
Special Article - Eating Disorders
Ann Nutr Disord & Ther. 2016; 3(1): 1031.
Development and Preliminary Evaluation of a Nutritional Psycho-Education Group in a Community Eating Disorders Service
Khatun R¹, Conroy M¹*, Jeffereys K¹ and Frampton IJ1,2
¹Eating Disorders Service, Cornwall Partnership NHS Foundation Trust, UK
²Department of Psychology, University of Exeter, UK
*Corresponding author: Conroy M, Eating Disorders Service, Cornwall Partnership NHS Foundation Trust, Truro Health Park, Truro. TR1 2JA, UK
Received: October 07, 2016; Accepted: November 11, 2016; Published: November 14, 2016
Abstract
Introduction: Restoring healthy attitudes towards food choice and nutrition are at the core of successful treatment for eating disorders. However, little is known about what constitutes effective nutritional psycho-education for service users. This study evaluates a dietitian-led nutritional psycho-education group treatment for adults with eating disorders, specifically Anorexia Nervosa, Bulimia Nervosa and Eating Disorder Not Otherwise Specified.
Materials and Methods: Thirty-six service users attended a Food Choices group and completed questionnaires (a Food Choices Quiz, Personal Feedback Scale and Hopes and Worries Worksheet) before and after the group. Individual changes in scores were analyzed using a within-subjects design and written hopes and worries statements were reviewed using thematic analysis.
Results: Participation in the group was associated with significant increases in scores on the Food Choices Quiz and Personal Feedback scales of knowledge, confidence, trust, and skills to plan and eat healthy meals. Core themes were identified within the Hopes and Worries Worksheet reflecting factors about the group itself, food and eating, health, control and capacity (to believe in self, trust in others, learn and change).
Discussion: These data provide empirical support for the clinical effectiveness of a dietitian-led nutritional psycho-education group in enhancing adult service user understanding and positive attitudes towards healthy food choices. Further studies of variants of this intervention for children with eating disorders and their parents, and web-based delivery are warranted.
Keywords: Eating disorders; Psycho-education; Dietetics
Introduction
Anorexia Nervosa (AN) is a serious psychiatric illness that primarily affects girls and young women. The salient features of AN are severe weight loss, body image disturbance, overvalued focus on shape and weight, and fear of fatness. Mortality, estimated to be at a rate of 5% per decade of illness [1], is amongst the highest of any psychiatric disorder [2], with risk increasing with chronicity. Inpatient treatment programs are largely successful in achieving the initial treatment aim of weight restoration. However, relapse is common, and the rate of re-hospitalization within a year after discharge is estimated to be as high as 50% [3].
Patients with AN restrict their intake of food, thereby decreasing energy and nutrient intake. In the short term, hospitalization changes eating behaviors dramatically: by the end of a patient’s hospital stay, daily food intake can exceed 3000kcals [4]. Similarly, it has been shown that patients’ per-meal calorie consumption increased during weight restoration treatment but nevertheless remained substantially less than the average consumed by healthy control participants [5]. At the beginning of admission, patients given a free choice and multiple food options had a mean intake per meal of 364kcals, which increased significantly to 516kcals [6]. Again, healthy participants consumed significantly more, at over 750kcals per meal.
Although significant improvement on most psychological measures is realized with weight gain, often to normal levels [7], weight restored patients often still struggle with food choice and caloric intake. Specifically, dietary choices made by weight-restored patients on an inpatient unit are consistently lower in energy density and diet variety [6]. When patients were asked to choose their own menus, they consumed significantly fewer calories than controls, and interestingly reduced calories from fat [8]. These results suggest that nutrition remains quite abnormal in patients despite substantial weight gain and improvements in many psychological characteristics following successful weight restoration treatment.
Bulimia Nervosa (BN) is characterized by episodes of recurrent binge eating accompanied by inappropriate compensatory behaviors such as self-induced vomiting. When patient participants were observed eating a non-binge meal (an amount of food that they could consume without needing to purge) they ate significantly fewer calories compared to a control group [9]. Moreover, individuals with BN also markedly restrict food intake between meals. Consequently the following destructive pattern emerges, whereby the individual binge-eats, then restricts caloric intake in an attempt to compensate, appetite increases, inadvertently encouraging another binge eating episode. Treatment aims to interrupt this restrict-binge-purge cycle by encouraging patients to follow regular balanced eating; a major component of Cognitive Behavioural Therapy (CBT), the most effective psychological treatment for BN [10].
Effective nutritional counseling (consisting of meal planning, nutritional education and weekly weighting) typically incorporates psycho-educational and supportive elements [11]. Modified nutritional counseling incorporating psychological assessment and reformulation increases patients’ motivation to change [12].
A community-based Eating Disorders Service serving a large rural population in the south west of the UK has developed an integrated treatment approach whereby group and individual therapy (i.e. cognitive behavioural therapy, dialectical behavioural therapy, family therapy etc) and dietetic interventions are utilized at different stages of a single therapeutic plan. Since 2012, all new referrals are invited to attend our dietitian-led nutritional psycho-education group, Food Choices, at the beginning of treatment in line with the UK National Collaborating Centre for Mental Health [13] recommendation that nutritional psycho-education should be a standard part of treatment for patients with eating disorders.
Recent findings suggest characteristic abnormalities in eating behavior persist following intensive and lengthy care and, as a consequence, re-hospitalization rates remain high. Inpatient programs typically provide varied diets to promote the restoration of a healthy body weight but it is unclear if they always offer education around healthy food choices. Eating disorders include restricting caloric intake and avoidance of certain food groups, typically fat, starchy foods and sugars. Therefore, a psycho-educational intervention, to improve knowledge about healthy food choices may enhance our ability to treat these challenging illnesses.
In the absence of scientifically-established nutritional treatment standards in the UK, the present study was designed to investigate the impact of attending a psycho educational Food Choices group, for service users with a DSM-IV diagnosable eating disorder (i.e. Anorexia Nervosa, Bulimia Nervosa or Eating Disorder Not Otherwise Specified). We predicted that participation in the group will result in service users: i) increasing their knowledge about regular balanced eating, basal metabolic rate and body composition; ii) feeling more supported and better skilled to challenge their disordered eating; and iii) addressing their hopes and worries concerning healthy food choices.
Materials and Methods
Participants
In total seventy-eight service users attended the Food Choices group between May 2012 and May 2015. Thirty-six adult service users (35 female; 1 male) aged 17 and above (mean age = 30, range 17-55 years) completed both pre and post measures. Demographic variables including age, sex, and Eating Disorder (ED) diagnosis are collected at initial assessment for all service users and collated as part of routine clinical referral statistics. At this stage we also collected Global Eating Disorder Examination - Questionnaire Version - EDE-Q [14], scores ranged from 0.806 to 5.638, and Body Mass Index (BMI) ranged from 13.89 to 32.38, see Table 1.The EDE-Q is a validated questionnaire assessing ED characteristics including Restraint, Eating Concern, Shape Concern and Weight Concern. The sub-group who completed the full set of measures did not differ from the remainder of the attendees in distribution of eating disorder subtype, Age, EDE-Q score or Body Mass Index (BMI, see Table 1); we therefore conclude that the data are representative of all attendees. In both sub-groups EDE-Q scores spanned the ‘average’ to ‘clinically significant’ range and BMI spanned the ‘severely underweight’ to ‘obese’ range.
Age
EDE-Q
BMI
AN
BN
EDNOS-restrict
EDNOS-binge purge
N
Completed pre & post
-
-
-
15
7
7
7
Incomplete
-
-
-
15
10
8
9
Mean, SD
Completed
29.89 (10.30)
4.38 (1.08)
19.48 (4.72)
-
-
-
-
Not completed
27.76 (9.88)
5.67 (2.16)
19.58 (4.78)
-
-
-
-
EDE-Q: Eating Disorder Examination-Questionnaire version; BMI: Body Mass Index; AN: Anorexia Nervosa; BN: Bulimia Nervosa; EDNOS: Eating Disorder Not Otherwise Specified.
Table 1: Mean (standard deviation) Demographic Characteristics of Service Users with completed verses incomplete assessment, pre and post group participation.
Intervention
Table 2 summarizes the aims, intended learning outcomes, resources and activities for each of the three weekly one and a halfhour sessions. The sessions were delivered by two of the authors [MC and KJ], both experienced and registered Specialist Dietitians in eating disorders. The Food Choices intervention is a manualized treatment (available on request) built on well-established principles of nutritional education and food exchanges.
Aim
Learning Outcomes
Activities & Resources
Session 1
Explain Basal Metabolic Rate (BMR) and Total Energy
-Explore understanding and beliefs about BMR and consider the energy requirements of different physiological systems
-Calculate individual estimated total energy requirement and share with the group
-Discuss the consequences of semi starvation on BMR
-Begins with a participative discussion about BMR, what it is and the systems maintained by BMR
-There is then the opportunity to calculate personal estimated energy requirements
-Finally, the effect of eating less than requirement is discussed
Session 2
Explore regular balanced and adequate nutrition
-List and discuss the advantages of regular eating
-Identify the 5 different food groups and consider the roles of the food groups in regulating hunger and fullness
-List the number of portions of food from each group required for a healthy woman/ man
-Use the portion guide to determine what constitutes a portion.
-What is meant by regular eating is explored
-The different food groups are identified and their roles in hunger and fullness discussed. The number of ‘portions’ from each food group required to make up a balanced adequate diet is shared.
-Lastly, in pairs using plastic food models ‘what is a portion’ is explored using our portion guide
Session 3
Discuss the different components of a healthy body and consider how semi-starvation and low body weight impair health.
-Identify the different components of a healthy body
-Consider the impact of fluid balance on body weight
-Discuss the impact of semi-starvation on muscles in the body
-Identify where we find fat in the body and the role of fat in the body
-Identify the minerals found in the body
-Describe osteoporosis and how semi-starvation may contribute to the development of osteoporosis
Consider the impact of semi-starvation on glycogen stores
-Using participative discussion and a ‘human torso’ model the different components of the body (water, protein, fat, minerals and glycogen) are discussed. The different factors which influence fluid balance are explored and how this impacts on body weight. The importance of normal amounts of muscle and fat in functioning is considered and what happens to muscle and fat in the body when a considerable amount of weight is lost. Osteoporosis is described and the impact of semi-starvation on bone health and glycogen stores discussed.
-Finally, group attendees are invited to provide feedback.
Table 2: Aims, intended learning outcomes, activities and resources for the Food Choices group.
Measures
A battery of measures was completed by all service users at the beginning of session 1 and, again, at the end of session 3. The measures were all developed specifically for this intervention and piloted in a previous unpublished study, based on the psychometric principles for routine outcome monitoring specified by the UK Improving Access to Psychological Therapies programme [15].
Food choices quiz
This is an eight item measure designed to capture service users’ knowledge of the three topics included in the Food Choices programme. For example, item 2 asks “Eating regular, adequate carbohydrates (starchy / sugary foods) everyday helps…, a) Healthy skin, b) Mood, c) Concentration, d) Energy levels, e) Improve eyesight, and f) Regulate appetite. Service users were instructed to circle all the answers that applied. A maximum score of 37 can be scored on the entire measure.
Personal feedback scale
This measure requires service users to rate, using a Likert scale ranging from 0 (“not at all”) to 10 (“extremely so”), five statements identified as key areas for service users with eating disorders. These include: i)”I feel knowledgeable about eating for better health”, ii) “I feel confident about eating for better health”, iii) “I feel I can trust the information given in the Food Choices Group”, iv) “I feel I have the skills to eat for better health” and, v) “I feel that I have the skills to plan meals and snacks for better health.” A maximum score of 50 can be scored on this measure.
Hope & worries worksheet
This measure invites service users to write down any hopes or worries they may have about attending the Food Choices group before it begins and then re-evaluate them at the end of the programme. Service users are also prompted to rate each of their personal hopes and worries on a Likert scale ranging from 0 (“not at all”) to 10 (“completely there”).
Analysis
The Design is a quasi-experimental study without control group. Data were anonymised and securely stored. Preliminary inspection of questionnaire responses indicated that the data were normally distributed. Therefore parametric models exploring mean and standard deviation scores were computed using the Analysis Tool Pak Add-in for Microsoft Excel. Analysis of responses to the Hopes and Worries Worksheet was conducted by two authors [RK and IF] using thematic analysis [16]. Themes were coded by the two authors independently, and then patterns were identified amongst the codes to produce core themes. The themes and subthemes were subsequently jointly reviewed to achieve a consensus. The study was approved by the appropriate local research and audit governance committee.
Results
Table 3 shows that participation in the Food Choices group was associated with statistically significant increases in scores on the Food Choices Quiz (Total Score) and Personal Feedback Scale (Knowledge, Confidence, Trust, Skills to Eat, and Skills to Plan), indicating improved knowledge about food choices and improved skills.
Pre
Post
Difference
t-test (df)
P value
Food Choices Quiz
Total Score
25.3 (3.92)
31.3 (3.26)
5.97 (4.71)
7.61 (35)
<.001**
Personal Feedback Scale
Knowledge
5.63 (2.02)
7.94 (1.11)
2.31 (1.95)
7.01 (34)
<.001**
Confidence
4.20 (2.13)
6.37 (1.85)
2.17 (2.26)
5.70 (34)
<.001**
Trust
7.61 (2.14)
8.97 (1.56)
1.36 (1.59)
5.14 (35)
<.001**
Skills to Eat
4.73 (2.59)
7.17 (1.78)
2.43 (2.49)
5.36 (29)
<.001**
Skills to Plan
4.73 (2.65)
7.33 (1.92)
2.60 (2.54)
5.61 (29)
<.001**
Table 3: Mean (standard deviations) for Pre, Post and Difference Scores and t-tests.
Pre- and post-group responses to the Hopes and Worries Worksheet were analyzed for all participants who completed this measure (irrespective of whether they had completed responses to the questionnaire measures). In total 44 participants were included, reporting 83 worries and 158 hopes. Thematic analysis identified five main themes: (1) group, (2) food/eating, (3) health, (4) control, and (5) capacity. We also identified subthemes for all themes and present these visually, as recommended for Thematic Analysis [16,17]; see Figure 1.
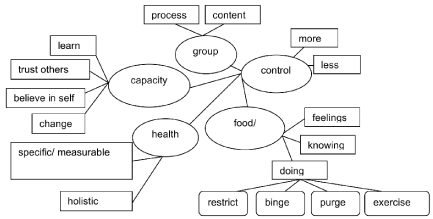
Figure 1: Thematic map, showing the five themes in relation to service users’ hopes and worries for the Food Choices group.
Theme 1 - Group: (a) content and (b) process
Worries: Participants worries were around the realization of what they were doing to their bodies. Other worries related to anxiety associated with being in a group and concerns that “people will judge” or that they would compare themselves to other group members, e.g. thigh width or overall weight.
Hopes: As well as being informative, participants hoped the group to be myth- busting and to challenge their eating disorder related beliefs and attitudes. Others looked for the group to also offer encouragement and instill hope. This was demonstrated in relation to both the group content, e.g. to be “reassured how much food is needed to maintain a healthy weight”, and the group process, e.g. “to feel I’m not alone and that there is hope for the future”.
Theme 2 - Food/Eating: (a) feelings, (b), knowing, and (c) doing
Worries: Participants were concerned that Food Choices may precipitate anxiety around eating or that the group would elicit difficult emotions and managing the anxiety around weight restoration. One person was concerned they may “develop an intense fear of food”. Participants also reported not knowing how exactly to fit regular eating into day to day life and were concerned they would not remember when to eat or that relying on hunger signals would lead to overeating.
Hopes: Participants report that they want to learn how to enjoy food again on their own, without guilt and anxiety and with others. Participants also hoped to stop restricting, over-exercising, bingeeating and self-induce vomiting. One person reported she hoped “to find the confidence to be able to eat a normal healthy diet without the constant battle that makes me feel like just giving up”.
Theme 3 - Health: (a) holistic, and (b) measurable/ specific
Worries: These reflected participants’ fears around either failing to weight restore (or maintain weight restoration) and around rapid weight gain. Other worries were associated with holistic health. For example, one participant said “I wouldn’t be happy in my own body image”.
Hopes: Participants wanted to work towards improved health in terms of weight restorations and being less preoccupied with food and, ultimately, recover. But hopes also extended to areas outside of eating. For example one participant said she hoped “to sleep more and think about food less.” Comments also reflected the hope that the group could also support participants to get their lives back. Specifically, participants said they hoped it would help “me as an individual,” “to be happy,” “to be free and able to enjoy life again,” “feel normal”, and to “live rather than exist.”
Theme 4 - Control: (a) more, and (b) less
Worries: Worries that tapped into the idea of more control were associated with rigidity and rule bound behaviors associated with eating disorders. Whereas, worries around less control were around the fear of failure, for example, “I’ll slip up/ relapse in the future after food choices” and “I will get worse” and where the person placed a lot of importance on factors outside of their control. For example, “I’ll feel too influenced by external factors.”
Hopes: Participants hoped to relinquish control, be less regimented and less rule bound. For example, wanting “to learn to let go,” “gain more flexibility with different foods and different situations.” In terms of having more control, participants’ responses were associated with the notion of accountability and taking action for themselves. One person hoped to “stop that habit for my health“.
Theme 5 - Capacity to: (a) believe in self, (b) trust in others, (c) learn, and (d) change
Worries: Participants’ reports suggested that they did not recognize that they had the capacity to participate in the group fully or benefit from the programme. Some participants talked about how they were too damaged to find the group useful. One person reported: “I feel too ashamed, too embarrassed, to take part. I should have sorted myself out by now”. Others spoke of mistrusting the information given by the Dietitians. For example, one person said “I won’t care what is said.” There were also concerns around not being able to follow the group content and not understanding the information given. The majority of participants’ worries echoed the concern of this participant, who said “Knowing what my body needs in order to function such as the amount of calories, but struggling to ensure I provide my body with it”.
Hopes: These were a mirror of the worries. Participants hoped they would learn, “correct,” “accurate information” from a trustworthy source and that participating in the group would afford change. Some talked about looking for motivation and wanting to succeed for themselves. A statement that sums this up is: “I hope the group will spur me into taking some positive action for myself”.
Discussion
The aim of the Food Choices Group was to offer a structured nutritional psycho-education programme for service users to increase awareness and understanding of core concepts of total energy usage, Basal Metabolic Rate (BMR), regular balanced and adequate nutrition, the components of a healthy body and the effects of semistarvation and low body weight on health. Preliminary analysis suggests that participation in the group by thirty six representative service users was associated with a significant increase in knowledge and positive attitudes towards healthy food choices, as measured by a Food Choices Quiz and Personal Feedback Scale.
Participants were also given the opportunity to record their worries and hopes for the group; subsequent thematic analysis revealed core themes in their responses that were consistent with the intended learning outcomes and content of the group sessions. Participants also raised concerns and hopes about being in sessions with other service users, suggesting that the ‘non-specific’ therapeutic aspects of the group process may itself be relevant to perceived value of participation.
This preliminary investigation had some important constraints. As a non-experimental study without a control group, we are not able to establish that the specific elements of the intervention per se were responsible for any of the observed changes. We also adopted broad inclusion criteria to enable clients with a range of eating disorders to participate. Future studies could adopt experimental designs and explore whether the programme has a differential impact on participants with different types of eating disorder.
It has been argued dietetic practice in the treatment of eating disorder patients is not well defined [18]. Most publications to date are descriptions of practice, with few evaluating the effectiveness of dietetic work. It has been argued that dietitians need to move from the clinical arena alone and become more involved in research, evaluating practice and defining a gold standard of nutritional treatment strategies that are best delivered by the dietitian [18]. The current evaluation is an initial attempt to evaluate a nutritional psych-education group in a community setting. We hope that the description and results of the present study will be helpful for other clinicians and researchers.
Although recent studies have begun to explore the nutritional components of weight restoration treatment (in terms of the dietary range and calorific value of food choices), there is a lack of knowledge about the ‘active ingredients’ of psycho-education programmes in promoting understanding of nutrition, healthy eating and their contribution to recovery. Anecdotally, participants in the Food Choices group appeared to be much more willing to participate in subsequent psychological therapies and less likely to drop out of treatment, a finding that has been shown for other ‘motivation enhancing’ interventions such as Cognitive Remediation Therapy [19]. Future studies could explore experimentally how Food Choices can contribute to improved overall outcome. Finally, we have been developing a guided self-help education pack version including DVD and workbook and a modified version for use in multi-family therapy for children with eating disorders; future studies could explore the acceptability and effectiveness of different delivery models for this promising innovative intervention.
Conclusion
A preliminary evaluation of a structured three-session dietitianled nutritional psycho-education Food Choices group suggests that participation is associated with significant improvement in service user understanding and positive attitudes towards healthy food choices for participants with significant eating disorders. Further evaluation is needed of both group and guided self-help versions to identify the active ingredients, long-term benefits and mechanisms of change.
References
- Sullivan PF. Mortality in anorexia nervosa. Am J Psychiatry. 1995; 152: 1073-1074.
- Papadopoulos FC, Ekbom A, Brandt L, Ekselius L. Excess mortality, causes of death and prognostic factors in anorexia nervosa. Br J Psychiatry. 2009; 194: 10-17.
- Pike KM. Long-term course of anorexia nervosa: response, relapse, remission, and recovery. Clin Psychol Rev. 1998; 18: 447-475.
- Pike KM, Walsh BT, Vitousek K, Wilson GT, Bauer J. Cognitive behavior therapy in the posthospitalization treatment of anorexia nervosa. Am J Psychiatry. 2003; 160: 2046-2049.
- Sysko R, Walsh BT, Schebendach J, Wilson GT. Eating behavior among women with anorexia nervosa. Am J Clin Nutr. 2005; 82: 296-301.
- Mayer LES, Schebendach J, Bodell LP, Shingleton RM, Walsh BT. Eating behavior in anorexia nervosa: before and after treatment. Int J Eat Disord. 2012; 45: 290-293.
- Attia E, Haiman C, Walsh BT, Flater SR. Does fluoxetine augment the inpatient treatment of anorexia nervosa? Am J Psychiatry. 1998; 155: 548-551.
- Hadigan CM, Anderson EJ, Miller KK, Hubbard JL, Herzog DB, Klibanski A, et al. Assessment of macronutrient and micronutrient intake in women with anorexia nervosa. Int J Eat Disord. 2000; 28: 284-292.
- Walsh BT. The importance of eating behavior in eating disorders. Physiol Behav. 2011; 104: 525-529.
- Wilson GT, Grilo CM, Vitousek KM. Psychological treatment of eating disorders. Am Psychol. 2007; 62: 199-216.
- Serfaty MA, Turkington D, Heap M, Ledsham L, Jolley E. Cognitive therapy versus dietary counselling in the outpatient treatment of anorexia nervosa: effects of the treatment phase. Eur Eat Disord Rev. 1999; 7: 334-350.
- Sorrentino D, Mucci A, Merlotti E, Galderisi S, Maj M. Modified nutritional counseling to increase motivation to treatment in anorexia nervosa. Eur Psychiatry. 2005; 20: 186-187.
- National Institute for Health and Care Excellence. Eating Disorders: Core interventions in the treatment and management of anorexia nervosa, bulimia nervosa and related disorders. London; 2004. Report No. CG9.
- Fairburn CG, Beglin SJ. Assessment of eating disorders: interview or self-report questionnaire? Int J Eat Disord. 1994; 16: 363-370.
- Boswell JF, Kraus DR, Miller SD, Lambert MJ. Implementing routine outcome monitoring in clinical practice: Benefits, challenges, and solutions. Psychother Res. 2015; 25: 6-19.
- Braun V, Clarke V. What can “thematic analysis”; offer health and wellbeing researchers? Int J Qual Stud Health Well-being. 2014; 9: 26152.
- Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006; 3: 77-101.
- Hart S, Russell J, Abraham S. Nutrition and dietetic practice in eating disorder management. J Hum Nutr Diet. 2011; 24: 144-153.
- Lock J, Agras WS, Fitzpatrick KK, Bryson SW, Jo B, Tchanturia K. Is outpatient cognitive remediation therapy feasible to use in randomized clinical trials for anorexia nervosa? Int J Eat Disord. 2013; 46: 567-575.