
Mini Review
Austin Pancreat Disord. 2017; 1(1): 1004.
Pancreatic Surgery in the Aged Population: Technical and Molecular Insights
César Machado MC*, Silva FP and César Machado MA
Emergency Medicine Department, University of Sao Paulo, Sao Paulo, Brazil
*Corresponding author: Marcel Cerqueira César Machado, Emergency Medicine Department, University of Sao Paulo, Sao Paulo, Brazil
Received: March 03, 2017; Accepted: March 21, 2017; Published: March 24, 2017
Abstract
Pancreatic resection is the only potentially curable treatment for pancreatic malignancies. Most of these malignancies occur in the aged population. In the past, these procedures were associated with significant morbidity and mortality. We herein reviewed recent advances in the knowledge of the physiological and immunological aspects of the aging process and improvements in the surgical techniques that have changed this scenario. We conclude that with appropriate selection, aged patients will outcomes similar to those of young patients, even after major pancreatic surgery.
Keywords: Pancreas; Cancer; Elderly; Surgery
Introduction
Pancreatic resection is currently the only curative treatment for pancreatic and biliary malignancies. Most of these malignancies occur mainly in aged patients [1]. In the past, pancreatic resection in the aged population was associated with increased morbidity and mortality rates of around 30% [2-4]. Indeed, aged patients have increased susceptibility to infection after surgical procedures [5].
Some recent reports, however, have shown that appropriate patient selection, establishment of good preoperative nutritional conditions, and appropriate management of the immunological and physiological changes that occur in the aged may reduce the morbidity and mortality associated with pancreatic resection [1], several other surgical procedures [6-9], and systemic inflammation in this population [10].
Aging and Systemic Inflammation
Aging is reportedly associated with a low-grade inflammatory state called inflammaging, which is characterized by higher production of proinflammatory cytokines than in younger patients [11].
Some studies have shown delayed increases in cytokine concentrations in aged patients after surgery [11]. We have also observed a delayed inflammatory response in aged patients who have undergone surgical procedures.
It is of paramount importance to consider that systemic inflammation is characterized by organ-specific alterations that may contribute to the increased morbidity in the aged population. In fact, we recently demonstrated that in a rodent model of acute pancreatitis, intestinal damage was much more severe in aged animals and was associated with increased bacterial translocation [12].
Such organ-specific alterations were further demonstrated in an experimental model of lung injury under conditions of systemic inflammation, in which the alterations were more severe in aged animals. The aged animals exhibited higher inducible nitric oxide synthase expression and lower extracellular superoxide dismutase expression than did young animals [13].
This low-grade inflammatory state is further documented by observation of monocyte activation and hypercytokinemia in aged patients following surgical interventions [14]. It has also been shown that mitogen-stimulated peripheral mononuclear cells in aged patients produce significantly higher levels of tumor necrosis factor (TNF)-a, interleukin (IL)-6 and IL-1-ß than do those in young patients [15].
Molecular Mechanisms of Age-Related Low- Grade Inflammatory State
Although several studies have been performed, the molecular mechanisms involved in inflammaging remain poorly understood. Involvement of the poly(ADP-ribose) polymerase-1 gene in inflammation and the aging process [16], the higher splenic tissue concentration of a-2A adrenergic receptors and phosphodiesterases, and the increased CD14 and toll-like receptor-4 expression in aged animals with sepsis are also associated with this increased inflammatory state in aged humans [17]. In a previous study of gene expression in aged patients with sepsis, we found disturbances in genes related to oxidative phosphorylation and mitochondrial function in peripheral neutrophils and considered that these disturbances may interfere with the neutrophils’ antimicrobial function [18].
Evaluation of the Aged Patient
When evaluating whether an aged patient is a candidate for pancreatic resection, we must use various biomarkers that will help to determine if the patient is fit for the procedure. One of these biomarkers is the patient’s walking speed. A previous study demonstrated an association between slower walking speeds and higher mortality rates [19]. Body composition (high body mass index) is also associated with age-related diseases, and a higher risk of mortality is associated with increased body fat and an increased waist circumference (>94cm for men and >77cm for women [20]. Certain inflammatory biomarkers of the aging process, such as IL-6, IL-1-ß, TNF-a, and C-reactive protein, are associated with various biophysical markers such as grip strength and gait speed, and may be used to evaluate the functional status of an aged patient [21]. Novel biomarkers are currently being evaluated and may be used in the future to better evaluate aged patients.
Pancreatic Resection in Aged Patients
Several recent studies of the feasibility of major pancreatic resection in the aged population have demonstrated that with appropriate perioperative management, aged patients may have outcomes similar to those of younger patients. Several reports have also shown that even more aggressive pancreatic resection in aged patients with vascular involvement is feasible without increased mortality [22].
A recent study unexpectedly found that aged patients undergoing very aggressive procedures such as modified Apple by pancreatic resection may have an even better prognosis than younger patients [23].
We studied 214 patients who had undergone pancreaticoduodenectomy in our center. The patients were divided into two groups based on age: Group I (patients aged <70 years) and Group II (those aged =70 years). The overall incidence of complications in Group II was 42.85%, while that in Group I was 28.5% (Table I). The overall incidence of complications among all 214 patients who underwent pancreaticoduodenectomy was 31.77%. All patients survived to the surgical procedure.
Age
Number of patients
number of complications (%)
70 yrs
49
21 (42.85)
< 70 yrs
165
47 (28.5)
p = 0.0577 (chi-square test).
Table 1: Pancreaticoduodenectomy in patients <70 and =70 years (personal data).
Several reports have shown that pancreatic resection in aged patients can be safely performed. A recent review found that patients aged =80 years had an increased incidence of postoperative mortality, morbidity and cardiac complications. However, comparison of only patients without differences in preoperative co morbidities revealed no increase in morbidity or mortality among patients aged =80 years [24].
Age alone is not an independent risk factor for complications; however, patient selection must be performed carefully [1, 25-27]. In a recent study, no differences were observed in the incidence of complications or in the overall morbidity and mortality rates between patients aged <75 and =75 years [24].
Thus, pancreatic resection can be recommended in aged patients if the presence of co morbidities and the surgeon and hospital volumes related to pancreatic resection are taken into account. Surgeon volume is inversely related to operative mortality for several procedures, including pancreatic resection [28].
The technical aspects of pancreatic resection, mainly pancreatic head resection, are important clues to the success of the procedure, especially in aged patients. Refinement of the dissection technique and reduction of tissue damage and bleeding are important in any procedure and are of particular importance in the aged patient. The technical aspects of reconstruction after pancreatic duodenal resection are also critical for the success of the procedure.
Our approach to reconstruction is based on the use of an isolated jejunal loop for the pancreatic enteric anastomosis with an emphasis on technical aspects and details [29]. This technique involves diversion of the pancreatic juice from the biliary secretion and may contribute to reducing the severity of pancreatic fistulas and their secondary complications [30]. It may therefore reduce morbidity, which is extremely important in aged patients.
Another important factor in the aged population is the increased bacterial translocation observed in these patients. Indeed, intestinal mucosal atrophy, epithelial tight junction damage, and increased bacterial populations have been observed in aged animals [31]. Our previous experimental study showed that in the presence of systemic inflammation, such as in acute pancreatitis, significantly higher bacterial translocation with increased numbers of bacterial colonies was present in the pancreas of aged animals. This was associated with a more severe local intestinal inflammatory response that included elevated expression of the COX-2 gene and decreased expression of tight junction protein genes [12]. Enteral deprivation can lead to increased expression of proinflammatory cytokines in the intestinal mucosa with epithelial damage and bacterial translocation [32] (Figure 1).
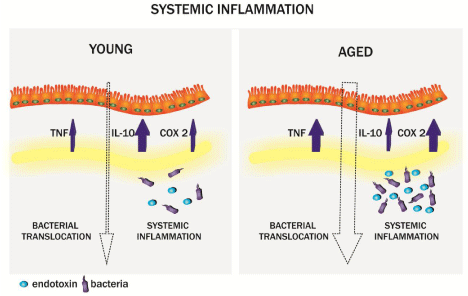
Figure 1: Schematic model of the inflammatory response in the bowel of
young and aged patients undergoing major pancreatic surgical procedures.
Therefore, aged patients requiring pancreatic surgery must undergo a very short preoperative fast and a short period of postoperative enteral deprivation. Early enteral nutrition has been shown to decrease the incidence of postoperative infectious complications in patients undergoing liver resection [33].
Enteral deprivation leads to a shift in the intestinal micro biota to predominantly Gram-negative Proteobacteria. This shift is associated with an increase in expression of proinflammatory cytokines within the mucosa, including interferon-γ and TNF-a. A concomitant loss of epithelial growth factors leads to a decrease in epithelial cell proliferation and increased apoptosis. The resulting loss of epithelial tight junction proteins contributes to intestinal barrier dysfunction. These mechanisms identify potential protective strategies against complications associated with total parenteral nutrition, such as modification of luminal bacteria, blockade of proinflammatory cytokines, or growth factor replacement [32].
Therefore, in aged patients undergoing pancreatic resection, we always leave an enteral feeding tube in place to begin enteral nutrition as soon as 24 hr after surgery, avoiding parenteral nutrition in this population.
Conclusion
Age is not an independent risk factor for complications or mortality following major pancreatic resection. A thorough understanding of the physiological and immunological characteristics of aging will allow for careful patient selection and use of the best available surgical techniques, providing aged patients with outcomes similar to those of younger patients, even after major pancreatic surgery.
References
- Shirai Y, Shiba H, Horiuchi T, Saito N, Furukawa K, Sakamoto T, et al. Assessment of Surgical Outcome After Pancreatic Resection in Extremely Elderly Patients. Anticancer research. 2016; 36: 2011-2017.
- Herter FP, Cooperman AM, Ahlborn TN, Antinori C. Surgical experience with pancreatic and periampullary cancer. Annals of surgery. 1982; 195: 274-281.
- Lerut JP, Gianello PR, Otte JB, Kestens PJ. Pancreatic duodenal resection. Surgical experience and evaluation of risk factors in 103 patients. Annals of surgery. 1984; 199: 432-437.
- Obertop H, Bruining HA, Schattenkerk ME, Eggink WF, Jeekel J, Van Houten H. Operative approach to cancer of the head of the pancreas and the periampullary region. The British journal of surgery. 1982; 69: 573-576.
- Surgery for colorectal cancer in elderly patients: a systematic review. Colorectal Cancer Collaborative Group. Lancet. 2000; 356: 968-974.
- Hosking MP, Warner MA, Lobdell CM, Offord KP, Melton LJ. Outcomes of surgery in patients 90 years of age and older. Jama. 1989; 261: 1909-1915.
- Koruda MJ, Sheldon GF. Surgery in the aged. Advances in surgery. 1991; 24: 293-331.
- Arenal JJ, Benito C, Concejo MP, Ortega E. Colorectal resection and primary anastomosis in patients aged 70 and older: prospective study. The European journal of surgery. 1999; 165: 593-597.
- Arenal JJ, de Teresa G, Tinoco C, Toledano M, Said A. Abdominal surgery in nonagenarians: short-term results. Surgery today. 2007; 37: 1064-1067.
- Machado MC, Coelho AM, Carneiro D’Albuquerque LA, Jancar S. Effect of ageing on systemic inflammatory response in acute pancreatitis. International journal of inflammation. 2012: 270319.
- Kudoh A, Katagai H, Takazawa T, Matsuki A. Plasma proinflammatory cytokine response to surgical stress in elderly patients. Cytokine. 2001; 15: 270-273.
- Barbeiro DF, Koike MK, Coelho AM, da Silva FP, Machado MC. Intestinal barrier dysfunction and increased COX-2 gene expression in the gut of elderly rats with acute pancreatitis. Pancreatology: official journal of the International Association of Pancreatology. 2016; 16: 52-56.
- Starr ME, Ueda J, Yamamoto S, Evers BM, Saito H. The effects of aging on pulmonary oxidative damage, protein nitration and extracellular superoxide dismutase down-regulation during systemic inflammation. Free radic biology & medicine. 2011; 50: 371-380.
- Ono S, Aosasa S, Tsujimoto H, Ueno C, Mochizuki H. Increased monocyte activation in elderly patients after surgical stress. Eur Surg Res. 2001; 33: 33-38.
- Fagiolo U, Cossarizza A, Santacaterina S, Ortolani C, Monti D, Paganelli R, et al. Increased cytokine production by peripheral blood mononuclear cells from healthy elderly people. Annals of the New York Academy of Sciences. 1992; 663: 490-493.
- Walston JD, Matteini AM, Nievergelt C, Lange LA, Fallin DM, Barzilai N, et al. Inflammation and stress-related candidate genes, plasma interleukin-6 levels, and longevity in older adults. Experimental gerontology. 2009; 44: 350-355
- Leong J, Zhou M, Jacob A, Wang P. Aging-related hyper inflammation in endotoxemia is mediated by the alpha2A-adrenoceptor and CD14/TLR4 pathways. Life sciences. 2010; 86: 740-746.
- Silva Pellegrina DV, Severino P, Barbeiro HV, Andreghetto F M, Tadeu Velasco I, Souza HP, et al. Septic Shock in Advanced Age: Transcriptome Analysis Reveals Altered Molecular Signatures in Neutrophil Granulocytes. PLOS one. 2015; 10: e0128341.
- Cooper R, Kuh D, Hardy R, Mortality Review G, Falcon, Teams HAS. Objectively measured physical capability levels and mortality: systematic review and meta-analysis. Bmj. 2010; 341: c4467.
- de Hollander EL, Bemelmans WJ, Boshuizen HC, Friedrich N, Wallaschofski H, Guallar-Castillon P, et al. The association between waist circumference and risk of mortality considering body mass index in 65- to 74-year-olds: a meta-analysis of 29 cohorts involving more than 58000 elderly persons. International journal of epidemiology. 2012; 41: 805-817.
- Visser M, Pahor M, Taaffe DR, Goodpaster BH, Simonsick EM, Newman AB, et al. Relationship of interleukin-6 and tumor necrosis factor-alpha with muscle mass and muscle strength in elderly men and women: the Health ABC Study. The journals of gerontology Series A, Biological sciences and medical sciences. 2002; 57: 326-332.
- Sun JW, Zhang PP, Ren H, Hao JH. Pancreaticoduodenectomy and pancreaticoduodenectomy combined with superior mesenteric-portal vein resection for elderly cancer patients. Hepatobiliary & pancreatic diseases international: HBPD INT. 2014; 13: 428-434.
- Wang X, Dong Y, Jin J, Liu Q, Zhan Q, Chen H, et al. Efficacy of modified Appleby surgery: a benefit for elderly patients? The Journal of surgical research. 2015; 194: 83-90.
- Casadei R, Ricci C, Lazzarini E, Taffurelli G, D’Ambra M, Mastroroberto M, et al. Pancreatic resection in patients 80 years or older: a meta-analysis and systematic review. Pancreas. 2014; 43: 1208-1218.
- Nakeeb A, Atef E, Hanafy E, Salem A, Askar W, Ezzat H, et al. Outcomes of pancreaticoduodenectomy in elderly patients. Hepatobiliary & pancreatic diseases international: HBPD INT. 2016; 15: 419-427.
- Oguro S, Shimada K, Kishi Y, Nara S, Esaki M, Kosuge T. Perioperative and long-term outcomes after pancreaticoduodenectomy in elderly patients 80 years of age and older. Lange beck’s archives of surgery/ Deutsche Gesellschaft fur Chirurgie. 2013; 398: 531-538.
- Marsoner K, Kornprat P, Sodeck G, Schagerl J, Langeder R, Csengeri D, et al. Pancreas Cancer Surgery in Octogenarians - Should We or Should We Not? Anticancer research. 2016; 36: 1979-1984.
- Birkmeyer JD, Stukel TA, Siewers AE, Goodney PP, Wennberg DE, Lucas FL. Surgeon volume and operative mortality in the United States. The New England journal of medicine. 2003; 349: 2117-2127.
- Machado MC, Machado MA. Systematic use of isolated pancreatic anastomosis after pancreatoduodenectomy: Five years of experience with zero mortality. European journal of surgical oncology: the journal of the European Society of Surgical Oncology and the British Association of Surgical Oncology. 2016; 42: 1584-1590.
- Ke S, Ding XM, Gao J, Zhao AM, Deng GY, Ma RL, et al. A prospective randomized trial of Roux-en-Y reconstruction with isolated pancreatic drainage versus conventional loop reconstruction after pancreaticoduodenectomy. Surgery. 2013; 153: 743-752.
- Ren WY, Wu KF, Li X, Luo M, Liu HC, Zhang SC, et al. Age-related changes in small intestinal mucosa epithelium architecture and epithelial tight junction in rat models. Aging clinical and experimental research. 2014; 26: 183-191.
- Demehri FR, Barrett M, Ralls MW, Miyasaka EA, Feng Y, Teitelbaum DH. Intestinal epithelial cell apoptosis and loss of barrier function in the setting of altered microbiota with enteral nutrient deprivation. Frontiers in cellular and infection microbiology. 2013; 3: 105.
- Togo S, Matsuo K, Tanaka K, Matsumoto C, Shimizu T, Ueda M, et al. Perioperative infection control and its effectiveness in hepatectomy patients. Journal of gastroenterology and Hepatology. 2007; 22: 1942-1948.