
Special Article - Cardiac Nursing
Austin J Nurs Health Care. 2017; 4(1): 1038.
Women’s Experiences and Decisions Related to Subsequent Pregnancies after Diagnosis of Peripartum Cardiomyopathy
Donnenwirth J¹* and Hess RF²
¹Administration, Aultman College, USA
²Research Department, Research for Health, USA
*Corresponding author: Donnenwirth J, Aultman College, 2600 Sixth St. S.W., Canton, OH, 44710, USA
Received: June 23, 2017; Accepted: July 10, 2017; Published: July 19, 2017
Abstract
Peripartum Cardiomyopathy (PPCM) is an idiopathic form of dilated cardiomyopathy which presents in a woman, without a pre-existing heart condition, in her last trimester of pregnancy or first five postpartum months. The trauma of this diagnosis is often augmented by a directive to forego future childbearing. Knowledge is lacking about women living with PPCM and their decisions about Subsequent Pregnancies (SSPs). The aim of this qualitative study was to explore the experiences of women living with PPCM and their decisions regarding a SSP.
A modified grounded theory guided the study. A purposive sample of 16 women was recruited using admission data of a hospital in northeast Ohio and from membership in a Facebook PPCM survivor group. Semi-structured interviews were conducted face-to-face and by telephone. Data were analyzed using constant comparison procedures. Four women had an SPP; seven women had none; three were still undecided. The core variable was the risk of relapse into heart failure impacts decisions about future pregnancies. Four major themes were: receiving the ultimatum ‘no more children’, weighing the risks of a SSP, making the decision about a SSP, and experiencing a SSP. Women with PPCM who desire additional children face emotional distress before, during, and after the decision making process because personal wishes and plans conflict with others’ opinions. Nurses may mitigate the trauma by helping the healthcare team plan an appropriate time and way to speak about future childbearing and by providing support and guidance when women are making a decision about a SSP.
Keywords: Decision making; Grounded theory; Heart failure; Peripartum cardiomyopathy; Subsequent pregnancy
Abbreviations
EF: Ejection Fraction; IVF: In-Vitro Fertilization; LVEF: Left Ventricular Ejection Fraction; LV: Left Ventricular; PPCM: Peripartum Cardiomyopathy; SD: Standard Deviation; SSP: Subsequent Pregnancy; SSPs: Subsequent Pregnancies
Introduction
Peripartum Cardiomyopathy (PPCM) is an idiopathic form of dilated cardiomyopathy which presents in a woman, without a pre-existing heart condition, in her last trimester of pregnancy or in the first five months postpartum. It is characterized by heart failure secondary to left ventricular dysfunction [1] with an Ejection Fraction (EF) less than 45% [2]. The incidence of PPCM varies around the world, from 1 in 300 to 1 in 3,000 live births [3-7]. Risk factors include pregnancy over the age of 25, black ethnicity, parity of four or greater, pregnancy- associated hypertension, and multiple gestation pregnancy [4,8].
The aim of our study was to explore experiences of women living with PPCM and their decisions regarding Subsequent Pregnancies (SSPs). Much prior research done on women with PPCM who had a SSP focused on incidence, maternal morbidity and mortality, and birth outcomes [1,3,6,9-12]. SP is associated with a risk of relapse when there is a deterioration of Left Ventricular (LV) function, particularly where the LV dysfunction persists after treatment [9]. Ten to fifty percent of women who have experienced a complete recovery from PPCM relapse into heart failure during or after a SSP [5,11,13]. SSP-related deaths continue to be a grave concern, with a mortality rate reported to be 16% [9].
Research on PPCM and subsequent pregnancies from a woman’s perspective is rare. Many women diagnosed with PPCM desire to have more children [9,14,15]. Hess and Weinland’s [15] analysis of 247 online postings related to PPCM revealed that SSP was the most frequently discussed topic. Some women described getting pregnant again and encouraged others, during support group encounters, to have hope. Some women expressed the pain and sorrow of an unfulfilled longing for more children while others considered the risk of relapse or death too great. Dekker and colleagues [14] analyzed posted narratives of 92 women diagnosed with PPCM active in online support groups. Many of the first time mothers were unhappy with the advice to not get pregnant again. Nine women had SSPs; eight had good outcomes; one relapsed into heart failure but recovered. Many others were still hoping to have another child. Patel et al [12] studied 19 PPCM women in Sweden; nine women (47%) desired more children while ten (53%) believed the risk of relapse was too great. None of these women had yet had a SSP. Chee [16] studied nine women with PPCM in Malaysia; two women who had regained normal LV function got pregnant against advice. One woman’s pregnancy was terminated at seven weeks gestation; the other woman gave birth without complications.
Methods
Design and sample criteria
A grounded theory design, with a focus on decision making, guided our study. Ethical approval was granted by the Human Research Review Board of the Aultman Health Foundation, Ohio USA. A purposive sample was recruited using these inclusion criteria: diagnosis of PPCM within the previous five years, ability to read and speak English, and agreeable to a tape-recorded interview.
Recruitment of participants
Since PPCM is a rare condition and recruiting participants is a challenge, two approaches were necessary to obtain an adequate sample size. First, the admission data of a hospital in northeast Ohio was accessed for cases of did not return our phone call; three were interviewed. After receiving ethical approval for a different recruitment tactic, messages with the consent form and interview guide were posted on a Facebook PPCM survivor group. Included on the consent form was a description of the researchers’ expertise, previous research on PPCM, and objectives of this study. Thirtyfour women initially contacted us asking for more details; 19 did not contact us again. Their reasons for non-participation are unknown. Two others were not eligible; 13 were interviewed. Each woman had the opportunity to ask questions before giving oral consent to participation. No participants withdrew from the study once they consented to the interview.
Data collection
The first author conducted 11 interviews and the second author did five. Three interviews took place face- to-face and thirteen were conducted over the telephone. Each interview lasted about 60 minutes. The face-to-face interviews were conducted in a private setting, either at the hospital or the participant’s home. Interview questions were broad and open-ended, such as: Tell me the background of your diagnosis with PPCM; describe being told about future pregnancies; talk to me about your decision about more children. Probing questions were used to delve deeper into participants’ comments. Field notes were made during the interviews. Each interview was transcribed verbatim by a hired transcriptionist. To maintain confidentiality, information that might identify the woman, including names of spouse, children, physicians, hospitals, and cities, was obscured in the transcripts.
Data analysis
Data analysis was done using a modified constant comparison method [17]. Each author individually used the following steps for the first 12 interviews. First each transcript was read while listening to the tape-recorded interview to be immersed in the data. At the next reading, illustrative words and phrases were highlighted with a pen. During the third reading, these key words and phrases were extracted and preliminary themes were developed. When comparing each of our themes we decided that data saturation had not been reached; the narratives were wide ranging and data quality was not rich enough to justify the themes [18]. Therefore four more women were interviewed with probing questions pulled from the original narratives. The previous steps were repeated with all 16 interviews and data saturation was reached. All significant statements related to the topic of SSP were extracted from each interview and the analysis process was repeated. Both authors independently wrote preliminary themes and sub-themes and then refined them together.
Results
Participants’ characteristics
Sixteen women living in the United States were interviewed with a mean age of 35.8 years; the majority were Caucasian, married, had at least a college education, and primiparous at diagnosis. Participants’ demographics are found in Table 1, comparing details at diagnosis and at time of interview. Table 2 details the participants’ cardiac and pregnancy history in relation to their PPCM diagnosis. One woman was diagnosed with PPCM before giving birth. Seven women had symptoms of PPCM before giving birth but were diagnosed after delivery. Eight women became symptomatic and were diagnosed during the postpartum period. Over half of the women were initially diagnosed with PPCM during their first pregnancy. Three women had decided before being diagnosed with PPCM that that pregnancy would be their last one. Seven women took measures to not get pregnant again after the PPCM diagnosis. Four women had a total of seven additional pregnancies. Three women were undecided and still weighing the risks of another pregnancy. Table 3 displays characteristics at diagnosis and summarizes reasons for or against SSPs; contraceptive methods are noted if known.
Variable
N (%)*At diagnosis
N(%)* At interview
Age
Range: 21-42 years of age
Range: 24-48 years of age
Mean 31.73 years (SD 6.3)
Mean 35.8 years (SD 6.3)
20-29
6 (37.5)
3 (18.7)
30-39
7 (43.7)
7 (43.7)
40=
2 (12.5)
5 (31.2)
Marital status
Married
15 (93.7)
13 (81.2)
Single
1 (6.2)
1 (6.2)
Separated
0 (0.0)
1 (6.2)
Education level attained
Some high school
2 (12.5)
High school graduate
2 (12.5)
Some college
1 (6.2)
Bachelor’s degree
4 (43.8)
Master’s degree
4 (25.0)
Race
Caucasian
15 (93.7)
Other
1 (6.3)
Employment status
Homemaker
3 (18.8)
5 (31.3)
Employed
12 (75.0)
8 (50.0)
Unemployed/on disability
0 (0.0)
2 (12.5)
*If sum does not reach sample size, this is an indication of missing data.
Table 1: Demographics of participants at diagnosis and at interview.
Variable
N(%)* at diagnosis
N(%)* at Interview
Personal history of cardiac problem
Yes
2 (12.5)
No
13 (86.7)
Family history of cardiac problems
Yes
3 (18.8)
No
12 (75.0)
Ejection Fraction (Mean 26.9 (SD 9.9.)
< 20%
3 (18.8)
20-30%
4 (25.1)
>30%
3 (18.8)
Number of Pregnancies
Beforediagnosis
Since diagnosis
0
9 (56.2)**
12 (75.0)
1
3 (18.7)
2 (12.5)
2
3 (18.7)
1 (6.2)
3
0 (0.0)
1 (6.2)
5
1 (6.3)
0 (0.0)
Subsequent pregnancy after diagnosis
Yes
4 (25.0)
No
12 (75.0)
*n(%) not equal sample size (100%) because of missing data; **9 women had diagnosis after first
pregnancy and birth
Table 2: Participants’ cardiac and pregnancy history.
Participant No.
Age at diagnosis
No. of pregnancies before PPCM diagnosis
Pregnancy at which diagnosed with PPCM
No. of subsequent pregnancies
Reason(s) given to risk or not risk a subsequent pregnancy
Method to prevent subsequent pregnancy
1
21
0
first
0
Had heart transplant; Danger of anti-rejection drugs on unborn fetus
Vasectomy
2
38
2
third
0
Pre-diagnosis decision
Vasectomy
3
28
1
second
0
Too many medical problems
Tubal ligation
4
26
0
first
0
Cardiologist adamantly against; not fully recovered; Husband not want to lose her
Unknown
5
33
0
first
1, may be more
EF** recovered, off medications –Didn’t want to risk life again but had done nothing definitive - “I think this is it.”
Unknown
6
27
0
first
0
Physically never recovered
Hysterectomy
7
40
1 (twins)
Second (twins)
0
Pre-diagnosis decision Had as many children as wanted
Stopped IVF*
8
unknown
0
first
1
Strongly wanted 2nd child; but wouldn’t risk 3rd ; relapsed during 2nd; husband older
Tubal ligation after PPCM-SSP
9
42
0
first
0
Already 42 years old; Cardiologist against it
Unknown
10
23
0
first
2
Quick recovery after diagnosis; Closely monitored – OK for 9 months - Asymptomatic drop in EF** at delivery of PPCM-SSP; Had new husband -wanted children with him
Currently pregnant
11
30
2
third
3
Never well informed of diagnosis & risks; told ‘no more’ after 6th child – still risking
No birth control for past 5 years
12
35
5 (miscarriages)
Sixth (twins)
0
Pre-diagnosis decision (twins); difficult pregnancy & delivery
Stopped IVF*
13
32
0
first
0
Told by doctors could die - Scared of risks
Tubal ligation
14
28
1
second
None, yet
Too many unknowns to risk SSP now - still considering having another child
Unknown
15
34
2
third
Physicians said it was too risky; Respected husband’s wish/age
Vasectomy
16
39
0
first
None, yet
considering SSP while weighing risks
Unknown
*IVF In Vitro Fertilization; **EF - Ejection Fraction
Table 3: Characteristics of women with PPCM and their reasons to risk or not risk pregnancy after their PPCM diagnosis.
Overview of theoretical model
The core variable identified through data analysis was the women’s realization that the risk of relapse into heart failure had changed their lives in relation to future pregnancies. Figure 1 is a graphic illustration of the process model grounded in the descriptions provided by the participants. Most women had planned a life with a specific number of children; some intentionally delayed childbearing until other parts of their life’s plan were in place. Everything changed when abruptly confronted with a life-threatening cardiac condition. Cardiac failure along with the continued risk of relapse led to physicians’ ultimatum of no more children for most of the participants; this risk was the filter by which the woman, and others in her life, came to a decision for or against another pregnancy.
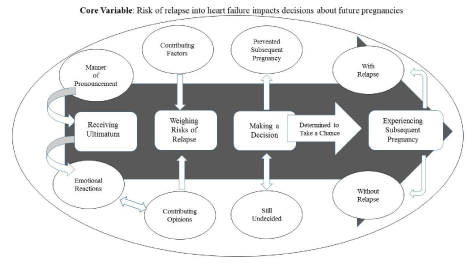
Figure 1: Process model of decision making for subsequent pregnancy after diagnosis of PPCM.
Life’s plans were particularly altered for the women who wanted more children but did not take the risk. These changes involved grieving and acceptance. One woman who risked a SSP said it this way.
I was 33 years old. I had waited all my life to have a baby. I did everything, I thought, the right way. I went to school. I got my degree. I started a career. I got married. I had waited my whole life to have a child. I never wanted just one child… So I decided. I wanted to titrate my medication at the one year mark. Everything stayed great. To me, I was like, ok. I am recovered. And that was pretty much how I made the decision. I felt it was my decision.
Another woman, who had not yet chosen to not get pregnant again, described living with PPCM and the risk of relapse this way. “It really makes you just see that your life can be altered at any moment and that you can be really at the will of it -of whatever it is that God wants.”
Themes
Four major themes were identified from the interviews: receiving the ultimatum ‘no more children’, weighing the risks, making the decision about a SSP, and experiencing a SSP. Nine sub-themes are described with quotes in Table 4.
Themes
Sub-themes
Quotes
Receiving the ultimatum ‘no more children’
Manner of pronouncement
Probably every single OB, cardiologist, assistant that came in, I was repeatedly told, “You know you can’t have any more children”. That was the only thing that was drilled into my head every moment I was at the hospital; that it could kill me, and that it’s a major no-no. They wanted me to go and get surgery and get, you know, “fixed”, you know. They wanted to make sure I had a birth control plan. That was definitely drilled.
Emotional reactions
I was devastated. Basically that destroyed everything inside of me. I was in shock.
Weighing the risk of relapse
Contributing factors
physically couldn’t keep up with more than one child. I have never physically been the same body wise since that.
My husband and I are not the youngest parents in the world.
We were pretty sure going in, especially with twins, that we would probably be done [having more children].
Contributing opinions
When we found out the chances of relapse were high my husband was fine with one child. He decided he didn’t want any more.
My heart was structurally sound, that is why [the physician] gave me the go ahead with the pregnancy.
Making the decision
No more pregnancies
Even a year out, two years out, [the doctors] kept saying the same thing. They scared me enough that when my son was six months old I went ahead and had a tubal. Some days I feel a little sad, but I’m 37, so I’m not a spring chicken anymore.
Still undecided
We want to give our daughter a sibling, for multiple reasons.
Determined to take the chance
I was angry. I didn’t want to give it up, not being my choice. With them telling me I couldn’t have subsequent children after my first one, I was ....kinda....like, I took it as a dare. No, not really. I had it set in my mind. I will have another child! I will prove them wrong.
Experiencing a subsequent pregnancy
Without relapse
The pregnancy was good. After having the baby I felt wonderful. I thought, “This is how it’s supposed to be.” I felt a 1000 times better having this baby.
With relapse
[With] my third and fourth children [I] had swelling. When I told [the doctor], she said I had to go immediately to a cardiologist.
Table 4: Themes and sub-themes illustrated with quotes.
Receiving the ultimatum ‘no more children’
The women in this study described frightening symptoms and difficult circumstances leading up to the diagnosis of PPCM. In addition, the manner in which most of the women were told they should not get pregnant again compounded the trauma. The diagnosis and the ultimatum ‘no more children’ were sudden and unexpected. Several women were told to not have any more children the same time they were informed of the diagnosis. One woman awoke in the intensive care unit. She said,
I wish that someone had thought about my emotional well-being as much as my physical well-being. Being told [to not have any more children] while laying there; to be in the state that you’re in and have someone throw that at you is SO depressing and saddening. You’re so scared in that moment. It’s not what you need. No one needs to say it. You’re not going to get pregnant…you know… I’m strapped up in an ICU to about 50 cords. I’m not getting pregnant anytime soon. It’s so honestly ridiculous. And I was told by multiple people in the most unkind ways. They walk into my ICU room and are like, “You know, you absolutely can never get pregnant again”. It’s just the most inappropriate time to have that discussion.
Emotional reactions varied and changed over time. There was shock, regret, sadness, guilt, and even defiance. One woman explained,
For the first year and a half that was a struggle. Still I tried to be thankful for what I have; for the new life I have; for the baby I have. But I think it’s just a mother’s nature, you know; it’s just that longing. I felt bad for my son, who like, he can never have a brother or sister. I felt guilty, you know, for not giving my husband another child.
Weighing the Risks of a Subsequent Pregnancy
Several factors contributed to a woman’s decision for or against a SSP including the severity of her medical condition, her level of recovery, her personality, age, and the number of children she already had and the number she wanted.
Within the year after my first was born my ejection fraction had returned to normal. At that time I had done enough poking around to find, to find that at another hospital, locally, there was a specialist who was taking an interest in PPCM. And…from what I had read and what I had researched I was realizing that the decision to not have other children was not a ‘one size fits all.’ Not necessarily.
Various people voiced their opinions on the decision about a SSP including spouses, other family members, cardiologists, obstetricians, and PPCM survivors. Several spouses said they preferred their wives alive rather than risking heart failure relapse and death to leave the family without a wife and mother. One woman said, The thing that [my husband’s name] and I have talked about is him, feeling like he’s got some concerns. [My husband says,] “What if it happens again and its worse this time, and we lose you? Then it’s me with one or two babies and I don’t have you, we don’t have you.” It’s better that it’s just the three of us then. I think he wants to really weigh the risk when we actually get to the point of really trying to get pregnant again.
Physicians expressed differing opinions about SSP to the women. Some were strict in their advice against another pregnancy. One woman explained, “The cardiologist said, “Well, you know, you are 23 years old. Your ejection fraction isn’t too far off of normal. We will put you on this medication and you will get better. . . Don’t ever get pregnant again!” Other physicians listened to the woman’s desire for more children and developed acceptable follow up plans. Women also discussed this difficult decision with women in PPCM support groups. One woman explained,
It’s one of the most highly discussed items on the support group network; people struggling with the decision; people inquiring. There aren’t many on there, but people who have had post-PPCM pregnancies; some very successful, some not as much. I would say it is definitely, I think, the most talked about topic. Everybody is interested in it because obviously it affects people in their childbearing years when they have this diagnosis. I would say the majority of people are told not to have any more pregnancies. There’s very, very few people on that support group network that say, “My doctor supports me getting pregnant again”. There are, but a very, very few.
Making the decision about a subsequent pregnancy
Three women had decided before the PPCM diagnosis that the current pregnancy was to be their last. The heart failure diagnosis reinforced that decision. Seven women made the definitive decision to not get pregnant again after the diagnosis. All had originally wanted more children so this decision did not come easy. One woman said, Me and [husband’s name] did not set a time frame for when we were going to have children. I finished college, we both worked on our careers. I wanted to start my career and do everything that married couples do. It took seven years. We planned on having two children . . . I waited to get pregnant until we were ready. I did everything by the book. . . I feel guilty that I cannot give my mom any more grandchildren. I can’t give my husband any more children.
Three women were still undecided when interviewed. One said,
I have a really hard time with it to this day. I love kids. My husband and I are both pastors. We always envisioned having a large family. At the end of the day I have to think, this is what gets me through today, it’s just that, you know, if I delivered a baby and I wasn’t here to be with my family anymore, that’s not worth it. And that’s sort of the end-all decision when I get those moments when I really want another child.
Four women decided to have at least one more pregnancy. They asked questions, searched for more information, participated in PPCM support groups, and watched their EF and medications closely. They minimized the risks by finding obstetricians and cardiologists who offered close supervision in this high risk situation.
Experiencing a subsequent pregnancy
Four of the 16 women had a SSP with varying experiences. One woman described her SSP this way.
My blood pressure stayed good the whole pregnancy. My ejection fraction stayed 50-55% throughout the pregnancy as well. I am not on any medication. I feel great. I love being a mom. Being a mom is one of the best roles that I have ever had in my life. I feel that coming through [the SSP] without any relapse, I feel like I ran a marathon and I won. I feel that I am very lucky.
Another woman diagnosed with PPCM during her first pregnancy, made a good recovery, and decided, with her husband and cardiologist, to have a second child. Thirty-six weeks into her pregnancy she relapsed with an EF of 30%.
I was a little scared. I thought I would not relapse because I was seeing the doctor all the time. I never thought I would relapse when I was pregnant because the first time I was 4 months post-partum when I was diagnosed. I was feeling all sorts of emotions. I was angry. I was scared.
Discussion
This is the first qualitative study to explore women’s experiences about a SSP after a diagnosis of PPCM from the woman’s perspective. Each woman’s life story is unique but commonalities are evident. The main reason women considered a SSP was the strong desire for more children. Gauging the risk of relapse was the central core of the decision making process. Women chose to not have a SSP because of ongoing poor health, medical advice, age, number of children, and others’ opinions. Factors affecting their reasoning included the way they were told to not get pregnant again, their emotional reactions to this ultimatum, and their personality.
Most of the women who experienced PPCM wanted or had planned to have more children. Almost all the women were informed abruptly, while still critically ill, that they should never get pregnant again. This ‘double blow’ increased the trauma of the experience. Women with PPCM described their feelings of anger, grief, and sadness related to loss of self-determination of the size of her family. This emotional trauma impacted their quality of life [19].
Women with PPCM usually experienced the resistance or ambivalence of spouses, health care professionals, and others, when they expressed the desire to get pregnant again. Some women accepted their spouses’ and physicians’ stance and chose not to get pregnant again; others did not. These findings are consistent with those in other studies regarding the decision for an SSP after a traumatic medical diagnosis [14,20,21]. Many women with PPCM were dissatisfied with the counseling they received [19]. Similar to women wanting another child after a neonatal loss [22], several women with PPCM sought second opinions from different obstetricians and cardiologists. Reassurance from providers who listened attentively to patients’ concerns was perceived as crucial [3,21,22]. Time with a pregnancy consultant for a debriefing session along with individualized care before and during the SSP was greatly appreciated [21].
First-time mothers with PPCM appeared to struggle more with advice to stop having children than women who already had other children. Permanent contraception was part of the struggle. Dekker et al [14] found many of the women advised to not get pregnant again had not taken permanent measures to avoid future conception. Those using contraception indicated the decision for or against a SSP was based on the risk of relapse and possible death could have on their families. PPCM patients need to be informed of their contraceptive options because the risk of relapse increases with SSP. In addition, attention must be given to potential interactions between hormonal contraceptives and heart failure medications [23].
Nursing Implications
Our findings lead to implications for nurses and midwives caring for women with PPCM in emergent settings or during follow up appointments. The topic of future pregnancies need not be broached in the emergency room or intensive care unit but should be discussed at a more appropriate time and place [11,14,15,24]. The woman and her family need the opportunity to ask questions, express grief, and process options for a future pregnancy at a post diagnosis consultation [25].
An individualized care plan, developed through shared decision making [26], is vital to support women and couples through the pre-pregnancy period and during a SSP [24,25]. Principles of shared decision making to include in the plan are the presentation of information on various levels of risk, communication of risks and benefits using pictographs and decision aids, and the use of a decision coach [27]. The plan should also include pre-conception counseling as well as close surveillance during pregnancy and child birth.
Standardized guidelines are lacking for the management of pregnancy-related heart disease during a SSP [9]. Women with persistent LV dysfunction and a LVEF less than 30% should probably never get pregnant [28]. Women with PPCM need advice on contraceptives appropriate for someone with a heart condition [29]. Consideration must be given to the risk of thromboemboli, arrhythmias, and the use of anticoagulants [30]. In regions of the world where family planning or pregnancy restraints are not encouraged, women with both normalized and persistent cardiomyopathy should be informed of the risks to mother and baby and counseled to not get pregnant again if management of cardiomyopathies with pregnancy is inadequate [31]. Again, this decision should be shared by the woman with PPCM, nurses, midwives, physicians, and key family members involved in her life [25].
Study Limitations and Recommendations for Future Research
This study was limited by selection bias and recall bias. All the participants in this study were Caucasian and lived in the United States; therefore these findings may not be representative of women of other ethnicities and or living in other countries. Data saturation produced rich information with recurrent themes but time may have blurred some of the memories women were asked to recall about their experiences. Since only four women in this study described a SSP, further research is needed on women who have made this choice. Despite these limitations, this study from the women’s perspectives, provides us with a wealth of knowledge into the emotional journey women with PPCM go through to make a decision for or against a SSP. Recommendations for future research include post-traumatic stress among women with PPCM, as well as the impact of PPCM on spouses and families.
Conclusion
Prior research evidence indicates a SSP is risky for women whose ejection fraction has not fully recovered after a diagnosis of PPCM. Recent research and close monitoring by cardiologists and obstetricians shows some women are able to have more children without severe relapse into heart failure. Women with PPCM who wish to have more children face emotional upheaval during the decision making process. The health care team, along with the woman and her supportive family and friends, must work together to weigh the risks and make a decision about a future pregnancy in a way that is healthy for her and her family.
References
- Sliwa K, Hilfiker-Kleiner D, Mebazaa A, Petrie MC, Maggioni AP, Regitz- Zagrosek V, et al. EUR Observational Research Programme: A worldwide registry on Peripartum Cardiomyopathy (PPCM) in conjunction with the Heart Failure Association of the European Society of Cardiology Working Group on PPCM. European Journal of Heart Failure. 2014; 16: 583-591.
- Sliwa K, Hilfiker-Kleiner D, Petrie MC, Mebazaa A, Pieske B, Buchmann E, et al. Current state of knowledge on aetiology, diagnosis, management, and therapy of peripartum cardiomyopathy: A position statement from the Heart Failure Association of the European Society of Cardiology Working Group on peripartum cardiomyopathy. European Journal of Heart Failure. 2010; 12: 767-778.
- Kolte D, Khera S, Aronow WS, Palaniswamy C, Mujib M, Ahn C, et al. Temporal trends in incidence and outcomes of peripartum cardiomyopathy in the United States: a nationwide population-based study. Journal of the American Heart Association. 2014; 3: e001056.
- Gunderson EP, Croen LA, Chiang V, Yoshida CK, Walton D, Go AS. Epidemiology of peripartum cardiomyopathy: Incidence, predictors, and outcomes. Obstetrics & Gynecology. 2011; 118: 583-591.
- Sliwa K, Fett J, Elkayam U. Peripartum cardiomyopathy. Lancet. 2006; 368: 687-693.
- Perveen S, Ainuddin J, Jabbar S, Soomro K, Ali A. Peripartum cardiomyopathy: Frequency and predictors and indicators of clinical outcome. Journal of Pakistan Medical Association. 2016; 66: 1517-1521.
- Fett JD, Christie LG, Murphy JG. Brief communication: Outcomes of subsequent pregnancy after peripartum cardiomyopathy: A case series from Haiti. Annals of Internal Medicine. 2006; 145: 30-34.
- Elkayam U. Clinical characteristics of peripartum cardiomyopathy in the United States: Diagnosis, prognosis, and management. Journal of the American College of Cardiology. 2011; 58: 659-670.
- Elkayam U. Risk of subsequent pregnancy in women with a history of peripartum cardiomyopathy. Journal of the American College of Cardiology. 2014; 64: 1629-1636.
- Davis M, Duvernoy C. Peripartum cardiomyopathy: Current knowledge and future directions. Women’s Health. 2015; 11: 565-573.
- Ersbøll AS, Damm P, Gustafsson F, Vejlstrup NG, Johansen M. Peripartum cardiomyopathy: A systematic literature review. AOGS Acta Obstetricia et Gynecologica Scandinavica. 2016; 95: 1205-1219.
- Patel H, Berg M, Barasa A, Begley C, Schaufelberger M. Symptoms in women with peripartum cardiomyopathy. Midwifery. 2016; 32: 14-20.
- Fett JD, Shah TP, McNamara DM. Why do some recovered peripartum cardiomyopathy mothers experience heart failure with a subsequent pregnancy? Current Treatment Options in Cardiovascular Medicine. 2015; 17: 354.
- Dekker RL, Morton CH, Singleton P, Lyndon A. Women’s experiences being diagnosed with peripartum cardiomyopathy: A qualitative study. Journal of Midwifery & Women’s Health. 2016; 61: 467-473.
- Hess RF, Weinland JD. The life-changing impact of peripartum cardiomyopathy: An analysis of online postings. MCN: The American Journal of Maternal Child Nursing. 2012; 37: 241-246.
- Chee KH. Favourable outcome after peripartum cardiomyopathy: A tenyear study on peripartum cardiomyopathy in a university hospital. Singapore Medical Journal. 2013; 54: 28-31.
- Polit DF, Tatano Beck C. Nursing research generating and assessing evidence for nursing practice. 10th Edn. Philadelphia: Wolters Kluwer. 2016.
- Fusch PI, Ness LR. Are we there yet? Data saturation in qualitative research. The Qualitative Report. 2015; 20: 1408.
- Koutrolou-Sotiropoulou P, Lima FV, Stergiopoulos K. Quality of life in survivors of peripartum cardiomyopathy. American Journal of Cardiology. 2016; 118: 258-263.
- Lee L, Mckenzie-McHarg K, Horsch A. Women’s decision making and experience of subsequent pregnancy following stillbirth. Journal of Midwifery & Women’s Health. 2013; 58: 431-439.
- Meaney S, Everard CM, Gallagher S, O’Donoghue K. Parents’ concerns about future pregnancy after stillbirth: A qualitative study. Health Expectations. 2016.
- Mills TA, Ricklesford C, Cooke A, Heazell AEP, Whitworth M, Lavender T. Parents’ experiences and expectations of care in pregnancy after stillbirth or neonatal death: A metasynthesis. BJOG: An International Journal of Obstetrics & Gynaecology. 2014; 121: 943-950.
- Hilfiker-Kleiner D, Haghikia A, Nonhoff J, Bauersachs J. Peripartum cardiomyopathy: Current management and future perspectives. European Heart Journal. 2015; 36: 1090-1097.
- Cruz-Herranz A, Illán-Gala I, Martínez-Sánchez P, Fuentes B, Díez-Tejedor E. Recurrence of stroke amongst women of reproductive age: Impact of and on subsequent pregnancies. European Journal of Neurology. 2015; 22: 681- e42.
- Fowler K, Schafer D, Sica M, Pogasic D, Gardner K, Szczepanski S, et al. 3 Peripartum Cardiomyopathy (PPCM): Interdisciplinary coordination for a complex patient population. Heart & Lung - The Journal of Acute and Critical Care. 2017; 46: 212-213.
- Coulter A. Shared decision making. Why patients’ preferences matter. 2012.
- Lin GA, Fagerlin A. Shared decision making. Circulation: Cardiovascular Quality and Outcomes. 2014; 7: 328-334.
- Regitz-Zagrosek V, Lundqvist CB, Borghi C, Cifkova R, Ferreira R, Foidart JM, et al. ESC Guidelines on the management of cardiovascular diseases during pregnancy. European Heart Journal. 2011; 32: 3147-3197.
- Hinze A, Kutty S, Sayles H, Sandene EK, Meza J, Kugler JD. Reproductive and contraceptive counseling received by adult women with congenital heart disease: A risk-based analysis. Congenital Heart Disease. 2013; 8: 20-31.
- Roos-Hesselink JW, Cornette J, Sliwa K, Pieper PG, Veldtman GR, Johnson MR. Contraception and cardiovascular disease. European Heart Journal. 2015; 36: 1728-1734.
- Mandal D, Mandal S, Mukherjee D, Biswas SC, Maiti TK, Chattopadhaya N, et al. Pregnancy and subsequent pregnancy outcomes in peripartum cardiomyopathy. Journal of Obstetrics and Gynaecology Research. 2011; 37: 222-227.