
Review Article
Ann Nutr Disord & Ther. 2015;2(2): 1024.
Nutritional Deficiencies in Obesity and After Weight Reduction
Owais Bhatti¹, Klaus Bielefeldt² and Salman Nusrat³*
¹Department of Internal Medicine, University of Oklahoma Health Sciences Center, USA
²Department of Gastroenterology, University of Pittsburg,USA
³Department of Gastroenterology, University of Oklahoma Health Sciences Center, USA
*Corresponding author: Salman Nusrat, Department of Internal Medicine, Section of Digestive Disease,University of Oklahoma Health Sciences Center, 920 Stanton Young Blvd, Oklahoma City, OK 73014, USA
Received: April 06, 2015; Accepted: June 24, 2015; Published: July 01, 2015
Abstract
The obesity epidemic in the USA requires physicians to have a better understanding of these patients’ nutritional needs. Obesity is a state of malnutrition and it is very common to find micronutrient deficiencies in these patients. Poor dietary choices, poor access to healthy foods and altered micronutrient metabolism likely results in micronutrient deficiency. Bariatric surgery is indicated for patients with BMI > 40 or > 35 with 2 or more obesity associated co-morbidities. Surgery has shown to result in sustained weight loss and decreased risk of future cardiovascular morbidity. Other benefits of bariatric surgery includes decreased incidence of diabetes, hypertension and all cause mortality. The increasingly popular bariatric procedures however can also result in malnutrition due to altered digestive tract anatomy, post surgical hypo caloric diets and excessive nausea/vomiting. We reviewed common micronutrient deficiencies (thiamine, B12, iron and vitamin D) and supplemental regimens for treating these deficiencies in obese and gastric bypass patients. Deficiencies of these micronutrients can result in Wernicke’s encephalopathy, peripheral neuropathy, beriberi, fatigue and osteoporosis. Close surveillance and aggressive supplementation regimens for preventing or treating micronutrient deficiencies are required.
Keywords: Obesity; Bariatric surgery; Gastric bypass; Nutrition and deficiencies
Abbreviations
BMI: Body Mass Index; SOS: Swedish Obese Subjects study; VBG: Vertical Banded Gastroplasty; RYGB: Roux en Y Gastric Bypass; GI: Gastrointestinal; BPD: Biliopancreatic Diversion; CRP: C Reactive Protein; HB: Hemoglobin; MCV: Mean Corpuscle Volume; PPARδ: Peroxisome Proliferator-Activated Receptor Delta; PTH: Parathyroid Hormone; WE: Wernicke’s encephalopathy; 25 OH D: 25-Hydroxyvitamin D; LAGB: Laparoscopic Adjustable Gastric Banding; RDI: Recommended Dietary Intake
Introduction
Obesity is defined as Body Mass Index (BMI) greater than 30 and is further classified as grade 1 (BMI 30 to 34.9), grade 2 (BMI 35 to 39.9) and grade 3 (BMI ≥40) [1]. It is one of the leading medical issues facing developed countries in modern medicine. The age– adjusted prevalence of obesity in the United States is 35.5% among adult men and 35.8% among adult women [2]. Obesity increases the risk for cardiovascular disease, diabetes, hypertension and dyslipidemia. In1987, Manson et al. [3] proved that being overweight (BMI >25) was associated with increased risk of death. In the same year, Donahue et al. [4] found an association between coronary heart disease and central obesity. In addition to the physical toll, mental health disorders are also more prevalent in obesity. A study (n=662) showed that obesity was more common among subjects suffering from depression when compared to subjects with normal BMI [5]. However it is worth noting that most medications used by psychiatrists are also associated with weight gain.
In terms of US dollars the cost of obesity is high and will continue to increase. In 2008 the US spent an estimated 147 billion dollars on the medical costs of obesity [6].
Bariatric surgery is shown to be effective in reducing weight and modifying the risk factors associated with cardiovascular morbidity. Based on current NIH guidelines, bariatric surgery should be considered for grade 3 obesity or grade 2 obesity with two or more comorbidities that are related to obesity (e.g. diabetes and hypertension) [7].
Compared with usual care, bariatric surgery is associated with decreased number of cardiovascular deaths and lower incidence of cardiovascular events in obese adults [8]. Surgery also decreased the risk of developing diabetes when compared to usual care in obese persons [9].
The most dramatic effect of bariatric surgery is weight loss. The Swedish Obese Subjects study (SOS) [10] showed that surgery resulted in 20-35 % loss of baseline weight (depending on type of procedure) compared to 1-2 % in control groups. It also showed a 40% decrease in adjusted all cause long term mortality compared to controls. The SOS trial also showed that bariatric surgery subjects had a higher rate of maintained weight-loss compared to control sat 2 years and 10 years of follow up. In addition, it decreased the incidence of diabetes especially in patients with impaired glucose tolerance [9,10]. Bariatric surgery has shown to either normalize blood pressure or reduce the need for antihypertensive therapy [11,12]. The effect seems to correlate with the degree of weight loss [12]. A meta-analysis of 29,000patients undergoing bariatric surgery, showed that bariatric surgery patients had 50% reduction in mortality, compared to non-surgical controls. There was also a 50% reduction in the risk of cardiovascular adverse events, such as lower rates of myocardial infarction (OR 0.46, 95% CI 0.30-0.69) and stroke (OR 0.49, 95% CI 0.32-0.75) [13].
Types of Procedures
Bariatric procedures can be divided into two broad categories: restrictive and malabsorptive. Restrictive procedures includes the laparoscopically placed adjustable gastric band, (Figure 1) and the Vertical Banded Gastroplasty (VBG) that forms a small gastric reservoir of about 15ml [14]. Sleeve gastrectomy is a restrictive procedure, which leaves a proximal gastric pouch of about 100 ml, by resecting much of the greater curvature and the antrum of the stomach [14].
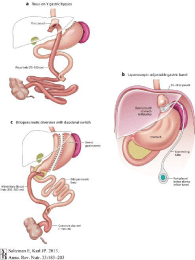
Figure 1: (a) Roux-en-Y gastric bypass, (b) Laparoscopic adjustable gastric
band and (c) Biliopancreatic diversion with duodenal switch.
The Roux-en-Y Gastric Bypass (RYGB) is a combined restrictive and malabsorptive procedure, in which the stomach is divided into a small pouch of about 30 ml, which remains in continuity with the proximal and distal GI tract (Figure 1). This procedure leaves the majority of the stomach blindly occluded and bypassed by ingested food particles. The gastric pouch connects to a Roux limb of jejunum, with the distal anastomosis with the small bowel being located, about a 100 cm distal from the ligament of Treitz [14]. This results in food particles bypassing some of the small intestine and decreasing the surface area for digestion and absorption. Also biliary and pancreatic secretions mix with chyme at the distal anastomosis and hence limit exposure to digestive enzymes contained in these secretions. The Biliopancreatic Diversion (BPD) with duodenal switch is another combined restrictive and malabsorptive procedure that essentially created two separate tracts. One tract carries nutrients and the other tract carries digestive enzymes. These tracts are only allowed to meet (and hence digestion allowed to take place) about 20 cm from the ileocecal valve [14] (Figure 1).
The RYGB is considered the most successful procedure as it can cause significant weight loss and has acceptable complication rates [15,16]. BPD results in the greatest amount of weight loss but its complication rates are higher [16]. The VBG is out of favor as weight loss is generally limited and not maintained. Evolving bariatric techniques include Laparoscopic Gastric Plication in which the stomach is incised along its longitudinal axis and resutured to create a plicated gastric fold [17]. The Intra Gastric Balloon is an endoluminal technique, in which a balloon is introduced and inflated using an endoscope [18]. As with all emerging procedures it will take time to establish the safety and the efficacy of these techniques.
Nutritional Deficiency and Obesity
The obesity epidemic in the United States may be viewed as a form of malnutrition with an obvious excess of calories, often supplied in the form of fat and sweetened beverages, but with a limit use of healthy foods. Prior studies clearly demonstrated a link between poverty rates, high fast food restaurant density and difficult access to supermarkets or other sources for fruits and vegetables [19]. Another hypothesis is that obesity is associated with an inflammatory state [20] that results in lower levels of specific nutrients due to sequestration, decrease in blood levels of serum markers or increased utilization [21]. A study in Mexico found that the prevalence of iron deficiency was significantly higher in obese women and children when compared to normal weight subjects. This was seen despite similar dietary intakes in both groups. Also CRP levels were 4 times higher in obese patients and a significant negative predictor of iron status [21].
Such findings may explain the apparent paradox that obese people may present with micronutrient deficiencies. An assessment of 232 morbidly obese subjects (BMI>35) showed deficiencies in ferritin (6.9%), hemoglobin (6.9%), vitamin B12 (18.1%) and folate (3.4%) [22]. Prevalence of anemia (in women only) significantly increased with BMI [22]. In another study by Schweiger et al. of 114 obese patients showed the prevalence of pre-operative nutritional deficiencies were: 35% for iron, 24% for folic acid and 6% for vitamin B12. In addition to this Hb and MCV (Mean Corpuscular Volume) levels were low in 19% [23].
There is some evidence of abnormal thiamine metabolism and asymptomatic thiamine deficiency in obesity [24,25]. Patrini et al. compared 10 obese women to 10 normal weight women and found that there was a significant decrease in plasma thiamine, thiamine monophosphate and total thiamine in obese subjects. It was also reported that there was an increase in plasma thiamine to thiamine monophosphate ratio and a decrease in plasma thiamine monophosphate to erythrocyte thiamine pyrophosphate ratio in obese subjects [24]. These altered mechanisms were suggestive of increased intracellular storage of thiamine as a response to thiamine deficiency in the body.
Vitamin B12 is a common deficiency in obese patients. Preoperative nutritional assessments have found Vitamin B12 deficiencies that vary between 3-11% [26-28].
Vitamin D deficiency is common in temperate zones and has been seen in obesity, with a reported prevalence ranging up to 60% [27,29]. There is evidence that suggests that adipogenesis and osteoblastogenesis are inversely related [30]. Activation of the Peroxisome Proliferator–Activated Receptor-δ (PPARδ) initiates adipogenesis and inhibits osteoblastogenesis [31]. Inactivity via skeletal unloading causes increased adipocyte differentiation at the expense of osteoblastogenesis. Serum levels of 25OHD (25-Hydroxyvitamin D are lower (due to storage in fat) and PTH (Parathyroid Hormone) levels are higher in obesity [32,33]. Obesity is also associated with higher levels of serum inflammatory markers that can potentially increase bone turnover [34]. It is not clear how this translates to risk of fracture as higher BMI can lead to increased or decreased risk of fracture depending on the type of bone [30].
There is some evidence of the association of iron deficiency with obesity. It has been suggested that the inflammatory state of obesity increases the production of proteins like hepcidin and lipocalin 2 that lead to iron sequestration in the reticuloendothelial system [35]. Since iron is highly reactive and can cause oxidative stress it has been postulated that increased iron deposition in adipose cells results in obesity aggravation via adipose cell endocrine dysfunction [35]. A study evaluating iron absorption using radiolabelled isotopes showed a significant decrease in iron absorption in obese women compared to overweight or normal weight subjects [36]. Pre-operative assessments have found obese subjects to be iron deficient up to 18 % [37].
Nutritional Deficiencies after Gastric Bypass
Nutritional deficiencies after bariatric surgery are multifactorial. Patients that are assessed for bariatric procedures are strongly encouraged to lose as much weight as possible prior to their procedure. Hence patients go on low calorie diets to lose weight and therefore are more susceptible to deficiencies of iron, B12 and calcium [38].
Bariatric surgery causesdrastic anatomical changes of the digestive tract that alters the normal process of digestion. The capacity of the stomach to hold food and secrete juices that facilitate digestion is reduced. For example after RYGB, the capacity of the remnant gastric pouch is only 20 ml [39]. Similarly, the surface area for digestion and absorption of food in the small intestine is markedly reduced, depending upon the amount of intestine resected. It is reasonable to presume that such alterations in the gut anatomy will adversely affect nutrient metabolism. This makes bariatric surgery patients more vulnerable to micronutrient deficiencies and protein energy malnutrition [40]. After surgery the patient is on a liquidonly diet for a month. This diet is gradually advanced to pureed diet over the next few months. Patients cannot tolerate large quantities of food after surgery and their daily caloric intake during the initial postoperative period typically ranges between 500-900 kcal/day [39,41]. It is difficult to maintain adequate micronutrient intake on such low caloric diets. Furthermore, postoperative complications like vomiting, obstruction, fistula formation, ulcers and dumping can also prevent adequate nutrition [42-44]. Small bowel obstruction is a late postoperative complication that can occur following RYGB [45]. The risk is higher with laparoscopic RYGB and the obstruction is usually due to internal hernias [45]. Fistula formation is a common complication of sleeve gastrectomy. A meta-analysis showed that fistula rates in sleeve gastrectomies were up to 2.2%(46). Other studies showed fistula rates ranging from 0 to 20% [46].
Considering the potential for nutritional deficiencies, patients are routinely asked to take multivitamins, supplemental calcium and iron. Supplementation is especially important for patients undergoing malabsorptive bariatric procedures. However studies have shown that patient compliance with these supplements is low and therefore it is difficult to maintain adequate nutrition. A study showed that over a 10-year period only 33% of patients were compliant with nutritional supplements [47]. High rates of non-compliance with supplementation make it even more difficult to treat micronutrient deficiencies.
Thiamine
Thiamine deficiencies after gastric bypass can result in weakness, polyneuropathies, beriberi, Wernicke’s Encephalopathy (WE), nystagmus and hearing loss [48-51]. The most serious manifestation of thiamine deficiency is Wernicke’s encephalopathy and the main risk factor identified was persistent vomiting and intravenous administration of glucose without thiamine [52-55]. There have been 16 reported cases of WE after restrictive weight loss procedures as reported by Milone et al. [53]. Wernicke’s encephalopathy leaves residual neurological defects in the majority of the affected [52,53]. The prevalence of thiamine deficiency in a study following 318 subjects for 2 years was 18% [56]. In a review of subjects who underwent bariatric surgery and developed Wernicke’s encephalopathy, 95%of the affected patients underwent bypass [52]. There are no randomized trials that estimate adequate thiamine replacement in WE. Dosing is empirical and there is wide variation in clinical practice. One method is to give 500 mg parenterally, three times per day for 2-3 days and if an effective response is observed, then 250 mg daily is given parenterally for 3-5 days [57].
Vitamin B12
The reported prevalence of B12 deficiency widely varies. Studies report a prevalence that ranges from 11% to 70% after the bariatric surgery [58-61]. It is worth mentioning that B12 deficiency is prevalent prior to surgery and can be as high as 18% [14]. B12 is mostly bound to protein in our diet. Gastric proteases are responsible for the release of bound B12. Parietal cells of the gastric mucosa secrete intrinsic factor that binds B12 and then transports it to be absorbed in the ileum. It stands to reason that bypass surgery would alter this process with resection of acid, proteases and intrinsic factor secreting cells. The prevalence of B12 deficiency increases after surgery for all patients, but it is found to be greatest with RYGB procedures and least with restrictive procedures [62]. Supplementation is recommended, as even with supplementation, vitamin B12 levels in a study were found to be in the lower thirds of the reference range [63]. Supplementation can be oral, intranasal, sublingual or intra muscular. The best evidence of efficacy is for the intramuscular route [64]. Many physicians choose parenteral administration to avoid clinical manifestations of deficiency, such as neuropathy or the development of anemia [65]. Intramuscular vitamin B12 can be given as 1000 mcg/week for 8 weeks and then 1000 mcg once a month for lifelong maintenance [66].
Vitamin D
Vitamin D deficiency is quite common in bariatric patients being assessed for surgery. In a review of 14 studies only 1 study reported a mean preoperative serum 25(OH) D concentration that was greater than 32 ng/mL [67]. Post operatively it is very difficult to assess the impact of bariatric surgery on vitamin D metabolism. In most studies vitamin D levels increase with aggressive supplemental regimens. However despite improvements in serum levels the prevalence of vitamin D deficiency remains high. In a study of a group of patients’ status post LAGB (Laparoscopic Adjustable Gastric Banding), vitamin D deficiency decreased from 58% to 33% but this was not significant [68].
In another study, 266 RYGB patients baseline serum 25(OH) D levels increased from 25 ng/ml to 34 ng/ml after a year [69]. Gastric bypass leads to bone loss, high PTH and 25(OH) D levels. This can be seen despite supplementation with calcium [70-72]. Vitamin D deficiency increases risk of hypocalcaemia, bone loss with resulting fractures and even osteomalacia.
Acutely hypocalcaemia can be associated with cramps and changes in sensory function, which have been reported after bariatric procedures [73,74]. Guidelines recommend supplementing post operatively with 3000 IU of either vitamin D2 or D3 per day. Dosage should be increased until a serum 25(OH) D level >30 ng/mL is reached. For more severe cases vitamin D2 or D3 doses can be as high as 50000-150,000 IU a week [75].
Iron
Iron deficiency after gastric bypass is common. A retrospective analysis of 959 subjects status post RYGB found that 51% were deficient in iron. Almost half of the iron deficient subjects (40%) were severely deficient [76]. Meat intolerance is common post gastric bypass and results in the absence of an important source of iron in the diet [77]. The overall low parietal cell mass of the pouch results in hypochlorydia and is thought to be one of the mechanisms that lead to decreased absorption of iron in the gut. Iron is absorbed in the duodenum and thus its removal compromises iron absorption. It has been shown using radiolabelled isotopes that iron absorption worsens after gastric bypass. Iron absorption was measured before and after gastric bypass and was found to be decreased in the latter [78]. Iron deficiency post operatively is corrected via parenteral administration. Oral administration can cause gastrointestinal side effects and their effectiveness is disputed [79]. Pre-operatively oral iron supplementation is recommended for patients who are not iron deficient. Iron supplementation for males is 65 mg of iron/ day and females require supplementation with 100 mg of iron/ day [80,81].
Conclusion
Obesity is a common disease in the USA. The incidence and prevalence of obesity is rapidly increasing in the USA. Obesity increases the risk of cardiovascular diseases, diabetes and dyslipidemia. Obesity also leads to poor self-esteem and lack of self-confidence as obese individuals consider or are considered as unattractive. Obesity and its associated health risks have a huge financial burden with the estimated cost around 147 billion dollars in 2008. Obesity is a paradoxical state of malnutrition that consists of excessive caloric intake and micronutrient deficiencies. This state can be partially explained by poor dietary choices and poor access to food rich in nutrients. It is also hypothesized that obesity is a state of inflammation and abnormal micronutrient metabolism that results in deficiencies of iron, b12 and vitamin D. The fact that obese people can have micronutrient deficiencies needs to be recognized. This will allow for increased screening, diagnosis and treatment of micronutrient deficiencies in obese people.
Bariatric surgery is indicated for obese individuals with BMI > 40 or BMI > 35 and two or more co-morbidities that are obesity related. Bariatric surgery has shown to help obese patients lose up to 20-35 % of baseline weight and decrease all cause mortality, incidence of diabetes and adverse cardiovascular events. Post bariatric surgery patients have also been found to have micronutrient deficiencies including iron, b12 and vitamin D. The cause of micronutrient deficiencies in patients who have undergone bariatric surgery is multifactorial. Micronutrient deficiencies after bariatric surgery is a result of pre existing micronutrient deficiencies severely decreased caloric intakes, surgical complications and perhaps altered post surgical digestive anatomy. Micronutrient metabolism in obesity is complex and not completely elucidated. As our understanding of the complex physiology of micronutrient digestion in obesity develops, so will our ability to treat micronutrient deficiencies. Further research needs to be done to address questions like Recommended Dietary Intake (RDI) of micronutrients for obese subject and RDI of micronutrients for post bariatric surgery patients. Also supplementation for micronutrient deficiencies for obese patients and bariatric surgery patients is not evidence based. Currently supplementation for bariatric surgery subjects is higher than RDI but there is little evidence of benefit. One could argue that even higher dose supplementation might still be inadequate.
Nutrition in bariatric surgery is challenging. The importance of identifying and treating micronutrient deficiencies prior to surgery is reiterated. After bariatric surgery it is important to maintain close follow up for nutritional status as deficiencies can result in devastating consequences including Wernicke’s encephalopathy, neuropathies and heart failure.
References
- Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of obesity in the United States, 2009-2010. NCHS Data Brief. 2012; 1-8.
- Flegal KM, Carroll MD, Kit BK, Ogden CL. Prevalence of obesity and trends in the distribution of body mass index among US adults, 1999-2010. JAMA. 2012; 307: 491-497.
- Manson JE, Stampfer MJ, Hennekens CH, Willett WC. Body weight and longevity. A reassessment. JAMA. 1987; 257: 353-358.
- Donahue RP, Abbott RD, Bloom E, Reed DM, Yano K. Central obesity and coronary heart disease in men. Lancet. 1987; 1: 821-824.
- Toups MS, Myers AK, Wisniewski SR, Kurian B, Morris DW, Rush AJ, et al. Relationship between obesity and depression: characteristics and treatment outcomes with antidepressant medication. Psychosomatic medicine. 2013; 75: 863-72.
- Finkelstein EA, Trogdon JG, Cohen JW, Dietz W. Annual medical spending attributable to obesity: payer-and service-specific estimates. Health Aff (Millwood). 2009; 28: w822-w831.
- Network W-cI. Bariatric Surgery for Severe Obesity. 2009.
- Sjöström L, Peltonen M, Jacobson P, Sjöström CD, Karason K, Wedel H, et al. Bariatric surgery and long-term cardiovascular events. JAMA. 2012; 307: 56-65.
- Carlsson LM, Peltonen M, Ahlin S, Anveden Å, Bouchard C, Carlsson B, et al. Bariatric surgery and prevention of type 2 diabetes in Swedish obese subjects. N Engl J Med. 2012; 367: 695-704.
- Sjostrom L. Review of the key results from the Swedish Obese Subjects (SOS) trial - a prospective controlled intervention study of bariatric surgery. Journal of internal medicine. 2013; 273: 219-234.
- Courcoulas AP, Christian NJ, Belle SH, Berk PD, Flum DR, Garcia L, et al. Weight change and health outcomes at 3 years after bariatric surgery among individuals with severe obesity. JAMA: the journal of the American Medical Association. 2013; 310: 2416-2425.
- Hinojosa MW, Varela JE, Smith BR, Che F, Nguyen NT. Resolution of systemic hypertension after laparoscopic gastric bypass. Journal of gastrointestinal surgery. 2009; 13: 793-797.
- Kwok CS, Pradhan A, Khan MA, Anderson SG, Keavney BD, Myint PK, et al. Bariatric surgery and its impact on cardiovascular disease and mortality: a systematic review and meta-analysis. Int J Cardiol. 2014; 173: 20-28.
- Saltzman E, Karl JP. Nutrient deficiencies after gastric bypass surgery. Annu Rev Nutr. 2013; 33: 183-203.
- Herron DM, Roohipour R. Bariatric surgical anatomy and mechanisms of action. Gastrointest Endosc Clin N Am. 2011; 21: 213-228.
- Switzer NJ, Mangat HS, Karmali S. Current trends in obesity: body composition assessment, weight regulation, and emerging techniques in managing severe obesity. Journal of interventional gastroenterology. 2013; 3: 34-36.
- Masoomi H, Nguyen NT, Stamos MJ, Smith BR. Overview of outcomes of laparoscopic and open Roux-en-Y gastric bypass in the United States. Surgical technology international. 2012; 22: 72-76.
- Genco A, Bruni T, Doldi SB, Forestieri P, Marino M, Busetto L, et al. BioEnterics Intragastric Balloon: The Italian Experience with 2,515 Patients. Obes Surg. 2005; 15: 1161-1164.
- Larson NI, Story MT, Nelson MC. Neighborhood environments: disparities in access to healthy foods in the U.S. Am J Prev Med. 2009; 36: 74-81.
- Visser M, Bouter LM, McQuillan GM, Wener MH, Harris TB. Elevated C-reactive protein levels in overweight and obese adults. JAMA. 1999; 282: 2131-2135.
- Cepeda-Lopez AC, Osendarp SJ, Melse-Boonstra A, Aeberli I, Gonzalez-Salazar F, Feskens E, et al. Sharply higher rates of iron deficiency in obese Mexican women and children are predicted by obesity-related inflammation rather than by differences in dietary iron intake. The American journal of clinical nutrition. 2011; 93: 975-983.
- Ernst B, Thurnheer M, Schmid SM, Schultes B. Evidence for the necessity to systematically assess micronutrient status prior to bariatric surgery. Obes Surg. 2009; 19: 66-73.
- Schweiger C, Weiss R, Berry E, Keidar A. Nutritional deficiencies in bariatric surgery candidates. Obes Surg. 2010; 20: 193-197.
- Patrini C, Griziotti A, Ricciardi L. Obese individuals as thiamin storers. Int J Obes Relat Metab Disord. 2004; 28: 920-924.
- Carrodeguas L, Kaidar-Person O, Szomstein S, Antozzi P, Rosenthal R. Preoperative thiamine deficiency in obese population undergoing laparoscopic bariatric surgery. Surgery for obesity and related diseases. 2005; 1: 517-522.
- Nicoletti CF, Lima TP, Donadelli SP, Salgado W, Marchini JS, Nonino CB. New look at nutritional care for obese patient candidates for bariatric surgery. Surgery for obesity and related diseases. 2013; 9: 520-525.
- de Luis DA, Pacheco D, Izaola O, Terroba MC, Cuellar L, Cabezas G. Micronutrient status in morbidly obese women before bariatric surgery. Surgery for obesity and related diseases. 2013; 9: 323-327.
- Damms-Machado A, Friedrich A, Kramer KM, Stingel K, Meile T, Kuper MA, et al. Pre- and postoperative nutritional deficiencies in obese patients undergoing laparoscopic sleeve gastrectomy. Obesity surgery. 2012; 22: 881-889.
- Moore CE, Sherman V. Vitamin D Supplementation Efficacy: Sleeve Gastrectomy Versus Gastric Bypass Surgery. Obesity surgery. 2014; 24: 2055-2060.
- Shapses SA, Sukumar D. Bone metabolism in obesity and weight loss. Annu Rev Nutr. 2012; 32: 287-309.
- Rosen CJ, Bouxsein ML. Mechanisms of disease: is osteoporosis the obesity of bone? Nat Clin Pract Rheumatol. 2006; 2: 35-43.
- Wortsman J, Matsuoka LY, Chen TC, Lu Z, Holick MF. Decreased bioavailability of vitamin D in obesity. Am J Clin Nutr. 2000; 72: 690-693.
- Bolland MJ, Grey AB, Ames RW, Horne AM, Gamble GD, Reid IR. Fat mass is an important predictor of parathyroid hormone levels in postmenopausal women. Bone. 2006; 38: 317-321.
- Guri AJ, Bassaganya-Riera J. Systemic effects of white adipose tissue dysregulation and obesity-related inflammation. Obesity (Silver Spring). 2011; 19: 689-700.
- Nikonorov AA, Skalnaya MG, Tinkov AA, Skalny AV. Mutual interaction between iron homeostasis and obesity pathogenesis. Journal of trace elements in medicine and biology: organ of the Society for Minerals and Trace Elements (GMS). 2015; 30: 207-214.
- Mujica-Coopman MF, Brito A, López de Romaña D, Pizarro F, Olivares M. Body mass index, iron absorption and iron status in childbearing age women. J Trace Elem Med Biol. 2015; 30: 215-219.
- Lefebvre P, Letois F, Sultan A, Nocca D, Mura T, Galtier F. Nutrient deficiencies in patients with obesity considering bariatric surgery: A cross-sectional study. Surgery for obesity and related diseases. 2014; 10: 540-546.
- Gardner CD, Kim S, Bersamin A, Dopler-Nelson M, Otten J, Oelrich B, et al. Micronutrient quality of weight-loss diets that focus on macronutrients: results from the A TO Z study. The American journal of clinical nutrition. 2010; 92: 304-312.
- Bavaresco M, Paganini S, Lima TP, Salgado W, Ceneviva R, Dos Santos JE, Nonino-Borges CB. Nutritional course of patients submitted to bariatric surgery. Obes Surg. 2010; 20: 716-721.
- Santarpia L, Grandone I, Alfonsi L, Sodo M, Contaldo F, Pasanisi F. Long-term medical complications after malabsorptive procedures: Effects of a late clinical nutritional intervention. Nutrition. 2014; 30: 1301-1305.
- Moize V, Geliebter A, Gluck ME, Yahav E, Lorence M, Colarusso T, et al. Obese patients have inadequate protein intake related to protein intolerance up to 1 year following Roux-en-Y gastric bypass. Obes Surg. 2003; 13: 23-28.
- Moon RC, Teixeira AF, Goldbach M, Jawad MA. Management and treatment outcomes of marginal ulcers after Roux-en-Y gastric bypass at a single high volume bariatric center. Surgery for obesity and related diseases. 2014; 10: 229-234.
- Benevides ML, Oliveira SS, de Aguilar-Nascimento JE. The combination of haloperidol, dexamethasone, and ondansetron for prevention of postoperative nausea and vomiting in laparoscopic sleeve gastrectomy: a randomized double-blind trial. Obesity surgery. 2013; 23: 1389-1396.
- Laurenius A, Olbers T, Naslund I, Karlsson J. Dumping syndrome following gastric bypass: validation of the dumping symptom rating scale. Obesity surgery. 2013; 23: 740-755.
- Acquafresca PA, Palermo M, Rogula T, Duza GE, Serra E. Early surgical complications after gastric by-pass: a literature review. Arq Bras Cir Dig. 2015; 28: 74-80.
- Montravers P, Augustin P, Zappella N, Dufour G, Arapis K, Chosidow D, et al. Diagnosis and management of the postoperative surgical and medical complications of bariatric surgery. Anaesth Crit Care Pain Med. 2015; 34: 45-52.
- Brolin RE, Gorman JH, Gorman RC, Petschenik AJ, Bradley LJ, Kenler HA, et al. Are vitamin B12 and folate deficiency clinically important after roux-en-Y gastric bypass? Journal of gastrointestinal surgery. 1998; 2: 436-42.
- Landais A, Saint-Georges G. [Wernicke's encephalopathy following sleeve gastrectomy for morbid obesity.]. La Revue de medecine interne / fondee par la Societe nationale francaise de medecine interne. 2014; 35: 760-763.
- Moize V, Ibarzabal A, Sanchez Dalmau B, Flores L, Andreu A, Lacy A, et al. Nystagmus: an uncommon neurological manifestation of thiamine deficiency as a serious complication of sleeve gastrectomy. Nutrition in clinical practice. 2012; 27: 788-792.
- Jethava A, Dasanu CA. Acute Wernicke encephalopathy and sensorineural hearing loss complicating bariatric surgery. Conn Med. 2012; 76: 603-605.
- Goselink RJ, Harlaar JJ, Vermeij FH, Biter UL, Mannaerts GH, den Heijer T. [Beriberi after bariatric surgery]. Nederlands tijdschrift voor geneeskunde. 2012; 155: A4500.
- Aasheim ET. Wernicke encephalopathy after bariatric surgery: a systematic review. Ann Surg. 2008; 248: 714-720.
- Milone M, Di Minno MN, Lupoli R, Maietta P, Bianco P, Pisapia A, et al. Wernicke encephalopathy in subjects undergoing restrictive weight loss surgery: a systematic review of literature data. European eating disorders review. 2014; 22: 223-229.
- Becker DA, Ingala EE, Martinez-Lage M, Price RS, Galetta SL. Dry Beriberi and Wernicke's encephalopathy following gastric lap band surgery. Journal of clinical neuroscience. 2012; 19: 1050-1052.
- Bozbora A, Coskun H, Ozarmagan S, Erbil Y, Ozbey N, Orham Y. A rare complication of adjustable gastric banding: Wernicke's encephalopathy. Obes Surg. 2000; 10: 274-275.
- Clements RH, Katasani VG, Palepu R, Leeth RR, Leath TD, Roy BP, et al. Incidence of vitamin deficiency after laparoscopic Roux-en-Y gastric bypass in a university hospital setting. The American surgeon. 2006; 72: 1196-1202.
- Sechi G, Serra A. Wernicke's encephalopathy: new clinical settings and recent advances in diagnosis and management. Lancet Neurol. 2007; 6: 442-455.
- Toh SY, Zarshenas N, Jorgensen J. Prevalence of nutrient deficiencies in bariatric patients. Nutrition. 2009; 25: 1150-1156.
- Vargas-Ruiz AG, Hernández-Rivera G, Herrera MF. Prevalence of iron, folate, and vitamin B12 deficiency anemia after laparoscopic Roux-en-Y gastric bypass. Obes Surg. 2008; 18: 288-293.
- Amaral JF, Thompson WR, Caldwell MD, Martin HF, Randall HT. Prospective hematologic evaluation of gastric exclusion surgery for morbid obesity. Ann Surg. 1985; 201: 186-193.
- Halverson JD, Zuckerman GR, Koehler RE, Gentry K, Michael HE, DeSchryver-Kecskemeti K. Gastric bypass for morbid obesity: a medical--surgical assessment. Ann Surg. 1981; 194: 152-160.
- Gudzune KA, Huizinga MM, Chang HY, Asamoah V, Gadgil M, Clark JM. Screening and diagnosis of micronutrient deficiencies before and after bariatric surgery. Obes Surg. 2013; 23: 1581-1589.
- Pech N, Meyer F, Lippert H, Manger T, Stroh C. Complications, reoperations, and nutrient deficiencies two years after sleeve gastrectomy. Journal of obesity. 2012; 2012: 828737.
- Majumder S, Soriano J, Louie Cruz A, Dasanu CA. Vitamin B12 deficiency in patients undergoing bariatric surgery: preventive strategies and key recommendations. Surgery for obesity and related diseases. 2013; 9: 1013-1019.
- Levinson R, Silverman JB, Catella JG, Rybak I, Jolin H, Isom K. Pharmacotherapy prevention and management of nutritional deficiencies post Roux-en-Y gastric bypass. Obes Surg. 2013; 23: 992-1000.
- Allied Health Sciences Section Ad Hoc Nutrition C, Aills L, Blankenship J, Buffington C, Furtado M, Parrott J. ASMBS Allied Health Nutritional Guidelines for the Surgical Weight Loss Patient. Surgery for obesity and related diseases. 2008; 4: S73-S108.
- Compher CW, Badellino KO, Boullata JI. Vitamin D and the bariatric surgical patient: a review. Obes Surg. 2008; 18: 220-224.
- DiGiorgi M, Daud A, Inabnet WB, Schrope B, Urban-Skuro M, Restuccia N, et al. Markers of bone and calcium metabolism following gastric bypass and laparoscopic adjustable gastric banding. Obesity surgery. 2008; 18: 1144-1148.
- Johnson JM, Maher JW, DeMaria EJ, Downs RW, Wolfe LG, Kellum JM. The long-term effects of gastric bypass on vitamin D metabolism. Ann Surg. 2006; 243: 701-704.
- Goode LR, Brolin RE, Chowdhury HA, Shapses SA. Bone and gastric bypass surgery: effects of dietary calcium and vitamin D. Obes Res. 2004; 12: 40-47.
- Vilarrasa N, San José P, García I, Gómez-Vaquero C, Miras PM, de Gordejuela AG, et al. Evaluation of bone mineral density loss in morbidly obese women after gastric bypass: 3-year follow-up. Obes Surg. 2011; 21: 465-472.
- Sinha N, Shieh A, Stein EM, Strain G, Schulman A, Pomp A, et al. Increased PTH and 1.25(OH)(2)D levels associated with increased markers of bone turnover following bariatric surgery. Obesity (Silver Spring). 2011; 19: 2388-2393.
- Panda S, Sharma K. Osteomalacia induced peripheral neuropathy after obesity reduction surgery. Ann Indian Acad Neurol. 2013; 16: 690-692.
- Atreja A, Abacan C, Licata A. A 51-year-old woman with debilitating cramps 12 years after bariatric surgery. Cleveland Clinic journal of medicine. 2003; 70: 423-426.
- Mechanick JI, Youdim A, Jones DB, Garvey WT, Hurley DL, McMahon MM, et al. Clinical practice guidelines for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient--2013 update: cosponsored by American Association of Clinical Endocrinologists, the Obesity Society, and American Society for Metabolic & Bariatric Surgery. Obesity (Silver Spring). 2013; 21: S1-S27.
- Obinwanne KM, Fredrickson KA, Mathiason MA, Kallies KJ, Farnen JP, Kothari SN. Incidence, treatment, and outcomes of iron deficiency after laparoscopic Roux-en-Y gastric bypass: a 10-year analysis. J Am Coll Surg. 2014; 218: 246-252.
- Avinoah E, Ovnat A, Charuzi I. Nutritional status seven years after Roux-en-Y gastric bypass surgery. Surgery. 1992; 111: 137-142.
- Ruz M, Carrasco F, Rojas P, Codoceo J, Inostroza J, Basfi-Fer K, Valencia A. Heme- and nonheme-iron absorption and iron status 12 mo after sleeve gastrectomy and Roux-en-Y gastric bypass in morbidly obese women. Am J Clin Nutr. 2012; 96: 810-817.
- Broeke R, Bravenboer B, Smulders FJ. Iron deficiency before and after bariatric surgery: the need for iron supplementation. Neth J Med. 2013; 71: 412-417.
- Fried M, Hainer V, Basdevant A, Buchwald H, Dietel M, Finer N, et al. Interdisciplinary European guidelines on surgery for severe obesity. Obes Facts. 2008; 87: 468-476.
- Aarts EO, van Wageningen B, Janssen IM, Berends FJ. Prevalence of Anemia and Related Deficiencies in the First Year following Laparoscopic Gastric Bypass for Morbid Obesity. J Obes. 2012; 2012: 193705.