Abstract
Eosinophilic granuloma is a lytic lesion, driving from histiocyte proliferation of the bone. The lesions mostly occur in long bones, rib or skull, but the involvement of temporal bones is rare. We report the case of a 4-year-old girl with isolated eosinophilic granuloma of petrous apex, presenting with fever and right abducens paralysis.
Keywords: Eosinophilic granuloma; Petrous bone
Introduction
Eosinophilic granuloma is a lytic lesion, driving from histiocyte proliferation of the bone [1] and is a form of Langerhans Cell Histiocytosis (LCH) that is classified into three spectrums of diseases: Letterer Siwe disease, Hand schuller Christian syndrome and Eosinophilic granuloma [2]. These three patterns of disease have specific clinical manifestation.
Eosinophilic granuloma might be confused with chronic otitis media, external otitis and chronic mastoiditis [3]. It usually occurs before the age of ten years and has been reported in skull, spine, ribs, femur and pelvis [4].
Treatment includes curettage, radiation, radiosurgery and injection of steroid in lesions [2].
In this report we present a 4 year old girl with petrous apex Eosinophilic granuloma.
Case Report
A 4-year-old girl was referred to the infectious ward of Children Medical Center, the referral pediatric center in Tehran, Iran from ENT ward with diagnosis of mastoiditis. She had a history of fever and headache for one month and right eye internal deviation for fifteen days before admission to ENT department.
Her CT scan which was done in ENT ward revealed a destructive lesion on the tip of petrous bone due to petrositis (Figures 1 & 2). Brain MRI revealed the increase of signal in air cells of mastoid and right petrous apex in T2 that suggested right mastoiditis and AOM (Figures 3 & 4).
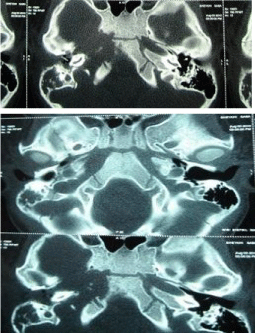
Figure 1 & 2: A destructive lesion on the tip of petrous bone.
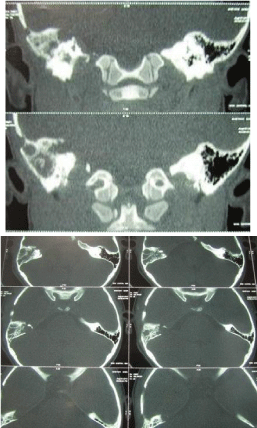
Figure 3 & 4: Brain MRI revealed the increase of signal in air cells of
mastoid and right petrous apex in T2.
On admission in our department she had fever without headache and vomiting. A complete examination showed that her ears were normal but she had abducens paralysis in right side and other exam was normal. The results of initial laboratory tests were as follows: WBC=8040/mm³, neutrophils=47/8%, lymphocytes=42/2%, hemoglobin=10/6g/dl, Platelet=456000/mm³.
ESR was 55 mg/dl and rose to 89 and 92 mg/dl during admission.
Neurosurgery consultation was done. The neurosurgeon confirmed the diagnosis of petrositis, so she was treated with clindamycin and ceftazidim for ten days. After treatment her eye deviation was slightly better so the follow up CT scan of temporal lobe was carried out (Figure 5).
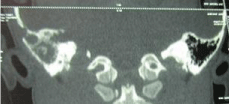
Figure 5: Follow up CT scan of temporal lobe.
The second CT scan of patient showed “Right mastoid air cells were opacified due to Eustachian tube involvment and external auditory canal appeared normal. Lytic lesion in the right apex petrous with lobulated erosion of the adjacent clivus bone associated with abnormal bulky soft tissue in the nasopharynx was observed. Extension of the lesion to the right cavernous sinus with same displacement of the ICA was noticed”.
Because of the extension of lesion despite the antimicrobial treatment, we planned to do the biopsy of patrons bone by consultation with ENT ward. Then the patients send to the ENT department and petrous bone biopsy was done.
Histiopatologic result of biopsy showed multiple tinny sections with indistinct cytoplasm and large rounded nuclei. There were also many eosinophils.
A diagnosis of eosinophilic granuloma was made and the patient was referred to the oncology department. They recommended follow up of patient without any treatment because the signs and symptoms of the patient were resolved after biopsy.
Discussion
Eosinophilic granuloma is a sub class of LCH that manifests itself with single or multiple lesions. This lesion usually occurs during the first decade of life and is mostly common in boys. The common sites of Eosinophilic granuloma are skull, long bone and spine. Also it can occur in the temporal lobe but it is rare.
Etiology of eosinophilie granuloma is unknown [2]. It is thought that abnormal immune regulations can lead to hyperplasia of langerhans cells [5]. Other causes of Eosinophilic granuloma can be trauma, hereditary disorders and metabolic disease [4]. Some studies suggest a role of viruses as the cause of disease [6,7].
The first report of the petrous apex Eosinophilic granuloma was reported in 1993 by Goldsmith [8].
Petrous apex granuloma usually is detected with cranial nerve palsy (V, VI, VII, VIII), headache, diplopia, vertigo and hearing loss [3]. The CT scan reveals destructive lesions in petrous apex. Biopsy is needed for the confirmation of diagnosis.
Pathologic finding shows langerhans cells and birbec granules on electron microscopy [2].
There are different kinds of treatment according to severity of disease including curettage, low dose radiation or corticosteroid injection [2].
Spontaneous remissions of single lesions have been reported after biopsy [9], but most exports suggest that lesions should be treated.
In our case the patient was on remission 6 months after biopsy without any treatment recently and we followed her by temporal CT without any progression.
References
- Oztrurk O, Baglam T, Inanli S, Sehitoglu MA. Eosinophilic Granuloma of the Temporal Bone. Otoscope. 2004; 2: 72-76.
- Jonas N, Mulwafu W, Khosa SA, Hendricks M. Case study: Langerhans Cell Histiocytosis (LCH). International Journal of Pediatric Otolaryngology. 2007; 3: 61-65.
- Kliegman R, Behrman R. Nelson Textbook of pediatrics 18th edition. 2649.
- Del Rio L, Lassaletta L, Martinez R, Sarria MJ, Gavilan J. Petrous bone Langerhans cell histiocytosis treated with Radiosurgery. Sterotact Funct Neurosurg. 2007; 85: 129-131.
- Irving RM, Broadbent V, Jones NS. Langerhans cell histiocytosis in children; management of head and neck manifestations. Laryngoscope. 1995; 104: 67-70.
- Mcclain K, Wriss RA. Viruses and Langerhans cell histiocytosis; is there a link? B J Cancer Suppl. 1994; 23: 34-36.
- Leany MA, Krejci SM, Friednash M. Human herpes virus 6 is present in lesions of Langerhans cell histiocytosis. J Invest Dermatol. 1995; 101: 642- 645.
- Derkuyes BM. Langerhans cell histiocytosis of the petrous bone and skull base. Am J otolorgicingol. 2002; 25: 27-32.
- Sweet RM, Kornblut AD, Hyams VJ. Eosinophilic granuloma in the temporal bone. Laryngoscope. 1979; 89: 1545-1552.
