
Review Article
Austin J Nurs Health Care. 2017; 4(1): 1036.
Telehealth Triage Nursing and Telemedicine: Joining Forces for Improved Care Delivery in a Primary Care Setting
Lee MR¹*, Ruehmann LL¹, Dively-White MT¹, Mathsen RL¹, Johnston JM¹ and Jensen TB²
¹Department of Nursing, Mayo Clinic, USA
²Department of Family Medicine, Mayo Clinic, USA
*Corresponding author: Lee MR, Department of Nursing, Mayo Clinic, 200 First Street SW, Rochester, Minnesota, USA
Received: March 21, 2017; Accepted: April 12, 2017; Published: April 20, 2017
Abstract
Changes in the United States’ system of providing health care are evolving from the health of individuals to population health management. More care is provided through non-visit care such as internet portals and telehealth triage. The following is a description of the telehealth triage system for ambulatory primary care at the Mayo Clinic, Rochester, Minnesota, which is based on a team model for community care. We describe the roles of members of the team, including the pivotal role of the telehealth triage nurse in collaboration with the Secondary Triage Additional Resource (STAR) providers in providing care while improving access and reducing emergency department visits. Telehealth nursing is a subspecialty of ambulatory care through the American Academy of Ambulatory Care Nursing and the American Nurses Association.
Keywords: Telehealth nursing; Telehealth triage; Primary care triage; Triage algorithms; Telehealth protocols; Team based patient care
Abbreviations
STAR: Secondary Triage Additional Resource; AAACN: American Academy of Ambulatory Care Nursing; ANA: American Nurses Association; RN: Registered Nurse; ECH: Employee and Community Health; APRN: Advanced Practice Registered Nurses; PA-C: Certified Physician Assistants; LPN: Licensed Practical Nurses; DST: Decision Support Tool; PAC: Patient Appointment Coordinator; MMoCC: Mayo Model of Community Care; PHM: Population Health Management; PCC: Patient Care Connection; POD: Provider of the Day
Introduction
The United States’ health care system is constantly evolving. Our focus is changing from the health of individuals to management of entire populations of patients. As the demand for affordable, highquality health care is on the rise across our nation, primary care organizations are challenged to create new, more efficient ways to deliver patient care. Reimbursement models and reduced access to a limited number of providers has led to the use of non-visit care, including internet portals for patients to access their care team to ask questions, obtain prescriptions, and communicate test results. Telehealth care has developed since the 1970’s as a quality, costeffective way to provide care to more patients, especially after regular clinic hours. Telehealth care reduces the off hours call burdens to the providers in primary care and visits to the local emergency departments. The use of triage tools provides consistent information and recommendations. The long-standing telehealth goal of ensuring the right patient receives the right level of care at the right time with the right provider is foundational to controlling the escalating cost of health care. Expanding the use of technology in health care delivery holds a promising solution [1-3].
Telehealth nursing is now a nursing subspecialty of ambulatory care through the American Academy of Ambulatory Care Nursing (AAACN) and the American Nurses Association (ANA) [2]. We will describe our institution’s current model for providing telehealth care to our employees and community through a population health management model.
History
In 2012 the process for a comprehensive redesign of our triage model of care delivery began. Our goal is to provide timely, safe, reliable, effective telephone triage for our patients. A multidisciplinary workgroup including front-line staff, nursing leadership, providers and administration identified four initiatives: call distribution (auto attendant), virtual centralization, complex patient care and secondary triage. The call distribution is intended to ensure the patient’s calls are appropriately triaged, scheduled and or resolved. Virtual centralization provides efficiency by utilizing telehealth triage RNs at different locations to answer phone calls within the primary practice. The complex patient program implements a reliable process for the management of complex patient care needs within the care team. The Secondary Triage Additional Resource (STAR) provider program uses a secondary provider covering all sites while maintaining RN autonomy. The initiative that we would like to explain in further detail is the STAR provider program.
Mayo Clinic’s primary care department, Employee and Community Health (ECH), embarked on a unique partnership between the telehealth triage RNs and primary care providers in November, 2014. Combining the expertise of the telehealth triage RNs with the provider’s clinical skill and knowledge has successfully expanded the services of the telehealth triage system to provide more non-visit care and patient centered advice beyond the triage algorithm tools.
STAR providers are staff physicians, Advanced Practice Registered Nurses (APRN) and Certified Physician Assistants (PAC) who are virtually available to the telehealth triage RNs to provide assistance with patient dispositions, pre-visit care or non-visit care. Family Medicine Providers are able to provide assistance for patients across the age continuum, while Internal Medicine Providers serve adult populations. The STAR provider’s primary responsibilities are to assist with level of care decisions, provide non-visit care, and assist with managing access challenges. It has been well received by patients, nurses, and providers.
Practice Demographics
Our primary care practice consists of seven clinics within a 15 mile radius in southeastern Minnesota. As a community practice, patients live within a 30 mile radius. Each clinic includes Family Medicine, Internal Medicine, and Pediatric and Adolescent Medicine divisions. As a teaching facility, three of our sites host a Physician Residency Practice. There are 308 providers (MD, APRN, PA-C, and resident physicians), 430 nurses (RN, LPN), and approximately 154,000 empaneled patients.
The telehealth triage RNs are virtually centralized, answering calls from all seven primary care clinic locations, serving patients of all age populations. There are 54 telehealth triage RNs with a designated full time equivalent of 34. There were greater than 152,000 calls managed by telehealth triage RNs in 2016. Staff is scheduled to work load, adjusting staffing numbers based on highest call volume times of the day. There are approximately 21 STAR providers who have dedicated time to the role in four hour increments. This results in approximately 1.0 to 2.0 full time provider equivalents.
The telehealth triage RNs are within Mayo Clinic’s Department of Nursing and are supported by a Medical Director, Nurse Administrator, Nurse Manager, Nursing Education Specialist (NES) and Telehealth Nurse Coordinator. The Telehealth Nurse Coordinator assists with the orientation process for new hires, but has a primary focus of maintaining the integrity of the program. To ensure patients receive high quality, safe telephonic care, the coordinator provides routine and targeted call monitoring, including documentation review. Coaching and mentoring new and seasoned staff is an important part of the coordinator’s role.
Decision Support Tool (DST) and Algorithms
Mayo Clinic’s Primary Care Ambulatory ECH Practice supports the clinical needs of patients by offering access to experienced registered nurses during business hours to assist with safe, efficient disposition recommendations. The telehealth triage RNs use an electronic Decision Support Tool (DST) built on a binary logic system to guide them through a network of sophisticated, evidence-based algorithms. The algorithms are designed to complement the critical thinking skills of experienced telehealth triage RNs to provide a comprehensive, efficient assessment of the patient’s acute symptoms. The DST delivers a suggested disposition for the patient including: ambulance, emergent care, urgent care, acute appointment, routine appointment, provider advice, or home care. The RN embraces a holistic approach by considering the patient’s medical history and current symptom pattern before agreeing or disagreeing with the system recommendation. The nurse may change the endpoint of the DST to either a more or less acute intervention.
The integrity of the system is maintained with continuous review by the Triage Algorithm Review Board, which is a multidisciplinary team, with front-line telehealth triage RNs heavily involved. They identify system revisions needed and test for accuracy after any changes have been made. Specially trained RNs make the desired edits to the DST system, and everyone on the team is involved with reviewing the most current evidence-based literature.
The successful pairing of experienced registered nurses using the DST to guide the most appropriate disposition for the patient, based on the nurse-patient interaction, has proven to provide safe, timely care. However, as the climate of healthcare provision evolves, patients are accessing the services of primary care with increased complexity of their healthcare needs, often complicated with underlying chronic conditions. The trend of increased patient acuity coupled with the demand for non-visit care by “healthy” patient populations creates new challenges for telehealth nursing.
The STAR provider adds another layer of expertise to the nurses’ knowledge and use of the DST. The telehealth triage nurse can contact the STAR provider by phone for any question or concern. Each STAR provider for Family Medicine and Internal Medicine is located at another site and uses the same type of telephone system as the PAC and telehealth triage RNs. Most of the sites have access to an electronic display board showing triage RNs and STAR providers who are currently logged into the system. The boards provide a constant visual of which nurses are on a call, who is available for the next call, and who is taking a break. This improves efficiency and yields statistics that help with staffing and service improvements. The STAR provider makes recommendations for additional advice for the patient, orders pre-visit tests to expedite office visits, may prescribe medication for patients who fall out of RN treatment protocols, assist with routine medication refills and may conference call with the patient and nurse for additional information and recommendations. Use of the STAR has improved the safety and dispositions of our increasingly complex patient population. It also has reduced emergency department visits, reduced the online portal messages to the care teams and helped ECH provide half of our patient care as non-visit care.
Process Flow
The flow of the ECH telephone triage is seen in Figure one. The calls are sorted into emergent, complex care patient, care coordinated patient and routine appointments. Patients needing forms or administrative information are routed to the secretaries. Those with acute issues are triaged by the telehealth triage RN and those needing routine appointments are directly scheduled (Figure 1).
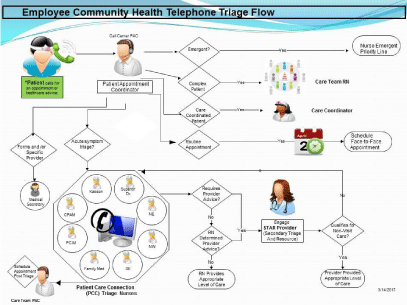
Figure 1: PCC work flow.
Employee and Community Health (ECH) has a large, diverse patient population, which generates more than 152,000 calls to the RN triage line per year. Efficiently routing these calls to meet patient needs is a challenging task. Patient Appointment Coordinators (PAC) provide the first touch for patients who call into the primary care clinics, and ensure the patient is connected to the appropriate care team member. The PAC serves an important role in the patient’s continuum of care by determining if the patient is having emergent symptoms, which require activation of the triage RN emergency priority line, or having non-life-threatening symptoms that would benefit from a telehealth triage RN assessment to determine the most appropriate disposition.
The highly skilled telehealth triage RNs will use the DST and honed critical thinking skills to determine the most appropriate level of care for the patient, or per RN discretion will seek STAR provider assistance for disposition recommendations, appointment access assistance, or possible non-visit care. After providing the patient with helpful self-care instructions, the patient is transferred back to the PAC for appointment scheduling.
If the patient has complex medical conditions and requires triage the PAC will quickly check the electronic medical record to determine if the patient has an assigned RN Care Coordinator, or if a designated complex care patient should be transferred to the Care Team RN to manage their needs.
Model of Care
The Mayo Model of Care (MMoC) places the patient at the center of an integrated clinical practice, daily striving to embody the elements of care: teamwork, respect, innovation, culture, quality, and scholarship [4,5]. This model is foundational to daily care. With the changing healthcare climate within the United States, health systems are moving to Population Health Management (PHM). Mayo approaches the population health transition as an opportunity to further its integrated practice across the enterprise and translate the MMoC within the primary care setting to the Mayo Model of Community Care (MMoCC). The MMoCC has several clinical programs including the following key components: access, care coordination, care transitions, chronic condition management, community engagement, palliative care, patient engagement, prevention, team-based care, and wellness. The telephone triage RNs are pivotal team members within the Mayo Model of Community Care as a critical link to assure the patient receives the most appropriate level of care [6].
The telehealth triage RNs are often the first or second line of access for the patient. The RN uses his/her critical thinking skills in combination with the clinical DST to determine the right level of care and determine access prioritization. The RNs’ clinical back grounds vary, with each bringing a unique skill-set to support the patient’s triage experience. When needed, communication between telehealth triage RNs occurs in person and virtually using an instant messaging system. The patient benefits from the telehealth triage RN team in addition to the expertise of the STAR provider and other MMoCC team members. For example, if a patient calls the triage line with cardiac symptoms, they will receive a comprehensive assessment from the telehealth triage RN and benefit from the RN’s critical thinking skills combined with the DST. Another option the RN has available is consulting the STAR provider, who can assist in determining the most appropriate level of care for the patient. If the STAR provider determines the patient does not need emergent care, but would benefit from a cardiology evaluation, the STAR provider can refer the patient to the Integrated Community Specialty Practice embedded within the primary care practice. The telehealth triage RN facilitates many transitions of care in their practice ranging from calling 911 for emergent residential calls to connecting a patient to a social worker within the clinical practice (Figure 2).
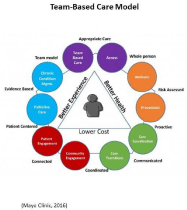
Figure 2: Team-based model.
Examples of Collaboration
Thirty-six year old female placed a call to the RN triage line about 2:00 p.m. She described painful swelling of her left calf that had gotten progressively worse over the past 24 hours. She denied trauma, shortness of breath, or chest pain. Documentation in the patient’s medical record revealed she was taking oral contraceptives, and unable to stop smoking after several attempts. The telehealth triage RN was suspicious of a Deep Vein Thrombosis (DVT), and consulted the STAR provider to assist with mid-afternoon access constraints. The STAR provider was able to add an appointment to the patient’s care team schedule and ordered a pre-visit ultrasound, which was positive for DVT. The patient was admitted directly to the hospital and by-passed the Emergency Department.
The mother of a four-year-old boy called concerned about her child having brief episodes of staring and abrupt pauses in activity, with no subsequent symptoms of confusion or drowsiness following the episodes. Ten minutes prior to the mother’s phone call he experienced an episode of staring that lasted approximately 5-10 seconds. However, he was alert, oriented, and interacting appropriately with his family since that time. The telehealth triage RN was suspicious of petit mal or absence seizures, but questioned the appropriate level of care. She consulted with the STAR provider who recommended she take her son to the Emergency Department for a Pediatric Neurology evaluation. This prevented an office visit to expedite care to the more appropriate provider.
Forty-two year old male called requesting prednisone for an asthma exacerbation. His symptoms consisted of a dry, intermittent cough and shortness of breath with exertion. He stated this is his “usual” asthma flare with an upper respiratory viral illness. He denied chest pain, respiratory distress, or persistent cough. He has a tight work schedule and prefers to not come in for an appointment. The telehealth triage RN consulted the STAR provider who verified in the electronic medical record that the patient typically needs prednisone for his asthma exacerbations, and does well with it. The provider ordered the prednisone as requested. The RN reviewed signs and symptoms of worsening illness, and provided home care instructions. The non-visit care prevented an office visit.
Forty-eight year old female from Somalia called with concerns of headache and breathing problems. A Somali interpreter was conferenced into the call. The patient stated that her “whole body” was feeling heavy and she described pain in her head and back. She noted that she had been feeling confused and that her breathing was heavy, even at rest. She continued to provide positive responses to all emergent symptoms during the triage assessment. The telehealth triage RN consulted the STAR provider who was familiar with the patient and able to provide a safe clinic disposition recommendation. An Emergency Department visit was successfully avoided.
Thirty-four year old professional called into the RN triage line to ask about depression. The PAC immediately transferred the patient to the RN Emergent priority line, who determined the patient was actively suicidal and had a plan to jump from the highest level of stairs in one of the buildings on campus. The telehealth triage RN immediately conferenced the STAR provider who joined the conversation. The STAR talked to the patient and confirmed that he was actively suicidal, and at high risk for self-harm. She talked to the patient to calm him while signaling another care team member, who notified security to assist with locating the patient. As security arrived the patient agreed to go with them to be evaluated in the local emergency department and be treated. The rapid collaboration between the PAC, triage RN, STAR provider, and security prevented the patient from self-harm.
Discussion
Benefits
Prior to implementing the STAR program, the telehealth triage RNs communicated with primary care providers through an internal messaging system, which didn’t allow for immediate assistance with patient dispositions. That process generated several touches by care team members before providing the advice or care the patient needed. For urgent needs the providers were paged, which often interrupted face-to-face patient care, and quickly became a source of provider dissatisfaction. Patients were often advised to seek a level of care that was higher than needed, which was viewed as a safe disposition without disrupting patient care within the care teams, but not a wise use of healthcare resources.
The benefits of implementing the telehealth triage RN and STAR provider program have been numerous. By ensuring patients access the healthcare system with the most appropriate level of care we conserve healthcare dollars and resources. The STAR providers also provide a large percentage of non-visit care, such as prescriptive management for episodic, acute illness, or making recommendations that are beyond the RN scope of practice. The first four months after implementation, we saved approximately 100 Emergency Department visits every month by providing prompt access to primary care. STAR providers order pre-visit laboratory tests and x-rays, which increases the efficiency of face-to-face visits. Having the STAR providers available for questions and assistance with patient dispositions has reduced the need for telehealth triage RNs to interrupt primary care providers and care team nurse colleagues during busy clinical hours. Many of the providers enjoy teaching, which has been an unanticipated benefit of professional growth for the triage RNs. The triage RNs have not only become more knowledgeable, but more confident in their triage assessment skills, and many have expressed greater job satisfaction. We don’t yet have metrics to measure patient satisfaction, but overall the anecdotal feedback from patients has been extremely positive.
Challenges
Implementation of any new program, especially one that impacts scarce provider resources, will hold challenges. We are fortunate that our leadership is committed to the Mayo Model of Community Care, which holds collaborative team work as foundational to meeting the needs of the patient. The STAR program aligns with that model by providing support to the RNs on the front lines as they strive to provide safe patient dispositions. However, despite high-level support, we still struggle with lack of STAR provider coverage during all hours of operation, specifically early morning hours and end of the day. The providers are scheduled for four-hour shifts, which is dedicated time, meaning they aren’t able to see patients during their scheduled shift. During a busy day, that can increase the workload of care team colleagues. Another challenge we discovered is not all providers are comfortable with providing non-visit care or assisting the RNs with patient directives. Some become comfortable after coaching from other STAR providers, but others prefer to not participate in the program. Due to the nature of the program and the virtual connection, STAR providers receive questions about patients in other Divisions. A Family Medicine provider may be asked to assist with managing a patient whose primary provider is in Internal Medicine, or Pediatric Adolescent Medicine, and vice versa. That potential was met with great apprehension by many of the providers prior to implementation. However, the experience has been positive overall and has gained broad support in ECH. On rare occasion the RN will disagree with the recommendations of the STAR provider, which may cause an uncomfortable conflict. The RN will ensure the patient is comfortable with the recommendation, and instruct the patient or care giver about the symptoms that may indicate worsening or progression of their condition. If worsening, the patient will be encouraged to call back, or seek care in the Emergency Department if the clinic is closed.
Lessons learned
Initially the telehealth triage RNs were apprehensive about calling the STAR providers for advice. However, as they became more familiar with the process and the providers, they embraced the program. The level of care data demonstrates the RNs are accessing the STAR provider for about 20% of calls, which are approximately 20,000 patients per year.
The volumes of calls and the breadth and depth of symptoms and questions the telehealth triage RNs manage was astounding to many of the providers. That revelation has created a deeper appreciation and respect for the telehealth triage RN, which has fostered an enhanced, trusting relationship. The RNs are feeling more valued in the important role they play in patient care.
Patients who gain the most
At the discretion of the telehealth triage RN, the STAR provider may be consulted for patients that may benefit from talking directly to a provider, those needing pre-visit tests, and those who qualify for non-visit care. The patients that reach the endpoints of emergent care, provider advice within four hours, or acute appointment have the most to gain by partnering the RN’s assessment with the STAR provider recommendations.
Safety
How safe is non-visit care is a fair question to ask. It’s a question we asked too as we brainstormed ways to deliver cost-effective, efficient patient care, yet maintain safe, high quality care.
During the pilot phase of implementing the STAR provider program, patient-nurse-provider interaction data was documented in a data base. Items tracked include patient identification number, patient symptoms, RN derived endpoint, and provider recommendation. Between January and April, 2015, telehealth triage RN’s consulted the STAR provider for 2,780 of the 54,475 patients they triaged. Of those patients, 39% had pre-visit tests ordered, 56% were given recommendations by the STAR provider that were beyond RN licensure, and 13% of the patients had no change in the RN’s original disposition. To determine the safety of the STAR provider’s decisions, we examined those patients who had the greatest downgrade between RN and provider recommendations. Twentyeight patients were downgraded from the RN derived endpoint of emergent care, to a provider’s recommendation of non-visit care. The 28 patient medical records were reviewed to determine if medical intervention was needed within two weeks following their triage encounter. Chart audits revealed fifteen patients required no further medical intervention after receiving non-visit care. Eleven patients had subsequent office visits, but only three were related to their original triage encounter, and required follow-up care for persistent respiratory symptoms. Two patients presented to the emergency department within 24 hours. One with dysfunctional vaginal bleeding, and the other was discharged to obtain a stool specimen for C-difficile. Ten of the 28 patients had seen their primary care provider prior to their triage encounter, and the STAR provider supported the primary provider’s original plan of care. The results of the chart audit demonstrated combining experienced telehealth triage RNs with the clinical expertise and prescriptive authority of the STAR providers supports a safe, efficient model of care delivery for a primary care population (Figure 3).
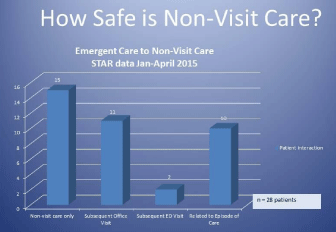
Figure 3: Non-visit care.
Conclusion
The Mayo Model of Community Care emphases collaboration between teams of health care professionals to provide evidence based coordinated, cost-effective, safe, appropriate care to populations of patients. The Employee and Community Health outpatient telephone triage system promotes these elements and has improved access by providing fifty percent of the patient experience as non-visit care.
Concordance
Algorithms contain logically sequenced, evidenced based, clinical questions to determine the acuity of symptoms being presented by a patient. The algorithms are designed to rule in or rule out the most emergent symptoms first. The binary logic system within the decision support tool displays questions based on the previous answer selected.
Care Coordination (CC) RNs work with patients who have chronic conditions and complex health care needs to improve their self-management skills, resulting in fewer hospitalizations, medical interventions, and Emergency Department visits. The Care Coordination RNs collaborate with the patients to develop a proactive plan for patient self-management and options for efficient, effective care when needed.
Care Team (CT) RNs work with primary care providers, providing direct patient care, patient education, and follow up on patient concerns. Care Team RNs also provide triage assessments using the same Decision Support Tool that the Patient Care Connection RNs use.
Patient Appointment Coordinators (PACs) receive incoming calls and determine whether they can schedule an appointment for the patient, whether to route the call to a Patient Care Connection RN for triage, or whether to route the call to a Care Team RN for follow up on previous concerns.
Patient Care Connection (PCC) or telehealth triage RNs receive incoming calls and triage patients, identifying the nature and urgency of patient health care needs as well as determining the appropriate disposition. Telehealth Triage RNs focus on assessment, prioritization, and referral to the appropriate level of care.
Protocols allow registered nurses to renew prescription medications, order labs, x-ray, treatments, or medication adjustments. Protocols are developed and approved by a multidisciplinary team including RNs, pharmacists, and authorized prescribers. Patients must meet strict inclusion criteria specifically designed for each protocol. A patient that doesn’t meet the protocol may receive an appointment or be discussed with the STAR provider.
Provider of the Day (POD) is a team provider who responds to acute or urgent issues when the STAR provider is not available. They also manage patient needs that need same-day response and medication renewals.
Secondary Triage Additional Resource (STAR) providers (MDs, APRNs, or PA-Cs) must have authorized prescribing privileges and be accessible virtually for the Patient Care Connection RNs via the Automatic Call Distribution management system. They actively collaborate with the RNs to ensure the right patient gets the right level of care, with the right provider, at the right time. They are a virtual resource for the telehealth triage RNs and assist with patient disposition decisions during hours of operation.
References
- Kvedar J, Coye MJ, Everett W. Connected Health: A Review of Technologies and Strategies to Improve Patient Care with Telemedicine and Telehealth. Health Affairs. 2014; 33: 194-199.
- Espensen, Maureen. Telehealth Nursing Practice Essentials. AAACN, American Academy of Ambulatory Care Nursing, Pitman, N.J. 2009.
- Rutenberg, Carol, Greenberg, Elizabeth M. The Art and Science of Telephone Triage. Anthony J. Jannetti, Inc., Pitman, N.J. 2012.
- Mayo Clinic. The Mayo Model of Community Care. 2016.
- Mayo Foundation for Medical Education and Research. Mayo Clinic: Mayo Clinic Model of Care. 2014.
- Matthews MR, Miller C, Stroebel RJ, Bunkers KS. Making the Paradigm Shift from Siloed Population Health Management to an Enterprise-Wide Approach. Population Health Management. 2017.