytocin throughout pregnancy. In: Oxytocin. New York, NY: Pergamon Press. 1961.
- Robinson C, Schumann R, Zhang P, Young RC. Oxytocin-induced desensitization of the oxytocin receptor. Am J Obstet Gynecol. 2003; 188: 497-502.
- Phaneuf S, Asbóth G, Carrasco MP, Liñares BR, Kimura T, Harris A, et al. Desensitization of oxytocin receptors in human myometrium. Hum Reprod Update. 1998; 4: 625-633.
- Phaneuf S, Rodriguez Linares B, TambyRaja RL, MacKenzie IZ, López Bernal A. Loss of myometrial oxytocin receptors during oxytocin-induced and oxytocin-augmented labour. J Reprod Fertil. 2000; 120: 91-97.
- Hayes EJ, Weinstein L. Improving patient safety and uniformity of care by a standardized regimen for the use of oxytocin. Am J Obstet Gynecol. 2008; 198: 622 -627.
- Kendrick AJ, Neilson JP. Continuous versus pulsatile oxytocin administration for the augmentation of labour. In: The Cochrane Collaboration, editor. Cochrane Database of Systematic Reviews. Chichester. UK: John Wiley & Sons. Ltd. 2015.
- Prevost M, Zelkowitz P, Tulandi T, Hayton B, Feeley N, Carter CS, et al. Oxytocin in Pregnancy and the Postpartum: Relations to Labor and Its Management. Front Public Health. 2014; 2: 1.
- Fernández IO, Gabriel MM, Martínez AM, Morillo AF-C, Sánchez FL, Costarelli V. Newborn feeding behaviour depressed by intrapartum oxytocin: a pilot study. Acta Paediatr Oslo Nor. 2012; 101: 749-754.
- Anagnostakis D, Messaritakis J, Damianos D, Mandyla H. Blood-brain barrier permeability in “healthy” infected and stressed neonates. J Pediatr. 1992; 121: 291-294.
- Noseworthy MD, Bray TM. Effect of oxidative stress on brain damage detected by MRI and in vivo 31P-NMR. Free Radic Biol Med. 1998; 24: 942-951.
- Bell AF, White-Traut R, Rankin K. Fetal exposure to synthetic oxytocin and the relationship with prefeeding cues within one hour post birth. Early Hum Dev. 2013; 89: 137-143.
- Gabriel MAM, Fernández IO, Martínez AMM, Armengod CG, Costarelli V, Santos IM, et al. Intrapartum synthetic oxytocin reduce the expression of primitive reflexes associated with breastfeeding. Breastfeed Med Off J Acad Breastfeed Med. 2015; 10: 209-213.
- Peigneux P, Orban P, Balteau E, Degueldre C, Luxen A, Laureys S, et al. Offline Persistence of Memory-Related Cerebral Activity during Active Wakefulness. Wilson MA, editor. PLoS Biol. 2006; 4: 100.
- Tambini A, Ketz N, Davachi L. Enhanced Brain Correlations during Rest Are Related to Memory for Recent Experiences. Neuron. 2010; 65: 280-290.
- Craig M, Wolbers T, Harris MA, Hauff P, Della Sala S, Dewar M. Comparable rest-related promotion of spatial memory consolidation in younger and older adults. Neurobiol Aging. 2016; 48: 143-152.
- Francis DD, Champagne FC, Meaney MJ. Variations in maternal behaviour are associated with differences in oxytocin receptor levels in the rat. J Neuroendocrinol. 2000; 12: 1145-1148.
- Edmond KM, Zandoh C, Quigley MA, Amenga-Etego S, Owusu-Agyei S, Kirkwood BR. Delayed breastfeeding initiation increases risk of neonatal mortality. Pediatrics. 2006; 117: 380-386.
- Paternoster DM, Micaglio M, Tambuscio B, Bracciante R, Chiarenza A. The effects of epidural analgesia and uterine contractions on fetal oxygen saturation during the first stage of labour. Int J Obstet Anesth. 2001; 10: 103-107.
- Crane JM, Young DC, Butt KD, Bennett KA, Hutchens D. Excessive uterine activity accompanying induced labor. Obstet Gynecol. 2001; 97: 926-931.
- Simpson KR, James DC. Effects of oxytocin-induced uterine hyper stimulation during labor on fetal oxygen status and fetal heart rate patterns. Am J Obstet Gynecol. 2008; 199: 34.e1-35.
- Buchanan SL, Patterson JA, Roberts CL, Morris JM, Ford JB. Trends and morbidity associated with oxytocin use in labour in nulliparas at term. Aust N Z J Obstet Gynaecol. 2012; 52: 173-178.
- Bobrow CS, Soothill PW. Causes and consequences of fetal acidosis. Arch Dis Child Fetal Neonatal Ed. 1999; 80: 246-249.
- Sabol BA, Caughey AB. Acidemia in neonates with a 5-minute Apgar score of 7 or greater - What are the outcomes? Am J Obstet Gynecol. 2016; 215: 486-486.
- Bakker PC, Kurver PH, Kuik DJ, Van Geijn HP. Elevated uterine activity increases the risk of fetal acidosis at birth. Am J Obstet Gynecol. 2007; 196: 313-316.
- Victory R, Penava D, da Silva O, Natale R, Richardson B. Umbilical cord pH and base excess values in relation to neonatal morbidity for infants delivered preterm. Is J Obstet Gynecol. 2003; 189: 803-807.
- Oscarsson ME, Amer-Wåhlin I, Rydhstroem H, Källén K. Outcome in obstetric care related to oxytocin use. A population-based study. Acta Obstet Gynecol Scand. 2006; 85: 1094-1098.
- Elander G, Lindberg T. Short mother-infant separation during first week of life influences the duration of breastfeeding. Acta Paediatr Scand. 1984; 73: 237-240.
- Bramson L, Lee JW, Moore E, Montgomery S, Neish C, Bahjri K, et al. Effect of early skin-to-skin mother--infant contact during the first 3 hours following birth on exclusive breastfeeding during the maternity hospital stay. J Hum Lact Off J Int Lact Consult Assoc. 2010; 26: 130-137.
- Wiberg-Itzel E, Pembe AB, Wray S, Wihlbäck A-C, Darj E, Hoesli I, et al. Level of lactate in amniotic fluid and its relation to the use of oxytocin and adverse neonatal outcome. Acta Obstet Gynecol Scand. 2014; 93: 80-85.
- Widström AM, Lilja G, Aaltomaa-Michalias P, Dahllöf A, Lintula M, Nissen E. Newborn behaviour to locate the breast when skin-to-skin: a possible method for enabling early self-regulation. Acta Paediatr Oslo Nor. 2011; 100: 79-85.
- Jonsson M, Nordén-Lindeberg S, Östlund I, Hanson U. Acidemia at birth, related to obstetric characteristics and to oxytocin use, during the last two hours of labor. Acta Obstet Gynecol Scand. 2008; 87: 745-750.
- Erickson EN, Emeis CL. Breastfeeding Outcomes After Oxytocin Use During Childbirth: An Integrative Review. J Midwifery Women’s Health. 2017; 62: 397-417.
- Jordan S, Emery S, Watkins A, Evans JD, Storey M, Morgan G. Associations of drugs routinely given in labour with breastfeeding at 48 hours: Analysis of the Cardiff Births Survey. BJOG Int J Obstet Gynaecol. 2009; 116: 1622-1629; discussion 1630-1632.
- Bai DL, Wu KM, Tarrant M. Association between intrapartum interventions and breastfeeding duration. J Midwifery Women’s Health. 2013; 58: 25-32.
- Connelly JJ. Are birth and oxytocin epienetic? (Poster session). In Washington DC. 2011.
- Smallwood M, Sareen A, Baker E, Hannusch R, Kwessi E, Williams T. Increased Risk of Autism Development in Children Whose Mothers Experienced Birth Complications or Received Labor and Delivery Drugs. ASN Neuro. 2016; 8: 1759091416659742.
- Oberg AS, D’Onofrio BM, Rickert ME, Hernandez-Diaz S, Ecker JL, Almqvist C, et al. Association of Labor Induction With Offspring Risk of Autism Spectrum Disorders. JAMA Pediatr. 2016; 170: e160965.
- Wang C, Geng H, Liu W, Zhang G. Prenatal, perinatal, and postnatal factors associated with autism: A meta-analysis. Medicine (Baltimore). 2017; 96: e6696.