
Clinical Image
Ann Obes Disord. 2016;1(3): 1015.
Endoscopic Diagnosis of Gastric Fold Herniation
Tai CM1,2, Tsai MS2,3 and Yu ML4,5,6,7*
¹Department of Internal Medicine, I-Shou University, Taiwan
²Department of Bariatric and Metabolic Surgery Center, I-Shou University, Taiwan
³Department of Surgery, I-Shou University, Kaohsiung, Taiwan
4Institute of Clinical Medicine, Kaohsiung Medical University, Taiwan
5Department of Internal Medicine and Hepatitis Center, Kaohsiung Medical University Hospital, Taiwan
6Institute of Internal Medicine, Kaohsiung Medical University, Taiwan
7Institute of Biomedical Sciences, National Sun Yat-Sen University, Taiwan
*Corresponding author: Ming-Lung Yu, Department of Internal Medicine, Kaohsiung Medical University Hospital, Hepatobiliary Division, 100 Tzyou Road, Kaohsiung City 807, Taiwan
Received: October 17, 2016; Accepted: October 20, 2016; Published: October 24, 2016
Clinical Image
A 40-year-old male underwent Laparoscopic Adjustable Gastric Banded Plication (LAGBP) for morbid obesity 4 years ago. He reported having upper abdominal pain for the past 2 months, and had mild tenderness to palpation in the epigastric area. Esophagogastroduodenoscopy disclosed a 0.6-cm hole on the plicated fold at the gastric fundus (Figure 1A). One large pouch with visible gastric folds was found behind the hole. The mucosa of the pouch was congested (Figure 1B).
Abdominal computed tomography revealed a herniated pouch with a thin gastric wall at the fundus (Figure 2). Laparoscopy revealed gastric fold herniation with congested gastric wall. The plication sutures were released, and the patient’s symptoms subsided. Gastric Fold Herniation (GFH) is one of the most serious complications after LAGBP and reoperation is usually needed [1,2]. Gastric necrosis requires resection, but deplication of the folds could relieve the symptoms if the herniated folds are only congested [3].
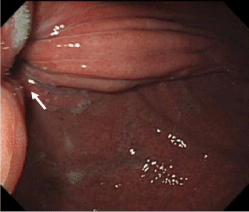
Figure 1A: 0.6-cm hole on the plicated fold at the gastric fundus.
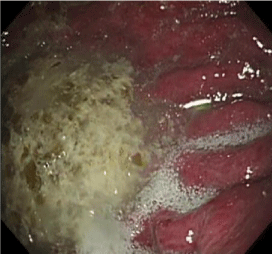
Figure 1B: One large pouch with visible gastric folds.
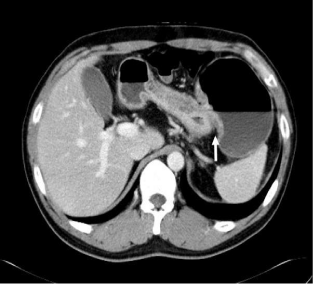
Figure 2: Herniated pouch with a thin gastric wall at the fundus.
References
- Tai CM, Chang PC, Huang CK. An unusual cause of vomiting after bariatric surgery. Gas-troenterology. 2013; 144: e1-2.
- Chang PC, Dev A, Katakwar A, Hsin MC, Tai CM, Huang CK. Management of gastric fold herniation after laparos-copic adjustable gastric banded plication: a single-center experience. Surg Obes Relat Dis. 2016; 12: 849-855.
- Goel R, Chang PC, Huang CK. Reversal of gastric plication after laparoscopic adjustable gastric banded plication. Surg Obes Relat Dis. 2013; 9: e14-15.