Case Report
Austin Oncol Case Rep. 2016; 1(1): 1003.
Refractory Hypoglycemia in T-Cell Lymphoma
Buyukaydina B¹*, Tunca M¹, Alayb M², Kazanciogluc R³ and Reha E³
¹Bezmialem Vakif University, Department of Internal Medicine, Turkey
²Yuzuncu Yil University, Department of Endocrinology, Turkey
³Bezmialem Vakif University, Department of Nephology, Turkey
*Corresponding author: Banu Buyukaydin, Bezmialem Vakif University, Department of Internal Medicine, Turkey
Received: June 01, 2016; Accepted: July 10, 2016; Published: July 13, 2016
Abstract
Hypoglycemia is commonly seen in diabetes mellitus patients; whereas it is rarely seen in a healthy person. In this case, we reported a male patient with a treatment-resistant hypoglycemia. A 53 years old male patient admitted to our clinic with debility, nausea and vomiting. Physical examination revealed lymphadenopathies in the left axilla and inguinal regions; and presence of right upper quadrant tenderness. Biochemical results revealed severe hypoglycemia, azotemia and elevation of liver enzymes. Histological result of the excisional lymph node biopsy was compatible with peripheral T cell lymphoma. In ward, the patient has repeated recurrent hypoglycemia, which did not resolve with all treatment given. His general condition deteriorated and he died due to sepsis. This case highlighted the need to rule out hematologic malignancies; precisely T-cell lymphoma in a patient who presented with resistant hypoglycemia in the presence of lymphadenopathy.
Keywords: Hypoglycemia, Lymphoma, IGF-II
Introduction
Hypoglycemia is defined as the occurrence of a variety of symptoms in association with plasma glucose concentration of 50mg/dl or less. Oral or parenteral glucose replacement is generally sufficient to provide normal levels. But in patients with resistance to this treatment, refractory hypoglycemia is mentioned.
Peripheral T-cell lymphoma is an aggressive Non-Hodgkin lymphoma that develops from T-cells in different stages of maturity and generally effects people over 60 years of age [1].
We presented a male patient followed with refractory hypoglycemia and finally diagnosed as T-cell lymphoma.
Case Presentation
A 53 years old male patient with an unknown medical illness presented with lethargy, debility, nausea and vomiting for two weeks. He was nonsmoker; never consumed alcohol and never had use addictive drug. Clinical examination was unremarkable except for multiple lymph node enlargement at the axillary and inguinal area; and presence of tenderness at the right upper quadrant of the abdomen.
The patients’ initial laboratory results are presented in (Table 1).
Laboratory Parameters
Results
Normal Range
Glucose
26
70-110 mg/dl
Sodium
135
135-148 mmol/L
Potassium
4.2
3.5-5.5 mmol/L
BUN
42
5-23 mg/dl
Creatinine
2.86
0.6-1.2 mg/dl
Uric Acid
14.1
2.4-5.7 mg/dl
ALT
175
0-55 U/L
AST
665
5-35 U/L
GGT
502
9-36 U/L
ALP
959
40-150 U/L
Total Protein
4.6
6-8.7 g/dl
Albumin
2.6
3.5-5.0 g/dl
Leukocyte
20540
4000-11000/mm3
Hb / Hct
14/41
11.5-16 g/dl /34-45 %
Trombocytes
203000
150000-450000 /mm3
Erythrocyte Sedimentation ra
6
0-20 mm/hr
Table 1: Biochemical results of patient with normal ranges.
He was hospitalized with the diagnosis of acute cholangitis and pre-renal azotemia. His thoracic and abdominal CT-scan showed bilateral pleural effusion and hepatomegaly. Endoscopic ultrasonography showed the presence of lymph nodes in portal hilum diameter up to 4cm.
In ward, he was noted to have serious refractory hypoglycemia episodes repeated despite the continuous dextrose infusion. The plasma glucose follow-up is presented in (Figure 1). Plasma insulin, c-peptide, cortisol and glucagon levels were all within normal range.
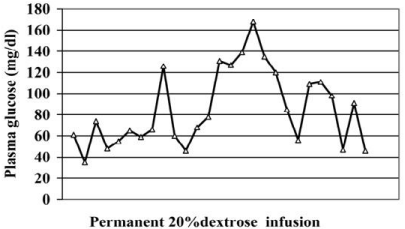
Figure 1: Plasma insulin, c-peptide, cortisol and glucagon levels were all
within the normal range.
An external biopsy of axillary lymph node showed a few small and mature looking T lymphocytes with cellular infiltration of approximately fifty percent of proliferation index. CD3 was positive. This finding was compatible to histological diagnosis of peripheral T-cell lymphoma with partial involvement of lymph ganglia.
While in ward patient had hypoglycemic attacks despite the continuous glucose infusion. The general condition worsened because of sepsis in the intensive care unit and the patient died due to septicemia. Additional investigation in terms of refractory hypoglycemia was not performed because of worsening general condition.
Discussion
Hypoglycemia is defined as the plasma glucose concentration of 50mg/dl or less and is a common complication in patients with diabetes, especially in these using sulfonylureas, meglitinides or insulin [2]. In patients without diabetes, the most common reason is drugs and Salicylates, Quinine, Pentamidine, Quinolone Antibiotics (Gatifloxacin), Disopyramide, inhibitors of angiotensin converting enzyme and beta blockers are generally responsible [3]. Other common disorders are malnourishment, endocrine disorders like insulinoma and cortisol deficiency, critical illnesses like chronic kidney disease, severe liver failure, mechanic ventilation, sepsis and septic shock [4]. Hypoglycemia usually responds to glucose infusion. If hypoglycemia does not respond to glucose infusion, it is life threatening and is called as refractory.
A possible cause of refractory hypoglycemia is a non islet cell tumor. In this type of hypoglycemia, tumoral secretion of incompletely processed insulin like growth factor-II (IGF-II), particularly in skeletal muscle, results in stimulation of insulin receptors and increases glucose utilization [5]. Other potential mechanisms include auto antibodies against insulin or insulin receptor and destruction of the liver or adrenal glands because of tumor burden. This type of hypoglycemia occurs in patients with fibromas, mesenchymal tumors, hepatocellular and colorectal carcinomas, myelomas and lymphomas [6,7].
Hypoglycemia is a rare presentation in multiple categories of B- and T-cell lymphoma. The patients’ presentation includes lactic acidosis and severe hypoglycemia [8,9]. The pathogenesis were overproduction of IGF-II. Another explanation for hypoglycemia and lactic acidosis in these cases; cancer cells favor aerobic glycolysis and produce the same amount of energy similar to normal cells; thus, more glucose shunted away from normal to cancer cells. This mechanism also uses amino acid, nucleotides and lipids as substrate and facilitate cell growth, proliferation and angiogenesis [10,11]. Aggressive glucose infusion, increase lactate production of tumor instead of serum glucose elevation. Metabolic improvement can be rectified by initiation of chemotherapy [12]. This pathogenetic process was probably responsible for our patients’ refractory hypoglycemia.
Peripheral T-cell lymphoma is a heterogeneous group of predominantly nodal T-cell lymphomas derived from various types of mature T-cells. The median age at diagnosis is 60 years and most patients presented with generalized lymphadenopathy. Hepatosplenomegaly, bone marrow, liver and spleen infiltration and leukemic transformations are seen in different percentages [13]. Diagnosis is based of tissue biopsy and sometimes lymph node biopsy. İmmunophenotype evaluation is essential. T-cell associated antigens are variably expressed for CD2, CD3, CD5 and CD7.
There is no general consensus regarding the preferred induction chemotherapy for peripheral T-cell lymphoma. CHOP (cyclophosphamide, doxorubicin, vincristine, and prednisone) with or without etoposide and EPOCH (etoposide, prednisone, vincristine, cyclophosphamide, doxorubicin) is among major treatment strategies [14]. Autologous hematopoietic cell transplantation is beneficial for patients in first complete remission. The role of radiotherapy remains undefined except for extranodal NK/T cell lymphoma. The clinical course of the disease is aggressive, and relapses are common.
In patients with non islet cell tumor presented with hypoglycemia, immediate correction and prevention of recurrent hypoglycemia is mandatory. But main treatment should focus for underlying malignancy. Difficult refractory hypoglycemia is controlled with glucocorticoids, diazoxide or glucagon [15,16].
Conclusion
Hematological malignancy causing hypoglycemia is a rare manifestation and partly understood. It has been associated with a high mortality rate. A patient who had profound or resistant hypoglycemia, a diagnosis of possible hematologic malignancy should be considered.
References
- William R. Macon. Peripheral T-Cell Lymphomas. Hematology/Oncology Clinics of North America. 2009; 23: 829-842.
- Barendse S, Singh H, Frier BM, Speight J. The impact of hypoglycemia on quality of life and related patient-reported outcomes in Type-2 diabetes. Diabet Med. 2012; 29: 293-302.
- Ogimoto A, Hamada M, Saeki H, Hiasa G, Ohtsuka T, Hashida H et al. Hypoglycemic syncope induced by a combination of cibenzoline and angiotensin converting enzyme inhibitor. Jpn Heart J. 2002; 42: 255-259.
- White BP, Southwood R. Persistent hypoglycemia of unknown etiology in a patient without diabetes: a case report and review. J Pharm Pract. 2013; 26: 138-143.
- Phillips LS, Robertson DG. Insulin-like growth factors and non-islet cell tumor hypoglycemia. Metabolism. 1993; 42: 1093-1101.
- Ma RC, Tong PC, Chan JC, Cockram CS, Chan MH. A 67-year-old woman with recurrent hypoglycemia: Non-islet cell tumour hypoglycemia. CMAJ. 2005; 173: 359-361.
- Di Comite G, Dagna L, Piatti PM, Monti LD, Tantardini F, Praderio L. Hypoglycaemia and lactic acidosis in a MALT non Hodgkin’s lymphoma. Leuk Lymphoma. 2002; 43: 1341-1342.
- Juffermans NP, Rijneveld AW, Zweegman S, Spijkstra JJ. Two patients with lactic acidosis and hypoglycaemia as initial presentation of a lymphoma. Ned Tijdschr Geneeskd. 2006; 150: 2770-2773.
- He YF, Wei W, Sun ZM, Ji CS, Wang G, Chen MP, et all. Fatal lactic acidosis and hypoglycemia in a patient with relapsed natural killer/T-cell lymphoma. Adv Ther. 2007; 24: 505-509.
- Vander Heiden MG, Cantley LC, Thompson CB. Understanding the Warburg effect: the metabolic requirements of cell proliferation. Science. 2009; 324:1029-1033.
- Végran F, Boidot R, Michiels C, Sonveaux P, Feron O. Lactate influx through the endothelial cell monocarboxylate transporter MCT1 supports an NF-κB/ IL-8 pathway that drives tumor angiogenesis. Cancer Res. 2011; 7: 2550- 2560.
- Elhomsy GC, Eranki V, Albert SG, Fesler MJ, Parker SM, Michael AG, et all. Hyper-warburgism,” a cause of asymptomatic hypoglycemia with lactic acidosis in a patient with non-Hodgkin’s lymphoma. J Clin Endocrinol Metab. 2012; 97: 4311-4316.
- Vose J, Armitage J, Weisenburger D. International T-Cell Lymphoma Project. International peripheral T-cell and natural killer/T-cell lymphoma study: pathology findings and clinical outcomes. J Clin Oncol. 2008; 26: 4124-4130.
- Schmitz N, Trümper L, Ziepert M, et al. Treatment and prognosis of mature T-cell and NK-cell lymphoma: an analysis of patients with T-cell lymphoma treated in studies of the German High-Grade Non-Hodgkin Lymphoma Study Group. Blood. 2010; 116: 3418-3425.
- Hoff AO, Vassilopoulou-Sellin R. The role of glucagon administration in the diagnosis and treatment of patients with tumor hypoglycemia. Cancer. 1998; 82: 1585-1592.
- Teale JD, Marks V. Glucocorticoid therapy suppresses abnormal secretion of big IGF-II by non-islet cell tumours inducing hypoglycaemia (NICTH). Clin Endocrinol. 1998; 49: 491-498.