
Research Article
Ann Nurs Res Pract. 2022; 7(1): 1049.
NICU Nursing Teamwork: Novel Framework and Implications for Practice
Kilcullen MP1, Woods AL2, Carroll S3,4,5, Balon-Lyon A6, Miller B7 and Salas E1*
1Rice University, TX, USA
2The University of Texas MD Anderson Cancer Center, USA
3Coastal Carolina Neonatology, PLLC, USA
4Children’s Hospital, Wilmington, NC, USA
5UNC Chapel Hill, USA
6Alberta Medical Association, USA
7Ronald McDonald House of Ann Arbor, USA
*Corresponding author: Salas E, Department of Psychological Sciences, Rice University, 429 Sewall Hall, Houston, TX 77005, USA
Received: February 01, 2022; Accepted: March 09, 2022; Published: March 09, 2022
Abstract
Objective: To develop a comprehensive framework for nursing teamwork in neonatal intensive care units (NICUs). Background: Modern healthcare practices have moved towards focusing on multidisciplinary team-based models for providing patient care. There is an abundance of literature focusing on hospital safety culture, but a lack of comprehensive frameworks informing safety initiatives at the team-level, with a focus on nurses. This gap is addressed by presenting an evidence-based framework for effective teamwork in this environment.
Materials and Methods: The development of the TeamNICU framework was informed by a review of the literature, expert opinion, and behavioral observations and interviews. An interdisciplinary collaboration of healthcare professionals and team science experts was utilized to identify the need for a teamwork framework for nurses and to identify competencies needed. The framework was refined after behavioral observations and semi-structured interviews were conducted to observe teamwork firsthand. Finally, a review of the literature was conducted to address any remaining gaps in the framework.
Results: The TeamNICU framework consists of four tiers: 1) team orientation/ mutual trust, coaching, competence, and accountability, 2) psychological safety and voice, 3) information exchange, coordination, and shared mental models, and 4) effective patient and family care. This triangle is surrounded by team and organizational conditions that impact teamwork in this environment.
Conclusions: The TeamNICU framework provides guidance for future researchers as well as a resource for practitioners.
Keywords: Teamwork; Team coordination; Psychological safety; Voice; Patient safety; Nursing
Introduction
Modern healthcare has moved towards a multidisciplinary teambased model for providing patient care. These multidisciplinary healthcare teams must coordinate in order to provide optimal care, and thus rely on effective teamwork and communication to safely care for patients [1]. Indeed, teamwork is essential for ensuring patient safety in the dynamic healthcare domain [2]. A voluntary and anonymous reporting of medical errors identified various incidents, including failure to follow policies or protocols, inattention, communication problems, and poor teamwork as some of the most frequently cited factors contributing to medical error [3]. Additionally, a Joint Commission investigation identified poor communication as a root cause in over 72% of perinatal injuries and deaths [4]. Previous research indicates that the odds of infants contracting healthcare-associated infection decrease by 18% with each 10% rise in respondents reporting good teamwork [5]. Therefore, effective teamwork can provide an avenue for enhancing patient care in healthcare. However, not all teams engage in effective teamwork at the outset, in fact, many individuals struggle to engage in teamwork and perform effectively as a unit. Fortunately, recent metaanalyses indicate that team training significantly improves teamwork and performance outcomes [6,7], and to pertinent to the present study, successful team training interventions rely on evidence-based frameworks.
Understanding communication and teamwork in healthcare is inherently complex and difficult to map due to the nested, interdependent nature of teams comprising the organizational structure. Depending on the unit, clinicians can have separate meetings to exchange information and engage in care planning (e.g., nurse huddle, physician huddle). Additionally, teams of healthcare personnel can often specialize in different types of cases, ranging from stable (i.e., primary care physicians) to critical care (i.e., emergency department), which can have their own separate meetings. Team interactions vary greatly, not only by which teams are interacting (e.g., transport interacting with surgical teams), but also by which individuals are on that team during the shift. Additionally, personnel within healthcare teams often rotate after a certain period of time, sometimes to give personnel a wide range of experience or to provide continuity of care to patients, and sometimes there is high turnover from residency and other time-limited programs. The nursing discipline is particularly complicated, as in any given healthcare team there can be nurses from varying specialties and educations. Understanding how these nurses communicate and work together collaboratively involves considering not only the challenges they face within their profession, but how they interact with other members of their healthcare team, including physicians, therapists, technicians, administration, and patients.
While there is an abundance of literature focusing on hospital safety culture and healthcare teamwork, there is a dearth of knowledge on the components of teamwork that focus on nurses. There exists a need for a comprehensive framework focused on nurses for informing safety initiatives at the team-level, as nurses face unique challenges and fulfill a distinct role within teams that warrants a tailored guided perspective. We address this gap by presenting an evidence-based framework for effective nursing teamwork. Development of the framework involved a three-fold effort entailing subject matter expert (SME) input, behavioral observations and interviews, and a literature review. We begin by explicating each step of the development process, then expand on each tier and component(s) of the framework. Practical implications are interlaced throughout - corresponding with each framework component. We conclude with a broader discussion and agenda for future research.
Materials and Methods
The initial framework was generated based on expert opinion from an interprofessional and interdisciplinary council of subject matter experts (SMEs) in team science, neonatal healthcare, and clinical research. Behavioral observations within a neonatal intensive care unit (NICU) by team science experts served as an opportunity to gain an unbiased, outsiders’ perspective into the functionality of teamwork between nurses and other clinicians. Additionally, semistructured interviews were conducted to clarify team roles and shed light on factors that facilitate and inhibit effective team performance in this environment. Finally, a literature review provided insight into any missing team-based elements and informed the final refinement of the TeamNICU framework. Elaboration on each of these phases of framework refinement is provided below, followed by an overview of the framework and detailed discussion of each framework factor.
SME council
The need for a comprehensive framework for effective nursing teamwork was first discussed during a Vermont Oxford Network (VON) conference in the northwestern region of the United States. The TeamNICU framework was first conceptualized through collaboration with interdisciplinary and interprofessional subject matter experts (SMEs) and experts in team science. It was conceived during a homeroom session that typically meets three times a year to discuss and problem-solve current needs. These homeroom sessions are composed of interdisciplinary and interprofessional personnel. The amalgamation of this effort resulted in the initial stages of the teamwork framework, specifically constructed to focus on nurses.
Behavioral observations and interviews
While expert opinion is crucial, we endeavored to dig deeper and place team science experts within a hospital to uncover additional elements of teamwork that may be essential in this environment. To further understand the complexities of teamwork with nurses, the researchers embedded themselves within a mid-to-large sized neonatal intensive care unit (NICU) in the south-central region of the United States, engaging in behavioral observations and conducting interviews.
Observational shifts were conducted to further understand teamwork behaviors within and between NICU teams. Each shift, two team science experts participated in observations to ensure that essential elements of teamwork were not missed. To capture a holistic understanding of teamwork, and not of any singular team, observations happened during a variety of time points. This procedure helped to ensure that lessons learned apply to the entire network, and not solely a specific type of team within that network. Observations involved shadowing a variety of clinicians, witnessing interdisciplinary and interprofessional huddles, and observing patient/family consults. Collectively, these sessions provided ample opportunity to observe how personnel and nurses in particular communicate and handle patient information, perform patient transitions between teams, and interact as a larger network, or multiteam system (i.e., team of teams), to effectively deliver patient care.
During each observation, the researchers continually took notes on team interaction and semi-structured interviews were conducted with personnel when time permitted. The researchers strived to be as unobtrusive during observations as possible as to not influence team functionality. Breaks between team interaction and individual tasks were utilized to ask questions regarding team communication and collaboration, roles and responsibilities, and barriers and facilitators to effective team functioning. Interviews also provided the researchers with opportunities to ask questions and seek clarity on the various aspects of teamwork that they witnessed.
Review of the literature
After developing the initial framework through collaboration between team science and healthcare experts and refining the framework after behavioral observations and interviews, relevant literature was integrated into the framework to add additional breadth and address remaining gaps. Specifically, we drew from contemporary and seminal research on healthcare, team effectiveness, and teamwork to extract and synthesize information relevant to nurse teamwork. This effort enhanced our understanding of teamwork and subsequently enriched our framework.
Results
Results from behavioral observations, interviews, and the literature review were qualitatively analyzed and prominent themes around teamwork were extracted. The integration of SME input, behavioral observations, interviews, and review of the literature resulted in the development of the hereby named TeamNICU framework. This framework (Figure 1) consists of four tiers, culminating in effective care, and the surrounding conditions that enable team effectiveness. Each element of the framework is discussed below, as well as the supporting evidence from the observations, interviews, and the literature.
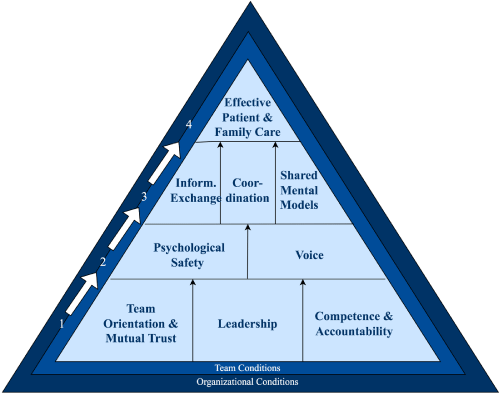
Figure 1: TeamNICU framework for team effectiveness.
Tier one
The first, foundational tier of the framework includes team orientation and mutual trust, leadership, and competence and accountability. Together, these components contribute towards the second tier of the framework, such that when they are present in healthcare teams’ providers and nurses in particular, individuals are more likely to feel their teams are psychologically safe and that they can exercise their voice and speak up. Given the rather severe hierarchical challenges present in healthcare teams, ensuring that these foundational components are present is crucial for enhancing nurse perceptions of psychological safety, enabling them to speak up about safety concerns or errors. In turn, increased voice in nursing should enhance information sharing, coordination, and shared mental models, reducing patient safety incidents by decreasing errors and catching errors before harm comes to a patient.
Team orientation/mutual trust: Team orientation is an individual’s propensity to prefer to work as part of a team to accomplish tasks [8]. The construct is not specific to any task or team, but rather taps into a general tendency to be comfortable in team settings and have confidence that teams are productive [9]. Team orientation has been identified as an essential element for team success [10,11]. When individuals are team-oriented, there is a mutual respect among the team members such that they trust each other with meaningful levels of responsibility and autonomy needed to achieve team goals. Previous work has found that team orientation can be enhanced in clinical settings when teams perform more frequent debriefs immediately after events occur [12].
Tier
Factor
Definition
1
Team Orientation
An individual's propensity to prefer to work as part of a team
Mutual Trust
A shared trust among team members that they will perform their roles and strive towards team goals
Leadership
Behaviors the leader engages in to establish, monitor, and achieve team goals
Competence
An individual's knowledge, skills, and abilities to perform their job roles and responsibilities
Accountability
How individuals are held responsible for accomplishing their tasks and fulfilling their role on the team
2
Psychological Safety
The degree to which team members feel comfortable speaking up in group settings
Voice
Individual behavior to speak up and express their opinions and concerns
3
Information Exchange
Communicating information within and between teams
Coordination
The degree to which knowledge and actions are aligned within and between teams to achieve overarching goals
Shared Mental Models
Shared understanding of the task and the roles and responsibilities of team members
4
Effective Patient & Family Care
The state of care provided to patients and families
Organizational & Team Conditions
The culture or environment in which the team operates
Table 1: TeamNICU factors and their respective definitions.
Healthcare literature enforces the need to build team relationships and cohesion [13], as well as establishing mutual trust and respect [2,14-16]. Indeed, team cooperation, which is attitudes and feelings such as team orientation and trust, constitute one of the eight C’s of team science [17]. These eight C’s of team science act as a scientifically based practical guide to understanding and improving teamwork and provide support for several elements of the proposed framework in this manuscript. Recent work has found that mutual trust is a prerequisite for nurses’ sense of safety and satisfaction with work [18]. Existing frameworks on healthcare teamwork include team orientation [19,20] and mutual trust [20-22]. Having sufficient team orientation and mutual trust within nurses and the other healthcare personnel that they interact with is essential for improving teamwork and ultimately to reduce patient safety events.
Implications for practice: Healthcare organizations should ensure that their team members are team-oriented and have a strong mutual trust between team members. There are several existing measures of team orientation [23,24] and mutual trust [25-27] that practitioners can use to diagnose their teams. If results indicate that there are deficits in either factor, leadership should utilize targeted interventions for improvement, and then follow up with additional measurement to ensure that positive changes in that factor occur. Existing evidence suggests that team orientation may be malleable, such that through training and positive team experiences an individual’s orientation towards teamwork can be enhanced [28,29]. Similarly, there exist team building exercises that can increase trust within teams [30]. Due to multiple team membership and member fluidity developing familiarity that predicts trust is often challenging, thus, interventions such as team building that require further interactions among team members are useful in promoting building bonds needed to foster mutual trust.
Leadership: Leadership is conceptualized as the enactment of leadership behaviors to establish and achieve team goals [31], and has been identified as an important aspect of teamwork for patient care [2]. Indeed, leadership is included in several existing frameworks of healthcare teamwork [20,22,32-34]. Four major leadership functions include information search and structure, information use and problem solving, managing personnel resources, and managing material resources [35]. There is evidence to suggest that effective coaching from leaders enhances goal attainment, resilience, and workplace well-being [36]. Within the function of managing personnel resources, expert coaching is an essential component, in which leaders should coach, develop, and motivate team members [35].
Specifically considering nurses, previous research suggests that to improve nursing performance, coaches (e.g., managers, team leaders) must engage in role preparation, understand the nature of motivation, foster internal motivation in nursing staff, and invest in positive relationships with subordinates [37]. Team leaders have a significant influence over team processes and performance, and leaders can often act as the most effective change agents, since they are routinely viewed as the holders of an organization’s values [38], when team culture or processes need adjustment. Therefore, if there are organizational values negatively affecting nurse teamwork, the team or unit leader can act as a change agent to shift team values in a positive direction (e.g., shifting focus to prioritizing patient safety over productivity).
Implications for practice: To evaluate the state of leadership within healthcare teams, organizations can either deploy safety culture assessments [39-41], which typically include leadership as a facet, or utilize leadership-specific measures [42,43]. Based on results, organizations can employ interventions to improve leadership as needed [44-46]. Additionally, there are interventions that target advancing women in leadership in healthcare, which may be particularly relevant for leadership roles within the nursing profession, such as charge nurses [47].
Competence and accountability: In order to build high performing provider teams, individual team members must be competent with their job-related knowledge and skills, as well as competent in safety skills and practices. These individuals must be held accountable to their job role and safety standards in order to ensure the effectiveness of the overall team and unit. Employee safety-related knowledge and competence is a key component of safety culture [48], and is critical for ensuring effective team care. Professional competence is listed as an essential element of teamwork in healthcare [14], but is present in few existing frameworks of healthcare teamwork [22]. When considering interprofessional teamwork in healthcare, there should be no assumption of competence in clinicians [49]. However, an employee’s belief that they are competent has been found to influence patient safety [50]. When there is team member turnover, new personnel need to be evaluated to make sure that they possess the clinical competence required for their work.
Not only must healthcare team members, such as nurses, be competent, but they must be held accountable for their actions and responsibilities, in order to ensure effective teamwork [14,16]. Healthcare teams can be held accountable to trust boards, general management, team managers, other team members, and clinical supervisors [51]. For team members to hold each other accountable, they must have a shared understanding of the roles and responsibilities of each team member. Time spent in behavioral observations indicated that having a shared understanding of team and individual responsibilities directly impacts employee and patient outcomes. Without this shared understanding which team members should be held accountable for which responsibilities, duties can be unnecessarily repeated or go unaddressed, resulting in wasted resources, provider burnout, or patient harm. In addition to developing a shared understanding of duties, it is crucial for nurses and care teams to set clear expectations for how those duties should be carried out (i.e., protocols, practices). When roles and responsibilities are effectively established within teams, all team members have a shared understanding of who is responsible for specific tasks and there are clear expectations for what that individual should do and how they should carry out that task.
Implications for practice: Healthcare organizations should ensure that all nurses and other providers in their teams have the necessary knowledge and skills to carry out the task assigned to them. Organizations can assess competency and accountability in their teams in a variety of different ways. One option is to send out a survey to providers, asking them to rate their perception of competency and accountability within their work environment [52]. Low results from such a survey would indicate the need for refresher training to improve safety competence, though any training deployed should target a specific deficit, which may require interviewing staff to uncover. To address issues with accountability, an overhaul of the system of personnel evaluation or incident reporting may be needed, such that providers that fail to complete their responsibilities are given feedback and the chance to learn from the error. Additionally, cross-training can be utilized to increase nurse and other provider awareness of team member roles, enhancing their ability to hold their team members accountable [53]. When assessing competency, and determining appropriate interventions, the mindset of team members should also be considered. Work on growth versus fixed mindsets holds implications for openness to learning new things, which is essential to fully engaging in interventions designed to enhance competence [54]. Therefore, deploying measures to assess team members’ mindsets could aid in determining readiness for competency training, or if supplemental training is needed to first target the mindset of the trainee.
Tier two
The second tier of the TeamNICU framework consists of psychological safety and voice. When individuals view their team as psychologically safe to take risks, they will be more likely to voice concerns and opinions. Nurses and other healthcare providers are more likely to feel that their team is psychologically safe and feel that they can voice their opinions when the factors in the first tier are present (e.g., effective leadership). This will in turn feed into the third tier, enabling effective information exchange, coordination, and shared mental models, ultimately improving patient care.
Psychological Safety: When a team is viewed as psychologically safe, individuals within the team feel comfortable speaking up during group discussions [55]. Psychological safety is of particular importance to the nurse population, because it fosters an environment in which personnel feel safe reporting mistakes and discussing errors, despite the presence of work hierarchy. Although a relatively new concept that’s getting traction in research, psychological safety is present as an essential factor of teamwork in recent healthcare teamwork frameworks [22]. Indeed, past research has found that nurses are more willing to report mistakes when they feel like their team is psychologically safe [55]. Psychological safety has been found to be an influential factor for patient safety competency in nurses [56]. Previous research has found that psychological safety predicts engagement in quality improvement work [57]. In healthcare environments in which there can be rotating physicians and presence of residents, there may be an exacerbated negative impact of hierarchy on psychological safety, such that it may be more difficult for team members to speak out and question one another [58]. Therefore, it is of particular importance to establish psychological safety in healthcare teams and ensure that it is maintained over time, despite turnover.
Implications for practice: Teams operating in healthcare contexts should routinely evaluate psychological safety, paying particular attention to the level of psychological safety reported by individuals that are not traditionally viewed as formal leaders. Psychological safety can be evaluated using several previously established measures [55,59-61]. Should psychological safety prove to be deficient in any given team, interventions and training programs can and should be utilized [62]. To further tailor interventions, organizations should consider assessing psychological safety across all team-unit structures. For example, nurses’ psychological safety could be high during rounds but low during patient handoffs.
Voice: Voice is a relatively new construct and there is not much empirical literature available, particularly focusing on nurse voice. In an article translating teamwork behaviors from aviation to healthcare [63], assertion, or an individual voicing their opinion through questions or statements of opinion during critical times, was listed as an essential component for teamwork in healthcare contexts. Additionally, the literature has highlighted the significance of empowerment in healthcare [16]. When nurses engage in safety voice behaviors, they feel empowered and are more satisfied with their work [64]. Past research has shown that increased mechanisms for employee voice are associated with high retention rates in healthcare settings [65]. When employees have multiple means to voice concerns, they have higher expectancy for problem resolution and higher perceived effectiveness of organizational procedures for resolving problems, leading to lower turnover rates. Indeed, limited employee voice has been shown to have negative effects on engagement levels [66], which understandably may result in increased turnover as engagement decreases.
Employees do or do not engage in voice based on their initial motivation to speak up, their belief that speaking up will bring about a desired result, and the risk level of speaking out [67], illustrating the importance of establishing psychological safety in teams with nurses to promote employee voice behaviors. Indeed, previous research has found that when healthcare providers perceive greater psychological safety, they are more likely to speak up and discuss colleagues’ mistakes [68]. A model of employee voice hypothesizes that several factors contribute to employee decisions to voice opinions or express concerns. These factors may include motive to help organization or team, the perceived cost or safety of voice (i.e., psychological safety), perceived efficacy of voice (i.e., impact of voice), contextual factors (e.g., organizational culture, team size, supervisor openness, leadership style, collective level beliefs), and individual factors (e.g., job attitudes, personality, demographics, experience and tenure, performance, position) [69]. This model in turn proposes that employee voice impacts both outcomes for the organization or team (e.g., decision making, learning, group harmony, error correction) and outcomes for the individual (e.g., job attitudes, stress, performance evaluation, rewards) [69]. Given the potential impact that employee voice can have on individual, team, and organizational outcomes, it is pertinent to include voice when conceptualizing any team-based framework for success.
Implications for practice: Empowering voice, particularly for nurses, is critical for healthcare team performance and safety-related outcomes. Nurses in particular can suffer from hierarchy-related issues when trying to voice opinions or safety-related concerns. Organizations and teams can evaluate the level of voice that their nurses and other providers feel that they have using established measures [70,71]. If perceptions of voice are low, there are existing interventions to promote voice [62,72] in healthcare personnel. The linkage between psychological safety and voice has been wellestablished in the literature [73,74] and both hold significant practical implications for nurse leaders. Research has supported that inclusive leadership in nurse managers (e.g., openness and accessibility) [75] can promote voice through positively influencing psychological safety [76]. In an applied setting, this translates to deploying interventions in nursing leadership that train inclusive leader behaviors, as these behaviors are linked to psychological safety which then encourages voice.
Tier three
The third tier of the TeamNICU framework is composed of information exchange, coordination, and shared mental models. This framework proposes that when the factors from the first two are present and strong, nurses are better able to exchange information, coordinate effectively, and develop shared mental models with their healthcare teams. In turn, when these elements are present and effective, the result will be improved patient and family care.
Information exchange: Information exchange, or communication, involves sharing unique information between teams and individuals [31]. Effective information exchange is particularly important in healthcare contexts, arguably more so than for fields outside of healthcare. Inaccurate information exchange and miscommunication can result in not only a detriment to team and organizational performance, but most importantly can negatively impact patient safety incidents. Behavioral observations and interviews unsurprisingly revealed that effective information exchange is a critical component of teamwork to ensure safe care of patients and help reduce burnout in employees. Patient information must be exchanged between personnel accurately and timely, to ensure safe care of the patient and avoid errors such as inaccurate medication dosage. Practical systems for disseminating information to all personnel, such that all changes in policies and procedures in the unit are communicated to all teams in a timely manner. This will likely help to reduce burnout in employees by preventing personnel from being unfairly disciplined for being unaware of changes in policies and standard procedures. In particular, the nurse liaison role was found to be particularly relevant for effective information exchange. Nurse liaisons should function such that they attend physician huddles and communicate relevant information between teams.
Communication is frequently cited as a crucial element of healthcare teamwork [20,32,34]. However, effective communication is also listed as one of the main challenges to collaborative teamwork in clinical settings [49]. Additionally, fostering effective communication is a key component of effective healthcare culture [13,16]. The three most commonly reported information sources in neonatal intensive care unit (NICU) environments are 1) bedside flowsheet; (2) conversations with nurses; and (3) conversations with resident physicians [77]. In addition to communicating effectively with team members, it is also essential for providers to communicate with parents [78].
Implications for practice: Practical systems for disseminating information to all personnel should be established, such that all changes in policies and procedures are communicated to all teams in a timely manner. This will reduce burnout in employees by preventing personnel from being unfairly disciplined for being unaware of changes in policies and standard procedures. Specifically, a nurse liaison role can be particularly effective in aiding interprofessional patient information exchange, particularly when team “huddles” are profession-based (i.e., nurse huddle separate from physician huddle). Nurse liaisons should function such that they attend physician huddles and communicate relevant information between teams. Additionally, communication between nurses and with other providers can be improved by implementing structured communication policies, such as the SBAR strategy [79]. The SBAR strategy for improving communication between clinicians advises providers to consider the Situation and state what is happening at the present time, discuss the Background or circumstances leading up to the situation, give an Assessment of what they think the problem is, and Recommend what should be done to correct the problem [79].
Coordination: Not only must nurses accurately exchange patient information, but they must also effectively coordinate patient care plans, such that every member of the team understands and accomplishes their roles and responsibilities. Coordination involves using strategies to align knowledge and actions within and between teams. Improving team coordination is essential for promoting patient safety and deploying team coordination training can help avoid adverse events [5,80]. The importance of coordination in teams in general is illustrated through its inclusion as one of the seven C’s of team science [81]. Coordination is particularly important for healthcare providers, who have to adapt their coordination strategies to situational requirements [2]. This could involve teams engaging in more implicit coordination during routine situations that they have extensive experience with, while utilizing more explicit coordination strategies during critical or novel situations. Indeed, the literature on coordination states that effective collaboration and coordination are essential elements of teamwork [14].
Implications for practice: It is essential for nurses to engage in effective coordination with their healthcare team. Healthcare team leaders can evaluate the effectiveness of their teams’ coordination using a variety of different measurement techniques [82]. If coordination is found to be poor, this can have significant implications for team performance and patient safety. Thankfully, there exist several strategies and interventions for improving coordination in healthcare teams that organizations can utilize [83]. Specifically, they present several quality improvement strategies to enhance care coordination, including instituting clinician and patient reminder systems and providing feedback about coordination.
Shared mental models: A team has a shared mental model when there is a shared understanding of the task that is to be performed and of the involved teamwork [84]. The literature on team science suggests that cognitions, or shared understanding among team members, are an essential element of teamwork [81]. Despite being critical for effective teamwork, one of the main challenges for collaborative teamwork in clinical practice is understanding others’ roles [49]. Healthcare team culture research emphasizes that team members need to understand job role clarity and foster shared goals among the team [13]. Indeed, dominant mental models shared by staff have been shown to influence actions and behaviors and contribute to infection rates (Luan, 2006). Established frameworks of healthcare teamwork include shared mental models and clear definition of roles and responsibilities [20,22,32,33]. There are several established methods for measuring shared mental models in healthcare [85], which can be used to evaluate shared mental models in teams and determine if there is a need for training and development.
Indeed, observations and interviews revealed a trend around establishing a shared understanding of team roles and responsibilities. In particular, perception of duties and establishing expectations emerged as two essential themes for healthcare team effectiveness. Having a shared understanding of team and individual responsibilities directly impacts employee and patient outcomes. When the team does not have a shared understanding of roles, duties can be unnecessarily repeated or go unaddressed, resulting in wasted resources, provider burnout, or patient harm. In addition to developing a shared understanding of duties, it is crucial for teams to set clear expectations for how those duties should be carried out (i.e., protocols, practices). When roles and responsibilities are effectively established within teams, all team members have a shared understanding of who is responsible for specific tasks and there are clear expectations for what that individual should do and how they should carry out that task.
Implications for practice: To ensure effective patient care, healthcare teams need to ensure that there exists a shared mental model between nurses and other members of the care team. When this shared mental model is not present, there can be issues with communication and coordination, resulting in preventable errors and potentially patient safety incidents. Shared mental models can be evaluated in a several different ways, and the existing literature is littered with various measures that have been utilized in healthcare [85-88]. After evaluation, if team results indicate deficits in shared mental models, team training can be deployed for improvement [87,89]. Additionally, guided team self-correction can be utilized to increase team mental models [7].
Organizational and team conditions
The environment in which teams operate greatly influences team processes and performance. External factors such as organizational climate and resources, can impact whether or not team members engage in effective teamwork behaviors. Several healthcare frameworks of teamwork include organizational and team conditions as critical for affecting teamwork [22]. Indeed, the last of the seven C’s of team science is conditions, or external factors that influence teamwork [81], reaffirming that establishing the right conditions is necessary to promote effective team performance. Organizational and team conditions for facilitating effective teamwork can include reinforcing teamwork, establishing a supportive culture for teamwork, and ensuring that executive and division leadership are on board for promoting teamwork [22]. Indeed, previous work has asserted that there are ten principles for team cultures that enforce the importance of establishing an appropriate environment or atmosphere for effective teamwork [13]. For example, if a nurse is offered an opportunity to attend a training that provides essential knowledge their team needs, they may not take up that opportunity if their organization does not provide support, encouragement, and time off to do so.
Implications for practice: Leadership must ensure that critical organizational and team conditions are present to promote effective teamwork. Using a healthcare framework presented, conditions should be evaluated to ensure that there exists a culture of support for teamwork, that leadership is committed to teamwork, and that teamwork is reinforced through an evaluation and reward system. Results can inform quality improvement efforts to enhance a culture of teamwork, and results must be reliable and accurate which is only achieved through creating systematic processes to collect, analyze, and report data evaluating both culture and the effectiveness of interventions.
Tier four
Effective patient and family care: The first three tiers of the framework, along with the surrounding organizational and team conditions, enable effective teamwork in neonatal intensive care units. This teamwork has a direct impact on patient and family care, such that when nurses and healthcare teams are effective, families will be more satisfied with the care that is provided and there will be improved patient outcomes. Each layer of the framework builds upon the other to facilitate effective team performance, with the ultimate goal being value-based care. Value-based care is the development and maintenance of a healthy system that prioritizes patient health outcomes relative to the cost of said outcome.(90,91) Nurses work on the frontlines and have arguably some of the highest degrees of faceto- face patient interactions. Value-based nursing care, as supported by the three preceding tiers, creates an environment that is proactive, and patient-centered.
Discussion
The current effort combines evidence from existing knowledge, subject matter experts, observations, and interviews to provide a novel, comprehensive framework for understanding the factors that contribute towards effective teamwork between nurses and other healthcare providers. These factors and the surrounding team and organizational conditions enable clinicians to collaborate effectively, enhancing patient-centered care and reducing error and safety incidents. There are limited frameworks that focus on nursing specifically, and existing healthcare teamwork frameworks fail to address several critical factors presented in this framework, such as voice, psychological safety, competence, and accountability.
Implications for Future Research
Future work could develop a survey to address all elements in this framework to be administered to healthcare units for refinement and validation, with particular emphasis of developing the measure with a nurse population. This survey could be used by consultants, organizations, and unit/team leaders to assess teamwork effectiveness and diagnose problem areas. These problem areas could in turn be targeted with training programs or other interventions for improvement. As discussed earlier, there are already several existing strategies [79] and trainings [92] that target elements of this framework.
After development and validation of a TeamNICU survey, future studies could investigate which components from this framework are the most predictive of team and organizational outcomes such as burnout, employee and family satisfaction, patient health outcomes. This may inform another round of refinement of the framework. Indeed, a systematic review found that high workload and ineffective interpersonal relationship contribute to high levels of burnout, and that these high levels of burnout were related to worsening patient safety [93]. Testing this framework could expand the current understanding of the factors that impact burnout in employees and patient safety outcomes.
Conclusion
There is a significant need to better understand teamwork in healthcare contexts, as ineffective teamwork can lead to patient safety incidents and loss of life. To shed light on this issue and address the need for improved teamwork in practice, the TeamNICU framework was constructed, illustrating the elements that influence effective teamwork in healthcare. This framework contributes to the literature by beginning with expert opinion and interdisciplinary collaboration of healthcare and nonhealthcare professionals, further refining the framework with evidence from observations, interviews, and a review of the literature. The TeamNICU framework can be utilized by practitioners and researchers alike to advance our understanding of teamwork in healthcare contexts and engage in quality safety initiatives to improve patient safety.
Acknowledgements
This work was partially supported by the Center for Clinical and Translational Sciences (UT Health Science Center, Houston, TX), which is funded by National Institutes of Health Clinical and Translational Award UL1 TR003167 from the National Center for Advancing Translational Sciences. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Center for Advancing Translational Sciences or the National Institutes of Health. Rice University is a partner in the award.
References
- Weller J, Boyd M, Cumin D. Teams, tribes and patient safety: overcoming barriers to effective teamwork in healthcare. Postgrad Med J. 2014; 90: 149- 154.
- TM. Teamwork and patient safety in dynamic domains of healthcare: A review of the literature. Acta Anaesthesiol Scand. 2009; 53: 143-151.
- Suresh G, Horbar J, Plsek P, Gray J, Edwards W, Shiono P, et al. Voluntary anonymous reporting of medical errors for neonatal intensive care. Pediatrics. 2004; 113: 1609-1618.
- The Joint Commission. Preventing infant death and injury during delivery Sentinel Event Alert. 2004.
- Profit J, Sharek PJ, Kan P, Rigdon J, Desai M, Nisbet CC, et al. Teamwork in the NICU setting and its association with health care-associated infections in very low birth weight infants. Am J Perinatol. 2017; 34: 1032-1040.
- Hughes AM, Gregory ME, Joseph DL, Sonesh SC, Marlow SL, Lacerenza CN, et al. Saving lives: A meta-analysis of team training in healthcare. J Appl Psychol [Internet]. 2016; 101: 1266-1304.
- Smith-Jentsch KA, Cannon-Bowers JA, Tannenbaum SI, Salas E. Guided team self-correction: Impacts on team mental models, processes, and effectiveness. Small Gr Res. 2008; 39: 303-327.
- Driskell JE, ES. Collective behavior and team performance. Hum Factors. 1992; 34: 277-288.
- Mohammed S, Angell LC. Surface- and deep-level diversity in workgroups: Examining the moderating effects of team orientation and team process on relationship conflict. J Organ Behav. 2004; 25: 1015-1039.
- Salas E, Sims DE, Burke CS. IS THERE A “BIG FIVE” IN TEAMWORK? Small Gr Res. 2005; 36: 555-599.
- Tait R. The attributes of leadership. Leadersh Organ Dev J. 1996; 17: 27-31.
- Lyman K. Relationship between post-resuscitation debriefings and perceptions of teamwork in emergency department nurses. Int Emerg Nurs. 2021; 57: 101005.
- Nicu BIVCH. Treatment team function and its effect on parental stress. Occup Ther Heal Care. 1995; 9: 17-50.
- VM. B. Teamwork in the neonatal intensive care unit. Phys Occup Ther Pediatr. 2013; 33: 5-26.
- Calnan M, Trust RR and health care. Sociol Compass. 2007; 1: 283-308.
- Ohlinger J, Brown MS, Laudert S, Swanson S, Fofah O, Group C. Development of potentially better practices for the neonatal intensive care unit as a culture of collaboration: Communication, accountability, respect, and empowerment. Pediatrics. 2003; 111: e471-481.
- Weaver S, Feitosa J, Salas E, Seddon R, Vozenilek J. The theoretical drivers and models of team performance and effectiveness for patient safety. Salas E, Frush K, editors. Improving patient safety through teamwork and team training. Oxford University Press. 2013: 3-26.
- Hovlin L, Gillsjo C, Dahl Aslan A, Hallgren J. Mutual trust is a prerequisite for nurses’ sense of safety and work satisfaction–Mobile Integrated Care Model: A qualitative interview study. Nord J Nurs Res. 2021.
- Kaiser JA, Westers JB. Nursing teamwork in a health system: A multisite study. J Nurs Manag. 2018; 26: 555-562.
- Kalisch BJ, Weaver SJ, Salas E. What does nursing teamwork look like? A qualitative study. J Nurs Care Qual. 2009; 24: 298-307.
- Kholed SN, Hassan NM, NZ H. Teamwork and collaboration in healthcare: Elements of inter-professional teamwork. Adv Sci Lett. 2017; 23: 10834- 10837.
- Zajac S, Woods A, Tannenbaum S, Salas E, CL H. Overcoming challenges to teamwork in healthcare: A team effectiveness framework and evidencebased guidance. Front Commun. 2021; 6: 606445.
- Driskell JE, Salas E, Hughes S. Collective Orientation and Team Performance: Development of an Individual Differences Measure. Gorman JC, Cooke NJ, Salas E, editors. Hum Factors J Hum Factors Ergon Soc. 2010; 52: 316-328.
- O’Shea P, Driskell JE, Goodwin G, Zbylut ML, Weiss SM. Development of a conditional reasoning measure of team orientation. Washington DC. 2004.
- WA K-S. Organizational trust: The influence of contextual variables. ProQuest Dissertations Publishing. 2002.
- McKnight DH, Choudhury V, CK. Developing and validating trust measures for e-commerce: An integrative typology. Inf Syst Res. 2002; 13: 334-359.
- Padma P, Rosa A, Antonio N. Antecedents and consequences of mutual trust in PPPs. J Relatsh Mark. 2017; 16: 163-178.
- Eby LT, GH D. Collectivistic orientation in teams: An individual and grouplevel analysis. J Organ Behav. 1997; 18: 275-295.
- Shaw JD, Duffy MK, EM S. Team reward attitude: Construct development and initial validation. J Organ Behav Int J Ind Occup Organ Psychol Behav. 2001; 22: 903-917.
- Lacerenza CN, Marlow SL, Tannenbaum SI, ES. Team development interventions: Evidence-based approaches for improving teamwork. Am Psychol. 2018; 73: 517-531.
- Salas E, Shuffler ML, Thayer AL, Bedwell WL, EH L. Understanding and improving teamwork in organizations: A scientifically based practical guide. Hum Res Manag. 2015; 54: 599-622.
- Lavelle M, Reedy GB, Cross S, Jaye P, Simpson T, JE A. An evidence based framework for the temporal observational analysis of teamwork in healthcare settings. Appl Ergon. 2020; 82: 102915.
- Mitropoulos P, Memarian B. A framework of teamwork attributes affecting workers’ safety. Constr Res Congr 2012 Constr Challenges a Flat World. 2012; 1400-1409.
- Rosen MA, Dietz AS, Yang T, Priebe CE, PJ P. An integrative framework for sensor-based measurement of teamwork in healthcare. J Am Med Inf Assoc. 2015; 22: 11-18.
- Burke CS, Stagl KC, Klein C, Goodwin GF, Salas E, Halpin SM. What type of leadership behaviors are functional in teams? A meta-analysis. Leadersh Q. 2006; 17: 288-307.
- Grant AM, Curtayne L, Burton G. Executive coaching enhances goal attainment, resilience and workplace well-being: A randomised controlled study. J Posit Psychol. 2009; 4: 396-407.
- Stapleton P, Henderson A, Creedy DK, Cooke M, Patterson E, Alexander H, et al. Boosting morale and improving performance in the nursing setting. J Nurs Manag. 2007; 15: 811-816.
- McCormack B, Rycroft-Malone J, DeCorby K, Hutchinson AM, Bucknall T, Kent B, et al. A realist review of interventions and strategies to promote evidence-informed healthcare: A focus on change agency. Implement Sci. 2013; 8: 107-119.
- Hedskold M, Pukk-Harenstam K, Berg E, Lindh M, Soop M, JO, et al. Psychometric properties of the hospital survey on patient safety culture, HSOPSC, applied on a large Swedish health care sample. BMC Health Serv Res. 2013; 13: 332-343.
- Pronovost P, BS. Assessing safety culture: Guidelines and recommendations. BMJ Qual Saf. 2005; 14: 231-233.
- Vogus TJ, KM S. The Safety Organizing Scale: Development and validation of a behavioral measure of safety culture in hospital nursing units. Med Care. 2007; 45: 46-54.
- Aarons GA, Ehrhart MG, LR. F. The implementation leadership scale (ILS): Development of a brief measure of unit level implementation leadership. Implement Sci. 2014; 9: 0-1.
- Tourangeau AE, McGilton K. Measuring leadership practices of nurses using the leadership practices inventory. Nurs Res. 2004; 53: 182-189.
- De Brun A, O’Donovan R, McAuliffe E. Interventions to develop collectivistic leadership in healthcare settings: a systematic review. BMC Health Serv Res. 2019; 19: 1-22.
- AS M. Using leadership development programs to improve quality and efficiency in healthcare. J Healthc Manag. 2008; 53: 319-331.
- Mianda S, AV. Developing and evaluating clinical leadership interventions for frontline healthcare providers: A review of the literature. BMC Health Serv Res. 2018; 18: 1-15.
- Mousa M, Boyle J, Skouteris H, Mullins A, Currie G, Riach K, et al. advancing women in healthcare leadership: a systematic review and meta-synthesis of multi-sector evidence on organizational interventions. E Clinical Medicine. 2021; 39: 101084.
- Bisbey TM, Kilcullen MP, Thomas EJ, Ottosen MJ, Tsao K, Salas E. Safety Culture: An Integration of Existing Models and a Framework for Understanding Its Development. Hum Factors. 2019.
- McCallin A, McCallin M. Factors influencing team working and strategies to facilitate successful collborative teamwork. New Zeal J Physiother. 2009; 37: 62-67.
- KT, Naveh E, ZS. Safety self-efficacy and safety performance: Potential antecedents and the moderation effect of standardization. Int J Health Care Qual Assur. 2007; 20: 572-584.
- SO. Responsibility and accountability in community mental health teams. Psychiatr Bull. 1995; 19: 281-285.
- Drach-Zahavy A, Leonenko M, Srulovici E. Towards a measure of accountability in nursing: A three-stage validation study. J Adv Nurs. 2018; 74: 2450-2464.
- Hedges AR, Johnson HJ, Kobulinsky LR, Estock JL, Eibling D, Seybert AL. Effects of Cross-Training on Medical Teams’ Teamwork and Collaboration: Use of Simulation. Pharm (Basel, Switzerland). 2019; 7.
- Dweck C. Carol Dweck revisits the growth mindset. Educ Week. 2015; 35: 20-24.
- Edmondson A. Psychological Safety and Learning Behavior in Work Teams. Adm Sci Q. 1999; 44: 350-383.
- Han JH, Teamwork RYS. Psychological safety, and patient safety competency among emergency nurses. Int Emerg Nurs. 2020; 51: 100892.
- Nembhard IM, AC E. Making it safe: The effects of leader inclusiveness and professional status on psychological safety and improvement efforts in health care teams. J Organ Behav Int J Ind Occup Organ Psychol Behav. 2006; 27: 941-966.
- Masten M, Sommerfeldt S, Gordan S, Greubel E, Canning C, Lioy J, et al. Evaluating teamwork in the neonatal intensive care unit: A survey of providers and parents. Adv Neonatal Care. 2019; 19: 285-293.
- JW H. Towards an observational measure for team psychological safety. Springer Theses. 2013.
- Ming C, Xiaoying G, Huizhen Z, Bin R. A review on psychological safety: Concepts, measurements, antecedents and consequences variables. In: International Conference on Social Science and Technology Education (ICSSTE 2015). Atlantis Press. 2015.
- O’Donovan R, Van Dun D, McAuliffe E. Measuring psychological safety in healthcare teams: Developing an observational measure to complement survey methods. BMC Med Res Methodol. 2020; 20: 1-17.
- O’Donovan R, McAuliffe E. A systematic review exploring the content and outcomes of interventions to improve psychological safety, speaking up and voice behaviour. BMC Health Serv Res. 2020; 20: 1-11.
- Thomas EJ, Sexton JB, RL. H. Translating teamwork behaviours from aviation to healthcare: Development of behavioural markers for neonatal resuscitation. BMJ Qual Saf. 2004; 13: i57-64.
- Morrow KJ, Gustavson AM, Jones J. Speaking up behaviours (safety voices) of healthcare workers: A metasynthesis of qualitative research studies. Int J Nurs Stud. 2016; 64: 42-51.
- DG S. Employee voice and employee retention. Acad Manag J. 1986; 29: 488-502.
- Almeida S, Frino B, Milosavljevic M. Employee voice in a semi?rural hospital: Impact of resourcing, decision?making and culture. Asia Pacific J Hum Resour. 2020; 58: 578-606.
- EW M. Employee voice and silence. Annu Rev Organ Psychol Organ Behav. 2014; 1: 173-197.
- Roussin CJ, Larraz E, Jamieson K, JM M. Psychological safety, self-efficacy, and speaking up in interprofessional health care simulation. Clin Simul Nurs. 2018; 17: 38-46.
- EW M. Employee voice behavior: Integration and directions for future research. Acad Manag Ann. 2011; 5: 373-412.
- Farh JL, Hackett RD, Liang J. Individual-level cultural values as moderators of perceived organizational support-employee outcome relationships in China: Comparing the effects of power distance and traditionality. Acad Manag J. 2007; 50: 715-729.
- Van Dyne L, JA L. Helping and voice extra-role behaviors: Evidence of construct and predictive validity. Acad Manag J. 1998; 41: 108-119.
- Sayre MM, McNeese-Smith D, Leach LS, LR P. An educational intervention to increase “speaking-up” behaviors in nurses and improve patient safety. J Nurs Care Qual. 2012; 27: 154-160.
- Edmondson A. The fearless organization: Creating psychological safety in the workplace for learning, innovation, and growth. Harvard Business School, editor. John Wiley & Sons. 2018.
- Sherf EN, Parke M, Isaakyan S. Distinguishing voice and silence at work: Unique relationships with perceived impact, psychological safety, and burnout. Acad Manag J. 2021; 64: 114-148.
- Carmeli A, Reiter-Palmon R, Ziv E. Inclusive leadership and employee involvement in creative tasks in the workplace: The mediating role of psychological safety. Creat Res J. 2010; 22: 250-260.
- Lee S, Dahinten V. Psychological Safety as a Mediator of the Relationship between Inclusive Leadership and Nurse Voice Behaviors and Error Reporting. J Nurs Scholarsh. 2021; 53: 737-745.
- Brown PJ, Borowitz SM, Novicoff W. Information exchange in the NICU: What sources of patient data do physicians prefer to use? Int J Med Inform. 2004; 73: 349-355.
- Jones L, Woodhouse D, Rowe J. Effective nurse parent communication: a study of parents’ perceptions in the NICU environment. Patient Educ Couns. 2007; 69: 206-212.
- Haig KM, Sutton S, JW. SBAR: A shared mental model for improving communication between clinicians. Jt Comm J Qual Patient Saf. 2006; 32: 167-175.
- Harris K, Treanor C, Salisbury M. Improving patient safety with team coordination: Challenges and strategies of implementation. J Obstet Gynecol Neonatal Nurs. 2006; 35: 557-566.
- Salas E, Shuffler M, Thayer A, Bedwell W, Lazzara E. Understanding and improving teamwork in organizations: A scientifically based practical guide. Hum Resour Manage. 2015; 54: 599-622.
- Nunez R, Lorenzo V, Navarrete M. Coordination among healthcare levels: Systematization of tools and measures. Gac Sanit. 2006; 20: 485-495.
- Tricco AC, Antony J, Ivers NM, Ashoor HM, Khan PA, Blondal E, et al. Effectiveness of quality improvement strategies for coordination of care to reduce use of health care services: A systematic review and meta-analysis. Cmaj. 2014; 186: E568-578.
- Jonker CM, Van Riemsdijk MB, BV. Shared mental models. In: Proceedings of International Workshop on Coordination, Organizations, Institutions, and Norms in Agent Systems; 2010 August. Heidelberg, Berlin: Springer. 2010.
- Gisick LM, Webster KL, Keebler JR, Lazzara EH, Fouquet S, Fletcher K, et al. Measuring shared mental models in healthcare. J Patient Saf Risk Manag. 2018; 23: 207-219.
- Dickinson TL, McIntyre RM. A conceptual framework for teamwork measurement. In: Brannick MT. SE, Prince CW, editors. Team Performance Assessment and Measurement. In: Psychology Press. 1997: 31-56.
- Floren LC, Donesky D, Whitaker E, Irby DM, ten Cate O, O’Brien BC. Are We on the Same Page? Shared Mental Models to Support Clinical Teamwork Among Health Professions Learners: A Scoping Review. Acad Med. 2018; 93.
- Morag I, AL Z. Evaluating teamwork among medical staff: How to measure and compare aspects of the team mental models of doctors and nurses. Appl Ergon. 2021; 94: 103418.
- Liaw SY, Wu LT, Wong LF, Soh SL, Chow YL, Ringsted C, et al. “Getting everyone on the same page”: Interprofessional team training to develop shared mental models on interprofessional rounds. J Gen Intern Med. 2019; 34: 2912-2917.
- Hirpa M, Woreta T, Addis H, Kebede S. What matters to patients? A timely question for value-based care. PLoS One. 2020; 15: e022785.
- S. Value-Based Health Care, a Global Assessment. 2016.
- King HB, Battles J, Baker DP, others. TeamSTEPPS: Team Strategies and Tools to Enhance Performance and Patient Safety. In: K. H, Battles JB, Keyes MA, others, editors. Advances in Patient Safety: New Directions and Alternative Approaches (Performance and Tools). Rockville (MD): Agency for Healthcare Research and Quality (US). 2008; 3.
- Garcia CD, Abreu LC, Ramos JL, Castro CF, Smiderle FR, Santos JA, et al. Influence of burnout on patient safety: Systematic review and meta-analysis. Medicina (B Aires). 2019; 55: 553-566.