
Case Report
J Ophthalmol & Vis Sci. 2024; 9(2): 1094
Central Toxic Keratopathy Versus Diffuse Lamellar Keratitis: A Rare Misdiagnosed Complication Post Laser Assisted in Situ Keratomileusis
Dalal M1*; Khanna R2; Dabral H3; Anuradha A4; Verma M5; Karan A6
1Indira Gandhi Hospital, Dwarka, New Delhi, India
2Rockhampton Hospital, Queensland, Australia
3Bhagwan Mahavir Medica Super Speciality Hospital, Ranchi, India
4Bhagwan Mahavir Medica Super Speciality Hospital, Ranchi, India
5Vision Plus Eye care solutions, Ranchi, India
6Rajendra Institute of Medical Sciences, Ranchi, India
*Corresponding author: Dalal M, Indira Gandhi Hospital, H. No. 104 Block A Sector 19, Dwarka, New Delhi, India. Tel: 0 9540941507 Email: drmin27@gmail.com
Received: August 12, 2024 Accepted: August 28, 2024 Published: September 05, 2024
Abstract
A 26 years old patient underwent uneventful laser assisted in situ keratomileusis presented on 3rd day postoperatively with grade 2 diffuse lamellar keratitis, which progressed to grade 3 in spite of hourly topical and oral steroids. The patient underwent flap up-lift with interface wash. On subsequent follow-ups, scarring persisted with hyperopic shift in refraction. The revised diagnosis of CTK was made. We report this case to make LASIK surgeons aware of this serious complication and how to differentiate it from DLK. Furthermore, such single cases can make database for large scale analytical studies.
Keywords: LASIK; Central Toxic Keratopathy; Diffuse Lamellar Keratopathy
Abbreviations: LASIK: Laser Assisted in Situ Keratomileusis; DLK: Diffuse Lamellar Keratitis; CTK: Central Toxic Keratopathy; OU: Oculus Utrique; OD: Oculus Dexter; OS: Oculus Sinister; BCVA: Best Corrected Visual Acuity; PRK: Photorefractive Keratectomy; OCT: Optical Coherence Tomography.
Introduction
In recent times, the Laser Assisted in Situ Keratomileusis (LASIK) surgery has been simplified by the outstanding improvements in the technology. This corresponding ease to do surgery has made it to be the most performed surgery in the world. Hence with such high volume, complications are bound to occur. Central Toxic Keratopathy (CTK) is a recently described complication after LASIK surgery. The focus of this case report is to elaborate the difference between the two entities and also to make clinicians aware of this rare but serious post LASIK complication.
Case Report
A 26 years old male patient underwent simultaneous bilateral uneventful LASIK surgery at our centre. He presented on 3rd day postoperatively with mild pain and redness oculus utrique (OU). Best Corrected Visual Acuity (BCVA) was 20/30. The slit lamp examination revealed localized areas of stromal haze in central cornea OU with few stromal lines in left eye. (Figure 1) The anterior chamber was quiet and rest of examination was unremarkable OU. Automated refraction was OD + 1.50 DS/ -1.25DC X 14° and OS +2.00 DS/ 0.25DC X 175°. Presuming it to be grade 2 diffuse lamellar keratitis (DLK), the frequency of topical steroid was increased to one hourly. On next day examination, visual acuity further dropped to 20/50 OU with progression of DLK to grade 3 with more pronounced white granular central confluent infiltrates with striae. (Figure 2) Flap up-lift with interface wash OU was done. After wash, the VA improved to 20/30 OD and 20/50 OS improving with pinhole to 20/20(p) OD and 20/30 OS respectively. The haze reduced in both eyes with mild superficial punctate scarring OD and fine central scarring with stromal lines OS. Patient was followed up frequently up to 2 months with no further reduction in haze and scarring with hyperopic shift in refraction. (Figure 3) The revised diagnosis of Central Toxic Keratopathy (CTK) was made and topical steroids were tapered. Patient was counseled for course of CTK to be prolonged but self-limiting resolvable condition. However, the patient lost follow up after 6 months with last automated refraction of OD +0.50 D and OS + 1.50 D.
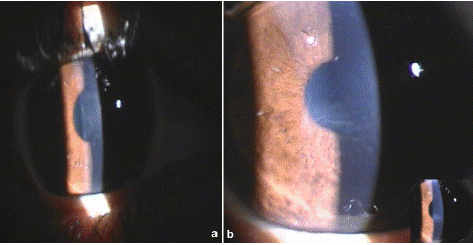
Figure 1: Right (a) and Left (b) eye at presentation post lasik.
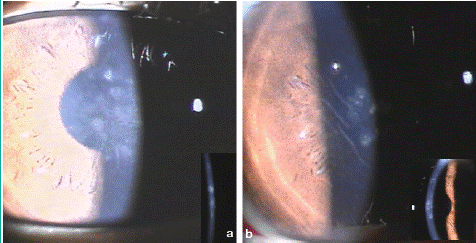
Figure 2: Grade 3 DLK noted bilaterally. (a) Right (b) Left.
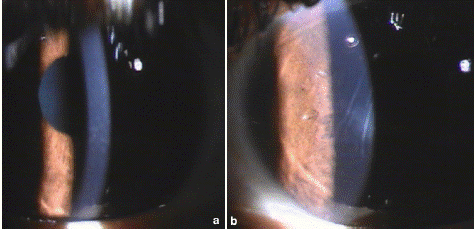
Figure 3: Status post 2 months. (a) Right (b) Left.
Discussion
Central toxic keratopathy is a rare, acute, non-inflammatory complication of LASIK surgery [1-3]. It was first described in 1989 by Fraenkel and colleagues. [4] It is characterized by central corneal opacification, striae and stromal tissue loss. This results in a hyperopic shift causing reduced quality of vision [1-3]. The incidence reported in the literature is only 0.0076-0.016% [5,6]. The etiology of CTK is uncertain and ambiguous. Hau and Allan and Hsu et al did confocal microscopy studies recently to study its cause and has described existence of keratocyte apoptosis in the affected central stromal matrix of CTK patients [7,8]. Other studies proposed hypersensitivity to tear film, toxic reaction due to laser photo-activation as possible causes [3,9].
The clinical appearance in CTK bears resemblance to many conditions like infectious keratitis, post Photorefractive Keratectomy (PRK) haze, corneal haze secondary to raised Intraocular Pressure (IOP) and DLK specifically grade 4 DLK. In Infectious keratitis, the corneal haze is associated with conjunctival congestion, anterior chamber reaction and presents with acute painful red eye [10,11]. CTK on contrary is non-inflammatory condition with quiet anterior chamber. The post PRK haze will have a positive history of PRK and not LASIK. The corneal haze secondary to raised IOP can easily be differentiated by IOP being normal in CTK. The most challenging is to differentiate CTK from grade 4 DLK. Both leads to reduction in corneal clarity with striae with hyperopic shift in early post-operative period. However, in CTK the signs typically begin on post-operative day 3-6. Whereas, in DLK, findings appear on very first day itself [1,4,6].
In CTK classic findings are central and extends anteriorly or posteriorly from the interface involving stroma. Whereas in DLK, the lesions are characteristically peripheral initially and gradually transform into central grade 3 and grade 4 over the course of 3-5 weeks and are limited upto interface [3,4,10,11]. Also, DLK being inflammatory processes presents with chamber reaction, conjunctival hyperemia or ciliary flush which CTK rarely exhibits being a non-inflammatory process [4]. The other differentiating feature is their course of disease. DLK is known to resolve within 5-8 days while CTK can persist for up to 18 months before spontaneously resolving [1,3,12].
Scheimpflug imaging highlights the exaggerated flattening of the anterior cornea that commonly accompanies CTK. Likewise, OCT images of eyes affected with CTK will characteristically show central corneal thinning and backscattering and a higher internal reflectivity [10,11]. As for the role of topical steroids, the recent confocal studies have suggested it to be a non-inflammatory condition. Hence, experts question the use of topical steroids for long which would only increase the morbidity by exposing the eye to risk of steroid induced cataract and glaucoma [8,9,11,12].
Sonmez et al and Moshirfar et al, suggest reserving an empirical topical corticosteroid therapy until a definitive diagnosis is made [1,3,10]. Because, if a patient had DLK and was misdiagnosed as having CTK, the failure to administer topical corticosteroids early in the development of DLK could have potentially disastrous consequences on the patient's vision. In our case, we chose to continue topical steroids beyond 1 month and then gradually tapered off.
Conclusion
CTK being a rare complication and often confused with DLK, is very less reported. Therefore, no accepted consensus exists both in terms of accurately identifying CTK & best management practices for the condition. Furthermore, the ambiguity whether or not CTK exists as a distinct entity or it is a part of the DLK spectrum remains unresolved. Given the striking resemblance of clinical features of the two conditions, we further warrant research to evaluate its etiology and treatment protocol.
References
- Moshirfar M, Madsen M, Wolsey D. Re: central toxic keratopathy: description of a syndrome in laser refractive surgery. Am J Ophthalmol. 2007; 144: 332–4.
- Mari Cotino JF, Suriano MM, De La Cruz Aguiló RI, Vila-Arteaga J. Central toxic keratopathy: a clinical case series. Br J Ophthalmol. 2013; 97: 701–3.
- Sonmez B, Maloney RK. Central toxic keratopathy: description of a syndrome in laser refractive surgery. Am J Ophthalmol. 2007; 143: 420–7.
- Fraenkel GE, Cohen PR, Sutton GL, Lawless MA, Rogers CM. Central focal interface opacity after laser in situ keratomileusis. J Refract Surg. 1998; 14: 571–576.
- Hadden OB, McGhee CN, Morris AT, Gray TB, Ring CP, Watson AS. Outbreak of diffuse lamellar keratitis caused by marking-pen toxicity. J Cataract Refract Surg. 2008; 34: 1121–4.
- Stonecipher KG, Ignacio TS, Stonecipher KG. Complications and management with the Femtosecond laser. In: Alió JL, Azar DT, editors. In Management of complications of refractive surgery. Springer Publishing; 2008.
- Hsu M, Tu E, Bouchard C. Confocal microscopy of contact lens keratitis presenting as central toxic keratopathy. Eye Contact Lens. 2011; 37: 377–80.
- Hau SC, Allan BD. In vivo confocal microscopy findings in central toxic keratopathy. J Cataract Refract Surg. 2012; 38: 710–12.
- Zhao J, Nagasaki T. Lacrimal gland as the major source of mouse tear factors that are cytotoxic to corneal keratocytes. Exp Eye Res. 2003; 77: 297–304.
- Moshirfar M, Hazin R, Khalifa YM. Central Toxic Keratopahy after LASIK surgery. Current Opinion in Ophthalmology. 2010; 21: 274-9.
- Hazin R, Daoud YJ, Khalifa YM. What is Central Toxic Keratopathy Syndrome if it is not Diffuse lamellar Keratitis Grade IV? Middle East Afr J Ophthalmol. 2010; 17: 60-2.
- Moshirfar M, Kurz C, Ghajarnia M. Contact lens-induced keratitis resembling central toxic keratopathy syndrome. Cornea. 2009; 28: 1077-80.