
Research Article
Austin Oncol. 2016; 1(1): 1003.
Multidetector CT Virtual Cystoscopy in Gross Painless Hematuria
Kemal Arda¹*, Hasan Aydin² and Ahmet Hakan Haliloglu³
¹Ankara Ataturk Training and Research Hospital Department of Radiology, Bilkent Ankara, Turkey
²Ankara Oncology Hospital, Department of Radiology, Demetevler, Ankara Turkey
³Ufuk University Dept of Urology, Balgat Ankara Turkey
*Corresponding author: Kemal Arda, Ankara Ataturk Training and Research Hospital Department of Radiology, Bilkent Ankara, Turkey
Received: December 09, 2015; Accepted: January 27, 2016; Published: January 29, 2016
Abstract
Purpose: The objective of this study was to investigate the diagnostic efficiency of Multidetector CT (MDCT) based virtual cystoscopy in the assessment of bladder tumors in gross, painless hematuria.
Materials and Methods: 30 patients (21 men, 9 women) with gross, painless hematuria who had not had recent diagnosis were included in this prospective study. MDCT based virtual cystoscopy was performed using 16-slice multidetector CT scanner in the supine and prone positions. After axial scanning, the axial images were assessed, followed by coronal, and sagittal multi planar reconstruction of the images. In addition, by using volume rendering technical algorithms shaded the surface display MDCT based virtual cystoscopy was performed. In the multiplanar and 3-Dimensional images obtained, the existence, localization, morphological features, environment invasion, adjacent lymph nodes, and if any metastases of the abdomen were assessed. Then, all patients underwent conventional cystoscopy examination as the gold standard.
Results: In 10 cases, 24 bladder masses were detected by MDCT based virtual cystoscopy whereas 23 lesions (ranged from 0.33-5.8 cm) were depicted by conventional cystoscopy. Eleven of the 24 bladder masses measured less than 1 cm in maximum diameter. At MDCT based virtual cystoscopy, one patient with poor bladder distention, and severe trabeculation was wrongly diagnosed as tumor. Histopathologic diagnoses of 18 of the 23 bladder masses were transitional cell carcinoma, one patient with four masses was mixed tumor (transitional cell carcinoma + squamous cell carcinoma), and one was adenocarcinoma. The sensitivity, the specificity, negative predictive value, and positive predictive value of MDCT based virtual cystoscopy for detecting bladder carcinoma were % 100, % 95,2, % 100, and % 95,6 respectively. In addition to bladder pathologies, renal or ureter calculi, kidney or ureter mass, kidney cysts and lympadenopathies were investigated.
Conclusion: MDCT based virtual cystoscopy in the assessment of the bladder tumors is a non- invasive method that can be used in gross painless hematuria.
Keywords: Bladder tumors; Virtual cystoscopy; Painless hematuria
Introduction
Gross, painless hematuria is the classical clinical sign of bladder malignancies [1-13]. The differential diagnosis of the hematuria frequently requires several imaging modalities [1]. Many imaging modalities such as Excretory-Urography (EU), ultrasonography, Computed Tomography (CT), retrograde ureterography, conventional cystoscopy, and ureteroscopy have been used in the evaluation of patients with hematuria [1]. Conventional cystoscopy is gold standard in the diagnosis, and plays a key role in follow-up of bladder malignancies. MDCT based virtual cystoscopy is new promising, alternative imaging technique for evaluation of bladder lesions that is noninvasive and has good patient acceptance [1-17]. The major limitation of the technique is the difficulty in depiction of small lesions.
CT may also be used for the diagnosis of the bladder disease, but the dome and the base of the bladder visualization are limited on the axial plane scanning. These areas can be easily evaluated in 3-Dimensional and multi planar reformatting images by using MDCT based virtual cystoscopy.
The objective of this study was to investigate the diagnostic efficiency of multidetector CT (MDCT) based virtual cystoscopy in the assessment of bladder tumors in gross, painless hematuria.
Materials and Methods
Patient population
Thirty patients (21 men, 9 women; age range 25-86 years; mean years ± SD, 54.7±17.4) presented with gross painless hematuria prospectively evaluated. They had been referred by the urology department for MDCT based virtual cystoscopy. The existence of haematuria was confirmed by urine analysis of each patients included the study. Patients who had kidney failure as determined by biochemical and urine analyses were excluded from the study. The study was approved by the hospital review board, and informed consent was obtained from all patients before the examination. All of the MDCT based virtual cystoscopic evaluations were performed before conventional cystoscopy and biopsy in order to avoid tumourlike lesions that could occur on bladder walls as a result of biopsy. The time interval between MDCT based virtual cystoscopy and conventional cystoscopy were less than 5 days.
CT technique
All CT examinations were performed with 16 slice Light speed CT scanner (GE Medical Systems, Milwaukee, Wis, USA), both in supine and prone positions with 120 kVp; section thickness of 1.25 mm; 0.5-second helical rotation time; and 250 mA.
Oral contrast material was not used. Unenhanced images were obtained from domes of the diaphragm to the symphysis pubis. One hundred milliliters of intravenous contrast media (Ioversol 350mgl/ Ml, Optiray, Covidien, Tyco, USA) was administered intravenously at a rate of 3mL/sec, with 60 second delay the nephrographic phase abdominopelvic contrast enhanced images were obtained. A 500 ml bag of normal saline solution was administered rapidly after the contrast material injection, to distend the urinary bladder. After bladder distention, before the virtual cystoscopic examination, all patients were asked to adopt supine and prone positions several times so that the contrast material and urine in the bladder could be adequately mixed to prevent sedimentation and fluid-fluid level of the contrast medium, and the urine in the bladder, and also to attenuate the entire bladder lumen homogeneously. After a scout view was obtained with the patient in the supine position to locate the bladder and confirm its adequate distention, single–breath-hold MDCT examination was performed both in supine and prone positions.
Source axial CT images were transferred to the workstation (AW 4.2 GE Medical Systems, Milwaukee, Wis, USA). MPR images 0.625 mm thick at 0.623 mm intervals were obtained in the transverse, coronal and sagittal planes to generate intraluminal views of the bladder. The time to generate these images was less than 60 seconds. Interactive endoscopic navigation using surface rendering algorithm were performed. During the interactive navigation the threshold values were manually adjusted for the pacification of the bladder. The lowest threshold level was determined as the highest value to differentiate the lumen from the wall or the mass on the axial images. The viewpoint of the observer was manipulated through 360 degrees in any axis to evaluate the internal surface of the bladder, especially the base of the bladder, which is difficult area for conventional cystoscopy.
Un-enhanced images thin-section obtained from the kidneys to the bladder demonstrate the dens opacification of the urinary tract.
Un-enhanced and reprographic-phase images were used for the characterization of the renal paranchimal abnormalities, particularly masses.
Source axial, MPR and MDCT based virtual images were prospectively interpreted, both separately and in combination, by two radiologists with 15 years and 4 years of experience in CT. These radiologists worked in concensus and were blinded to the results of conventional cystoscopy. The number, size, localization, and morphologic features of the lesions were studied. The bladder lesions were classified as polypoid, sessile, and areas of wall thickening. The time spent on study interpretation was approximately 10 minutes. The MDCT based virtual cystoscopy findings were compared with the conventional cystoscopy, which was considered as the gold standard. MDCT based virtual cystoscopy and conventional cystoscopy findings were correlated with histologic diagnosis.
Conventional cystoscopy
Conventional cystoscopy with a flexible cystoscope was performed on all patients, and biopsies of suspicious lesions were taken by urologist in the urology department. Techniques used for conventional cystoscopy included, in 24 patients, 2I F rigid cystoscopy (Karl Stor 2 Endoscope, Hopkins II, Berlin, Germany) with a 30º field of view. Number, location, size, morphology and pathologic findings of the lesions were studied.
Statistical analysis
Statistical analysis was performed according to the number of the lesions (not the number of patients) because each patient had one or multiple lesions. Using the conventional cystoscopic findings as the reference standard, the presence or absence of a bladder lesion at each site was evaluated on the MDCT based virtual cystoscopy together with multiplanar reconstruction images. We calculated the sensitivity, specificity, Positive Predictive Values (PPV), and Negative Predictive Values (NPV), and accuracy of virtual cystoscopy. NPV and PPV were calculated on a per patient basis: if at least one tumor per patient was detected on both virtual and conventional cystoscopy, the patient was counted as a true-positive. When tumors were not detected with either diagnostic method, we considered patients as true-negatives. If a tumor or tumor like lesion was detected by MDCT based virtual cystoscopy but not detected by conventional cystoscopy, the patient was counted as a false-positive.
Results
MDCT based virtual cystoscopy
The procedure was well tolerated by all patients and no complication was reported. Mixing of the contrast material and urine was adequate on the supine scan in all patients. The bladder distention was not adequate in one patient.
Renal or ureteral calculi were detected in 6 of the cases. One solid renal mass and 13 cystic renal masses were detected on CT examination. In these twenty patients MDCT based virtual cystoscopy and conventional cystoscopy examinations were normal.
Five patients had a single bladder lesion (Figure 1-3), two patients had two bladder lesions, and three patients had four or more lesions on MDCT based virtual cystoscopy evaluation.
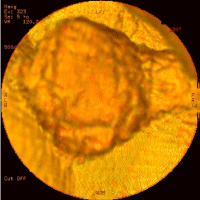
Figure 1: Surface rendering MDCT based virtual cystoscopy image
demonstrates polipoid mass.
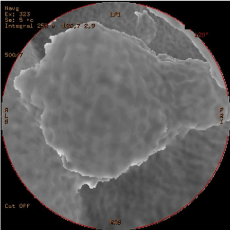
Figure 2: Integral MDCT based virtual cystoscopy image demonstrates same
polipoid mass.
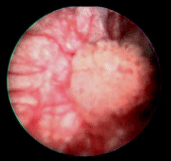
Figure 3: The lesion identified by convential cystoscopy.
MDCT based virtual cystoscopy showed 24 masses arising from the urinary bladder. The tumor diameters, location, and the morphology (pedinculated or sessile), and pathologic diagnosis of all 24 bladder masses were summarized at (Table 1). Nineteen masses were reported to have irregular surface and three of them were found to be smooth surfaced at MDCT based virtual cystoscopy.
N
Sex
Age
Virtual Cystoscopic Localization of the Mass
Virtual Cystoscopic Diameter of the Mass
Conventional Cystoscopic Diameter of the Mass
Pathologic Diagnosis of the Mass
1
M
80
Prostatic surface
18mm irregular surfaced polipoid mass
A 15mm diameter polipoid
Transitional cell carcinoma (TCC)
2
M
64
Prostatic surface
20 mm irregular surfaced polipoid mass
Cystoscopy was normal.
3
M
86
neck of the diverticula
at the anterior wall, at the left posterior wall, at the inferior wall of the bladder
an 18mm diameter irregular surfaced polipoid mass
a 5mm irregular surfaced polipoid mass,
a 20mm diameters mass,
a 5.2mm diameter irregular surfaced mass
A 20mm diameters polipoid mass,
a 5mm diameter polipoid mass,
a 20mm diameter polipoid mass,
3-4mm polipoid mass
TCC
4
M
60
inferior wall, at the right inferior wall, at the superior wall, at the left superior wall, at the right superior wall, the anterior wall
A 9mm diameter irregular surfaced mass,
a 46mm diameter irregular surfaced mass,
a 8.8mm diameter irregular surfaced mass,
a 25mm diameter irregular surfaced mass,
a 58mm diameter irregular surfaced mass,
The bladder wall thickening of was measured as 15mm.
A 8 mm polipoid mass,
45 mm polipoid mass,
9 mm diameter mass,
23 mm polipoid mass,
55 mm polipoid mass,
3mm flat wall lesion
TCC
5
M
72
at the left side
15mm and 31mm diameters irregular surfaced polipoid masses
15mm and 30mm diameter of polipoid masses
TCC
6
M
42
at the right superior wall
A 28mm diameter irregular surfaced polipoid mass
A 30mm diameter polipoid mass
TCC
7
M
69
at the bladder neck, at the left inferior wall, at the right side that originates outside the bladder, at the posterior wall, left bladder wall
A 20mm diameter irregular surfaced mass,
a 3.3mm diameter irregular surfaced mass,
a 45mm diameter smooth surfaced mass,
a 12mm diameter irregular surfaced polipoid mass,
4mm was irregular surfaced mass
a 20mm polipoid mass,
a 4mm polipoid mass,
A 40mm diameter polipoid mass,
A 15 mm polipoid mass
Multiple diffuse milimetric masses (appearance of carcinoma in situ).
mixed tumor (TCC + Squamous cell carcinoma)
8
F
86
at right posterior wall,
at the left superior wall
A 21mm diameter smooth surfaced mass,
a 22mm diameters irregular surfaced mass
A 20mm diameters polipoid mass,
a 20mm diameters polipoid mass
TCC
9
M
46
at the anterior wall
A 5mm diameters smooth surfaced polipoid mass
A 5mm diameter polipoid mass
TCC
10
F
49
at the superior wall
A 22mm diameter irregular surfaced polipoid mass
A 21mm diameter polipoid mass .
Adeno-carcinoma
Table 1: The MDCT based virtual cystoscopy, conventional cystoscopy and pathologic diagnosis of the urinary bladder masses.
The degree of the bladder trabeculation with virtual cystoscopy was mild in four patients, moderate in 8 patients, and severe in 12 patients.
Bladder diverticulas were detected in one patient at virtual cystoscopy and was confirmed at conventional cystoscopy.
There was no false negative patient in our series.
In one patient with poor bladder distention, and severe trabeculation, a 20 mm diameter irregular surfaced polipoid mass at prostatic surface of the bladder was detected at MDCT based virtual cystoscopy (Figure 4, 5) , but conventional cystoscopic examination of this patient was normal. This was the only false positive case at MDCT based virtual cystoscopy in our study. The histopathologic evaluation of this patient was normal.
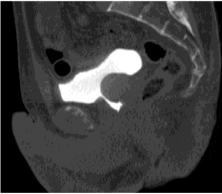
Figure 4: In patient with poor bladder distention, a 20 mm diameter irregular
surfaced polipoid mass at prostatic surface of the bladder is seen on sagittal
MDCT image.
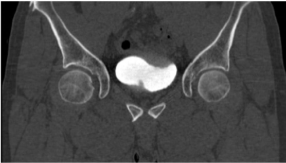
Figure 5: In one patient with poor bladder distention, severe trabeculation
of the anterior-superior wall of the urinary bladder, and a 20 mm diameter
irregular surfaced polipoid mass at prostatic surface of the bladder is seen on
coronal MDCT image.
As a result CT based virtual cystopy detected all 23 of the proved urinary bladder masses.
Conventional cystoscopy
A total of 23 bladder lesions in 10 of 30 patients (33,3%) were shown to have lesions at conventional cystoscopy. Among the patients with bladder lesions, 4 patients had a single bladder lesion, two patients had two lesions, and three patients had four or more lesions. The sum of tumor diameter in each bladder lesions ranged from 0.3 to 4 centimeters.
In pathologic evaluation, 18 of the 23 bladder masses were transitional cell carcinoma, one patient with four masses was mixed tumor (transitional cell carcinoma + squamous cell carcinoma), and one patient was adenocarcinoma.
The sensitivity, the specificity, negative predictive value, and positive predictive value of MDCT based virtual cystoscopy for detecting bladder carcinoma were %100, %95,2, %100, and %95,6 respectively.
Discussion
Differential diagnosis of hematuria frequently requires several imaging modalities such as excretory urography (EU), ultrasonography, CT, retrograde urethrography, pyelography, cystoscopy, and ureteroscopy have been used in the evaluation of gross painless hematuria [13]. There are more than 160 causes of hematuria, such as renal, ureteral or bladder calculi, renal masses, infection, trauma, drug toxicity, coagulopathy, urinary bladder carcinoma [13].
A single CT examination helps to perform a comprehensive evaluation of hematuria. Unenhanced CT images are ideal for detecting non-obstructing calculi. Renal masses frequently manifest with hematuria [1]. Unenhanced and reprographic phase CT imaging demonstrate and characterize renal masses accurately. CT imaging is excellent for differentiating renal cyst from neoplasm [1]. In addition, CT may directly demonstrate the impression on the collection system.
However gross, painless hematuria is the classical clinical sign of bladder malignancies, bladder abnormalities such as neoplasm, diverticula’s, and cystitis are the common causes of the hematuria (1,7,8,9,13). Bladder diseases could be evaluated with ultrasonography, CT or MR based virtual cystography, EU, or conventional cystoscopy (6,9).
Conventional cystosopy is the gold standard in the diagnosis of urinary bladder tumors [1,4,6,7,8,11,13,14].There are several disadvantages of conventional cystoscopy. While the conventional cystoscopic evaluation, the physician may miss tumors at the base and the neck of the urinary bladder due to the limited flexibility of the cystoscope near the the neck of the bladder, especially in males [15]. During the conventional cystoscopic evaluation the clinician has to distinguish tumors from surface deformations due to neighboring structures, due to the inability to show neighboring structures [15]. During conventional cystoscopy sedation is frequently necessary, and the procedure is invasive. An iatrogenic injury to bladder and the urethra may occur and urinary sepsis develops in 5%-10% of patients [11]. It is not easy to show the diverticula of the urinary bladder with conventional cystoscopy, and the luminal geometry within the diverticula’s cannot be evaluated by this technique.
Bladder is an appropriate site for MDCT based virtual imaging because of its simple luminal morphology, and the absence of involuntary peristalsis. Using CT based virtual cystoscopy have many advantages in the evaluation of bladder malignancies. First of all this technique is noninvasive, comfortable and easily acceptable imaging technique for evaluation of the urinary bladder with similar accuracy to conventional cystoscopy in the diagnosis of urinary bladder neoplasms larger than 0,5cm [3,9]. Sedation is not required. Virtual cystoscopy can be used for mapping luminal geometry of the urinary bladder with radiation doses as low as 0.48 mSievert [7]. In addition it can show neighboring structures, and local invasion [5,6,7,9]. Tumors within the bladder diverticula’s can be easily demonstrated by CT based virtual cystoscopy [8]. The viewpoint of the observer can be manipulated through 360 degrees in any axis to evaluate internal surface of the urinary bladder. Virtual cystoscopy offers valuable information about the location, the size, the depth of invasion of the tumor, the involvement of perivesical fatty tissue, and enlarged lymph nodes [3,9,10]. Urinary bladder distention is essential for optimal CT cystoscopic evaluation [9]. Flat bladder tumor detection is still the major limitation of CT based virtual cystoscopy. Also, MDCT based virtual cystoscopy gives no information about the color and texture of the bladder mucosa; therefore, it can not be used to detect carcinoma in situ. And It does not produce tissue for histopathologic evaluation.
Jaume et al reported an image processing algorithm in the detection of the urinary bladder tumors with CT scanning. This algorithm achieves 89% sensitivity and 88% specificity, 48% positive predictive value, and 98% negative predictive value [15]. In our study, we used contrast material filled urinary bladder for virtual cystoscopy. We performed virtual cystoscopy in addition to the contrastenhanced abdominopelvic CT examination. A satisfactory evaluation of the entire urinary tract was achieved by this examination. The axial images, reformatted sagittal-coronal-oblique MPR images and virtual images were interpreted together to increase the sensitivity and specificity of the examination. In this study there were no false negative cases. One of the patients with severe trabeculation of the urinary bladder wall was false positive on MDCT based virtual cystoscopy. Some researchers prefer to fill the bladder by air [16- 17], we preferred to fill the bladder by contrast media because we could evaluate the parenchymal organs in the same session. The results of this study suggest a high accuracy of CT imaging based virtual cystoscopy in the diagnosis of urinary bladder cancer. The positive predictive value of virtual cystoscopic evaluation was 90%. The negative predictive value of virtual cystoscopic evaluation was 100%. The spatial resolution of the virtual cystoscopy is comparable to that of conventional cystoscopy. As a result, MDCT based virtual cystoscopy in the assessment of the bladder tumors is a promising, non-invasive, diagnostic method that can be used in gross painless hematuria.
References
- Joffe SA, Servaes S, Okon S, Horowitz M. Multi-detector row CT urography in the evaluation of hematuria. Radiographics. 2003; 23: 1441-1455.
- Kundra V, Silverman PM. Imaging in oncology from the University of Texas M. D. Anderson Cancer Center. Imaging in the diagnosis, staging, and followup of cancer of the urinary bladder. AJR Am J Roentgenol. 2003; 180: 1045- 1054.
- Melissourgos Nikolas, Davilas Ilias, Liapis Dimitrios, Skrekas Thomas, Tromboukis Konstantinos, Lykourinas Michael. Comparison of virtual cystoscopy and conventional cystoscopy findings in patients with bladder cancer. European Urology 2002; 1: 49.
- Lämmle M, Beer A, Settles M, Hannig C, Schwaibold H, Drews C. Reliability of MR imaging-based virtual cystoscopy in the diagnosis of cancer of the urinary bladder. AJR Am J Roentgenol. 2002; 178: 1483-1488.
- Jeong Kon Kim, Soon-Youn Park, Ho Sung Kim, Soo Hyun Kim, Kyoung-Sik Cho. Comparison of virtual cystoscopy, multiplanar reformation, and source CT images with contrast material-filled bladder for detection lesions. AJR 2005; 185: 689-696.
- Kim JK, Ahn JH, Park T, Ahn HJ, Kim CS, Cho KS. Virtual cystoscopy of the contrast material-filled bladder in patients with gross hematuria. AJR Am J Roentgenol. 2002; 179: 763-768.
- Tsili ACh, Tsampoulas C, Chatziparaskevas N, Silakos A, Kalef-Ezra J, Sofikitis N, Efremidis SC. Computed tomographic virtual cystoscopy for the detection of urinary bladder neoplasms. Eur Urol. 2004; 46: 579-585.
- Halil Arslan, Kadir Ceylan, Mustafa Harman, Yüksel Yilmaz, Osman Temizoz, Saban Can. Virtaul Computed Tomography Cystoscopy in bladder pathologies. Int Braz J Urol. 2006; 32: 147-154.
- Julie H Song, Isaac R Francis, Joel F Platt, Richard H Cohan, Jamil Mohsin, Stephanie J Kielb, et al. Bladder tumor detection at virtual cystoscopy. Radiology 2001; 218: 95-100.
- Sarwat Hussian, Joyce A Loeffler, Richard K Babayan, Helen M Fenlon. Thin-section Helical Computed Tomography of the bladder: initial clinical experience with virtual reality imaging. Urology 1997; 50: 685-689.
- Fenlon HM, Bell TV, Ahari HK, Hussain S. Virtual cystoscopy: early clinical experience. Radiology. 1997; 205: 272-275.
- Roman F J Browne, Conor P Meehan, Jane Colville, Raymond Power, William C Torreggiani. Transitional cell carcinoma of the upper urinary tract: Spectrum of imaging findings. Radiographics 2005; 25: 1609-1627.
- Schreyer AG, Fielding JR, Warfield SK, Lee JH, Loughlin KR, Dumanli H, Jolesz FA. Virtual CT cystoscopy: color mapping of bladder wall thickness. Invest Radiol. 2000; 35: 331-334.
- Roy C, Merran S . [Imaging and pathology of bladder tumors]. J Radiol. 2002; 83: 843-859, discussion 861-2.
- Jaume S, Ferrant M, Macq B, Hoyte L, Fielding JR, Schreyer A, Kikinis R. Tumor detection in the bladder wall with a measurement of abnormal thickness in CT scans. IEEE Trans Biomed Eng. 2003; 50: 383-390.
- Abrol S, Jairath A, Ganpule S, Ganpule A, Mishra S, Sabnis R, Desai M. Can CT Virtual Cystoscopy Replace Conventional Cystoscopy in Early Detection of Bladder Cancer? Adv Urol. 2015; 2015: 926590.
- Gabr AH, Elbadry M, Elsherief A, Tawfiek ER. Computed tomography-virtual cystoscopy in the evaluation of a bladder mass: Could it replace standard conventional cystoscopy? Arab J Urol. 2013; 11: 369-374.