
Special Article - Eating Disorders
Ann Nutr Disord & Ther. 2017; 4(2): 1044.
Nutritional Rehabilitation for Eating Disorders: River Centre Clinic Program Description
Garner DM1,2*, Desai JJ¹, Desmond M¹, Good A¹ and Wohlers J³
¹River Centre Clinic, USA
²River Centre Foundation, USA
³Centre Syracuse and Buffalo Centre for Eating Disorders, USA
*Corresponding author: David M Garner, River Centre Clinic, 5465 Main Street, Sylvania, OH 43560, USA
Received: April 09, 2017; Accepted: May 11, 2017; Published: May 18, 2017
Abstract
Nutritional rehabilitation plays a central role in the treatment of eating disorders, and the varied plans recommended; however, it is noteworthy that the details of this aspect of treatment are rarely specified and little has been written on the theoretical principles behind the different approaches. This report describes our approach in sufficient detail to allow our outcomes to be replicated and compared with other programs. Our approach to meal planning has been referred to as “mechanical eating” and consists of a structured eating program in which quantity of food consumed, type of food consumed and spacing of meals, are all specified in advance. This approach is designed to temporarily remove decision-making associated with eating and relies on a set of rules for starting, maintaining, and stopping eating designed to override the complex physiological and psychological cues that typically disrupt normal eating among those with eating disorders. It diverges markedly from the Exchange System recommended in many nutritional rehabilitation programs. It relies heavily on using commercially available packaged meals and prescribing the exact number of Calories to be consumed throughout the day. Body weight is checked on each treatment day and Calories are adjusted to promote steady weight gain in anorexia nervosa and weight stabilization in other eating disorders when weight suppression is less prominent. We have anticipated potential criticisms of this approach and have provided the theoretical and practical basis for our model.
Keywords: Anorexia nervosa; Eating disorders; Nutritional rehabilitation; Body weight
Introduction
The plan for nutritional rehabilitation varies significantly between different eating disorder programs. Despite the central role of nutritional rehabilitation in the treatment of eating disorders, and the varied plans recommended, it is noteworthy that the details of this aspect of treatment are rarely specified and there is even less written on the theoretical principles behind the different approaches. Hart, Franklin, Russell & Abraham [1] reviewed 26 papers describing the feeding methods used in the inpatient treatment of Anorexia Nervosa (AN) and conclude that there are no evidence-based guidelines for the best and safest method for nutritional rehabilitation comparing four different feeding methods: 1) food only, 2) high energy food supplements plus food, 3) nasogastric feeding and 4) Total Parenteral Nutrition (TPN). Most papers reviewed describe two or more of these methods applied during treatment. Similar findings are reported by Garber and colleagues [2] in another recent review of inpatient programs indicating that the most popular approaches to re-nutrition use either meals only or combine meals with nasogastric feeding. Both reviews recommend that all reports on refeeding should include, at a minimum, admission and discharge BMI, weight change during treatment and length of stay. The lack of detail regarding the feeding regimes employed as well as the limited evidence on efficacy led to the view that no conclusion could be offered regarding the most effective method of achieving nutritional rehabilitation in AN. The aim of this paper is to provide sufficient detail about our approach to facilitate replication in other settings as well as understand the methods we follow so that our outcomes [3] can be compared to other programs.
Our approach to nutritional rehabilitation has been employed for more than 20 years in our Partial Hospitalization Program (PHP) and Adolescent Residential Program (ARP) in Ohio and more recently in two programs in New York. The Ohio PHP is for adults and combines 35 hours per week (11:30 am - 6:30 pm, 5 days-a-week, 7 hours-aday) of programmatic treatment with the option of independent dormitory-style living outside of program hours at no additional cost. The average age for those admitted to the PHP is 25.7 years (range: 18-67 years old). The ARP is 24 hours a day, 7 days-a-week; however, patients are often stepped down to fewer days near discharge based on clinical need and parent availability for monitoring. The average age for adolescents is 15.5 years (range: 9-17 years). Both programs follow a well-established evidence-based enhanced cognitivebehavioral treatment model that integrates individual, group, and family therapy [4-8]. The nutritional rehabilitation component of our structured approach, sometimes referred to as “mechanical eating,” has been described earlier for outpatient treatment [9,10]. Because of its meticulous attention to detail, the use of Calories (rather than the exchange system) and the reliance on commercially available packaged meals, our current approach to meal planning has been the subject of some controversy, although to our knowledge, not in the written literature. Thus, we will try to anticipate and address possible concerns that could be raised about certain aspects of this highly effective approach to nutritional rehabilitation.
The ultimate nutritional goals in the treatment of eating disorders are to help patients: 1) achieve and maintain an appropriate body weight, and 2) become more relaxed about the process of eating evidenced by eating a wide variety and enough food without guilt or resorting to dangerous compensatory behaviors. Most nutritional programs recognize the importance of encouraging regular eating patterns and incorporating previously avoided foods into the food plan. One of the first steps in this process is nutrition education with particular emphasis on dispelling myths about food and eating that are typical of those suffering from eating disorders [10]. The response to accurate information about eating and weight is central to mapping the proper course of treatment that addresses motivational impediments to change. Food, eating and weight are highly emotionally charged topics and failure to present a clear rationale behind the approach to nutritional rehabilitation can seriously impede motivation to change.
Different systems employed for food intake and meal planning
In a review of feeding methods used in inpatient treatment of AN, Hart and colleagues [11] reported that the most common protocol was nasogastric feeding and food followed by high-energy liquid supplements and food. In a separate review, Garber et al. [2] found that meal-based approaches and nasogastric plus oral intake were both common in inpatient treatment settings and that both can administer higher Calorie levels safely in mildly or moderately malnourished patients. Most inpatient programs for anorexia nervosa rely upon meals alone for energy intake; however, a significant proportion either combines meals or meal supplements with nasogastric feeding [12]. A minority rely upon total parenteral nutrition for weight restoration. There is some evidence for the success of non-hospital treatment settings in weight restoration; however, most of the studies published provide insufficient detail in the description of the nutritional rehabilitation program to allow replication in other settings [2]. An important consideration in describing nutritional rehabilitation for AN as well as other eating disorders is the system for planning and implementing meals.
Most authorities agree that planning meals in advance and eating according to a schedule are useful strategies in the management of eating disorders. However, descriptions of meal planning differ markedly in the details of the approach. Recommendations diverge in the degree to which structure and rigidity are applied to meal planning. Some programs are highly structured and insist on adherence to a specific plan for eating with clear rules pertaining to the amounts and types of food to be eaten. Others are more flexible and encourage patients to eat what is comfortable with gradual progression toward improved eating patterns. In some cases, advice is inconsistent. Sometimes there is a mix of planning meals in advance alongside strategies that encourage flexibility or spontaneity in eating with little attention to the potential impact of inconsistencies and contradictions in methods. For example, Brunzell and Hendrickson- Nelson [13] suggest planning eating in advance but also advocate eating in response to hunger and satiety cues without clarifying when to use these different approaches. We find that patients find this mixing of models to be confusing.
Our approach to meal planning consists of a structured eating program in which quantity of food consumed, type of food consumed and spacing of meals, are all specified in advance. We explain the plan and the rationale in the initial assessment to increase compliance on the first day of treatment. It is emphasized that this process is not designed to take away control from patients but rather to ultimately increase their sense of control and choice around food intake. Patients are encouraged to accept the view that adherence to the structured plan may be thought of as “an experiment” that will give them a better understanding of the relationship between caloric intake and weight [4,8]. Resistance can be diminished by reminding patients that they are not making a commitment to permanent change by participating in this “experiment” and it does not prohibit them from returning to their eating disorder in the future if they are unhappy with recovery. The aim of structured eating is to replace their current depleted state, dietary chaos and sense of hopelessness with predictability, control and possibly new options for the future.
Goal weight range: It is well established that low discharge weights are negatively associated with outcomes in studies of adolescent and adult AN patients [14-21]. In multisite study, Steinhausen and colleagues [22] present convincing data indicating the “strong effect of insufficient weight gain during first admission and lower BMI at the first discharge emphasizes the importance of adequate interventions” (p. 29). Traditionally, objectively low body weight, usually measured as BMI, has been the target for measuring outcome; however, recent studies have identified the magnitude of weight suppression as an important predictive variable in AN [23,24]. Determining the goal weight range for an eating disorder patient entering treatment is not a precise science since there are genetic and environmental factors responsible for significant individual differences in expected body weight. In setting goal weights, we are informed by highest past high weights as well as growth chart trajectories, particularly for adolescents. Patients begin treatment with the knowledge that they are on a weight gain or a weight maintenance protocol but we generally do not share an exact target weight range at the beginning of treatment. It is explained that with enough information, we can usually arrive at a good estimate of a healthy body weight; however, it is first necessary to collect detailed information on their weight history, growth charts and metabolic response to Calories prescribed during treatment. Most patients initially disagree with goal weight ranges and it is important to gently convey the notion that we really do not determine body weight in the strict sense since it is their biology that establishes and regulates body weight. Obviously, goal weight is a sensitive topic for patients and discussions must be sensitive to the patient’s level of insight and tolerance for change. As patients receive more education on the biology of weight regulation and its implications regarding their personal weight history, preliminary weight goals are established and shared with the patient along with the knowledge that the goal weight range may need to be adjusted over time. Again, it is important to convey the concept of treatment as “an experiment” designed to restore health, eliminate food preoccupations, and reduce vulnerability to binge eating that can result in marked increases in body weight.
For patients who need to gain weight in treatment, Calories need to be prescribed to create gradual and systematic weight gain at a rate of 2-3 pounds a week. If patients gain too quickly, then they need to know that their Calories will be cut. Once a maintenance weight has been achieved, Calories will be adjusted to keep weight within a 5-pound range. This reassurance can be bolstered by reviewing examples of weight charts like the one in Figure 1 which shows this steady and predictable increase in weight followed by maintenance in the goal weight range. It is both surprising and reassuring to many patients how rapidly metabolic rate is boosted in response to increases in Calories prescribed [25] (see triangles in Figure 1). Patients are encouraged to view food as “medication” and the “dosage” is designed to increase metabolic rate while creating predicable weight gain. If weight gain is not the main goal of treatment, then the Calories are adjusted to maintain a stable body weight that is consistent with the patient’s genetic and/or biological predisposition and this can be expected to lead to a marked decline in disturbed eating patterns, as well as emotional and cognitive symptoms. It is our assumption that normalization of body weight is absolutely required to promote “healing” from the ravages of chaotic eating patterns and chronic starvation/dieting.
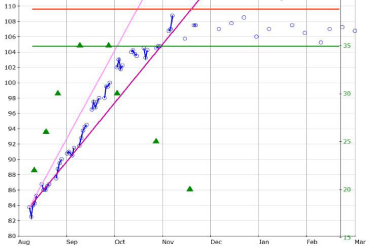
Figure 1: Figure 1 illustrates weight gain and maintenance for an anorexia
nervosa patient in the Partial Hospitalization Program (PHP). The circles
represent weight on days of PHP with connected lines representing
contiguous days of treatment. Spaces early in treatment reflect weekends
and later denote outpatient meetings after discharge from PHP. The goal
weight range for this patient is represented by the two parallel lines at 104
lbs. and 109 lbs. respectively. The triangles are Calorie levels as seen on the
right vertical axis.
Daily weighing protocol: All patients are weighed backwards on a scale on treatment program days and their weight is recorded in a medical record that can generate body weight graphs. Resistance to blind weighing is countered by letting patients know that there is a tendency to over-react to minor shifts in daily weight that we strongly suggest that they focus on trends when we show them their weight graph after the first week of treatment. Patients usually review their weight graphs with their therapist weekly; however, some are content to review weights less often. Some patients are particularly sensitive to numbers and prefer to see their weight trends but without the numbers.
Any deviation from the eating plan, whether under-eating or over-eating, is strongly discouraged. Patients are encouraged to be honest and consume every Calorie since failure to do so will result in “bad data” leading to a poor understanding of their caloric needs when they reach a maintenance weight. For patients who refuse to follow the meal plan and cannot tolerate weight gain at the Partial Hospitalization or Residential levels of care, transfer to an inpatient setting may be necessary. Most patients will admit that the structured eating plan and predictable weight gain in a non-hospital setting is far more acceptable than the more restrictive hospital setting that may rely on more aggressive approaches to re-nutrition such as tube feeding, TPN or mandatory supplements. It can be helpful for patients to know that their feelings about their bodies can improve with treatment. Patients can benefit from the knowledge that body image and beliefs about weight can change during treatment. Although AN patients gain a significant amount of weight during treatment (an average of about 20 pounds), we have reported significant improvements on all EDI-3 [26] scales at discharge, including improvements in Body Dissatisfaction and Drive for Thinness [3].
Patients are strongly encouraged to be weighed weekly after discharge by their therapist or physician and to swiftly return to a higher level of care if downward weight trends cannot be interrupted in outpatient treatment. There is a tendency to view readmission as “a failure” and this inevitably results in a costly full-blown relapse. Readmission for “booster treatment” early in the relapse process can be very effective and much less costly than weight restoration following a full relapse [3]. Even modest efforts to restrict intake must be discouraged because of the risk of relapse and binge eating among those who have never shown this eating pattern (i.e. almost 90% of patients who present with the “pure restricting” eating pattern will resort to binge eating weight over a 8 year follow-up) [27].
Overriding disruptive physiological and psychological cues: The structured approach to meal planning is designed to temporarily remove decision-making associated with eating by relying on a set of rules for starting, maintaining and stopping eating. It is aimed at overriding the complex physiological and psychological cues that typically disrupt normal eating among those with eating disorders. It is well-established that restrictive dieting and weight suppression lead to extraordinary disruption in the physiological mechanisms that regulate hunger and satiety. The profound biological and psychological impact of severe dietary restriction and weight suppression is best illustrated by the classic study of experimental semi-starvation by Keys et al., [28] in which normal men lost a significant amount of body weight over six months leading to dramatic disruption in internal hunger and satiety cues, binge eating, food preoccupations and emotional disturbance during weight loss. This study of normal volunteers illustrates that binge eating, confusion in hunger and satiety cues, food obsessions, and emotional symptoms did not normalize immediately following weight restoration but persisted for up to one year after body weight returned to normal levels. We have summarized this study and described its relevance in distinguishing primary from secondary symptoms of eating disorders [9,10,29]. It also makes it clear that recovery is not possible without normalization of body weight. The structured eating plan we advocate is a powerful shorter-term strategy for countering the extreme starvation induced physiological derangement that is typical of those suffering from severe eating disorders. If restrictive eating, binge eating and compensatory behaviors can be held in check, the damage caused by severe weight suppression slowly abates and eating will become more naturally regulated by internal signals.
It is well-known from the clinical literature on eating disorders that restrictive eating, bingeing and engaging in compensatory behaviors can be triggered by a host of psychological (non-nutritional) factors such as feeling fat, guilt, anxiety, depression, and anger [4]. These triggers may be functional by moderating unpleasant emotions in the short run but they are obviously self-defeating in the long run. Positive cues, such as feeling “in control,” virtuous or thinner, can also trigger eating disordered behavior and, in some cases, the eating disorder itself can have a positive connotation [8,30] which reinforces continued symptomatic behaviors. Our structured eating plan is designed to override intense psychologically driven “urges”, or shifts in thinking and feeling that can trigger a collapse in adherence to meal planning goals. In sum, eating for nutritional reasons is the long-term objective. However, for most of those suffering from serious eating disorders, psychological triggers are so intense early in treatment that it is unrealistic to assume that eating can be normalized by simply intensifying the focus on subtle hunger and satiety cues.
Meal planning phases
Meal planning can be divided into three phases. During the initial phase of our approach to meal planning, Calorie levels are specified in advance with an emphasis on completing all Calories in the amounts and times prescribed. In this first phase, staffs members take responsibility for planning and preparing meals after consulting with the patient about certain food preferences and patients are encouraged to complete meals within 30 minutes. On the first day of treatment, the rationale for the plan is carefully explained and patients are presented with three meals carefully chosen to be low on the hierarchy of feared meals along with the statement: “I know that you probably do not feel comfortable eating any of these meals; however, they are carefully Calorie controlled. Which one of these choices would you prefer?” Usually with some encouragement, one of the meals is chosen. Patients are provided with the theoretical rationale for the value of exposure to feared foods and response prevention (i.e. inhibit compensatory restrictive dieting and other compensatory behaviors) within the context of carefully monitored body weight. Gradually, patients are provided with foods that elicit greater anxiety and patients are shown that the Calories are kept exactly at the level prescribed. As will be discussed later, the Calorie level is set based on body weight, weight history, and recent eating patterns. Body weight is assessed on each program day and changes in Calorie levels are made to maintain goals for body weight in treatment. This first phase usually lasts for one or two weeks based on the patient’s success in acclimating to the structure of the meal plan and their motivation to address idiosyncratic eating (slow eating, inappropriate bite size, etc.). Even more resistant patients will comply with staff encouragement and feedback so that they can select their own foods in the next phase of treatment.
In the second phase, patients create their own meal plans but work closely with staff members who provide feedback to help maintain adherence to all aspects of the plan including a high level of exposure to feared foods. Patients are also encouraged to challenge “food ruts”, overly narrow eating patterns, by eating wide variety of foods. This phase lasts from 5 to 10 weeks. In the third phase, patients plan meals on their own with more relaxed staff feedback about food choices. This phase often is implemented after the patient is discharged from Partial Hospitalization or Residential Program levels of care. The duration of this phase is quite variable. Some patients prefer the safety and security of adhering closely to the structure of meal planning to mitigate guilt about perhaps eating “too much” and guard against relapse. Patients may engage in this rigid form of meal planning for six-months or a year or more and often endure social or family pressures to stop meal planning and “eat normally.” We try to remind patients and those close to them that while eating disorders can have a fatal outcome, this is not the case for prolonged meal planning. Even though rigid meal planning may not be aesthetically pleasing, if it leads to a feeling of safety and prevents relapse, it is a small price to pay. Moreover, because rigid meal planning is tedious and time-consuming, it almost always wanes overtime. The eventual goal is for patients to become more relaxed about the process of eating evidenced by eating a wide variety of foods and consuming an amount of food to maintain their healthy body weight without reverting to restrictive dieting or dangerous compensatory behaviors. It has been our experience that moving too quickly toward a more flexible approach in some areas (e.g. making judgments about food preparation, portion sizes and eating in response to hunger and satiety cues) can lead to much slower progress in exposure to feared foods and less confidence that body weight responds in a predictable manner. It is better to err on the side of caution and meal plan longer than necessary than to prematurely discontinue with the risk of relapse.
In sum, the early phase of meal planning is highly structured; meals and snacks are specifically designed to provide a high level of exposure to feared foods. Greater flexibility is introduced in later phases of meal planning but there still is an emphasis on adherence to “mechanical eating” to reduce the likelihood of deviating from the nutritional goals in treatment. During all three phases, psychoeducation related to common dietary myths, the ineffectiveness of dieting, the effects of starvation on behavior, and the biology of weight regulation are critical to creating motivation to maintain compliance with program principles.
Meal planning structure
Meal planning focuses on three specific components specified in advance: 1) The quantity of foods consumed; 2) The types of specific food items consumed; and 3) The timing or spacing of meals.
Quantity of Foods Consumed
For mildly or moderately emaciated AN patients, the initial Calorie level is typically set at 1,800-2,200 a day and gradually increased 3,500-4,000 Calories a day in 400-500 increments to achieve the desired 2-3 pound-a-week rate of weight gain. The rationale for increasing Calories in 400-500 Calorie increments is that smaller increases would require more Calorie changes over the course of treatment and since each increase is upsetting, fewer are generally better. According to recent reports, a greater rate of weight gain for mildly or moderately malnourished patients can be achieved without medical complications [2,31-34]. Moreover, a higher rate of weight gain has been shown in some studies to be an important predictor of short-term clinical outcome after discharge [35,36]. Despite the findings that a rate of weight gain of 2-3 pounds a week is achievable and safe for most AN patients, more than 70% of inpatient programs increase Calories slowly and fail to achieve the 2 pounds per week standard [11]. It has been recommended that for extremely emaciated AN patients, the initial Calorie levels should be lower and the initial rate of weight gain should be slower to minimize the risk of refeeding syndrome [37]. Therefore, for extremely emaciated AN patients, particularly for those with hypokalemia, hypoglycemia, hypophosphatemia or hypomagnesemia, we typically start Calories at as few as 1,400-1,600 a day and placed them on a low carbohydrate diet to reduce the risk of refeeding syndrome. Once laboratory values normalize, Calories are increased to achieve the target rate of weight gain of 2-3 pounds a week and their overall pace of weight gain tends to be somewhat faster than for less emaciated patients. Consistent with earlier reports, we have found that the greater rate of weight gain is safe and we have not experienced any cases of refeeding syndrome in the past 20 years.
There is significant variability in the Calorie requirements to achieve the desired rate of weight gain goal of 2-3 pounds per week [38-40] as well as the Calories required to maintain a stable body weight. The reasons for this wide range have been attributed to individual differences in body weight history, thermo-regulatory response to food, fluid shifts, age, and physical activity [12]. However, it is important to emphasize that Calorie needs vary considerably even across individuals who do not have eating disorders [41]. Patients with a history of obesity may be hypometabolic and gain weight easily. Others require more Calories to achieve the 2-3 pounds of weight gain per week. Kaye et al. [42] have shown the amount of exercise typical for AN patients can account for a three-fold increase in the Calories required to gain 1 kilogram of body weight. Patients are generally receptive to the rationale that starting on a higher number of Calories is effective in increasing metabolic rate which, in turn, burns more Calories [25]. In our clinical experience, this protects against urges to engage in binge eating. The number of Calories prescribed may seem excessive to some emaciated patients, particularly those who have maintained their weight on far fewer Calories prior to admission; however, it is useful to remind patients that a 500 Calorie increase translates into no more than one additional pound per week without factoring in the increase in metabolic rate created by the Calorie increase. Moreover, it is explained that Calories will be cut if the slope of the weight gain curve is faster than that agreed upon. Once the patient is 3-5 pounds from their tentative goal weight range, Calories are reduced so that they can “settle” within a 5-pound range.
In our adult partial hospitalization and adolescent residential programs, we follow the same structured approach to nutritional rehabilitation for patients with BN and other serious eating disorders as employed for AN. The initial number of Calories typically prescribed for BN patients is between 2,000 and 2,500 per day. Prescribing Calories and carefully monitoring weight daily diverges significantly from earlier recommendations by Fairburn for BN in which patients are “actively discouraged from counting Calories, and especially from any tendency to keep a running total” (p. 173) [43]. A detailed exploration of the patient’s weight history may reveal that their weight is as suppressed as the typical for AN [44,46]. High levels of weight suppression have been associated with higher levels of binge eating [47], greater weight gain in treatment [48], poor outcome in the cognitive-behavioral treatment of BN [49], and a longer time to full remission [50]; although some studies have failed to replicate the association with treatment outcome [51]. For those patients who are highly weight suppressed, Calorie requirements are generally less than for those closer to their highest weight. Ideally, Calories are adjusted based on understanding of the patient’s likely “non-dieting” body weight in the absence of weight suppression. The widespread failure to understand the fact that there are marked individual differences in caloric needs and expected body weight means that most patients require considerable psychoeducation regarding set-point, “settling point,” and the biology of weight regulation to accept a higher body weight [10,52].
Metric for prescribing food intake: Calories versus the Exchange System. Different meal planning systems have been recommended in re-nutrition programs for eating disorders. As indicated in the preceding sections, we rely on Calories in discussing the quantity of food intake. Although little has been written about the respective advantages and disadvantages of the various metrics used with patients with eating disorders, we believe that the rationale for prescribing Calories in a precise manner is appropriate on practical and theoretical grounds. According to Reiter & Graves [53] the two most common foundations for developing meal plans are the Exchange System and My Pyramid (p.132). The Exchange System is probably the most widely used approach in eating disorder treatment programs and involves categorizing foods into six groups in which the portion sizes are specified and the foods in each group are roughly equivalent in caloric value and macronutrient content according to the American Diabetes Association [54]. In this system, foods within each nutrient-dense group can be traded or “exchanged” with another food within that group. The Exchange System was developed for the diabetic population and this patient group has no apparent systematic selection bias toward selecting “exchanges” designed to lose weight. The logic of the Exchange System is that the small Calorie differences in equivalent exchanges would even out over time in the absence of any systematic bias toward consuming fewer Calories. This contrasts with eating disorder patients who characteristically try to restrict food intake and Calories to lose weight. We sometimes illustrate the problem with the Exchange System in the treatment of eating disorders with the graphic illustrated in Figure 2. When it is explained that both Apple 1 and Apple 2 represent two fruit exchanges, patients are asked which one would they pick given their eating disorder and they almost invariably pick Apple 2. If the choice is now between all three apples, patients choose the smaller one (Apple 3) as part of their restrictive dieting mindset. For patients with the proclivity for binge eating, it may be a bit more complex; however, when asked to choose this hypothetical apple, they also invariably pick the smaller apple because of their predilection toward dieting. Nevertheless, in the act of binge eating, they might lose control and eat the larger apple or five apples (or more likely a highly calorific alternative).
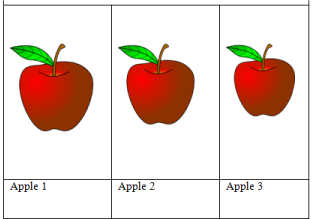
Figure 2: One large apple = 2 fruit exchanges. All three of the apples above
are “large” apples. What determines the eating disorder patient’s choice
versus that of the diabetic patient?
With the Exchange System, eating disorder patients intentionally or sometimes unintentionally tend to “shave” Calories by picking a smaller quantity of food or lower Calorie food items (e.g. low fat, diet foods) having the same exchange value. The problem with the exchange system is that it is inherently imprecise and allows for systematic estimation errors, in the context of extreme fears of “eating too much.” The consequence is a tendency to drift toward restricting caloric intake over time. As stated earlier, the final goal of treatment is to help patients become more relaxed and natural in their approach to eating. However, it is not necessary to progress toward this goal in a linear manner. We use the analogy that structured eating is like a splint on a broken bone- it maintains rigidity and structure while healing takes place. In this case, structure allows a period of stability followed by gradual and incremental progress toward a more flexible or “normal” eating style. The intensity of fear around eating is overwhelming early in treatment and this fear can be lessened by reassurance that the system that we use is precise and that we are committed to not having patients eat one Calorie above their meal plan and by the same token, we want them to not eat one Calorie less. By having knowledge of exactly how many Calories patients are consuming, and carefully monitoring their weight, we can assure them that they will not be allowed to gain outside of their weight range. The reassurance, predictability, and safety are of paramount importance. This practice helps build trust between patients and staff as well as trust in the program’s efficacy. Later, once the patient can see that weight and weight changes are predictable, with staff being equally willing to cut Calories as to raise them in accordance with the nutritional plan, patients are reassured. They virtually never are enthusiastic about weight gain but in many cases, the lack of predictability is the major source of fear. Patients in our program have expressed that it is easy to “manipulate” the exchange system and avoid challenging feared foods.
The meticulous attention to detail related to nutritional rehabilitation (i.e. prescribing precise Calorie levels, showing painstaking vigilance during meals, and therapists having daily access of body weight) is meant to reassure patients that their worries about food and weight are taken very seriously. We jokingly assert that we are even more “obsessed” about Calorie level and weight than most patients since our reputation depends on them being able to trust that we will be conscientious and that we are ultra-responsible in temporarily “managing” body weight. Thus, the structured nature of the nutritional rehabilitation plan is designed to increase the person’s control over the eating process and to minimize the tendency to lose control over eating and body weight. The aim is for patients to begin to develop confidence that they can eat the specified amounts of food without inappropriate weight gain. We encourage “good data” by discouraging symptomatic behavior so that patients can develop confidence in their weight and intake over time.
Does Calorie-counting increase preoccupations with food and Calories?: One of the most commonly raised criticisms of counting Calories and fat grams in meal planning is that it serves to reinforce obsessive preoccupations with food. First, it is hard to imagine how one could increase the level of Calorie preoccupation in a group of eating disorder patients who are already obsessively fixated on Calories. If there is a ceiling effect to preoccupation, most seriously ill eating disorder patients are very near this ceiling. Second, particularly for highly anxious, obsession and perfectionist patients, a more precise system of quantifying food intake (devoid of estimation error) increases certainty and predictability and this allows most to rather quickly begin eating a wide range of foods in appropriate amounts. These perfectionist patients have a cognitive style characterized by a preference for order, precision, exactness, symmetry and sameness in the interest of avoiding perceived adverse outcomes. In this way, the cognitive style and information processing biases are harnessed in the interest of the therapeutic goals of nutritional rehabilitation. Third, this structured system related to food intake also works well for impulsive patients who benefit from external controls to counteract their tendency toward poor planning and impetuous decisions related to food choices. Finally, perhaps the most compelling argument for the system we propose is empirical in that we have achieved very positive body weight outcomes using this nutritional rehabilitation plan [3].
Calories as energy: It is often helpful to defuse the surplus meaning that is ascribed to the word “Calorie” with a psychoeducational approach. For patients, the word has often taken on a special and pejorative meaning associated with body fat. Patients benefit from being reminded that a Calorie is defined technically as a unit of energy equal to the amount of heat required to raise one kilogram of water by 1° Celsius under standard initial temperature. Calories, just like British Thermal Units (BTUs), are simply units of energy. At least for the purposes of energy and weight gain, patients need to be reminded that “a Calorie is a Calorie is a Calorie” [9]. The same is true for the pejorative connotations for word “fat” including the myth that dietary fat converts directly to body fat unlike other sources of food energy. Psychoeducation that reviews the importance of dietary fat can be very helpful. For example, some essential fatty acids require consuming dietary fat and lipids are necessary for the absorption of fat-soluble vitamins, cellular membrane function, gene regulation, wiring between brain regions (see [55] for an excellent summary).
“Intuitive Eating”: The structured eating plan we advocate sharply contrasts with the intuitive or mindful approaches to eating that emphasizes learning to eat in response to physiological cues rather than situational or emotional cues [56,57]. Intuitive eating is considered to have three central features: 1) unconditional permission to eat when hungry and what food is desired; 2) eating for physical rather than emotional reasons; and, 3) reliance on internal hunger and satiety cues to determine when and how much to eat [57]. It rests on the assumption that greater attention to hunger and satiety cues are sufficient to override the profound physiological disturbance created by severe or prolonged weight suppression and chaotic eating. We believe that intuitive eating is a very constructive approach for chronic dieters who may have mildly disordered eating and weight preoccupation. It is the cornerstone of the progressive approach to size acceptance as an alternative to traditional weight loss programs [58,59]. Moreover, it has been shown that in obese chronic dieters, this approach does not lead to weight gain in the long run and it is very helpful in improving the psychological functioning of those plagued by the pattern of oscillation between dieting and overeating [56]. However, given what we know about the profound disruption of internal cues that results with significant and sustained weight suppression (e.g. think again about the starvation volunteers), it is naïve to assume that simply exerting greater willpower and redirecting attention more sharply on internal cues are sufficient to correct the problem with those with serious AN. As indicated earlier, in BN, the magnitude of weight suppression can be as great as for AN but the premorbid weight is simply higher [60]. Therefore, it is our view that intuitive eating is a misguided approach to those with serious eating disorders. At least in the short run, structured eating provides a more effective framework for holding turbulent and unreliable physiological and psychological cues in check while the salubrious effects of nutritional rehabilitation take place. Patients report having attempted “intuitive eating” prior to seeking treatment but have been unsuccessful in their failed attempts to attend to unreliable cues for hunger/fullness and/or their emotional states which results in inconsistencies in gauging quantity and quality of food intake.
Types of Foodstuffs
At the beginning of treatment, most patients have little sense of what constitutes “normal” eating. They try to restrict food intake, delay eating and divide food into “good” and “bad” categories, and engage in a host of idiosyncratic food avoidance and weight-losing behaviors. It is common for patients to defend their food choices by suggesting that they are mere “preferences.” It is more likely that they feel compelled to make certain choices or engage in food-related “safety-seeking behaviors” due to extreme fear of weight gain or loss of control. Food choices are sometimes based on nutritional myths (e.g., “Calories from dietary fat are stored as body fat, in contrast to Calories from protein and carbohydrate, which are burned off”). Some behaviors represent extreme interpretations of otherwise sensible dietary guidelines. For example, limiting red meat, saturated fats, or sugar may be sensible for the general population; however, avoiding them because of an intense and irrational fear may be linked to eating disorder psychopathology rather than based on sound health recommendations. Even after considerable work has gone into refuting nutritional myths, patients are typically overwhelmed by intense anxiety elicited by certain foods and bodily sensations (e.g. fullness) that have become associated with feared consequences. Patients are anxious about the types of food they eat, the amounts they consume, the timing of meals and the sensations of fullness that they experience after consuming even meals of moderate size. Their worry and anxiety about eating is the stimulus driving compensatory behaviors. The most effective strategy to diminish intense foodrelated anxiety is repeated exposure to the food stimuli (quality and quantity) that elicit the anxiety. Exposure therapy is a cornerstone of our nutritional rehabilitation treatment plan. For exposure to be successful, patients need to be exposed to fear eliciting food stimuli, to be convinced that the dangers that they perceive to be associated with these foods are unwarranted.
To ensure that exposure is maximized during the phase of treatment where all meals are supervised, patients must select feared foods as part of their meal plan. They are typically allowed to select no more than three specific foods that they simply do not like (as opposed to foods that elicit fear because of their perceived or real caloric density). Since most patients fear dietary fat, in our program, meals consist of at least 25% dietary fat. Larger percentages of dietary fat are sometimes prescribed to: 1) reduce the volume of food for those who are prescribed a large number of Calories (3,000 or more); or 2) to reduce the percentage of carbohydrates because of heightened risk of refeeding syndrome or because they are diabetic; 3) to reduce hunger, and 4) to provide exposure to certain feared foods.
Our program rarely uses liquid supplements. High Calorie liquid supplements have been recommended in to promote weight gain with a smaller volume of food and to help patients who are struggling with satiety; however, they can also reinforce food avoidance and foster dependence on artificial food sources [11]. It has been our experience that some patients prefer liquid supplements because they permit avoidance of feared foods and negative feelings associated with eating. In these cases, it is important to emphasize that exposure and desensitization to a wide range of food items is central to overcoming eating fears and ultimately being able to regain personal control of eating and eat in a “normal” manner. For a very small minority of patients who are unable to complete meals early in treatment, we may temporarily use liquid supplements along with regular meals.
Microwavable frozen entrées
The technology that we have employed for more than 20 years relies heavily on commercially available frozen entrées. We realize that there are valid criticisms of the widespread use of commercially available frozen foods such as excessive sodium content and potentially unwanted ingredients. However, the use of microwavable foods is not being advocated as a lifestyle choice for the general public but rather as part of a simple, and effective remedial strategy that has proven helpful in assisting eating disorder patients in nutritional rehabilitation. Commercially available packaged foods have several distinct advantages over the traditional “cafeteria” dining used in most eating disorder programs.
1. Portion-size controlled: A significant advantage of microwavable frozen entrées is that the portions are predetermined eliminating the guesswork in determining portion size. The controlled portions and the precise measurements reduce fears of loss of control. It also helps patients estimate portion sizes and appropriate servings when they transition to a more flexible eating plan.
2. Calories and macronutrients are exact: The nutritional information on the package specifying Calories per serving and the grams of macronutrients (including dietary fat) are unambiguous. This minimizes debate about the number of Calories in meals since the content of each meal is printed on the package. Foods other than packaged (e.g. frozen vegetables, liquids, and other readily available foods) are also used but the portions are measured precisely and checked by staff trained in meal planning. If certain meals are not available, patients can easily switch one meal for another that is calorically equivalent underscoring the primacy of Calorie content over caloric connotation.
3. Technology can be transported home: One of the most important benefits of microwavable meals is that the methodology employed throughout treatment can be readily implemented with the same precision outside of treatment (weekend home visits) and after discharge. This means that the blueprint for eating is consistent throughout the course of treatment and after discharge. In contrast, some other approaches (such as using hospital-based meals) require the patient to adjust to an entirely new eating plan at discharge. We tell patients that relapse prevention in the eating domain starts on the first day of treatment and they can have confidence that what they learn in treatment can be deployed once they are discharged. Also, nutritional information is widely available for most foods in restaurants which allow patients to engage in more “normal” eating in social events.
4. Commercial health standards are high: Flash freezing and commercial packaging reduces risk of spoilage and rapid heating of frozen foods reduces leaching of water-soluble nutrients from microwavable foods. Studies have shown that the nutritional value of frozen fruits and vegetables are generally equal to or higher that their fresh counterparts [61,62]. The CDC estimates that each year 48 million Americans get sick, 128,000 are hospitalized and 3,000 die of food borne illness [63]. This risk is minimized in flash frozen meals.
5. Wide range of meal selection: The range of microwavable frozen entrées available maximizes the ability to individualize exposure to feared foods during the course of treatment. Schebendach and colleagues [64] found that energy density and diet diversity are predictive of weight maintenance in AN patients.
6. Cost-effective: In the treatment setting, microwavable foods reduce costs since kitchen staff and an expensive commercial kitchen are not required. The cost-savings can be reallocated to therapy staff or translated into more economical treatment.
7. Simple and efficient: Relying on commercially available microwavable frozen entrées makes meal preparation simple and efficient. All meals can be reduced to interchangeable Calories and this minimizes the amount of time immersed in meal preparation. The simplicity of planning meals reduces obsession ruminations surrounding meal planning and preparation.
8. Patients take responsibility for meal planning and preparation: Early in treatment, patients select meals with staff assistance and later take responsibility for planning and preparation of all meals.
Common objections to microwavable foods
Patients and families often raise objections regarding the use of microwavable foods. It is important to address these objections and to reiterate that this aspect of meal planning is not intended to be part of a permanent lifestyle change but rather is a plan that is effective in healing the greatest health risk currently facing the patient.
Objections that need to be countered:
1. Using microwavable foods teaches poor nutrition: This argument does not consider the context of the person trying to overcome a life-threatening eating disorder. A major impediment to eating is worry and uncertainty related to the effects of food on body weight. The goal of frozen entrées is not to achieve a theoretical ideal of “optimal nutrition” or to make a permanent lifestyle choice but rather it is part of a remedial strategy that is very effective in dealing with treatment and relapse. Also, this “mechanical eating plan” is efficient because it reduces the agonizing and time-consuming decision-making that can take away from discussing meaningful psychological topics. It is important to emphasize relative health risks by weighing the enormous dangers associated with an eating disorder versus the minor putative risks of microwavable or processed foods.
2. Patients will become accustomed to eating “unhealthy” foods: Concerns are sometimes expressed that people will become “addicted” to microwavable meals or develop enduring unhealthy eating habits because of exposure to these foods. Again, context is everything. What is “healthy” in one context may not necessarily apply in another. We sometimes use the analogy that chemotherapy would hardly be recommended to facilitate health for the general public but in the right context, it can be lifesaving. Once the person’s eating disorder has been resolved, we fully appreciate that there are a range of non-eating disordered eating styles that could be considered appropriate as the long-term goal.
3. Patients will become accustomed to eating large amounts of food: Similarly, it has been argued that the amount of food in nutritional rehabilitation should not exceed the amount that patients would ordinarily eat at their target body weight based on the theory that the exposure to greater amounts will lead to tolerance to overconsumption [65]. This ignores the fact that the nutritional setting conditions for those who are underweight or weight suppressed are entirely different than those who have acclimated to complete nutritional rehabilitation. In our experience, eating disorders endure the same gradual normalization of appetite and eating patterns months after weight restoration as described by the Keys Starvation Study volunteers. Exposure to feared foods does not mean that people will grow to like them anymore that exposure therapy for a germ phobic (e.g. putting their hands in the toilet bowl to eradicate their fear) would lead them to develop an affinity for germs once the exposure therapy is complete.
Spacing Eating
The structured approach to meal planning includes eating prescribed meals and snacks at set times spaced throughout the day [9]. Ideally, the plan should include three meals and one or two snacks spread evenly throughout the day. In general, eating disorder patients have difficulties starting and stopping eating. Many are fixated on myth-laden dieting rules or are highly ambivalent about when and how much to eat. Typical problematic patterns are skipping breakfast, delaying eating, or deciding that eating is not permissible past a certain time in the evening. These tendencies can be lessened by eating at specific pre-set times. In this way, the clock becomes a potent discriminative stimulus for initiating meals which makes delayed eating less likely. Eating at prearranged times, along with other elements of meal planning mentioned earlier are designed to operationally define “not dieting” since many patients are very confused about what this means in practical terms. As mentioned earlier, to encourage compliance, it is helpful to educate patients about the metabolic benefits of spacing eating throughout the day.
There are circumstances where we deviate from the three meals and two snacks plan. For example, we typically ask most patients who begin in our 7-hours-a-day Partial Hospitalization Program to consume all Calories within the program day which means that they temporarily refrain from eating breakfast and evening snack. The rationale is to increase the likelihood that all prescribed Calories are consumed early in treatment for underweight patients who are nutritionally compromised or those prone to chaotic eating. We explain that this should not be interpreted as punitive in any way but rather reflects our concern that it would be unfair to burden them with choices about how much to eat outside of therapeutic supervision so early in treatment. It is important to be able to assure patients that the number of Calories consumed need to be exact so adjustments can be made to ensure that neither too many nor too few Calories are being prescribed. Once patients feel confident in eating per the structured meal plan, a breakfast and evening snack are incorporated. Psychoeducational topics are emphasized that support eating at regular pre-determined times. These include the metabolic advantages of spreading meals out over the day including increasing thermogenesis, lipid profiles and peak insulin response [66]. Finally, eating according to the clock reduces the likelihood of binge eating or under eating in reaction to internal or external non-nutritional cues.
In sum, nutritional rehabilitation plans vary significantly between different eating disorder programs; however, it is noteworthy that the details of this aspect of treatment are rarely specified and there is even less written on the theoretical principles behind these approaches. Despite the lack of detail, different approaches to nutritional rehabilitation have been used successfully in different eating disorder treatment programs. Our approach to meal planning and nutritional rehabilitation was developed to add structure to the eating plan in a partial hospitalization treatment and has been extended to adolescent residential treatment. It can be easily explained and has high patient acceptance by patients at the end of treatment. Moreover, it has been shown to be effective in our settings [3]. We have found that these same principles apply equally well with outpatients even though the same level of rigidity and structure may not be required. Nevertheless, given the notable contrasts between these approaches, it would not be surprising to find that some patients would find one system more palatable or more effective than another. Comparing the relative effectiveness of different methods and matching effectiveness to patient variables would be a fruitful area for future research.
References
- Hart S, Franklin RC, Russell J, Abraham S. A review of feeding methods used in the treatment of anorexia nervosa. Journal of Eating Disorders. 2013; 1: 36.
- Garber AK, Sawyer SM, Golden NH, Guarda AS, Katzman DK, Kohn MR, et al. A systematic review of approaches to refeeding in patients with anorexia nervosa. International Journal of Eating Disorders. 2016; 49: 293-310.
- Garner DM, Desmond M, Desai J, Lockert J. The disconnect between treatment outcome data and reimbursement for the treatment of anorexia nervosa. International Journal of Physiatry. 2016; 2: 006.
- Garner DM, Bemis KM. A cognitive-behavioral approach to anorexia nervosa. Cognitive Therapy and Research. 1982; 6: 123-150.
- Garner D, Bemis K. Cognitive Therapy for Anorexia Nervosa. In: Garner DM, Garfinkel PE, eds. Handbook of Psychotherapy for Anorexia and Bulimia. New York, NY: Guildford Press; 1985:107-146.
- Garner DM, Davis R. Principles of Cognitive-Behavioral Therapy for Bulimia Nervosa. American Mental Health Counselors Association Journal. 1986; 8: 185-192.
- Garner DM, Rockert W, Davis R, Garner MV, Olmsted MP, Eagle M. Comparison of cognitive-behavioral and supportive-expressive therapy for bulimia nervosa. American Journal of Psychiatry. 1993; 150: 37-46.
- Garner DM, Vitousek K, Pike KM. Cognitive Behavioral Therapy for Anorexia Nervosa. In: Garfinkel DMGaPE, ed. Handbook of Treatment for Eating Disorders. New York: Guilford Press. 1997: 94-144.
- Garner DM, Rockert W, Olmsted MP, Johnson C, Coscina D. Psychoeducational principles in the treatment of bulimia and anorexia nervosa. In: Garfinkel DMGaPE, ed. Handbook of Psychotherapy for Anorexia Nervosa and Bulimia. New York: Guilford Press. 1985: 513-572.
- Garner D. Psychoeducational principles in treatment. In: Garner DM, Garfinkel PE, eds. Handbook of treatment for eating disorders (2nd ed.). New York, NY US: Guilford Press; 1997:147-177.
- Hart S, Franklin RC, Russell J, Abraham S. A review of feeding methods used in the treatment of anorexia nervosa. Journal of Eating Disorders. 2013; 1: 36.
- Marzola E, Nasser JA, Hashim SA, Shih PAB, Kaye WH. Nutritional rehabilitation in anorexia nervosa: review of the literature and implications for treatment. Bmc Psychiatry. 2013; 13.
- Brunzell C, Hendrickson-Nelson M. Nutrition Counseling. In: Mitchell JE, ed. The Outpatient Treatment of Eating Disorders: A Guide for Therapists, Dietitians, and Physicians. Minneapolis, MN: University of Minnesota Press. 2001: 242-278.
- Baran SA, Weltzin TE, Kaye WH. Low discharge weight and outcome in anorexia nervosa. American Journal of Psychiatry. 1995; 152: 1070-1072.
- Bean P, Loomis CC, Timmel P, Hallinan P, Moore S, Mammel J, et al. Outcome variables for anorexic males and females one year after discharge from residential treatment. J Addict Dis. 2004; 23: 83-94.
- Castro-Fornieles J, Casula V, Saura B, Martinez E, Lazaro L, Vila M, et al. Predictors of weight maintenance after hospital discharge in adolescent anorexia nervosa. Int J Eat Disord. 2007; 40: 129-135.
- Commerford MC, Licinio J, Halmi KA. Guidelines for discharging eating disorder inpatients. Eating Disorders. 1997; 5: 69-74.
- Bessesen DH, Bull S, Cornier MA. Trafficking of dietary fat and resistance to obesity. Physiology & Behavior. 2008; 94: 681-688.
- Steinhausen H-C. The outcome of anorexia nervosa in the 20th century. The American journal of psychiatry. 2002; 159: 1284-1293.
- Steinhausen HC. Outcome of eating disorders. Child Adolesc Psychiatr Clin N Am. 2009; 18: 225-242.
- Agras WS. The consequences and costs of the eating disorders. Psychiatric Clinics of North America. 2001; 24: 371-379.
- Steinhausen HC, Grigoroiu-Serbanescu M, Boyadjieva S, Neumarker KJ, Metzke CW. The relevance of body weight in the medium-term to long-term course of adolescent anorexia nervosa. Findings from a multisite study. Int J Eat Disord. 2009; 42: 19-25
- Wildes JE, Marcus MD. Weight suppression as a predictor of weight gain and response to intensive behavioral treatment in patients with anorexia nervosa. Behaviour Research and Therapy. 2012; 50: 266-274.
- Witt AA, Berkowitz SA, Gillberg C, Lowe MR, Råstam M, Wentz E. Weight suppression and body mass index interact to predict long-term weight outcomes in adolescent-onset anorexia nervosa. Journal of Consulting and Clinical Psychology. 2014; 82: 1207-1211.
- Konrad KK, Carels RA, Garner DM. Metabolic and psychological changes during refeeding in anorexia nervosa. Eat Weight Disord. 2007; 12: 20-26.
- Garner DM. Eating Disorder Inventory (EDI-3) Professional Manual. Odessa, FL: Psychological Assessment Resources. 2004.
- Eddy KT, Dorer DL, Franko DL, Tahilani K, Thompson-Brenner H, Herzog DB. Diagnostic crossover in anorexia nervosa and bulimia nervosa: Implications for DSM-V. American Journal of Psychiatry. 2008; 165: 245-250.
- Keys A, Brozek J, Henschel A, Mickelsen O, Taylor HL. The Biology of Human Starvation (2 volumes). St. Paul, MN: University of Minnesota Press. 1950.
- Garner D. The effects of starvation on behavior: implications for dieting and eating disorders. Healthy Weight J. 1998; 21: 68-72.
- Vandereycken W. Can Eating Disorders Become ‘Contagious’ in Group Therapy and Specialized Inpatient Care? European Eating Disorders Review. 2011; 19: 289-295.
- Garber AK, Michihata N, Hetnal K, Shafer MA, Moscicki AB. A Prospective Examination of Weight Gain in Hospitalized Adolescents with Anorexia Nervosa on a Recommended Refeeding Protocol. Journal of Adolescent Health. 2012; 50: 24-29.
- Redgrave GW, Coughlin JW, Schreyer CC, Martin LM, Leonpacher AK, Seide M, et al. Refeeding and weight restoration outcomes in anorexia nervosa: Challenging current guidelines. International Journal of Eating Disorders. 2015; 48: 866-873.
- Smith K, Lesser J, Brandenburg B, Lesser A, Cici J, Juenneman R, et al. Outcomes of an inpatient refeeding protocol in youth with Anorexia Nervosa and atypical Anorexia Nervosa at Children’s Hospitals and Clinics of Minnesota. Journal of Eating Disorders. 2016; 4: 35.
- Maginot TR, Kumar MM, Shiels J, Kaye W, Rhee KE. Outcomes of an inpatient refeeding protocol in youth with anorexia nervosa: Rady Children’s Hospital San Diego/University of California, San Diego. Journal of Eating Disorders. 2017; 5: 1.
- Castro J, Deulofeu R, Gila A, Puig J, Toro J. Persistence of nutritional deficiencies after short-term weight recovery in adolescents with anorexia nervosa. International Journal of Eating Disorders. 2004; 35: 169-178.
- Lund BC, Hernandez ER, Yates WR, Mitchell JR, McKee PA, Johnson CL. Rate of inpatient weight restoration predicts outcome in anorexia nervosa. Int J Eat Disord. 2009; 42: 301-305.
- Khan L, Ahmed J, Khan S, MacFie J. Refeeding Syndrome: A Literature Review. Gastroenterology Research and Practice. 2011; 2011.
- Sunday SR, Hahmi KA. Energy intake and body composition in anorexia and bulimia nervosa. Physiology & Behavior. 2003; 78: 11-17.
- Walker J, Roberts SL, Halmi KA, Goldberg SC. Caloric requirements for weight gain in anorexia nervosa. American Journal of Clinical Nutrition. 1979; 32: 1397-1400.
- Stordy BJ, Marks V, Kalucy RS, Crisp AH. Weight gain, thermic effect of glucose and resting metabolic rate during recovery from anorexia nervosa. American Journal of Clinical Nutrition. 1977; 30: 138-146.
- George V, Tremblay A, Despres J, Landry M, Allard L, Leblanc C, et al. Further evidence for the presence of” small eaters” and” large eaters” among women. The American journal of clinical nutrition. 1991; 53: 425-429.
- Kaye W, Gwirtsman H, Obarzanek E, George DT. Relative importance of caloric intake needed to gain weight and level of physical activity in anorexia nervosa. American Journal of clinical nutrition. 1988.
- Fairburn C. Cognitive-behavioral treatment for bulimia. In: Garfinkel DMGPE, ed. Handbook of Psychotherapy for Anorexia Nervosa and Bulimia. New York: Guilford Press; 1985: 160-192.
- Garner D, Olmsted M, Garfinkel P. Similarities among bulimic groups selected by different weights and weight histories. J Psychiatr Res. 1985; 19: 129-134.
- Garner DM, Fairburn CG. Relationship between anorexia nervosa and bulimia nervosa: Diagnostic implications. Garner DM, Garfinkel PE, editors. In: Diagnostic issues in anorexia nervosa and bulimia nervosa. New York: Brunner/Mazel; 1988: 56-79.
- Russell G. Bulimia nervosa- ominous variant of anorexia nervosa. Psychological Medicine. 1979; 9: 429-488.
- Butryn ML, Juarascio A, Lowe MR. The Relation of Weight Suppression and BMI to Bulimic Symptoms. International Journal of Eating Disorders. 2011; 44: 612-617.
- Carter FA, McIntosh VVW, Joyce PR, Bulik CM. Weight Suppression Predicts Weight Gain Over Treatment but Not Treatment Completion or Outcome in Bulimia Nervosa. Journal of Abnormal Psychology. 2008; 117: 936-940.
- Butryn ML. Weight suppression is a robust predictor of outcome in the cognitive-behavioral treatment of bulimia nervosa. J Abnorm Psychol. 2006; 115: 62-67.
- Lowe MR, Berner LA, Swanson SA, Clark VL, Eddy KT, Franko DL, et al. Weight Suppression Predicts Time to Remission From Bulimia Nervosa. Journal of Consulting and Clinical Psychology. 2011; 79: 772-776.
- Zunker C, Crosby RD, Mitchell JE, Wonderlich SA, Peterson CB, Crow SJ. Weight Suppression as a Predictor Variable in Treatment Trials of Bulimia Nervosa and Binge Eating Disorder. International Journal of Eating Disorders. 2011; 44: 727-730.
- Keijer J, Hoevenaars FPM, Nieuwenhuizen A, van Schothorst EM. Nutrigenomics of Body Weight Regulation: A Rationale for Careful Dissection of Individual Contributors. Nutrients. 2014; 6: 4531-4551.
- Reiter CS, Graves L. Nutrition Therapy for Eating Disorders. Nutrition in Clinical Practice. 2010; 25: 122-136.
- Wheeler ML, Franz M, Barrier P, Holler H, Cronmiller N, Delahanty LM. Macronutrient and Energy Database for the 1995 Exchange Lists for Meal Planning. Journal of the American Dietetic Association. 1996; 96: 1167-1171.
- Marzola E, Nasser JA, Hashim SA, Shih PA, Kaye WH. Nutritional rehabilitation in anorexia nervosa: review of the literature and implications for treatment. Bmc Psychiatry. 2013; 13.
- Bacon L, Stern J, Van Loan M, Keim N. Size acceptance and intuitive eating improve health for obese, female chronic dieters. J Am Diet Assoc. 2005; 105: 929-936.
- Tylka TL, Wilcox JA. Are intuitive eating and eating disorder symptomatology opposite poles of the same construct? Journal of Counseling Psychology. 2006; 53: 474-485.
- Bacon L, Aphramor L. Weight Science: Evaluating the Evidence for a Paradigm Shift. Nutrition Journal. 2011; 10: 9.
- Bacon L, Stern JS, Van Loan MD, Keim NL. Size acceptance and intuitive eating improve health for obese, female chronic dieters. Journal of the American Dietetic Association. 2005; 105: 929-936.
- Garner DM. Cognitive therapy for bulimia nervosa. Adolesc Psychiatry. 1986; 13: 358-390.
- Bouzari A, Holstege D, Barrett DM. Mineral, fiber, and total phenolic retention in eight fruits and vegetables: A comparison of refrigerated and frozen storage. Journal of Agricultural and Food Chemistry. 2015; 63: 951-956.
- Bouzari A, Holstege D, Barrett DM. Vitamin Retention in Eight Fruits and Vegetables: A Comparison of Refrigerated and Frozen Storage. Journal of Agricultural and Food Chemistry. 2015; 63: 957-962.
- Gould L, Walsh KA, Vieira AR, Herman K, Williams IT, Hall AJ, et al. Surveillance for Foodborne Disease Outbreaks - United States, 1998-2008. Atlanta: Centers for Disease Control and Prevention. 2013: 1-38.
- Schebendach J, Mayer LES, Devlin MJ, Attia E, Walsh BT. Dietary energy density and diet variety as risk factors for relapse in anorexia nervosa: A replication. International Journal of Eating Disorders. 2012; 45: 79-84.
- APA. American Psychiatric Association Practice Guidelines for the Treatment of Patients with Eating Disorders. New York: American Psychiatric Association. 2006.
- Farshchi HR, Taylor MA, Macdonald IA. Beneficial metabolic effects of regular meal frequency on dietary thermogenesis, insulin sensitivity, and fasting lipid profiles in healthy obese women. The American journal of clinical nutrition. 2005; 81: 16-24.