
Special Article - Malnutrition
Ann Nutr Disord & Ther. 2016; 3(2): 1034.
Malnutrition of Preschool Children in China: Past, Present and Future
Caixia D¹, Wang H², Zhengyu Y³ and Yin SA³*
¹Gansu Center for Disease Control and Prevention, China
²Department of Population Research, China Population and Development Research Center, China
³National Institute for Nutrition and Health, Chinese Center for Disease Control and Prevention, China
*Corresponding author: Yin Shi-an, National Institute for Nutrition and Health, Chinese Center for Disease Control and Prevention, Beijing, China
Received: September 26, 2016; Accepted: November 25, 2016; Published: November 28, 2016
Abstract
Children are the most vulnerable group to nutrition deficiency, especially for the children under 5 years of age. This paper reviewed the prevalence of malnutrition including stunting, underweight, wasting in past (before reforming and opening-up) and present (after reforming and opening-up) and doubleburden in undernutrition and over-nutrition of Chinese preschool children in future. With fast economic growth, health and nutrition status among the rural population has shown significant improvement in the past decades in China. However, malnutrition of Children remains a large health challenge in some poor and remote rural areas of North-western, South-western and Midwestern provinces of China. At the same time, the co-existence of underuntrition and over-nutrition (overweight and obesity) in both urban and rural areas has been called a “double burden” of disease. The prevalence of overweight and obesity in the urban areas is higher than that in rural areas, while nutrient deficiencies and wasting among rural children are much more common compared to the urban areas. Nutritional improvement for preschool children as public health policies should focus on implementing strategies such as alleviating poverty and improving household economic status, increasing dietary diversity, enhancing mothers’ nutrition education to address these deficiencies among children, carrying out supplementation and food fortification.
Keywords: Children; Malnutrition; Double-burden; China
Introduction
Children are the future for human beings and the foundation of sustainable human development of society. However, children are the most vulnerable group to nutrition deficiency, especially for the children under 5 years of age. Malnutrition in children is still a major health concern worldwide [1], which could result in the increase of morbidity and mortality of infectious diseases due to the decrease of immune ability [2-5], irreversible damage to the physical and mental health related to cognitive ability of children as well as also adversely long-term impact on economic performance such as the health and working productivity throughout adulthood [1-5]. Moreover, malnutrition prevalence of children is an important indicator of the Millennium Development Goals (MDG) set between 1990 and 2015.
Malnutrition includes stunting, underweight, wasting, and micronutrient deficiencies (vitamins and minerals) in general. Recent years, the term of malnutrition also covers overweight and obesity [6-9]. This article focuses on the prevalence of stunting (height-forage z-score < -2 based on WHO growth standard 2006), underweight (weight-for-age z-score < -2 based on WHO growth standard 2006), wasting (weight-for-height z-score < -2 based on WHO growth standard 2006) in past (before reforming and opening-up) and present (after reforming and opening-up) and double burden in undernutrition and over-nutrition of Chinese preschool children in future.
Past - Malnutrition is one of the Major Health Concerns before 1970s
China was a poor agricultural country about half centuries. During that time, China was a country with the largest agricultural population who was illiterate or semi-literate in the world. The number of children under 7 years was about 130 million which accounted for 13% of the whole population 40 years ago and there were about 80% of population living in the rural areas 30 or 40 years ago. Before the founding of the People’s Republic of China (1949), there was no complete survey data on children’s growth and development. It was estimated that the growth and developmental status would be very poor and infant mortality had as high as about two hundred per thousand in poverty rural areas of China [10]. Between the late 1950s and the late 1970s in China, improvement on food supply including quantity and quality virtually had not been taken place and available food was barely adequate to cover essential growth and work requirements in most areas [11]. During the neonatal period and first six-month period, most of infants (over 80%) were breastfed and their growth pattern was almost similar to the infants in the industrialized countries. After six months of age in rural areas or four months of age in urban areas, many infants were weaned from the breastfeeding or introduced with complementary food low in nutrient and/or energy density, which resulted in high prevalence of suboptimal growth, and micronutrient deficiencies such as iron, vitamin A, zinc, and B-vitamins [12]. Malnutrition of children under five years of age remained a large health challenge in China. During the winter of 1959 to the autumn of 1961, the Chinese Great Famine began and was more devastating in rural areas which resulted in highest mortality rate during the most severe period. Even though there were no data on children’ nutritional status at that time, it would be predicted that the preschool children’ situation (higher malnutrition prevalence and mortality) would be even worse due to severe food shortage [13-15].
Since the founding of People’s Republic of China on October of 1949, small sample surveys on children’ growth and development had been conducted in several cities. However, such surveys had some limitations in designs and methods. The first national nutrition survey in China was conducted in 1959, when the whole country experienced a serious natural disaster. The survey results were not published due to abnormal conditions in the whole national situation [13-15]. It was reported that the rapid increase in the prevalence of metabolic syndrome in middle-aged and elderly people in China was associated with the combination of exposure to famine (1959-1962) during the fetal stage and childhood and better economic status in adulthood [13-17].
The first published large-scale survey on children’s growth and development in 1975 was a survey of children’s physical development status in nine cities with consolidated method and supported by the central government. According to the surveyed result from 9 cities in 1975 [18], children’ weight and height from nine urban areas improved significantly compared with the data before liberation (1949). For example, the children’s growth and development of each age’s group in 1975 all had more significant improvement than that of results obtained from children aged from neonates to 11 years living well good condition in four urban areas of Beijing in 1937-1940 [18]. Before four decades, approximately 20 million infants were annually born in China and malnutrition was prevalent at that time.
Present - The Prevalence of Malnutrition Decreased Significantly from 1980 to 2015
Before 1970s, China was once one of the poorest countries in the world. For example, in 1981,it was estimated that poverty rate was about 84.0% in China, which accounted for 43.6% of total number of absolute poverty in the world. However, since reforming and openingup from 1980s, million poverty populations, poverty rate and ratio of total number of absolute poverty accounted in the world decreased to 157.1 million, 11.8% and 12.9% at the end of 2010, respectively, which resulted in the reduction of 678 million poverty populations, 72.2% poverty rate and 30.7% of total number of absolute poverty.
Following the implementation of a new reform and opening-up in China since 1978, it has already been bringing in a greater supply of non-staple foods such as animal foods including fish, poultry, eggs, milk and their products as well as a variety of vegetables and fruits, and appreciably improved Chinese diets due to the political stability of agriculture policies. All of these efforts have significantly improved the nutritional and health status of children in China. According to the second National Nutrition Survey in the autumn of 1982 (data were not published), survival problem, including food and clothing supply, has been basically solved and population’s nutrition status has been improved at national level in China. The average intake of energy and protein was respectively 67g/d and 2484 kcal/d reaching the Recommended Dietary Allowance (RDA) in that time and the signs and symptoms of typical nutrition deficiency diseases were rare. However, due to the unbalanced development at that time, there have been still millions of people living in remote areas and/ or mountainous areas, whose survival problem remains to be solved.
The second National Nutrition Survey was conducted in the autumn of 1982, but the data of this survey were not published and no information on malnutrition of children could be used. The change of malnutrition prevalence of children under five or six years of ages in China from 1992 to 2013 was showed in Figure 1. After reforming and opening-up and comprehensive development during the recent 30 years or so, China has rapidly achieved modernization and industrialization which has rapidly increased national power, obviously improved household income and resident’s living conditions and nutrition status, and significantly decreased the malnutrition prevalence in preschool children at nationwide. In 2013, the prevalence of underweight among children under 5 years in China was 2.4th% with an 85% decrease from 1992. The prevalence of stunting was 8.1%, with a 75% decrease from 1992, and the prevalence of wasting was 1.9%, with a 50% decrease from 1992. Prevalence of underweight and stunting among rural children was 3.1% and 11.3%, respectively by 2013. This represented an 84.0% and 67.7% decrease, respectively, from 1992 [19-21]. The prevalence of stunting was higher for children aged 1247 months and the prevalence of underweight was higher for children aged 48~59 months. The prevalence of undernutrition was higher in rural areas than in urban areas, especially in poor rural areas [22]. Figure 2 showed that all these were related to the dietary diversity and quality improvement. For example, even though there was not so much change of protein intake from 1982 to 2013, percentage of protein intake from animal food has been continuously increased, however, the proportion of protein intake from cereals and its product continued to decline during this period.
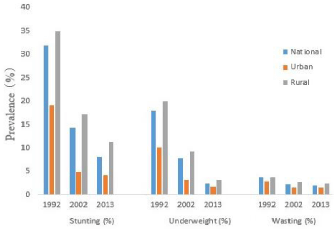
Figure 1: The change of malnutrition prevalence of children under five years
of ages in China from 1992 to 2013.
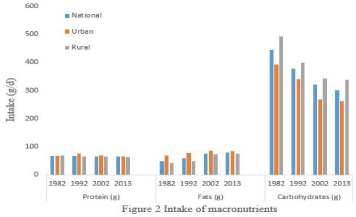
Figure 2: Intake of macronutrients.
The other surveys also showed that the same trend on malnutrition decline in children under 5 years of age in China. For example, according to child nutrition monitoring and improving projects in 1985-1989, involving children under 6 years of age in 18 poverty sites from 7 provinces, municipalities and autonomous regions, prevalence of stunting, underweight, and wasting was respectively 18.8%~78.1%, 11.6%~49.1%, and 5% based on WHO growth reference (Child Nutrition Monitoring and Improving Project in 1985-1989, unpublished data). The following project, involving 117000 children under 5 years living in 101 counties from 27 provinces, municipalities and autonomous regions in 1990~1995, showed that prevalence of stunting decreased from 36.2% in 1990 to 28.7% in 1995; percentage of underweight decreased from 23.7% in 1990 to 17.7% in 1995; and the change of wasting was not so significant which was related to the slower improvement in height (Child Nutrition Monitoring and Improving Project in 1990-1995, unpublished data). According to the physical measurement of preschool children from 9 cities in 1985, the average height and body weight were higher than that results in 1975 at the same age of group, but the growth and development status of Chinese children was still below the WHO recommended standard. Especially, children’s height and body weight in the rural areas were significantly lower than that of urban children. Date from 18 rural sites in 1985-1987 showed that the height and body weight of children living in low economic level of the family (annual per capita income < 200 Yuan) were significantly lower than that of children living in the family with average per capita income higher than 500 Yuan (the Physical Measurement of Preschool Children from 9 Cities in 1985, unpublished data).During 1990-1998, the prevalence of underweight was reduced from 8.0% in 1990 to 2.7% in 1998 in urban areas, and from 22.0% to 12.6% in rural areas; and stunting was respectively decreased from 9.4% to 4.1% in urban and from 41.4% to 22.0% in rural areas [23]. In 2005, Pei et al [24] reported that the prevalence of undernutrition evaluated by the Composite Index of Anthropometric Failure (CIFA) among children under three years of age in rural Western China was, 21.7% based on a total of 13532 children aged 0-36 months recruited from 45 counties and 10 provinces in Western China. In the survey of malnutrition and its influencing factors in children under 5 years of age in poor areas of China in 2009, the prevalence of stunting, underweight and wasting were 15.9%, 7.8% and 3.7%, respectively [25].
The improvement of child nutrition could be associated with rapid and sustained economic growth, which has fully proved by China’s development experience within recent 3 decades [26]. However, most of surveys indicated that program on children nutrition improvement should aim at improving malnutrition (especially stunting) and focus on child-bearing women and children under two years of age in order to prevent wasting and stunting in childhood [27].
Future - Facing Double-Burden of Malnutrition Since 2015
The scientific evidence on DOHaD (Developmental Origins of Health and Disease) indicates that the probability and necessity of prevention of adult diseases should start in the early life by promoting maternal and child health and reducing malnutrition by provision of high-quality complementary foods, promotion of a well-balanced dietary pattern and health literacy in the public. Because children are the future of a country or nation, achieving prosperity and sustainable development for a nation must start from teaching and training children in good condition both the physical and mental health.
In China, with fast economic growth, health and nutrition status among the rural population has shown significant improvement in the past decades. However, malnutrition of Children still remains a large health challenge in some poor and remote rural areas of North-western, South-western and Midwestern provinces of China [22,24,25,28]. The prevalence of micronutrient deficiency varied, including vitamin D, vitamin A, vitamin B2 and vitamin B12, irondeficient anemia, zinc, which were more substantial in rural areas compared with urban areas [29].
At the same time, the co-existence of underuntrition and overnutrition (overweight and obesity) in both urban and rural areas has been termed a “double burden” of disease. The prevalence of overweight and obesity in the urban area is higher than that in rural areas, while nutrient deficiencies and wasting among rural children are much more common compared to the urban areas. The data from National Survey on Nutrition and Chronic Diseases (2010-2013) revealed that the prevalence of stunting, underweight and wasting was respectively 8.1% (4.2% in urban, 11.3% in rural and 19.0% in poor areas), 2.5% (1.7% in urban, 3.2% in rural and 5.1% in poor areas) and 2.0% (1.5% in urban, 2.4% in rural and 2.7% in poor areas) in children under six years, while the prevalence of overweight was as high as 8.4% (same percentage in urban and rural areas)and the prevalence of obesity was as 3.1% (3.3% in urban and 2.9% rural areas) at the same age group [21].
The following issues also need greater attention such as significant urban-rural and regional disparities in child nutrition status, high prevalence of anemia and other micronutrient deficiencies among children; and nutrition concerns among vulnerable child groups, including migrant children in urban areas, and left-behind children in rural areas.
Nutritional improvement for preschool children as public health policies should focus on implementing strategies such as alleviating poverty and improving household economic status, increasing dietary diversity, enhancing mothers’ nutrition education to address these deficiencies among children, carrying out supplementation and food fortification which are all effective ways to reduce the prevalence of malnutrition and micronutrient deficiencies in children under five years of age, especially improving stunting in those children under two years of age in poor and remote rural areas [30].
References
- de Onis M and Branca F. Childhood stunting: a global perspective. Maternal & Child Nutrition. 2016; 12: 12-26.
- Bourke CD, Berkley JA, Prendergast AJ. Immune dysfunction as a cause and consequence of malnutrition. Trends in Immunology. 2016; 37: 386-396.
- Black RE, Allen LH, Butta ZA, Caulfield LE, de Onis M, Ezzati M, et al. Maternal and child nudernutrition: global and regional exposures and health consequences. Lancet. 2008; 371: 243-260.
- Hoddinott J, Alderman H, Behrman JR, Horton S. The economic rationale for investing in stunting reduction. Maternal & Child Nutrition. 2013; 9: 69-82.
- Mengistu K, Alemu K, Destaw B. Prevalence of malnutrition and associated factors among children aged 6-59 months at HidabuAbote district, North Shewa, Oromia regional state. J Nutr Disord Ther. 2013; T1: 001.
- Ngo J, Ortiz-Andrellucchi A, Serra-Majem L. Malnutrition: Concept, classification and magnitude. The Encyclopedia of Food and Health. 2016; 3: 610-630.
- Victory CG, Adair L, Fall C, Hallal PC, Martorell R, Richter L, et al. Maternal and child undernutrition: consequences for adult health and human capital. Lancet. 2008; 371: 340-357.
- Wilson HJ, Dickinson F, Hoffman DJ, Grififths PL, Bogin B, Varela-Silva MI. Fat free mass explains the relationship between stunting and energy expenditure in urban Mexican Maya children. Annals of Human Biology. 2012; 39: 432-439.
- Adair LS, Fall CHD, Osmond C, Stein AD, Martorell R, Ramirez-Zea M, et al. Association of linear growth and relative weight gain during early life with adult health and human capital in countries of low and middle income: findings from five birth cohort studies. Lancet. 2013; 382: 525-534.
- Li LM. Reflections on the public health of People’s Republic of China for the past 60 years. Chin J Publ Health Med. 2014; 30: 311-315.
- Smil V. China’s food: availability, requirements, composition, prospects. Food Policy. 1981; 6: 67-77.
- Yeung DL. Nutrition of infants and young children in China. Nutr Res. 1988; 8: 105-117.
- Wang Z, Li C, Yang Z, Zou Z, Ma J. Infant exposure to Chinese famine increased the risk of hypertension in adulthood: results from the China health and retirement longitudinal study. BMC Public Health. 2016; 16: 435.
- Wang N, Wang X, Li Q, Chen Y, Zhu C, Chen Y, et al. The famine exposure in early life and metabolic syndrome in adulthood. Clinical Nutrition. 2015.
- Li Y, He Y, Qi L, Jaddoe VW, Feskens EJM, Yang XG, et al. Exposure to the Chinese famine in early life and the risk of hyperglycemia and type 2 diabetes in adulthood. Diavetes. 2010; 59: 2400-2406.
- Xu H, Li L, Zhang Z, Liu J. Is natural experiment a cure? Re-examining the long-term health effects of China’s 1959-1961 famine. Social Science & Medicine. 2016; 148: 110-122.
- Wang N, Wang X, Han B, Li Q, Chen Y, Zhu C, et al. Is exposure to famine in childhood and economic development in adulthood associated with diabetes? J Clin Endocrinol Metab. 2015; 100: 4514-4523.
- Collaboration group of physical development of children and teenage from nine cites and Institute of Pediatrics of Chinese Academy of Medical Sciences. The investigation of physical development of children and teenage in the People’s Republic of China. Chinese Medical Journal. 1977; 57: 720- 725. (In Chinese).
- Ge K. The dietary and nutritional status of Chinese population – Children and adolescents (1992 National Nutrition Survey). Beijing: People’s Medical Publishing House. 1999. 2. (In Chinese).
- Yin S, Lai J. Nutritional status of children aged 0-6 years – 2002 National Nutrition and Health Survey. Beijing: People’s Medical Publishing House. 2008. (In Chinese).
- Bureau of Disease Prevention and Control in the National Health and Family Planning Commission. The report of nutrition and chronic disease status in Chinese populations (2015). Beijing: People’s medical publishing house. 2016: 21-29. (In Chinese).
- Yu D, Zhao L, Yang Z, Chang S, Yu W, Fang H, et al. Comparision of undernutrition prevalence of children under 5 years in China between 2002 and 2013. Biomed Environ Sci. 2016; 29: 165-176.
- Chang S, Fu Z, He W, Chen C. Current situation and trend of child growth in China. J Hyg Res. 2000; 29: 270-275. (In Chinese).
- Pei L, Ren L and Yan H. A survey of undernutrition in children under three years of age in rural Western China. BMC Public Health. 2014; 14: 121.
- Yu D, Liu A, Yu W, Zhang B, Zhang J, Jia F, et al. Status of malnutrition and its influencing factors in children under 5 years of age in poor areas of China in 2009. J Hyg Res. 2011; 40: 714-718.
- Wu L, Yang Z, Yin S, Zhu M, Gao H. The relationship between socioeconomic development and malnutrition in children younger than 5 years in China during the period 1990 to 2010.Asia Pac J Clin Nutr. 2015; 24: 665-673.
- Ramli, Agho KE, Inder KJ, Bowe SJ, Jocabs J, Dibley MJ. Prevalence and risk factors for stunting and severe stunting among under-fives in North Maluku province of Indonesia. BMC Pediatrics. 2009; 9: 64.
- Feng A, Wang L, Chen X, Liu X, Li L, Wang B, et al. Developmental origins of health and disease (DOHaD): Implications for health and nutritional issues among rural children in China. Bio Science Trends. 2015; 9: 82-87.
- Wong AYS, Chan EW, Chui CSL, Sutcliffe AG, Wong CK. The phenomenon of micronutrient deficiency among children in China: a systematic review of the literature. Public Health Nutrition. 2013; 17: 2605-2618.
- Zhang N, Becares L, Chandola T. Patterns and determinants of doubleburden of malnutrition among rural children: evidence from China. Plos One. 2016.